TL;DR
Epic FHIR APIs allow modern applications to access clinical data from the Epic EHR using the FHIR standard and SMART on FHIR authentication. However, Epic FHIR APIs are not plug-and-play. Each Epic EHR deployment determines which APIs, scopes, and write capabilities are available, so integrations require security approvals, a technical architecture, and coordination with each health system. In practice, implementing Epic FHIR APIs typically takes 3–6 months per organization, making governance, integration planning, and scalable architecture essential for digital health platforms.
“Is integrating with Epic as simple as connecting an API?”
Many organizations assume accessing data from the Epic EHR is a straightforward integration.
In reality, connecting applications to Epic requires more than technical API calls. Epic FHIR APIs enable digital health platforms, patient apps, analytics tools, and remote monitoring systems to securely retrieve clinical data using the FHIR standard and SMART on FHIR authentication.
However, these integrations are not plug-and-play. Each health system controls which APIs, scopes, and permissions are available, and onboarding often requires security reviews, governance approvals, and coordination with hospital IT teams.
For healthcare technology leaders, understanding how Epic FHIR APIs work in real-world deployments is essential for building scalable digital health platforms across multiple Epic environments.
I. What Are Epic FHIR APIs and How Do They Work?
Healthcare organizations increasingly rely on modern interoperability standards to allow applications to access data from the Epic EHR. Among these standards, Epic FHIR APIs have become the primary mechanism for enabling third-party applications to retrieve and exchange clinical information within Epic environments.
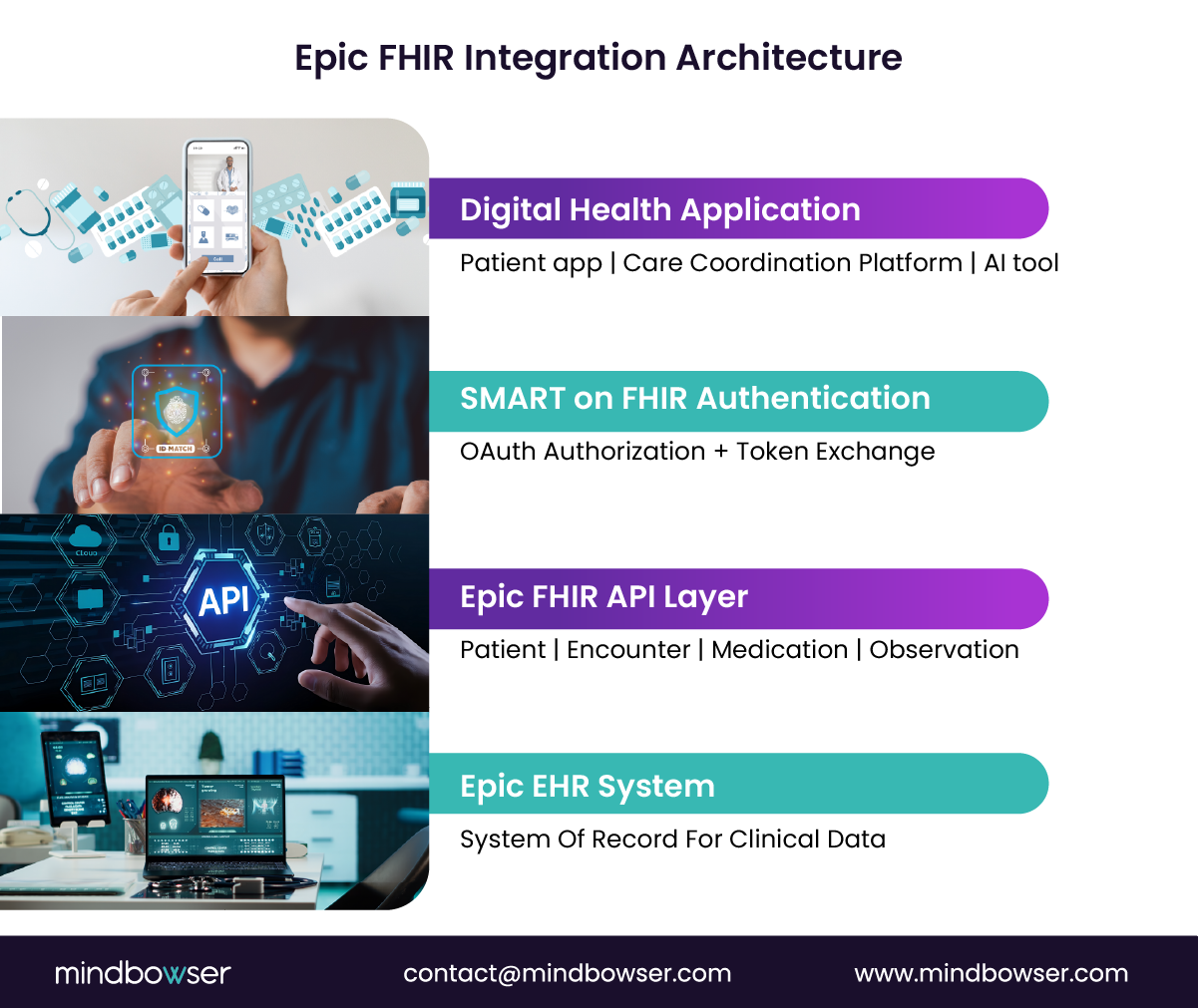
