TL;DR
- Most RPM programs break down at the care manager workflow layer, not at the device or analytics layer.
- Care managers are forced into manual outreach, fragmented dashboards, and inconsistent escalation, driving missed readings and low patient adherence.
- Elderly and chronic-care populations consistently respond better to simplified, non-app engagement models (SMS, automated nudges) than complex mobile apps.
- When RPM workflows are not aligned to how care teams actually operate, clinical visibility degrades, and operational costs rise.
- Workflow-first RPM design reduces follow-ups, improves adherence, and provides leadership with a predictable, auditable care-delivery model.
Why does the care manager workflow break down in most RPM programs?
Most RPM programs are designed around devices and data capture, not around how care managers are expected to operate every day. That is where the RPM care manager workflow starts to break down.
In the consultation call, the issue wasn’t whether data could be collected. Devices were in place, and readings were technically available.
The failure became apparent after that point, when readings were missed, patients didn’t respond, and care managers had to decide what to do next without a clear, system-driven remote patient monitoring workflow.
That gap forces care teams into manual work: chasing patients, switching tools, and relying on individual judgment instead of predictable escalation. Over time, this leads to more missed follow-ups, greater operational friction, and increased RPM alert fatigue.
RPM doesn’t fail at the data layer. It fails at the RPM care manager workflow layer, where engagement, escalation, and documentation should work as one.
This is where most remote patient monitoring workflow issues begin to surface.
I. Where RPM Care Manager Workflow Friction Actually Shows Up
Across mid-market providers, we see the same breakdown points:
- Manual patient follow-ups
Care managers chase missing readings one patient at a time, often outside the system of record. - Fragmented engagement tools
Devices, reminders, alerts, and documentation are maintained in separate systems with no unified workflow. - Inconsistent escalation logic
Abnormal readings don’t trigger predictable actions; some get missed, others create alert fatigue. - Poor fit for elderly patients
App-heavy RPM models assume digital fluency that doesn’t exist among a large portion of the chronic care population.
The result: care managers spend more time managing tools than managing patients.

II. What Fails Before Leadership Sees It
By the time RPM performance shows up in leadership dashboards, the damage is already done:
- Missed readings are treated as patient non-compliance instead of workflow design failure
- Care manager burnout increases as panels grow
- Clinical visibility becomes episodic, not continuous
- ROI discussions stall because outcomes can’t be tied to consistent execution
This isn’t a staffing issue. It’s a workflow architecture issue.
III. How RPM Care Manager Workflow Design Impacts Workload
Poor engagement design increases hidden work and pushes the RPM care manager workflow back into manual mode.
From the consultation call, one pattern was clear: the more the RPM program relied on apps, the more work shifted back to the care team.
A. App-heavy Rpm Models Increase Hidden Workload
On paper, apps look efficient. In practice, they introduce friction:
- Elderly patients forget logins, notifications, or steps
- Readings fail silently when apps aren’t opened
- Care managers must manually check who hasn’t engaged
- Follow-ups move to phone calls, texts, and spreadsheets outside the RPM platform
What’s framed as “patient non-adherence” becomes care manager recovery work.
B. SMS And Automated Nudges Change The Math
Simplified engagement models, especially SMS-based workflows, behave differently:
- Messages reach patients without requiring app adoption
- Reminders are time-bound and contextual (not generic push alerts)
- Non-response can trigger automated escalation, not manual chasing
- Care managers intervene only when thresholds are crossed
This doesn’t remove clinical oversight. It protects it by ensuring attention is spent where it matters.
C. Workflow-first Engagement Reduces Operational Drag
When engagement is embedded into the workflow:
- Panels scale without proportional staffing increases
- Adherence improves without adding touchpoints
- Escalation becomes predictable and auditable
- Care managers move from “monitoring activity” to managing risk
This is the difference between RPM as a pilot and RPM as a program.
