Remote patient monitoring cost varies widely depending on how the program is designed, from device-led pilots to fully integrated, workflow-driven systems. For healthcare providers, the real question isn’t just “how much does RPM cost,” but how those costs scale with patient volume, staffing, and clinical outcomes.
A typical remote patient monitoring program includes device costs, platform fees, care team operations, and integration with existing systems. However, the total cost—and ROI—depends heavily on whether you use a SaaS platform, build a custom solution, or partner with a managed RPM provider.
As interest grows, understanding the cost of remote patient monitoring becomes crucial for providers and investors. Several components contribute to the total cost, from device procurement and platform subscriptions to training and compliance requirements. While the upfront investment may vary based on the scale and sophistication of the solution, the long-term savings and improved outcomes make remote patient monitoring a cost-effective tool in transforming healthcare delivery.
Breakdown of RPM Costs
Understanding the cost of remote patient monitoring involves analyzing the major components contributing to the total investment. These typically include device acquisition, software subscriptions, and operational implementation—all of which vary depending on the scale and complexity of your remote patient monitoring program.
A. Device Costs
One of the foundational aspects of remote patient monitoring is using medical-grade devices to collect real-time health data. Standard devices include blood pressure monitors, glucose meters, pulse oximeters, and wearable sensors that transmit data to healthcare providers. Device costs vary widely depending on type and clinical grade. Basic RPM devices (such as blood pressure monitors or pulse oximeters) may cost under $100 per unit, while advanced kits with multiple connected devices can exceed $150–$300 depending on configuration and vendor.
B. Software and Platform Costs
RPM platform pricing typically ranges from $80 to $200 per patient per month, depending on features, level of automation, and vendor model. Costs increase with advanced capabilities such as AI-based triage, care coordination workflows, and EHR integration.
C. Operational and Implementation Costs
Beyond devices and software, operational expenses are pivotal in determining the overall cost of remote patient monitoring. This includes hiring clinical staff for real-time monitoring and follow-ups, and training staff and patients to use RPM tools effectively. Maintenance costs—like software updates, technical support, and compliance measures—are essential to ensure smooth program execution.
In addition to these costs, the overall remote patient monitoring cost varies significantly based on the deployment model. SaaS RPM platforms typically involve predictable per-patient monthly fees, while managed RPM services bundle staffing and outreach into higher per-patient costs. In contrast, custom-built RPM systems require higher upfront investment for development and integration but reduce per-patient cost significantly as programs scale and patient volumes increase.
How Many Care Managers Do You Need?
Clinical staffing is the largest hidden cost in most RPM programs. Industry-typical care manager-to-patient ratios as of 2026:
- Standard chronic care RPM (HF, HTN, diabetes): 1 FTE per 150-200 patients
- High-acuity or post-discharge RPM: 1 FTE per 100-125 patients
- AI-assisted / exception-based workflow programs: 1 FTE per 200-300 patients
A US-based RN care manager fully loaded (salary + benefits + overhead) typically runs $110K-$145K per year. At 175 patients per FTE, that’s roughly $52-69 per patient per month in clinical staffing alone, before any platform, device, or billing operations cost.
The unit-economics question every program must answer: at what capture rate does staffing cost get covered by reimbursement? At $244 PPPM stacked revenue (RPM + CCM, see billing page) and 70% claim capture, net is roughly $171 PPPM revenue against $200-260 PPPM all-in cost. That’s underwater. At 90% capture and full RPM + CCM stacking, the math turns positive. Capture rate is the single biggest controllable cost lever, not platform price.
What Is the All-In Cost Per Patient Per Month?