At a technical level, Epic FHIR APIs expose selected clinical resources from the Epic EHR using the HL7 Fast Healthcare Interoperability Resources (FHIR) specification. These APIs allow external applications to request structured healthcare data, including patient demographics, medications, allergies, encounters, conditions, and laboratory results.
Access is typically controlled using SMART on FHIR Epic authentication. This framework combines OAuth 2.0 authorization with FHIR data resources, allowing applications to securely request permission to access patient information stored in the Epic EHR.
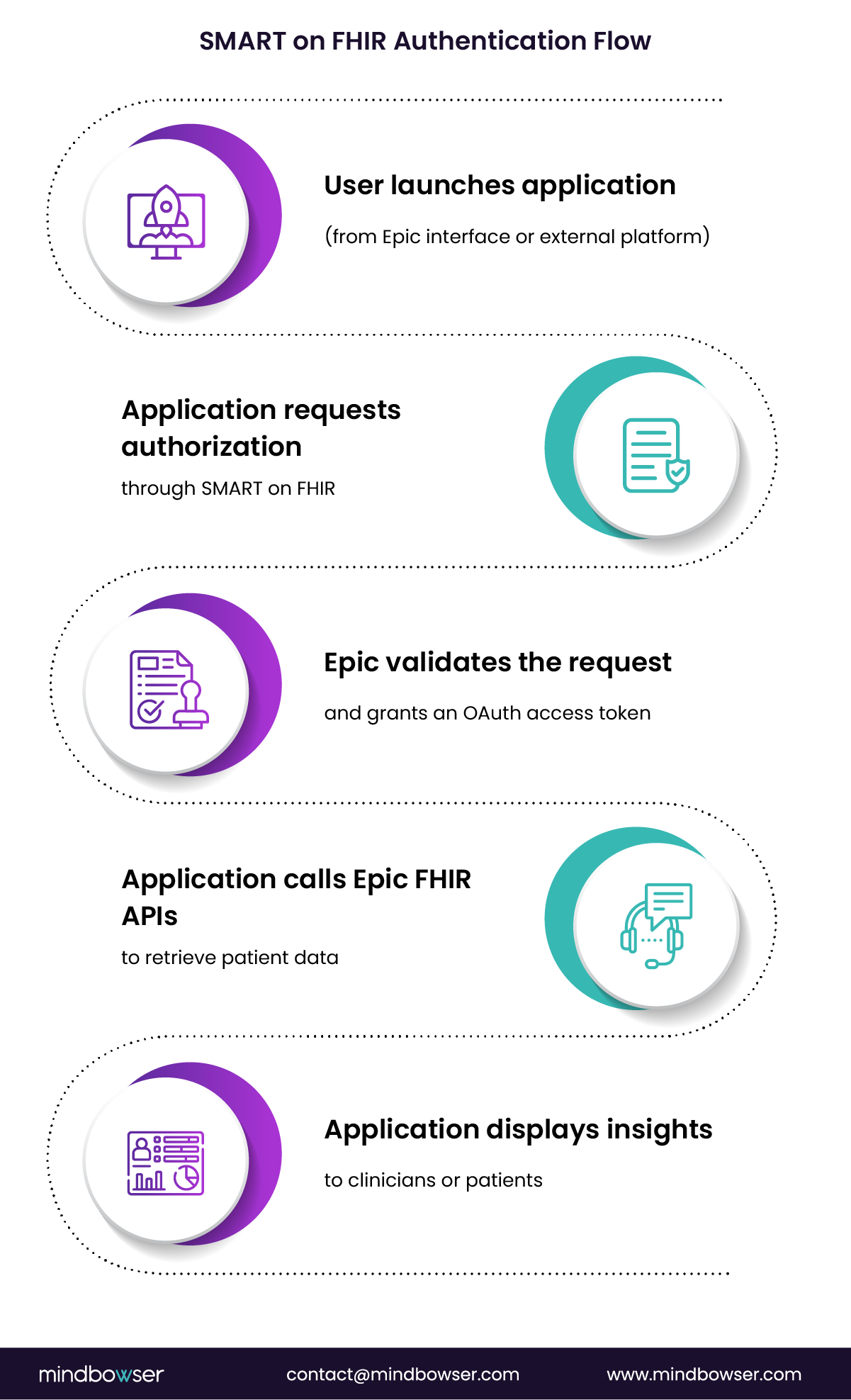
In practice, the workflow operates as follows:
- A user launches an application connected to an Epic environment
- The application requests authorization through SMART on FHIR
- Epic validates the request and grants a token based on approved scopes
- The application calls Epic FHIR APIs to retrieve clinical resources
This approach allows applications to integrate with the Epic EHR without requiring direct database access or proprietary interfaces. For many healthcare organizations, Epic FHIR APIs represent the most accessible path to enabling modern digital health capabilities.
However, the architecture is intentionally controlled and restricted. Epic exposes only specific resources and operations through its FHIR layer. Health systems deploying the Epic EHR also decide which Epic interoperability APIs are available to external vendors.
As a result, two hospitals running the same Epic EHR version may support different FHIR resources, scopes, or write capabilities.
This variability has important implications for platform architects. Teams building digital health applications must design integrations that can adapt to multiple configurations of the Epic EHR rather than assuming a uniform interface.
In most environments, Epic FHIR APIs support three primary integration patterns:
- Patient-facing applications accessing records through SMART authentication
- Provider workflow tools embedded inside the Epic EHR interface
