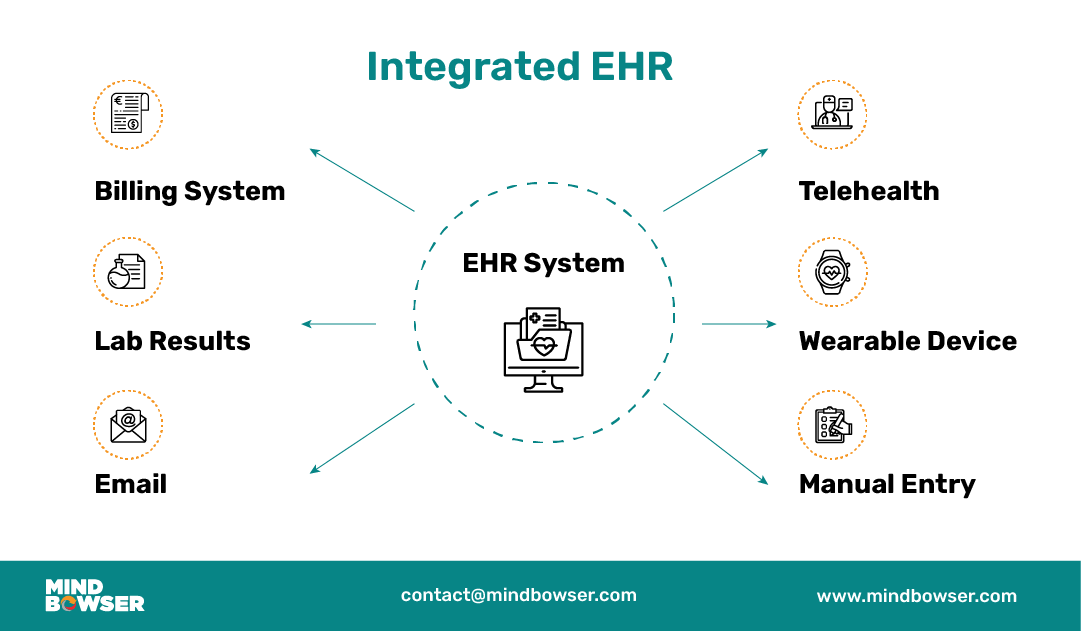
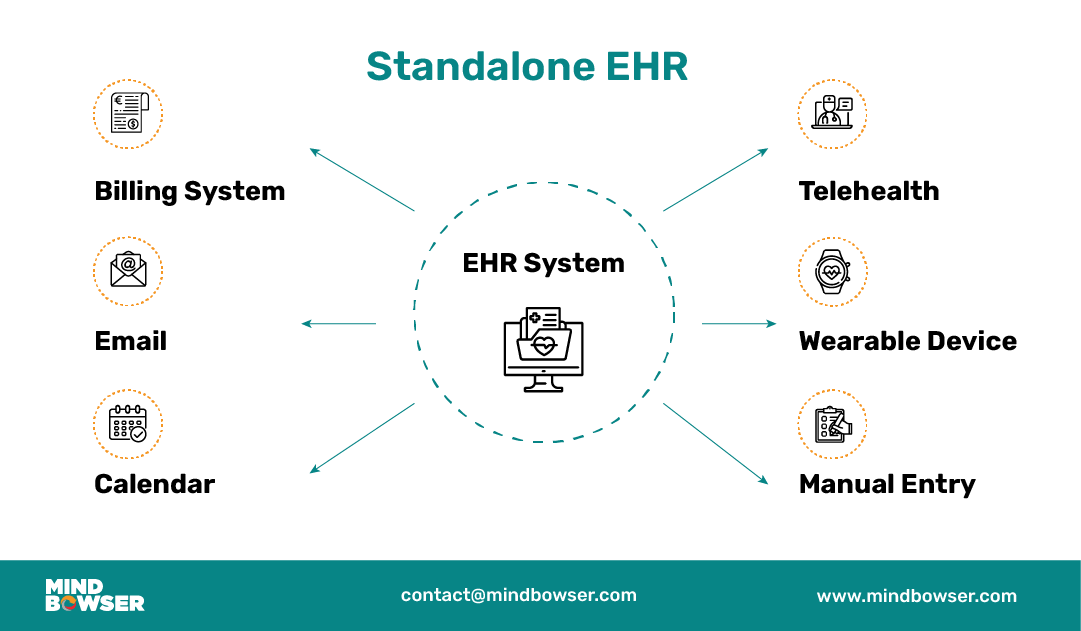
For mid-sized hospitals, the gap becomes clear when evaluating operational efficiency. Integrated EHRs simplify the handoff between front-desk scheduling, medical documentation, and claims management. Standalone systems, on the other hand, create stopgaps that affect everything from staff productivity to billing timelines.