The pricing tiers most vendors publish (SaaS, custom, managed) cover platform cost only. Total program cost per patient is meaningfully higher once devices, clinical staffing, integration, and billing operations are added. Here is the all-in PPPM range by deployment model, based on industry-typical ranges as of 2026:
| Cost Component | DIY In-House (build + buy + staff) | SaaS Platform + Your Clinical Staff | Full Managed Service (devices + platform + monitoring outsourced) |
|---|---|---|---|
| Devices (amortized over 24 months) | $5-15 PPPM | $5-15 PPPM | Bundled |
| Software platform | $10-25 PPPM (build amortized) | $80-150 PPPM | Bundled |
| Clinical staffing (1 FTE per 150-200 patients) | $55-80 PPPM | $55-80 PPPM | Bundled |
| Integration / IT / compliance (steady state) | $10-20 PPPM | $5-15 PPPM | Bundled |
| Billing / RCM operations | $5-10 PPPM | $5-10 PPPM | Bundled (typically) |
| Total all-in PPPM | ~$85-150 PPPM | ~$150-270 PPPM | $120-300 PPPM (vendor-set, publicly cited range) |
Why DIY in-house is cheaper PPPM but not always the right call: the build cost (typically $100K-$300K+ upfront for custom RPM software per the Pricing Models table below) creates a fixed investment that only pays off at scale. At 100 patients, the per-patient amortization is high. At 1,000 patients, in-house can run 30-50% lower PPPM than a SaaS-plus-staff hybrid. The breakpoint typically lands somewhere between 300-500 patients depending on staffing model and integration depth.