- External care coordination platforms retrieving data from the Epic system
Because the Epic EHR remains the system of record for most clinical data, these integrations are usually read-focused. Write access via Epic FHIR APIs is available but often limited and must be explicitly enabled by the health system.
For healthcare technology leaders, the key takeaway is architectural. Epic FHIR APIs provide a standards-based interoperability layer, but they operate within governance controls defined by each Epic EHR deployment.
Understanding these constraints early is critical when designing scalable healthcare platforms.
Epic FHIR APIs enable standardized access to Epic clinical data, but successful integration depends on authentication models, site-specific API availability, and careful integration architecture.
II. Epic Integration Methods in the Epic Ecosystem
| Method | Best For | Limitations | When to Use |
|---|---|---|---|
| HL7 v2 | ADT feeds, batch data exchange | Legacy format | Backend workflows |
| FHIR APIs | Real-time application integration | Site variability | Modern digital health apps |
| Interconnect | Deep Epic workflows | Requires Epic build | Advanced enterprise integrations |
Healthcare organizations integrating with the Epic EHR rarely rely on a single interoperability method. Instead, Epic supports several integration mechanisms designed for different technical and operational use cases. Understanding these options is critical for platform architects designing scalable Epic EHR integration strategies.
Among these methods, Epic FHIR APIs serve as the modern interoperability layer for most digital health applications. They allow external systems to access structured clinical data in real time using the FHIR standard and SMART authentication. For patient applications, care coordination tools, and analytics platforms, Epic FHIR APIs are often the preferred approach because they align with modern API-based architecture.