IV. Pros and Cons of Standalone EHR
Standalone EHRs can make sense in certain settings, but the benefits come with trade-offs. For clinics or specialty providers with minimal integration needs, they offer simplicity. For growing systems, they can quickly become a bottleneck.
A. Pros OF Standalone EHR:
- Low setup barrier – Ideal for smaller practices with limited workflows.
- Minimal training curve – Staff can get up and running quickly with fewer modules to learn.
- Cost-efficient in the short term – Initial investment is often lower than that of integrated systems.
B. Cons of Standalone EHR:
- Lacks interoperability – Doesn’t connect well with billing platforms, patient portals, or remote monitoring tools.
- Manual workflows – Limits automation for claims, reminders, and data syncing.
- Restricted growth – Adding capabilities like telehealth or AI-driven scheduling often requires third-party workarounds.
- Patient experience suffers due to a lack of real-time access to a comprehensive care history and cross-departmental visibility.
As more care shifts toward continuity, digital engagement, and proactive intervention, the downsides of standalone systems become increasingly difficult to overlook.
V. Custom EHR: The Third Option
While integrated EHRs are ideal for many hospitals, a custom EHR offers a unique balance of flexibility and functionality, especially for mid-sized hospitals with complex workflows. Unlike standalone systems, custom EHRs allow hospitals to design a solution that fits their specific needs while still benefiting from some level of integration. Whether you’re incorporating specialized features like telemedicine integration or advanced AI-driven diagnostics, a custom EHR can be tailored for your unique patient care goals.
Custom EHRs provide the ability to build exactly what’s needed, avoiding unnecessary modules or restrictions. However, they come with their own challenges, especially around development time, upfront costs, and the need for ongoing maintenance. But for hospitals that need specialized features or are integrating with proprietary systems, a custom EHR might be the perfect middle ground between the simplicity of a standalone and the depth of an integrated system.
Looking to Build Your Own Custom Integrated EHR?
VI. Pros and Cons of Integrated EHR
Integrated EHRs aren’t just about connecting systems, they’re about improving how care is delivered, documented, and reimbursed. For mid-sized hospitals, they set the foundation for scale, compliance, and smarter operations.
A. Pros of Integrated EHR:
- Unified patient records – Everyone sees the same up-to-date information, reducing duplication and medical errors.
- Supports modern care models – Enables telehealth, remote patient monitoring, and automated care planning.
- AI-ready infrastructure –Built to connect with workflows like EduCare AI for patient education and DischargeFollow AI for post-discharge follow-ups; no custom setup needed.
- Streamlines communication – Smoother coordination between the front office, nursing, physicians, and billing staff.
B. Cons of Integrated EHR:
- Higher upfront investment – More robust functionality requires a larger initial investment in implementation and integration.
- Requires planning and change management – Shifting workflows and retraining staff takes time and buy-in.
- Vendor coordination, especially when third-party platforms or legacy systems are involved.
Still, for organizations preparing for risk-based contracts, hospital-at-home models, or multi-location growth, integrated EHRs offer a much stronger return over time.