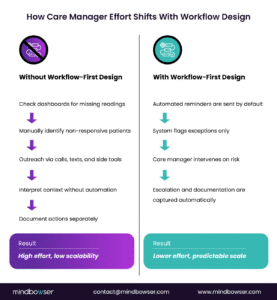
IV. What a Remote Patient Monitoring Workflow Should Actually Look Like
A strong remote patient monitoring workflow reduces unnecessary decisions and creates a more predictable operating model for care teams.
Workflow-first RPM isn’t a feature. It’s an operating model.
From the call, the strongest signal was this: care teams don’t need more data, they need fewer decisions per patient, with clearer defaults.
A. Core Components Of A Workflow-first Rpm Design
In mature RPM programs, the workflow is intentionally constrained:
- Single intake → multiple devices
Patients can use different RPM devices, but data is centralized in a single normalized flow rather than in parallel dashboards. - Defined engagement paths
Reminders, nudges, and follow-ups are pre-configured by condition, patient segment, and risk, not left to individual care managers. - Rule-based escalation
Abnormal readings, missed readings, or prolonged inactivity automatically trigger specific actions. - Exception-driven intervention
Care managers step in only when thresholds are crossed, not to monitor baseline activity.
This structure turns RPM from continuous surveillance into managed exception handling.
B. Where Most Rpm Architectures Fall Short
Programs fail when:
- Engagement logic lives outside the care workflow
- Alerts lack clinical context or prioritization
- Documentation is manual or duplicated
- Escalations are tribal knowledge, not system behavior
Each gap adds invisible labor, and that labor scales linearly with patient volume.
C. Designing For Auditability And Compliance
Workflow-first design also supports compliance:
- Clear logs of outreach, response, and escalation
- Consistent documentation paths aligned to care plans
- Reduced ad hoc communication outside approved systems
This matters when RPM moves from pilot to reimbursed, reportable care.
V. How To Evaluate Your Current Care Manager Workflow (before Scaling Rpm)
Before adding devices, vendors, or headcount, leadership needs clarity on one question:
Is our RPM workflow designed to scale or to survive?
Based on what surfaced in the call and across similar programs, here’s a practical evaluation lens.
A. 5 Workflow Questions Every Rpm Leader Should Answer
- Where do missed readings surface first?
- Inside the RPM platform
- Or through manual checking and follow-ups?
- What triggers care manager action today?
- Clear, rule-based thresholds
- Or individual judgment and inbox monitoring?
- How much engagement is automated vs manual?
- Are reminders and nudges system-driven?
- Or dependent on care manager availability?
- Can you explain escalation logic to an auditor?
- Is it documented and consistent?
- Or learned informally over time?
- Does workflow complexity increase with patient volume?
- Or does the system absorb scale without added effort?
If these answers aren’t consistent across the team, the issue isn’t adoption, it’s architecture.
B. Early Warning Signs You’re Scaling Too Fast
- Care managers rely on side tools (personal texts, notes, spreadsheets)
- “High-touch” becomes the default, not the exception
- Leadership sees adherence issues without visibility into root causes
- ROI conversations stall because outcomes can’t be operationally explained
These are signals to pause expansion, not to push harder.
VI. How RPM Alert Fatigue Hurts ROI and Care Team Performance
Devices or dashboards don’t drive RPM ROI. It’s driven by how consistently care workflows execute at scale.
From the call, the financial tension was clear: teams were investing in RPM, but outcomes felt fragile because execution hinged too heavily on people rather than systems.
A. The Hidden Cost Centers Leadership Often Misses
When workflows aren’t designed upfront, costs show up indirectly:
- Care manager time leakage
Manual follow-ups, duplicate documentation, and tool switching consume hours that don’t show up as line items. - Unpredictable staffing needs
As panels grow, so does labor often without a clear productivity model. - Clinical risk from missed signals
Incomplete readings reduce intervention effectiveness and increase downstream utilization risk. - Inconclusive ROI reporting
When execution varies, leadership can’t confidently tie RPM spend to outcomes.
These costs compound quietly as programs expand.
B. Workflow-first Design Creates Measurable Leverage
When RPM workflows are intentional:
- Care manager panels expand without linear staffing growth
- Engagement improves without adding touchpoints
- Escalations become timely and defensible
- Leadership gains confidence in program economics
ROI becomes less about proving value and more about protecting margin and reducing risk.