However, Epic interoperability APIs are only one component of the broader Epic integration ecosystem.
Many hospitals still rely heavily on HL7 v2 messaging for operational workflows. Admission, discharge, and transfer (ADT) feeds are commonly delivered using HL7 interfaces that push updates from the Epic EHR to downstream systems such as billing platforms, data warehouses, and care management tools. While reliable, HL7 messages are event-driven rather than query-based, which limits their usefulness for real-time applications.
For deeper integrations, Epic provides Interconnect, a proprietary interface layer that allows applications to interact with advanced Epic EHR workflows. These integrations can support activities such as order placement, documentation workflows, and operational automation. However, Interconnect integrations typically require configuration and development within the Epic environment itself, making them more complex to deploy.
Because each integration method serves a different purpose, healthcare organizations often combine multiple approaches. A digital health platform may use Epic FHIR APIs for real-time access to patient data, HL7 feeds for operational events, and deeper Epic interfaces for workflow automation.
For CIOs and interoperability leaders, the key architectural decision is selecting the appropriate method based on application requirements and the capabilities available within each Epic EHR deployment.
Epic FHIR APIs enable modern application integration, but effective Epic interoperability strategies often combine APIs, HL7 messaging, and deeper Epic interface layers.
III. When Epic FHIR APIs Are the Right Integration Approach
For many digital health platforms, Epic FHIR APIs provide the most practical path to integrating with the Epic EHR. They enable secure, standards-based access to clinical data while allowing applications to operate outside the core Epic environment.
But the key architectural question for technology leaders is simple.
When are Epic FHIR APIs actually the right integration method?
In general, Epic FHIR APIs work best when applications need structured, real-time access to patient data without requiring big changes to Epic workflows.
Most modern healthcare applications fall into this category. Patient engagement platforms, care coordination tools, analytics dashboards, and clinical AI applications typically retrieve patient data from the Epic EHR to power their functionality.
These platforms usually require access to common FHIR resources, such as:
- Patient demographics
- Medication lists
- Allergies and conditions
- Encounters and care plans
- Laboratory results
Because Epic FHIR APIs expose these resources through standardized endpoints, they allow developers to build applications that can integrate with multiple Epic EHR deployments while maintaining a consistent application architecture.
Another major advantage is compatibility with SMART on FHIR Epic authentication. This framework allows applications to launch directly within the Epic EHR interface or operate as external applications authorized by the health system.
This model supports several common integration scenarios.
1. Patient-facing applications
Mobile apps that allow patients to access health records, schedule visits, or view care plans frequently rely on Epic FHIR APIs to retrieve data from the Epic EHR.
2. Clinical decision support tools
AI-driven platforms often analyze patient data from the Epic EHR to generate risk scores, recommendations, or alerts for clinicians.
3. Care coordination platforms
Population health and care management systems use Epic FHIR APIs to synchronize patient data across providers, specialists, and remote monitoring tools.
In each scenario, the application retrieves data from the Epic EHR, processes it externally, and presents insights to clinicians or patients.
The Epic system remains the system of record.
That architectural boundary is intentional. Epic allows applications to access data through Epic FHIR APIs, but the core clinical workflows and documentation processes remain controlled within the Epic EHR environment.
For CIOs and CTOs evaluating integration strategies, the takeaway is clear.
If your application needs reliable access to standardized patient data from the Epic EHR, Epic FHIR APIs are usually the correct starting point.
However, they are not the only integration method available, and they are not always sufficient for complex enterprise workflows.
IV. When Epic FHIR APIs Are Not Enough
While Epic FHIR APIs provide a powerful interoperability layer, they do not cover every integration scenario within the Epic EHR ecosystem. Healthcare technology leaders often discover this limitation during implementation rather than during architecture planning.
The reason is structural. Epic exposes selected clinical data through Epic interoperability APIs. Still, the full functionality of the Epic EHR remains tightly governed by workflow configuration, operational policies, and security controls set by each health system.
So the critical question becomes:
When do Epic FHIR APIs become insufficient for integration?