Why managed services cost more PPPM: the markup pays for the vendor’s clinical staff, device logistics, and compliance overhead. For programs without internal RPM operational capacity, managed is the fastest path to revenue. For programs with care management infrastructure already in place, it’s redundant cost.
The right model depends on three questions covered in the Build vs Buy section below.
RPM Pricing Models: SaaS vs Custom vs Managed Services
SaaS RPM Platform
- $80–$150 per patient/month
- Fast deployment
- Limited workflow customization
Custom RPM Platform
- Higher upfront ($100K–$300K+ depending on scope)
- Lower long-term cost at scale
- Full workflow control
Managed RPM Services
- $120–$300 per patient/month
- Includes staffing + outreach
- Less internal burden, lower control
What Factors Influence Remote Patient Monitoring Cost?
Several clinical, operational, and technical factors directly influence remote patient monitoring cost, especially as programs scale across patient populations:
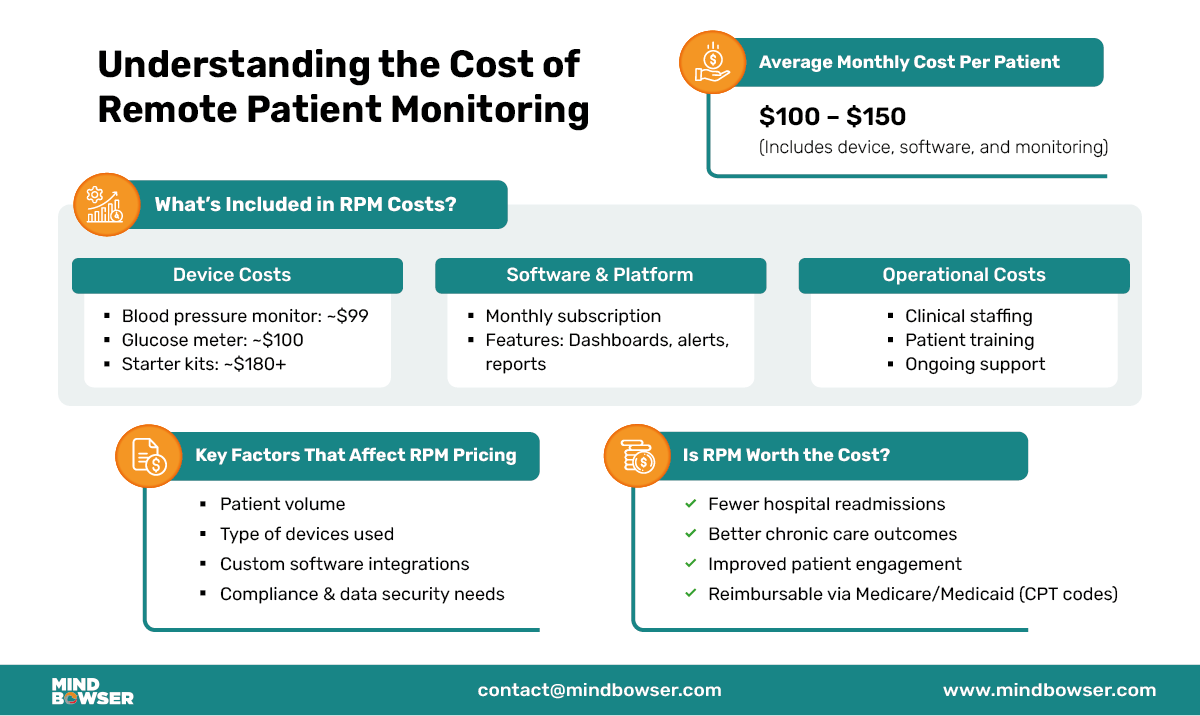
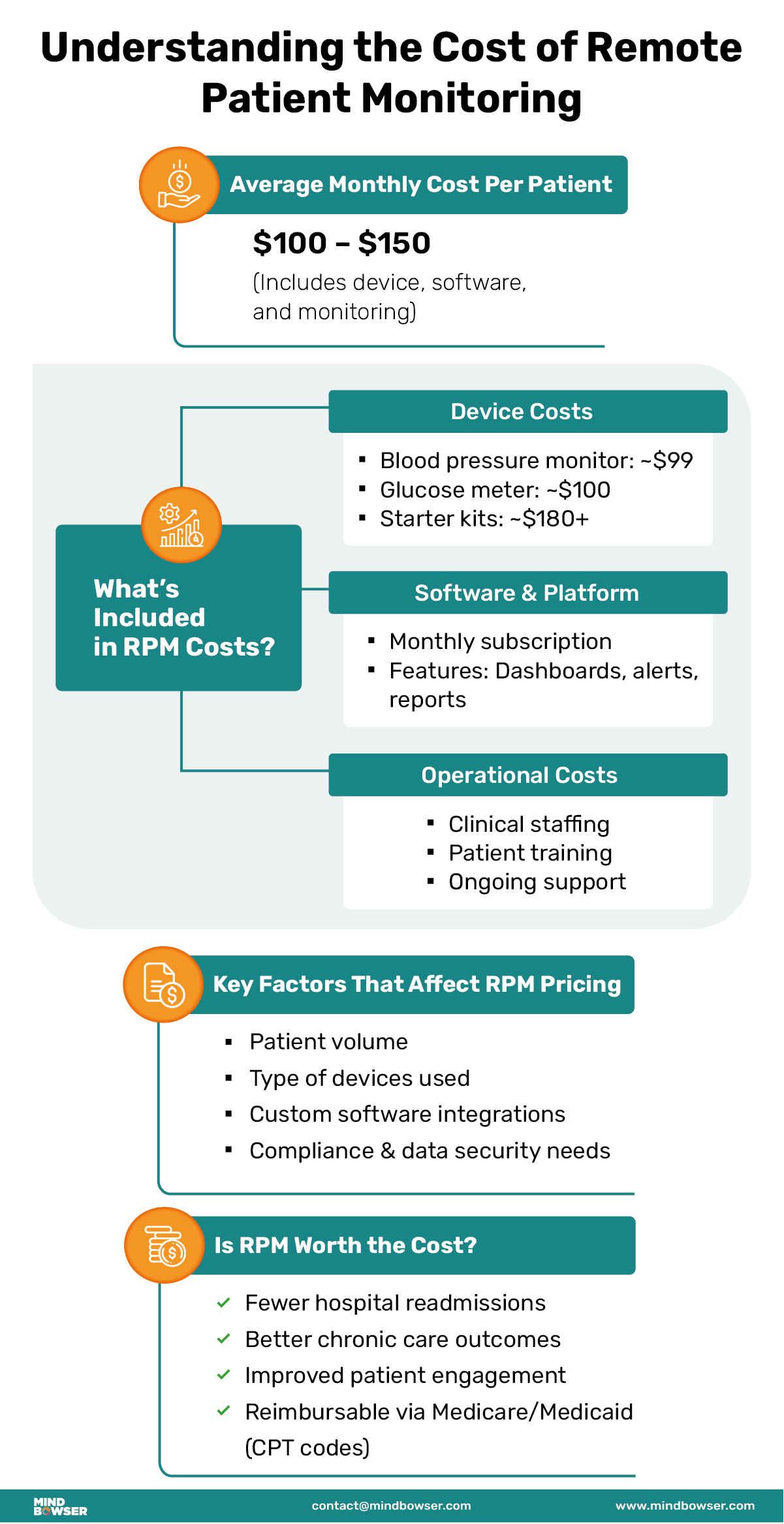
✅ Patient Population Size
Larger patient populations tend to reduce the per-patient cost due to economies of scale. When RPM services are deployed across more individuals, fixed expenses, such as platform subscriptions and care team staffing, are distributed, making the program more cost-efficient.
