TL;DR
Epic Phoenix is Epic’s transplant-specific module designed to manage the entire transplant lifecycle, from evaluation and waitlist management to surgery and long-term follow-up, all within a single Epic record.
The Epic Phoenix module embeds UNOS-aligned workflows, structured documentation, and longitudinal episode tracking directly into daily transplant operations, reducing manual work and compliance risk. Native integration with the Epic ecosystem ensures transplant data flows seamlessly across labs, pharmacy, cardiology, and other specialties.
While often compared to Epic Beacon, Epic Phoenix is purpose-built for organ transplant care, not oncology treatment.
“Can this system actually handle the regulatory, clinical, and operational risk of running a transplant program without creating more work for my team?”
Transplant programs sit at the sharp edge of healthcare. Every workflow is regulated. Every delay has consequences. Every data gap becomes a compliance risk.
Epic Phoenix was built for that environment.
Embedded directly within the organization’s core clinical record, Epic Phoenix is a transplant-specific solution designed to manage the full lifecycle of organ transplantation, from referral and evaluation through waitlist management, surgery, and lifelong follow-up. Rather than relying on standalone tracking tools, it uses the same integrated data foundation as the broader health system, allowing transplant information to move fluidly across specialties instead of residing in a disconnected system.
Within Epic’s specialty portfolio, Epic Phoenix is often mentioned alongside Epic Beacon, the oncology module. The comparison is intentional. Both support high-risk, protocol-driven care over long periods. Both replace fragmented documentation with structured workflows inside Epic. The difference is focus. Epic Phoenix is built around organs, donors, recipients, and regulatory reporting, while Epic Beacon is built around chemotherapy regimens and oncology treatment plans.
For transplant programs, this distinction matters. Transplant care is not episodic. It is longitudinal, regulated, and unforgiving of errors. Epic Phoenix exists to meet those demands inside a single, unified patient record.
Epic Phoenix is not an add-on. It is the system of record for modern transplant programs.
I. What Is Epic Phoenix?
Epic Phoenix is a transplant-specific clinical application built inside the Epic Electronic Medical Record to manage the operational and clinical complexity of organ transplantation. It functions as a centralized command center for transplant programs, bringing donor, recipient, and organ data into a single longitudinal record.
At its core, the Epic Phoenix module supports every role involved in transplant care. Transplant coordinators use it to manage evaluations, documentation, and waitlist status. Surgeons and physicians rely on it to provide a comprehensive clinical picture across pre- and post-transplant care. Administrative teams use it to track compliance, reporting, and program performance. Everyone works from the same data, in real time.
What makes Epic Phoenix distinct is that it is not a bolt-on system. It is native to Epic. That means it shares the same Chronicles database, security model, and reporting infrastructure as the rest of the platform. Data entered in Epic Phoenix is immediately available to other Epic modules without re-entry or reconciliation. Lab results, medications, imaging, and specialty notes are automatically integrated into the transplant record.
The Epic Phoenix module also supports both sides of transplantation. Donor and recipient workflows are managed in parallel, with structured tools designed to track eligibility, evaluations, and outcomes for each. This dual-track capability is essential for programs managing living donors alongside recipients.
Importantly, Epic Phoenix is used across multiple organ programs within the same institution. Heart, kidney, liver, lung, and other transplant services can operate within one consistent framework while maintaining organ-specific requirements and reporting standards.
Epic Phoenix is the system transplant teams use to replace spreadsheets, external registries, and disconnected tools with one authoritative record.
II. Why Transplant Programs Need Epic Phoenix
Transplant programs do not fail because clinicians lack skill. They fail when systems cannot keep up with complexity.
Organ transplantation combines long timelines, dual patient tracks, and constant regulatory pressure. Standard EMR workflows were not designed for that reality. Epic Phoenix exists because transplant care breaks generic models.