The answer typically appears in three situations.
A. Complex Clinical Workflow Integration
Many healthcare workflows occur entirely inside the Epic EHR. Order placement, documentation templates, and task routing are examples of processes that depend on internal Epic configuration.
In these cases, Epic FHIR APIs cannot directly trigger or modify workflows. Organizations may need deeper Epic interfaces or system-specific integration methods to interact with these processes.
B. High-Volume Transaction Processing
Some enterprise platforms require constant bidirectional data exchange with the Epic EHR. Examples include revenue cycle automation tools, scheduling platforms, and operational systems that process large volumes of updates.
Because rate limits and scope restrictions typically govern Epic FHIR APIs, they may not support high-frequency transactional workloads. Alternative integration models are often required.
C. Write Access to the Epic EHR
Read access through Epic FHIR APIs is common. Write access is not.
Many health systems restrict external applications’ ability to create or modify records within the Epic EHR. When write access is allowed, it often applies only to specific resources such as observations, questionnaires, or patient-generated data.
This creates an important architectural boundary. Epic allows applications to read broadly but write selectively.
For organizations building clinical platforms, this distinction can shape the entire system design. Applications may analyze data retrieved from the Epic EHR, generate insights, and then return recommendations to clinicians rather than automatically updating records.
In practice, this hybrid model is common across healthcare platforms that integrate with Epic FHIR APIs.
The lesson for CIOs and digital health leaders is straightforward. Epic FHIR APIs are the entry point to interoperability, but they are only one layer in the broader Epic integration architecture.
Understanding where APIs end, and deeper Epic workflows begin, is essential when planning enterprise integration strategies.
V. The Real Timeline for Epic FHIR Integrations
Many organizations assume that integrating with the Epic EHR using Epic FHIR APIs will follow a standard API deployment timeline. In reality, the technical build is often the fastest part of the process. The majority of time is spent on governance approvals, security validation, and onboarding procedures defined by each health system.

A useful rule for planning.
Expect 3–6 months to onboard each Epic EHR customer.