Related Read: Benefits and Challenges of The Electronic Health Record
VII. When to Choose an Integrated EHR Over a Standalone?
If your organization is looking beyond basic documentation and into coordinated, patient-centered care, an integrated EHR isn’t optional; it’s foundational.
Here are clear indicators it’s time to move beyond a standalone system:
A. You’re expanding across multiple sites or service lines
Integrated EHRs ensure a unified view of patient data across departments, specialties, and locations, reducing duplication and improving handoffs.
B. You’re launching telehealth or remote patient monitoring programs
Integrated platforms can capture real-time vitals, sync them with the clinical record, and make that data actionable for care teams.
C. Your care models rely on data-driven insights
Whether it’s hospitalization risk, care plan optimization, or early warning systems, integrated infrastructure allows clinical teams to act on complete patient profiles.
D. You’re focused on patient experience
Integrated systems enable the delivery of appointment reminders, secure messaging, education, and self-service portals as part of a connected journey, rather than fragmented touchpoints.
Standalone EHRs can’t carry this weight. For organizations aligning with value-based care, payer collaboration, or scaling digital offerings, integrated systems make these efforts possible and sustainable.
VIII. How Mindbowser Can Help You with EHR Integration?
At Mindbowser, we’ve supported hospitals in transitioning from fragmented systems to fully integrated, interoperable infrastructures; without disrupting operations or blowing timelines.
Here’s how we help make that transition smoother:
- EHR and wearable integrations at scale
We’ve successfully integrated with over 20 major EHR platforms, including Epic EHR, Cerner EHR, and Athenahealth EHR, as well as more than 100 medical devices and wearables. Our clients don’t just get APIs; they get a roadmap for compliance and continuity. - FHIR-first, SMART-ready development
Whether you’re building a custom module or embedding a SMART on FHIR app, our team brings hands-on experience. We’ve delivered workflows, such as AI Medical Summary and Cardiovascular Risk Prediction, that run seamlessly within native EHR environments. - Built-in compliance
Security isn’t an afterthought. With infrastructure powered by PHISecure, a workflow for built-in compliance, we ensure HIPAA and SOC 2 standards are met across all endpoints. - Digital front door enablers
We help providers simplify scheduling, chat, and outreach by using workflows like Appointly and ChatIQ, built to run inside existing EHR workflows, not around them.
Whether you’re rebuilding your digital infrastructure or incrementally integrating one system at a time, we align with your roadmap and regulatory environment, not just the tech stack.
Looking to upgrade from a siloed system to a smarter, integrated EHR?
Let’s talk about building the right foundation for your care delivery goals.
Conclusion
Integrated EHRs are no longer a luxury; they’re a prerequisite for delivering coordinated, efficient, and data-informed care. While standalone systems may offer a quick fix, they often fall short of meeting modern clinical needs, regulatory demands, and patient expectations.
For mid-sized hospitals scaling fast, the ability to connect systems, automate workflows, and surface meaningful insights from patient data is critical. Integrated EHRs lay the foundation for that transformation.
At Mindbowser, we don’t just integrate systems; we help organizations build future-ready infrastructure. Whether you’re focused on RPM, telehealth, or AI-driven care, we align your tech with your long-term goals.
An integrated EHR brings together clinical, billing, lab, imaging, and external data sources, providing a real-time, unified view of the patient across the care continuum.
The main types include:
- Standalone EHR – Operates in isolation, without external connectivity
- Integrated EHR – Connects multiple systems and departments
- Cloud-based EHR – Hosted off-premise with access over the internet, can be standalone or integrated
It’s an electronic patient record system that aggregates data across platforms, enabling clinicians, administrators, and care teams to access a shared, up-to-date record from anywhere in the care journey.




















 BLOGS
BLOGS  NEWSROOM
NEWSROOM  CASE STUDIES
CASE STUDIES  WEBINARS
WEBINARS  PODCASTS
PODCASTS  ASSET HUB
ASSET HUB  EVENT CALENDAR
EVENT CALENDAR