A. The operational reality transplant leaders face
Most transplant programs struggle with the same structural issues:
- Parallel patient tracking
Donors and recipients must be evaluated, cleared, and monitored simultaneously without data bleeding between records. - High-risk data dependency
A single missing lab, outdated status, or undocumented assessment can delay a transplant or trigger compliance findings. - Continuous regulatory oversight
UNOS requires accurate, frequent reporting on waitlists, transplants, and outcomes. Manual reconciliation is not sustainable. - Longitudinal care complexity
Transplant care does not end at discharge; post-transplant monitoring, rejection surveillance, and medication adherence last for life.
Generic EMR tools treat these as edge cases. For transplant programs, they are the core workload.
B. Where Epic Phoenix changes the equation
The Epic Phoenix module addresses these pressures by design, not configuration.
It enables transplant teams to:
- Capture structured evaluation data that supports eligibility decisions
- Maintain real-time waitlist accuracy aligned with UNOS requirements
- Link all transplant-related encounters into a single episode of care
- Support long-term post-transplant management without external systems
Because Epic Phoenix is native to Epic, this work happens inside the same chart used by cardiology, oncology, pharmacy, and primary care. There is no parallel documentation and no manual syncing.
Key insight: Epic Phoenix reduces risk by reducing fragmentation.
Without a system like Epic Phoenix, transplant teams often rely on spreadsheets, legacy registries, or disconnected tools. That creates more work, not less, and introduces failure points precisely when precision matters most.
Transplant programs need Epic Phoenix because the cost of getting it wrong is too high.
III. Core Capabilities
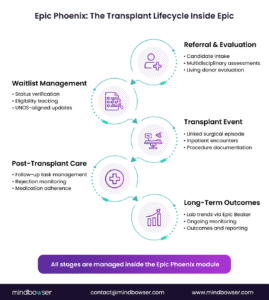
Epic Phoenix is organized around how transplant programs actually work, not how generic EMRs expect them to work. Its capabilities map directly to the transplant lifecycle, with purpose-built tools at each phase.
Below is how those capabilities show up in practice.
A. Pre-Transplant
The pre-transplant phase is where risk starts to accumulate. Eligibility decisions depend on complete, current, and well-organized data.
Epic Phoenix supports this phase by centralizing evaluation workflows and documentation.
Key capabilities include:
- Structured evaluation tracking
All required assessments, consults, and tests are captured in one place, reducing missed steps. - Multidisciplinary coordination
Inputs from surgery, medicine, social work, and finance are visible within the same record. - Donor and recipient alignment
Living donor workflows run in parallel with recipient evaluations without duplicating effort.
This structure helps teams move candidates through evaluation with fewer delays and clearer accountability.
B. Waitlist
Waitlist management is one of the most regulated aspects of transplant care, and one of the easiest places for errors to occur.
The Epic Phoenix module provides tools to:
- Maintain accurate waitlist status in real time
- Support verification and reconciliation processes
- Track changes in eligibility without losing historical context
Because the waitlist data lives in Epic, updates made by the care team are immediately reflected across reporting and compliance workflows.
C. Event
A transplant is not a single encounter. It is a sequence of tightly connected events.
Epic Phoenix links all transplant-related encounters into a unified episode of care. This includes:
- Surgical admission and procedure details
- Inpatient recovery
- Early post-operative follow-up
By grouping these encounters, teams can review the transplant as a single clinical narrative rather than a series of fragmented visits. That clarity supports both care delivery and outcome analysis.
D. Post-Transplant
Post-transplant care is where long-term success is determined.
Epic Phoenix is particularly strong in this phase, offering tools for:
- Follow-up task management to ensure appointments and labs are completed
- Rejection monitoring through structured documentation and alerts
- Medication management for complex immunosuppressive regimens
Medication adherence is a known risk factor for graft failure. Built-in reminders and monitoring tools help teams intervene earlier rather than later.
E. Lab and Beaker Integration
Lab data drives transplant decisions. Delays or missed results carry real consequences.
Epic Phoenix integrates directly with Epic Beaker to enable:
- Real-time lab result visibility
- Centralized order management
- Faster clinical interpretation across teams
Clinicians do not need to leave the transplant workflow to find critical lab data. It is already there.