Even when the application already supports Epic FHIR APIs, every hospital or health system operates its own Epic environment and must approve external integrations individually.
This creates a multi-phase implementation process that involves both technical and operational workstreams.
Typical Epic FHIR Integration Timeline
| Phase | Key Activities | Typical Duration |
|---|---|---|
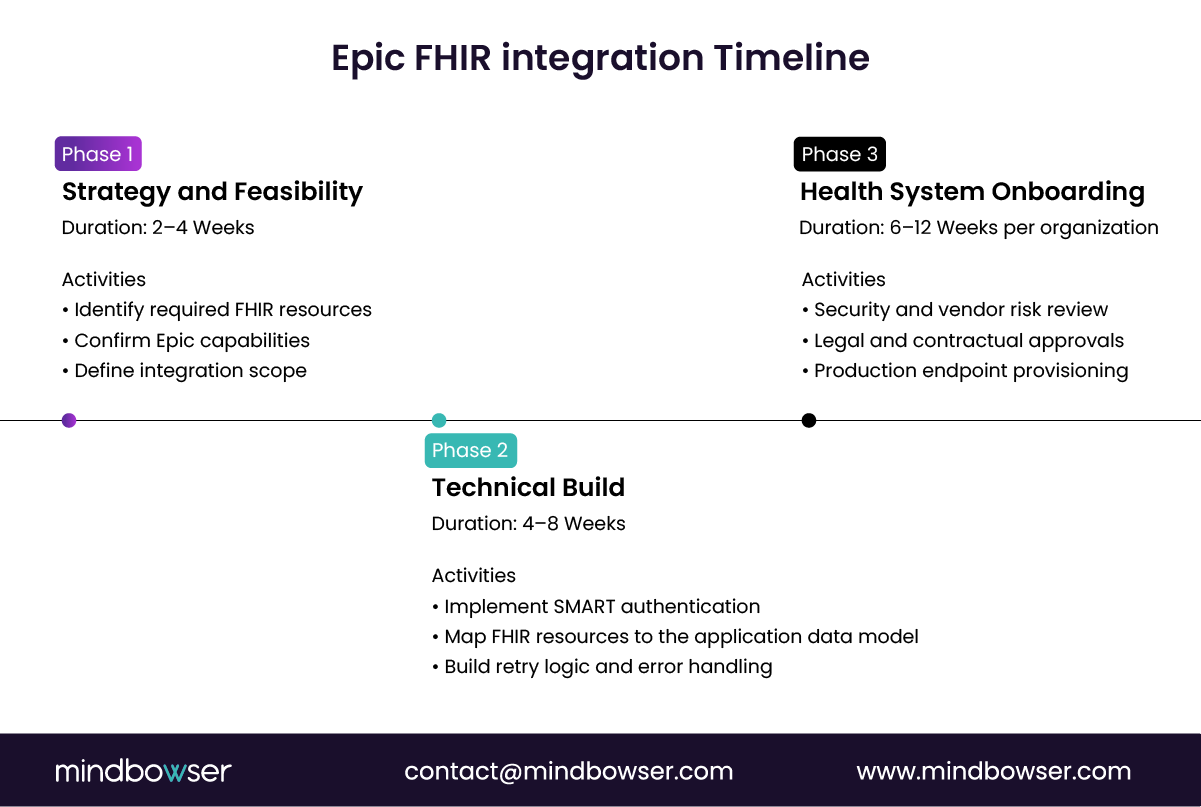
| Phase 1 – Strategy & Feasibility | Define data scope, identify supported resources, and validate write access | 2–4 weeks |
| Phase 2 – Technical Build | SMART auth setup, data mapping, error handling, retry logic | 4–8 weeks |
| Phase 3 – Health System Onboarding | Security review, contractual approvals, and endpoint provisioning | 6–12 weeks per site |
During Phase 1, integration teams evaluate which Epic FHIR APIs are available within the target Epic EHR environment. Resource availability can vary widely between health systems, so early validation prevents architecture issues later.
In Phase 2, engineering teams implement SMART on FHIR Epic authentication, configure API endpoints, and map FHIR resources into the application’s internal data model. This phase also includes error handling and performance optimization for production workloads.
Health systems running the Epic EHR typically require vendor security assessments, legal agreements, and technical validation before allowing applications to access Epic interoperability APIs. This review process often involves multiple departments, including IT security, compliance, interoperability teams, and clinical governance committees.
Every Epic customer is a separate integration project.
For organizations building platforms that serve multiple health systems, this operational reality becomes a key scaling challenge. Even if an application already supports Epic FHIR APIs, each new Epic EHR client requires its own approval process, endpoint configuration, and production validation.
Understanding this timeline helps CIOs and platform leaders plan integration programs more accurately and allocate the resources required for long-term interoperability success.
Looking to Build a Custom EHR with Epic Integration Capabilities?
VI. Designing Scalable Epic FHIR Integration Architecture
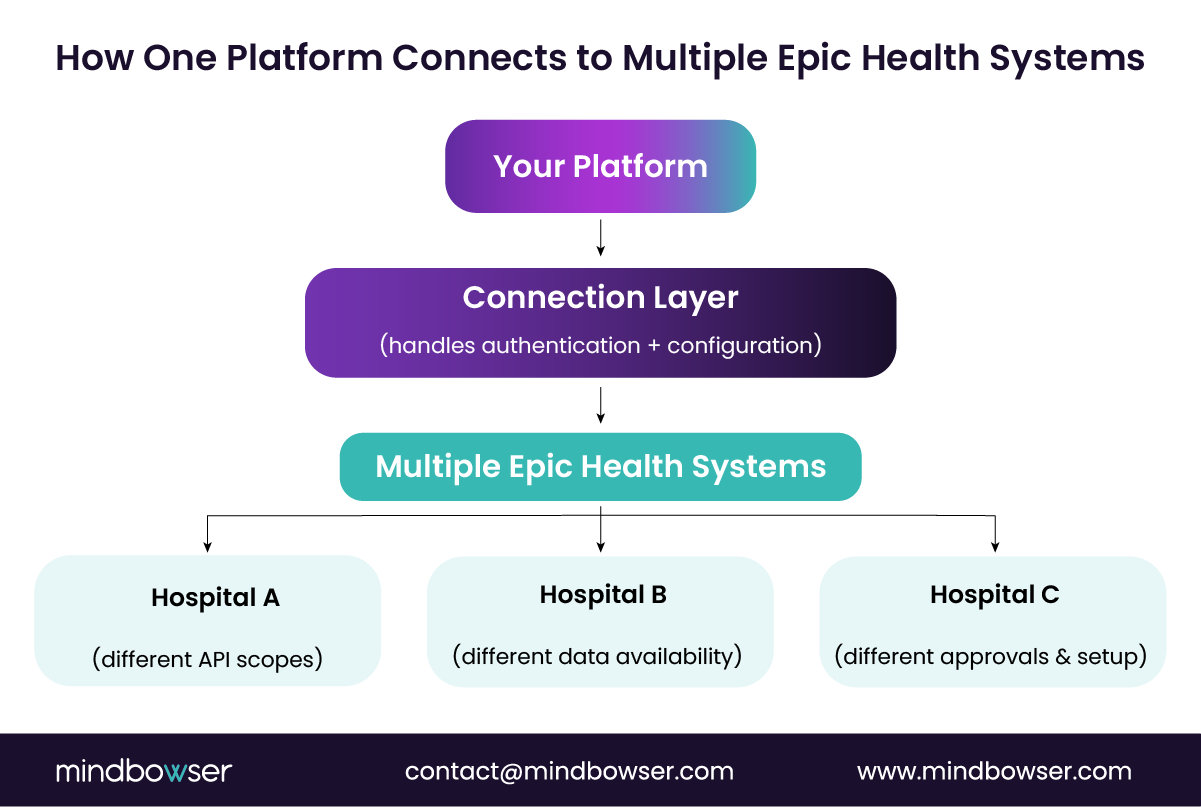
Building a single integration with the Epic EHR is manageable. Designing a platform that works across many health systems is a challenge in its own right. Organizations that scale digital health products quickly discover that Epic FHIR APIs behave differently across Epic environments.