✅ Device Sophistication
The more advanced the monitoring devices, the higher the overall cost. Devices with real-time tracking, multiple sensors, or wireless connectivity command a premium compared to basic vitals trackers. These features, while beneficial, can significantly increase the initial and ongoing expenses.
✅ Customization Needs
Tailoring the RPM platform to fit a healthcare practice’s unique workflows, branding, or EHR integration needs can raise implementation costs. Customized dashboards, alerts, and data visualization often require additional development and maintenance.
✅ Compliance and Security Requirements
Ensuring HIPAA compliance and robust data security is essential, but comes with added costs. This includes encrypted data transmission, secure storage, user authentication, and regular security audits—all critical to protecting patient information and maintaining trust.
Related read: Remote Patient Monitoring Billing: CPT Codes & Reimbursement
Cost-Benefit Analysis
When assessing the cost of remote patient monitoring, it’s crucial to consider the upfront expenses and the long-term financial and clinical benefits it delivers. Healthcare businesses may create a sustainable model that promotes improved health outcomes and cost control by investing in remote patient monitoring, which unlocks value across operational and patient care dimensions.
☑️ Financial Benefits
One of the most tangible advantages of remote patient monitoring is reducing hospital readmissions. By continuously tracking patient health data, providers can identify complications early and intervene before hospital-level care is needed, significantly decreasing costly readmissions.
Remote patient monitoring brings measurable improvements in operational efficiency—automating routine monitoring tasks, improving workflow, and helping clinical staff focus on critical care. Additionally, the cost of remote patient monitoring can be offset by new revenue opportunities from improved patient satisfaction, better reimbursement rates, and expanded remote care programs, making it a financially sound investment.
Programs that incorporate AI remote patient monitoring further reduce manual review, improve early risk detection, and increase care team efficiency.
☑️ Clinical Benefits
Beyond the numbers, the clinical impact of remote patient monitoring is equally compelling. It encourages enhanced patient engagement, allowing individuals to participate more actively in their health management. This ongoing connection fosters trust and adherence to care plans.
Remote patient monitoring enables proactive care management—empowering providers to act on early warning signs before issues escalate. Over time, this leads to better outcomes, especially in managing chronic conditions like diabetes, hypertension, or heart disease.
ROI of Remote Patient Monitoring Programs
Remote patient monitoring programs deliver measurable financial and operational returns when designed with scalability and workflow efficiency in mind.
RPM programs deliver measurable returns when designed with full revenue capture and concurrent care management billing in mind. The ROI math fails when programs bill RPM in isolation. It works when RPM is one revenue stream in a stacked chronic care program.
Worked example: 200-patient program, 12-month view
| Line item | Without CCM stacking (RPM only) | With CCM stacking (RPM + CCM) | With CCM stacking + 90% capture rate |
|---|---|---|---|
| Per patient per month revenue | ~$135 (99454 + 99457 + 99458 at 70% capture) | ~$171 (RPM + CCM at 70% capture, $244 PPPM gross) | ~$220 (RPM + CCM at 90% capture) |
| 200 patients monthly revenue | $27,000 | $34,200 | $44,000 |
| 200 patients monthly cost (mid-range) | $40,000 | $40,000 | $40,000 |
| Monthly net (revenue – cost) | -$13,000 | -$5,800 | +$4,000 |
| Plus avoided readmissions (3-4 patients/year saved x $15K) | +$3,750/mo | +$3,750/mo | +$3,750/mo |
| Total monthly net | -$9,250 | -$2,050 | +$7,750 |
| Annualized | -$111K | -$24K | +$93K |
Three insights from the math:
- RPM alone does not pay for itself at 200 patients with typical 70% capture rates. The audit-friendly headline of “RPM ROI” is real only when paired with concurrent care management billing.