F. Reporting
Reporting is not an afterthought in transplant programs. It is continuous.
Epic Phoenix supports:
- Clinical and operational dashboards through Radar
- Registry and regulatory reporting
- Internal performance analysis across organ programs
Because reporting draws from structured, real-time data, teams spend less time validating numbers and more time acting on them.
Epic Phoenix mirrors the transplant lifecycle, giving teams the right tools at the exact point they are needed.
We Improved Predictive Accuracy in Childbirth with Advanced EHR Integration
IV. Epic Ecosystem Fit
Transplant programs do not operate in isolation. Patients move across specialties, settings, and care teams. Epic Phoenix is designed to operate within a broader clinical ecosystem, not as a standalone transplant tool.
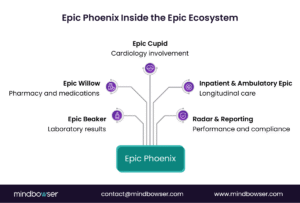
A. Native to the Epic Platform
Epic Phoenix is built on the same Epic foundation as every other clinical module. This matters operationally and clinically.
- Shared data model
Phoenix uses the same Chronicles database as the rest of Epic, eliminating duplicate records and manual reconciliation. - Unified security and access controls
Role-based access, auditing, and compliance policies apply consistently across transplant and non-transplant workflows. - Single patient chart
Transplant data resides within the longitudinal Epic record rather than in a separate system.
This native architecture enables transplant information to remain accurate as patients move through the health system.
B. Cross-Specialty Connectivity
Transplant patients are medically complex by definition. Their care regularly spans multiple specialties.
Epic Phoenix connects directly with other Epic modules, including:
- Epic Beaker for transplant-specific lab workflows
- Epic Willow for pharmacy and immunosuppressive medication management
- Epic Cupid for cardiology involvement in transplant candidates
- Primary care and inpatient modules for longitudinal care coordination
Because these modules share data in real time, specialists see the transplant context without additional documentation steps.
C. Relationship to Epic Beacon
Within the Epic ecosystem, Epic Phoenix and Epic Beacon share a common design philosophy across different clinical domains.
- Both support high-risk, protocol-driven care
- Both manage longitudinal patient journeys
- Both replace external, specialty-specific systems
The distinction is purpose. Epic Phoenix is centered on organs, donors, recipients, and regulatory reporting. Epic Beacon is centered on oncology treatment plans and chemotherapy delivery.
This parallel design enables organizations running both transplant and oncology programs to standardize the documentation and management of complex care across departments.
D. Operational Impact of Ecosystem Fit
When Epic Phoenix is fully integrated into the Epic environment, transplant programs gain:
- Fewer handoffs between systems
- Better visibility for non-transplant clinicians
- Cleaner reporting and analytics
- Reduced documentation burden for transplant teams
The ecosystem fit is not a technical detail. It is what makes Phoenix sustainable at scale.
Epic Phoenix works because it works with Epic, not alongside it.
V. Epic Phoenix vs Epic Beacon
Epic built both Epic Phoenix and Epic Beacon for the same reason: some clinical programs are too complex, too regulated, and too high-risk for generic EMR workflows. The similarity often confuses. The differences matter.
A. How They Are Related
At a platform level, Epic Phoenix and Epic Beacon share the same DNA.
- Same Epic foundation
Both modules run on Epic’s core platform and use the same underlying database and reporting stack. - Specialty-specific design
Each module replaces external, niche systems with workflows designed by and for specialty clinicians. - Longitudinal care focus
Both support care journeys that span months or years, not single encounters.
This shared foundation is why health systems often evaluate them side by side.
B. Where Epic Phoenix and Epic Beacon Diverge
| Feature | Epic Phoenix | Epic Beacon |
| Primary focus | Organ transplant management | Oncology and chemotherapy |
| Core patient groups | Donors and transplant recipients | Adult and pediatric oncology patients |
| Workflow anchor | Organs, waitlists, transplant episodes | Treatment plans and chemotherapy regimens |
| Visit structure | Linked transplant episodes | Series Visit Types |
| Regulatory reporting | UNOS and transplant registries | National cancer registries |
C. Key Similarities in Practice
Despite serving different clinical domains, the modules behave similarly in daily operations.
