TLDR;
EHR integration is a non-negotiable strategic mandate. This guide details how robust EHRs drive ROI by enhancing patient safety (via CDSS), eliminating costly administrative waste, and mitigating technical risks through mandatory adoption of modern standards like FHIR.
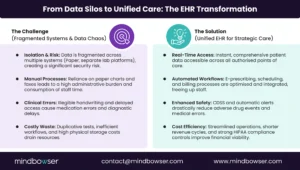
Electronic Health Records (EHR) are the cornerstone of modern care, representing a definitive shift from the fragmented, costly paper systems of the past.
Looking for EHR Software Development Services?
IV. The Definitive Benefits of Adopting EHR Solutions

A. Core Clinical and Patient Safety Gains (The Quality Mandate)
- Enhanced Diagnostic Accuracy via CDSS: Systems include Clinical Decision Support Systems (CDSS) and provide alerts for potential drug interactions and allergies, significantly reducing medical errors. These essential capabilities define the core EHR benefits to patients by establishing a proactive clinical safety net.
- Reduced Medical Errors: The system acts as a crucial safety net. It automatically scans for potential dangers, such as drug-drug interactions, allergies, and dosing errors, leading to a marked decrease in medication mistakes and adverse events.
- Superior Care Coordination: EHRs enable secure, real-time sharing of comprehensive patient data (medications, lab results, discharge summaries) among all authorised providers, minimising care gaps and reducing the need for duplicative testing.
- Improved Patient Outcomes: By supporting evidence-based practices and providing easy access to treatment history, EHRs enable clinicians to monitor progress and initiate timely interventions, leading to faster treatments and reduced complications.
B. Operational Efficiency and Financial ROI (The Business Case)
- Streamlined Revenue Cycle Management (RCM): Integrated EHRs automate insurance verification, prior authorizations, and claim submission. This reduces manual entry errors, a leading cause of claim denials, and accelerates the payment cycle.
- Reduced Administrative Burden: EHRs automate tasks like scheduling, billing, and documentation, streamlining workflows and improving productivity. These operational advantages are among the most immediate and tangible EHR system benefits, as they significantly reduce time spent on manual processes. EHR adoption correlates with massive administrative efficiency gains.
- Strategic Validation: EHR vs. Paper: EHRs offer robust digital security, encryption, and comprehensive audit logs that are mandatory for HIPAA compliance, providing a level of data protection and accountability that physical records cannot match.
- Boosted Patient Engagement: Patient portals provide secure access to records, lab results, and communication tools, empowering patients to participate actively in their own care and increasing compliance. This direct digital access is a cornerstone of realising EHR benefits to patients.
EHRs automate tasks like scheduling, billing, and documentation, streamlining workflows and improving productivity.
These functional advantages define the core EHR system benefits that accelerate organisational efficiency.
V. Strategic Hurdles to EHR Success: Technical and Operational Challenges
The full value of the EHR is only realised by proactively mitigating the top implementation pitfalls and operational friction points.
A. Key Technical and Operational Hurdles
| Challenge | Impact on Strategy | Mitigation Strategy |
| Workflow Disruption & Usability | Implementation causes temporary productivity losses due to complex interfaces and excessive documentation time, leading to physician burnout. | Customisation and UI/UX improvements are crucial to ensure the system is easy to navigate. |
| High Costs & Time Investment | High upfront costs for software, hardware, and ongoing maintenance. Transferring data from existing systems can be time-consuming. | Focus on pre-built accelerators to reduce bespoke development expenses and justify long-term cost savings. |
| Interoperability & Data Standards | Data remains fragmented across vendor systems, limiting seamless information sharing. | Mandate FHIR adoption and use robust data-mapping tools to achieve semantic interoperability. |
| Security Risk & Downtime | EHRs are targets for cyberattacks. System downtime or power outages can render critical patient information inaccessible. | Requires robust security measures, data backups, and strict role-based access controls (in compliance with HIPAA). |
The legacy challenge is acute when dealing with specialised platforms. See how to overcome this by addressing Epic Integration and Legacy Data Systems.
B. Practical Interoperability Challenges in Real Deployments
Interoperability sounds straightforward until the first deployment. FHIR resources vary widely across vendors, versions, and even environments. HL7 SIU and ADT segments behave differently depending on configuration, forcing teams to build and maintain ACK logic for each partner.
Mapping drift appears when non-production and production systems don’t match field names, IDs, or routing rules.
In practice, live integrations depend on TCP/MLLP transport, VPN tunnels, endpoint whitelisting, and ongoing monitoring. These are not theoretical hurdles; they are the daily friction points that slow project timelines and demand continuous technical oversight.
C. Why Scheduling Automation Fails Without Bidirectional EHR Integration
Scheduling automation breaks down when the surrounding systems cannot read and write updates to the EHR. Many workflows start with CSV files to handle appointment verification, reminders, and post-discharge follow-ups. Those files are snapshots, not a live feed. Delays create errors, and small volumes expose the limits quickly.