C. What Executives Should Measure Instead
Rather than focusing only on enrollment or device counts, mature programs track:
- % of interventions triggered automatically vs manually
- Average care manager actions per patient per week
- Time from abnormal reading to documented response
- Adherence recovery rate after automated nudges
These metrics reveal whether RPM is operationally sound or structurally fragile.
This will close with a clear, consultative CTA aligned to leadership readiness.
VII. How to Improve an RPM Care Manager Workflow Without Adding More Tools
Most RPM programs don’t need a reset. They need a workflow correction.
The shift isn’t about replacing devices or adding new tools; it’s about redesigning how engagement, escalation, and documentation work together.
A. A Practical Transition Path
For mid-market providers and scaling healthtech teams, the move typically looks like this:
- Map the current care manager workflow (end-to-end)
- From patient onboarding to escalation to documentation
- Identify where manual work compensates for system gaps
- Standardize engagement by patient segment
- Elderly vs digitally fluent populations
- Chronic vs post-acute use cases
- Default to low-friction channels (SMS, automated reminders) where appropriate
- Define escalation as system behavior, not team knowledge
- What happens after one missed reading? Three?
- What constitutes a clinical vs an operational alert?
- Design for exceptions, not constant oversight
- Care managers should manage risk, not monitor activity
- Automation handles the baseline; humans handle judgment
- Validate compliance and auditability early
- Ensure outreach, responses, and actions are logged consistently
- Align workflows with reimbursement and reporting requirements
This approach reduces variability before it reduces cost.
B. When To Reassess Before Scaling
If your RPM program shows any of the following, it’s time to pause expansion:
- Care managers rely on personal workarounds
- Engagement success varies widely by patient cohort
- Escalations aren’t explainable outside the team
- ROI discussions feel qualitative, not operational
These are solvable problems, but only if addressed at the workflow layer.
Case Example: Workflow-First RPM Redesign
We helped a digital health platform redesign its RPM program around a workflow-first model, replacing manual follow-ups with rule-based escalation and SMS-driven engagement.
As a result, care teams reduced manual outreach, improved patient adherence, and achieved over 90% engagement consistency across patient cohorts (based on internal project data).
More importantly, care managers were able to handle larger patient panels without increasing workload, shifting focus from task execution to clinical decision-making.

Next Step: Assess Before You Scale
For teams planning to expand RPM panels or redesign engagement models, a workflow-first assessment often surfaces faster gains than adding new technology.
A focused review of care manager workflows, engagement logic, and escalation paths can identify where automation should replace manual effort and where clinical judgment should remain central.
That clarity is what turns RPM from a promising initiative into a dependable program.
An RPM care manager workflow is the process used to monitor patient readings, trigger follow-ups, document outreach, and escalate issues when needed. A strong workflow helps care teams manage more patients without relying on manual workarounds.
Alert fatigue in RPM programs usually happens when abnormal readings, missed readings, and reminders are not prioritized correctly. Without rule-based escalation, care managers end up reviewing too many low-value alerts and can miss the signals that matter most.
RPM workflows reduce care manager workload by automating reminders, follow-ups, and escalation steps based on patient behavior and clinical thresholds. This shifts care teams away from manual outreach and toward exception-based intervention.
Without tight EHR integration, RPM workflows create duplicate documentation and constant context switching for care managers. Effective integration ensures patient data, outreach, and escalations flow into the clinical workflow instead of creating a separate system.
RPM programs scale more effectively when patient segmentation, engagement, and escalation are rule-based and automated. This allows care managers to oversee larger panels while focusing only on patients who need intervention.




















 BLOGS
BLOGS  NEWSROOM
NEWSROOM  CASE STUDIES
CASE STUDIES  WEBINARS
WEBINARS  PODCASTS
PODCASTS  ASSET HUB
ASSET HUB  EVENT CALENDAR
EVENT CALENDAR 





