- Protocol-driven workflows
Phoenix manages immunosuppression and rejection monitoring. Beacon manages chemotherapy protocols. - Medication complexity
Both place heavy emphasis on safe medication ordering, scheduling, and adherence. - Structured documentation
Each replaces free-text and external tools with structured, reportable data.
This is why organizations that run both transplant and oncology programs often standardize governance and training across the two.
D. Core Differences That Matter
The divergence appears once workflows begin.
- Clinical model
- Epic Phoenix is organized around organs, donors, recipients, and waitlist status.
- Epic Beacon is organized around time-bound treatment regimens.
- External dependencies
Phoenix integrates directly with UNOS and transplant registries. Beacon focuses on oncology staging and cancer registry reporting. - Lifecycle length
Transplant care is lifelong. Oncology care is episodic, even when extended.
These differences drive configuration, staffing, and reporting decisions.
E. When to Use Each Module
Choosing incorrectly creates friction fast.
- Use Epic Phoenix when managing:
- Organ transplant evaluations
- Living and deceased donors
- Waitlists and transplant episodes
- Long-term post-transplant care
- Use Epic Beacon when managing:
- Chemotherapy and radiation workflows
- Oncology treatment planning
- Cancer staging and registry reporting
They solve different problems, even though they look similar from the outside.
Epic Phoenix and Epic Beacon are siblings, not substitutes.
VI. Implementation Considerations
Implementing Epic Phoenix is not a routine module rollout. It is a program-level transformation that touches clinical workflows, regulatory processes, and daily operations across transplant services.
Programs that treat it like a standard Epic install struggle. Programs that plan deliberately do well.
A. Training and Change Management
Transplant workflows are specialized, and so is the training required to support them.
- Role-based education
Training must be tailored for coordinators, surgeons, physicians, nurses, and administrative staff. Each role interacts with the Epic Phoenix module differently. - Multiple learning formats
Successful programs use a mix of eLearning modules, written guides, and short videos to reinforce key workflows. - Extended ramp-up period
Transplant teams often need additional time after training to build confidence, especially with waitlist and UNOS-related tasks.
Training is not a one-time event. It is an ongoing investment.
B. Data Conversion and Legacy Systems
Most transplant programs bring years or decades of legacy data into Epic Phoenix.
- Historical transplant records
Prior transplants, outcomes, and follow-up data often live in legacy systems or homegrown databases. - Selective conversion strategy
Programs must determine which data should be converted, which can be archived, and which should remain read-only. - Validation and reconciliation
Converted data must be validated carefully to avoid introducing errors into active transplant workflows.
The University of Nebraska Medical Center adopted this approach when migrating data from its long-standing OTTR platform to Epic Phoenix.
C. Go-Live Support Model
Go-live is where theoretical readiness meets real-world pressure.
- Command center support
Many organizations establish command centers staffed with Epic and transplant subject-matter experts. - At-the-elbow assistance
Immediate support during live workflows helps prevent workarounds from forming. - Rapid issue resolution
Early identification and correction of workflow gaps builds clinician trust in the system.
This support window is critical for long-term adoption.
D. Stakeholder Engagement
Transplant programs are deeply multidisciplinary. Implementation fails without broad ownership.
- Clinical leadership involvement
Surgeons and medical directors must be involved early to validate workflows. - Coordinator input
Coordinators often feel the operational impact first and should help shape the configuration. - Administrative alignment
Reporting, compliance, and registry requirements must be addressed up front.
When these groups align, Epic Phoenix becomes a shared asset instead of an imposed tool.
Epic Phoenix implementations succeed when transplant teams are treated as partners, not end users.
Build a Custom EHR with Epic Integration Capabilities
VII. Mindbowser Benefits
Epic Phoenix provides transplant programs with a platform. Mindbowser makes it work the way transplant teams actually operate.
This is not about a generic configuration. It is about reducing operational risk, protecting compliance, and removing friction from day-to-day transplant work.