True automation requires SIU/ADT write-back so confirmations, cancellations, and reschedules appear correctly inside the EHR. Without that bidirectional flow, staff face conflicting schedules, patients receive inconsistent communication, and leaders cannot rely on the data to guide throughput decisions. Reliable scheduling automation depends on an always-current EHR record.
VI. Powering Digital Health with EHR Use Cases
Integration is the engine that drives modern, patient-centric applications, ensuring functionality and maximising the ROI of your EHR.
- Remote Patient Monitoring (RPM): Integration ensures that real-time vitals, biometrics, and alerts are pushed to the EHR, enabling physicians to manage chronic conditions proactively.
- Telemedicine Platforms: Integration ensures providers can immediately pull complete patient medical histories and automatically document detailed encounter notes, guaranteeing compliance and continuity of care.
- Revenue Cycle Management: Financial efficiency is maximised through integration that automates billing by pulling clinical codes directly from the EHR for claims and real-time eligibility checks.
VII. HealthConnect CoPilot: Accelerating EHR Implementation ROI
For decision-makers focused on speed and cost-effectiveness, bespoke integration projects are often too slow, risky, and expensive. HealthConnect CoPilot is designed to eliminate these hurdles by leveraging advanced accelerators and domain expertise.
It shifts the integration process from costly, custom coding to efficient, standards-based configuration.
A. Quantifiable Cost Benefits for Decision-Makers
HealthConnect CoPilot offers unparalleled speed and cost control by leveraging pre-built accelerators and domain expertise:
- Cost Reduction: Reduces overall integration costs by up to 60%. This massive saving is achieved by using pre-certified, pre-built components rather than initiating extensive custom EHR development and mapping for every unique connection point.
- Development Speed: Slashes development time by 80%, allowing organisations to realise project benefits sooner and accelerate time-to-market. This rapid deployment minimises the implementation window and reduces the risk of project fatigue.
- Go-To-Market: Speeds up product deployment by 50%, ensuring new digital health initiatives can quickly capture market share and begin generating revenue sooner.
B. Key Features and Impact on Risk Mitigation
HealthConnect CoPilot provides a secure and compliant platform designed for seamless data synchronisation:
- Standardised APIs & FHIR Compliance: The platform mandates FHIR adoption and ensures instant compatibility with multiple healthcare applications by standardising data formats for consistency. This directly mitigates the risk of interoperability failure caused by legacy system incompatibility.
- Secure Data Exchange: Employs strong security measures, including end-to-end encryption and multi-factor authentication, to ensure strict HIPAA compliance for all patient data transactions. This proactively reduces exposure to security risks and the potential cost of data breaches.
- Expert Oversight: The platform is backed by Mindbowser’s specialised domain experts, who provide the strategic oversight necessary to navigate complex regulatory and technical landscapes. This guidance is essential for maximising the long-term benefits of the EHR system and ensuring your implementation remains on track.

Integrated EHRs provide complete, real-time patient histories, enabling automatic alerts for allergies, drug interactions, and contraindications. This reduces diagnostic errors and strengthens clinical decision support, delivering one of the most significant EHR benefits to patients.
EHRs automate scheduling, documentation, billing, claim validation, and information retrieval. Automation eliminates manual steps that delay workflows, allowing staff to refocus time on direct patient care.
EHRs standardise clinical data, track outcomes, and automate reporting capabilities essential for VBC success. Reliable documentation allows organisations to meet quality metrics and receive incentive-based reimbursements.
Interoperability ensures clinical data flows across providers, labs, imaging systems, and care teams. Without standards like FHIR, EHR benefits are diminished due to data silos, inconsistent formats, and incomplete patient records.
Common blockers include:
1. Variability in HL7 v2 messages
2. FHIR implementation differences across vendors
3. Mapping drift across environments
4. VPN and endpoint whitelisting
5. Smart-on-FHIR or OAuth key provisioning
6. HL7 ACK handling requirements
These hidden complexities were highlighted in real integration discussions.
CSV workflows emerge when EHR API access or credential approvals are still pending. They are often used for appointment reminders, post-discharge follow-ups, or patient engagement tasks.
However, CSV-based workflows cannot synchronise cancellations or updates with the EHR, causing accuracy and workflow issues.
Custom integrations (using tools like Mirth, Kafka, and custom microservices) often take three to six months per EHR.
Modern integration platforms can configure sandbox and production environments within days once credentials and workflows are defined.
Reliable integration ensures real-time vitals, biometrics, alerts, and encounter notes flow directly into the EHR.
For patient engagement platforms, integration enables automated reminders, post-discharge follow-ups, and scheduling updates, capabilities that are impossible without consistent read/write connectivity.
Integrated systems use encryption, audit logs, role-based access, and secure authorisation protocols such as OAuth 2.0. Eliminating fragmented paper records or manual transfers significantly reduces PHI exposure.
Key considerations include:
1. Time to market (custom: months; managed: days)
2. Engineering bandwidth and expertise (HL7, SIU/ADT, ACKs, Smart-on-FHIR)
3. Long-term maintenance and monitoring
4. Compliance requirements and disaster recovery
These were the central evaluation concerns raised by technology leaders in real integration conversations.
