- CCM stacking turns RPM from a loss leader into break-even. Adding CCM revenue to the same patient panel is the largest revenue lever available without adding any additional patients or clinical FTE.
- Capture rate is the largest controllable cost lever. Going from 70% to 90% capture (closing denial reasons documented on the billing page) drives a $20K+ per month swing on the same patient panel. Most programs treat capture rate as a billing problem. It is a platform-and-workflow problem.
Payback period for an RPM program:
Typically 6-14 months for programs that hit 80%+ capture rate from launch with CCM stacking enabled. Programs that start with RPM-only billing and add CCM later typically take 18-30 months to break even on the Year 1 setup investment.
Total Cost of Ownership: Year 1 vs Year 3
Year 1 RPM cost is dominated by setup. Year 2 onward is steady-state operations plus growth. The 3-year view changes, which deployment model wins on cost.
| Cost component | Year 1 (200 patients, setup-heavy) | Year 2 (300 patients, steady state) | Year 3 (500 patients, scaling) |
|---|---|---|---|
| One-time setup (build / config / integration) | $80K-$200K (custom) or $15K-$40K (SaaS onboarding) | $0 | $0 |
| Devices (amortized) | $20K-$40K | $30K-$60K | $50K-$100K |
| Platform | $15K-$45K (custom maintenance) or $200K-$360K (SaaS at $80-150 PPPM) | $300K-$540K (SaaS) or $20K-$60K (custom) | $500K-$900K (SaaS) or $30K-$80K (custom) |
| Clinical staffing (RN care managers) | $130K-$170K (1 FTE) | $200K-$260K (1.5 FTE) | $330K-$440K (2.5 FTE) |
| Integration / IT / compliance | $30K-$60K | $20K-$40K | $30K-$60K |
| Billing operations | $15K-$25K | $20K-$35K | $30K-$50K |
| Total Year cost (SaaS path) | ~$390K-$735K | ~$575K-$945K | ~$945K-$1.55M |
| Total Year cost (Custom build path) | ~$290K-$540K | ~$285K-$465K | ~$465K-$770K |
| 3-year cumulative (SaaS path) | n/a | n/a | ~$1.91M-$3.23M |
| 3-year cumulative (Custom path) | n/a | n/a | ~$1.04M-$1.78M |
Talk to Our Experts if You Want to Build an RPM Platform That Improves Revenue Capture and ROI
Strategies to Optimize RPM Costs
Implementing remote patient monitoring can involve a significant investment, but thoughtful planning helps keep costs manageable. Hospitals and providers can reduce long-term expenses using smart choices during deployment and scaling.
▶️ Prioritize Essential Features
Start by identifying the core features that align with your clinical goals. Instead of opting for every available function, focus on the tools supporting your workflows— patient alerts, data tracking, and clinician dashboards. Avoiding feature overload reduces upfront costs and limits unnecessary complexity.
Designing a strong RPM care manager workflow is critical to reducing manual effort, improving patient follow-up, and controlling long-term operational costs.
▶️ Leverage Cloud-Based Solutions
Cloud platforms remove the need for on-premise infrastructure, lowering setup and maintenance costs. They also offer flexibility to scale as patient volumes grow, making it easier to adapt without large capital investments.
▶️ Select the Right Development Team
Partnering with a skilled development team ensures efficient execution, faster time-to-market, and fewer reworks. Look for teams with experience in healthcare software and regulatory compliance to minimize hidden costs tied to delays or missed standards.
▶️ Integrate Telehealth and Wearables
Bundling remote patient monitoring with telehealth visits and wearable integration helps consolidate tools and services. This improves care delivery and reduces separate vendor costs, enabling a more efficient care model.
Related read: Wearable Integration in Healthcare: How It Transforms Patient Monitoring and Care?