Each health system controls its own Epic configuration, which means supported resources, authentication scopes, and rate limits may vary. Applications integrating with Epic FHIR APIs must therefore be designed with flexibility rather than assuming a single universal configuration.
A scalable Epic EHR integration architecture typically includes three core components.
1. Integration Gateway Layer
A gateway or middleware layer sits between the application platform and the Epic EHR. This layer manages authentication, token refresh, API orchestration, and endpoint routing for Epic interoperability APIs.
Instead of embedding Epic logic directly inside the product, the gateway centralizes the integration logic required to interact with Epic FHIR APIs.
2. Resource Normalization Layer
FHIR resources retrieved from the Epic EHR may differ between health systems depending on configuration and available scopes. A normalization layer maps incoming data to a consistent internal schema, allowing applications to operate without relying on site-specific data structures.
This approach allows platforms to maintain stable product logic while adapting to variations in Epic FHIR APIs across organizations.
3. Site Configuration Management
Every Epic client introduces its own endpoints, OAuth scopes, and operational policies. Managing these differences requires a configuration framework that tracks site-specific settings for each Epic EHR environment.
Configuration may include:
- Endpoint URLs
- Supported FHIR resources
- Approved OAuth scopes
- Request rate limits
- Environment credentials
Without this layer, multi-site integrations using Epic FHIR APIs quickly become difficult to maintain.
Another architectural priority is resiliency. Production integrations with the Epic EHR must handle intermittent API failures, rate limits, and network disruptions. Retry logic, caching strategies, and request throttling are often required to maintain stable performance.
Organizations planning large-scale interoperability initiatives often work with specialized FHIR integration services to implement these architectural patterns and manage cross-system complexity.
When implemented correctly, Epic FHIR APIs allow platforms to connect to multiple Epic EHR deployments while maintaining a stable internal architecture. The difference between a working integration and a scalable one usually comes down to how well these architectural layers are designed.
VII. Operational Realities of Deploying Epic FHIR Integrations
Consider a common scenario.