A. Transplant-First Workflow Design
Transplant programs are not interchangeable. Organ mix, volume, and regulatory nuance vary by center.
Mindbowser designs Epic Phoenix workflows based on how your teams operate in practice.
- Coordinator-centered workflows
We map evaluation, waitlist, and follow-up tasks to real coordinator responsibilities, not abstract system steps. - Organ-specific logic
Kidney, liver, heart, and lung programs often operate differently. We account for those differences without breaking standardization. - End-to-end lifecycle alignment
From referral intake through lifelong post-transplant monitoring, workflows remain connected.
The result is fewer workarounds and higher adoption.
B. UNOS and Regulatory Alignment by Design
Compliance is not optional in transplant care. It must be embedded.
Mindbowser helps ensure the Epic Phoenix module is structured to support:
- Accurate waitlist data capture aligned with UNOS requirements
- Consistent status updates that reduce manual reconciliation
- Audit-ready documentation for internal and external reviews
By designing workflows with reporting in mind, programs avoid retrofitting compliance after go-live.
C. Integrated Clinical and Operational Data
Transplant leaders need more than documentation. They need visibility.
Mindbowser enables:
- Clean data flow between Epic Phoenix, labs, pharmacy, and specialty modules
- Reliable reporting inputs for dashboards and registries
- Reduced duplicate entries across transplant and non-transplant teams
This strengthens both clinical decision-making and program management.
D. Speed Without Sacrificing Control
Transplant programs cannot afford prolonged disruption.
Mindbowser applies proven delivery accelerators to:
- Shorten configuration cycles
- Reduce rework during validation
- Support smoother go-lives
At the same time, clients retain full ownership of their Epic build decisions and intellectual property.
Mindbowser helps transplant programs get the full value of Epic Phoenix without adding complexity.
VIII. Real-World Adoption
Epic Phoenix is not theoretical. It is already embedded in how major transplant centers operate today.
One of the clearest examples comes from an academic medical center with high transplant volume and long institutional memory.
A. University of Nebraska Medical Center (UNMC)
In 2019, the University of Nebraska Medical Center transitioned its transplant program from the legacy OTTR (Organ Transplant Tracking Record) platform to Epic Phoenix.
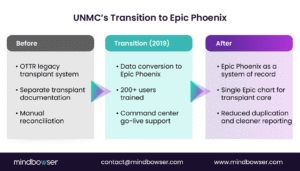
This was not a minor upgrade. OTTR had been in use since the 1990sand supported decades of transplant activity.
Key outcomes from the transition included:
- Single system documentation
Transplant teams no longer document in both Epic and a separate transplant system. All transplant workflows have been migrated to the Epic environment. - Large-scale user adoption
More than 200 users across transplant services were trained on the Epic Phoenix module. - Structured go-live support
A command center model was used to provide immediate support during early adoption.
The result was a measurable reduction in duplicate work and improved confidence in data accuracy across transplant teams.
B. National Footprint and Maturity
By the time UNMC implemented Epic Phoenix, it was estimated that roughly 50 percent of transplant programs in the United States were already documenting transplants in Epic Phoenix.
This level of adoption signals maturity.
- Phoenix is no longer an early-stage specialty module
- Best practices are shared across institutions
- Peer-driven configuration continues to refine workflows
For transplant leaders, this matters. It means lessons learned elsewhere can be applied locally instead of starting from scratch.
C. What Adoption Teaches Transplant Leaders
Real-world adoption highlights a consistent pattern:
- Programs gain efficiency when transplant workflows live inside Epic
- Data quality improves when structured documentation replaces external tools
- Clinician trust increases when reporting aligns with daily workflows
Epic Phoenix succeeds when it is treated as the transplant system of record, not just another module.
Epic Phoenix has moved from pilot to platform for transplant programs nationwide.
IX. Future Direction
Transplant medicine does not stand still, and neither does Epic Phoenix. As transplant volumes grow and regulatory expectations increase, the platform is evolving to support faster decisions, better coordination, and broader visibility.