How Can Mindbowser Help You With the Cost of Remote Patient Monitoring?
Mindbowser helps healthcare organizations control and optimize the cost of remote patient monitoring by offering end-to-end support, from strategy to deployment, focused on clinical value and ROI.
➡️ Custom RPM Software Development: We build only the features you need, reducing unnecessary expenses while ensuring patient and clinician usability.
➡️ Cloud-Native Architecture: Our solutions are built on scalable cloud platforms (AWS, GCP), helping you minimize infrastructure costs and future-proof your RPM system.
➡️ Wearables and EHR Integration: Our accelerator makes it easy to connect RPM devices (e.g., Dexcom, Apple Health) and integrate with EHRs like Epic or Cerner without starting from scratch.
➡️ HIPAA-Compliant and Interoperable: Every solution we develop adheres to HIPAA, HL7, and FHIR standards, so you avoid costly compliance pitfalls later.
With a proven track record in building remote care platforms, we help you launch faster, reduce overhead, and deliver better outcomes—all while keeping your remote patient monitoring costs under control.

Conclusion
Remote patient monitoring offers a cost-effective solution for modern healthcare challenges by enabling proactive care, reducing hospital readmissions, and improving chronic disease management. While the initial costs can seem high, the long-term savings, operational efficiencies, and better health outcomes provide a solid return on investment for providers and payers alike.
As technology evolves, remote patient monitoring will become even more accessible and affordable. Integrations with wearable devices, AI-based analytics, and telehealth platforms are expected to streamline workflows further. For providers aiming to future-proof their care delivery models, remote patient monitoring is not just a cost—it’s a strategic investment in smarter, value-based care.
Remote patient monitoring all-in cost typically ranges from $150 to $300 per patient per month, depending on deployment model (DIY in-house, SaaS + your clinical staff, or full managed service). The platform-only cost is $80-$200 PPPM. Total cost adds devices, clinical staffing, integration, and billing operations on top. Reimbursement under the 2026 CPT family (99453, 99454, 99445, 99457, 99458, 99470, 99091) plus concurrent CCM stacking can return $200-$300 PPPM gross revenue per dual-enrolled patient.
RPM platform cost depends on device types, integration complexity, patient volume, staffing model, and workflow customization requirements.
Custom RPM systems have higher upfront costs but become more cost-effective at scale, while SaaS platforms offer faster deployment with recurring per-patient fees.
RPM reduces healthcare costs by preventing readmissions, enabling early intervention, and improving care team efficiency through automation and continuous monitoring.
Hidden costs include care team staffing, patient onboarding, workflow inefficiencies, integration challenges, and ongoing compliance requirements.
Typically 6-14 months for programs that launch with 80%+ claim capture rate and concurrent CCM billing enabled. Programs that start with RPM-only billing and add CCM stacking later usually take 18-30 months to break even on Year 1 setup investment. Capture rate is the single biggest variable. A program at 90% capture breaks even meaningfully faster than one at 70%.
Three drivers create most of the variance: (1) what the vendor includes versus charges as add-ons (clinical staffing, device logistics, billing support), (2) integration depth (basic FHIR ingestion vs full bidirectional EHR write-back), and (3) volume tier discounts that kick in at 250 / 500 / 1,000 patients. Headline PPPM numbers from vendor marketing often exclude one or more of these.
Clinical staffing. Most cost models focus on platform PPPM and devices, but at 1 FTE per 150-200 patients and ~$110K-$145K per RN care manager all-in, staffing typically runs $52-$69 PPPM, often more than the platform. Programs without exception-based workflows and AI-assisted triage hit higher staffing ratios (1 per 100 patients), driving PPPM staffing costs above $90.




















 BLOGS
BLOGS  NEWSROOM
NEWSROOM  CASE STUDIES
CASE STUDIES  WEBINARS
WEBINARS  PODCASTS
PODCASTS  ASSET HUB
ASSET HUB  EVENT CALENDAR
EVENT CALENDAR 





