A. Referral and Network Visibility
One of the emerging focus areas for Epic Phoenix is referral management.
- Earlier referral tracking
Tools such as Epic’s PatientStatus are designed to help transplant centers manage inbound referrals more effectively. - Bidirectional communication
Referring providers, both Epic and non-Epic, can receive patient status updates without manual outreach. - Reduced referral leakage
Better visibility helps programs identify stalled evaluations and intervene sooner.
For transplant directors, this translates into stronger relationships with referring networks and more predictable intake.
B. Real-Time and Predictive Analytics
Data volume in transplant care is enormous. The next step is using it more effectively.
- Near real-time performance monitoring
Expanded Radar dashboards will allow programs to track activity, outcomes, and bottlenecks as they emerge. - Decision-support potential
As analytics mature, Phoenix is expected to support more proactive clinical insights around transplant readiness and post-transplant risk. - Operational forecasting
Better data aggregation supports staffing, scheduling, and capacity planning.
The emphasis is not on abstract analytics. It is on usable signals embedded in daily workflows.
C. Deeper Ecosystem Integration
Future development continues Epic’s broader strategy of tighter module integration.
- Smoother cross-specialty data access
Transplant data will become even more visible to cardiology, oncology, pharmacy, and primary care teams. - Fewer context switches
Clinicians will spend less time navigating between tools and more time acting on information. - Cleaner longitudinal records
The transplant journey will remain intact across years of care.
The future of Epic Phoenix is about making complex transplant data easier to act on, not harder to manage.

Epic Phoenix in Practice
Transplant medicine demands systems that can carry clinical, operational, and regulatory weight without slowing teams down. Epic Phoenix meets that demand by embedding transplant-specific workflows directly into the Epic ecosystem, rather than forcing programs to manage parallel tools or workarounds.
Across the transplant lifecycle, Epic Phoenix supports how care is actually delivered—donor and recipient workflows run in parallel. Waitlist status, transplant events, and long-term follow-up remain connected. Regulatory requirements, such as UNOS reporting, are integrated into daily workflows rather than bolted on after the fact.
What strengthens Phoenix further is where it lives. Because it is native to Epic, transplant data flows naturally to labs, pharmacy, cardiology, oncology, and primary care. Clinicians outside the transplant team see the full context of a patient’s history, not fragments. In this environment, Epic Phoenix and Epic Beacon reflect the same design philosophy applied to different specialties: complex care needs purpose-built tools.
For transplant leaders, the conclusion is straightforward. Fragmented systems increase risk. Unified, longitudinal records reduce it. Epic Phoenix has become the transplant system of record for a growing share of programs because it aligns technology with the realities of transplant care, not the other way around.
UNOS does not legally mandate Epic Phoenix, but it is increasingly considered the operational standard for Epic-based transplant programs. Because the Epic Phoenix module supports structured waitlist management, UNOS-aligned data capture, and transplant episode tracking, many programs adopt it to reduce compliance risk and manual reporting effort.
Yes. Epic Phoenix is designed to support multiple organ programs simultaneously, such as kidney, liver, heart, and lung, within the same Epic instance. Each program can maintain organ-specific workflows and requirements while sharing a consistent data model and reporting framework.
The Epic Phoenix module provides a structured foundation, but real-world success depends on workflow configuration and governance. Programs can tailor evaluation steps, task routing, reporting views, and follow-up processes to match how coordinators and clinicians actually work, while still maintaining regulatory alignment.
In most cases, yes. Epic Phoenix is designed to replace external transplant-tracking tools, spreadsheets, and legacy systems by serving as the single system of record for transplant care within Epic. Some programs may retain a limited set of external tools during transition periods, but long-term duplication is typically eliminated.
Epic Phoenix supports accreditation and audit readiness by maintaining structured, longitudinal transplant documentation within the Epic chart. Because evaluations, waitlist changes, transplant events, and follow-up activities are all traceable, programs can respond to audits with less manual evidence gathering.
