A digital health company builds a platform that successfully integrates with Epic FHIR APIs at one hospital. The engineering team assumes the architecture will work the same way when onboarding the next customer running the Epic EHR.
The second deployment begins. Authentication works. The application connects to the endpoint. But several FHIR resources return fields that differ from the expected ones. One OAuth scope is not approved. Rate limits are lower than the original site.
The integration works. But not the same way.
This situation occurs frequently when organizations begin scaling across multiple Epic EHR environments. Even though the platform uses standardized Epic interoperability APIs, each health system operates its own configuration and governance model.
Now imagine a larger rollout. Your platform supports ten health systems running the Epic EHR. Each organization has different:
- API scopes approved for external vendors
- FHIR resources enabled within Epic FHIR APIs
- Security approval processes
- Infrastructure policies for production access
From an engineering perspective, the integration surface expands quickly. Operational teams must manage multiple endpoints, authentication credentials, security approvals, and environment configurations across every Epic EHR customer.
This is where many interoperability initiatives begin to encounter friction. The technology works. The operational coordination becomes the real challenge.
Teams responsible for Epic EHR integration must work closely with hospital interoperability teams, security departments, and compliance stakeholders. These relationships often determine how quickly production access to Epic FHIR APIs can be approved.
Another practical consideration involves testing environments. Epic sandboxes used for development may not perfectly reflect production configurations. Applications that function correctly in sandbox environments sometimes require adjustments when connected to live Epic EHR systems.
For platform leaders, the lesson is operational rather than technical. Scaling integrations using Epic FHIR APIs requires governance processes, deployment playbooks, and coordination frameworks that extend beyond the engineering team.
Organizations that treat Epic interoperability as a long-term operational program rather than a one-time integration effort are better positioned to successfully support multiple health systems.
VIII. Common Production Challenges with Epic FHIR APIs
Once applications move from development to production, organizations begin to encounter the practical limitations of working with Epic FHIR APIs across multiple Epic EHR environments. The FHIR standard itself rarely causes these challenges. Instead, they emerge from differences in configuration, governance policies, and operational controls across health systems.
Production environments for the Epic EHR are designed with strict safeguards in place. These controls protect clinical systems but also introduce complexity for external applications consuming Epic interoperability APIs.
A few challenges appear consistently across implementations.
First, resource variability. Even when applications call the same Epic FHIR APIs, the available data fields may differ between health systems. One hospital may expose detailed encounter data, while another limits access to basic patient demographics. Integration architectures must therefore account for variable data structures across Epic deployments.
Second, authorization constraints. Access to Epic FHIR APIs is controlled through OAuth scopes approved by each hospital’s IT governance team. If an application requests a scope that has not been approved within a specific Epic EHR environment, the request fails. This often requires early coordination with health system interoperability teams to validate scope availability.
Third, there are environmental differences between development sandboxes and live systems. Sandbox environments used for testing may support simplified datasets or broader permissions than production Epic EHR systems. As a result, integrations that function in testing environments sometimes require adjustments when deployed against real clinical systems.
Finally, performance considerations. Applications using Epic FHIR APIs must respect rate limits and optimize queries to avoid excessive API requests. Inefficient calls can lead to throttling or degraded performance when retrieving data from the Epic EHR.
These challenges are well understood by organizations that operate at scale across multiple Epic customers.
A. Common Epic FHIR Production Challenges
| Challenge | Root Cause | Mitigation Strategy |
|---|---|---|
| Resource variability | Different Epic configurations per site | Configurable resource mapping |
| Scope authorization failures | OAuth restrictions | Early scope validation |
| Sandbox vs production differences | Sandbox limitations | Production testing workflow |
| Performance bottlenecks | Rate limits, inefficient queries | Caching + request optimization |
Addressing these issues requires strong integration governance and architecture designed specifically for the realities of the Epic EHR ecosystem.
Organizations that anticipate these production constraints early are far more successful when deploying Epic FHIR APIs across multiple health systems.
IX. How Epic FHIR APIs Enable Digital Health and Remote Care Platforms
Healthcare delivery is expanding beyond the hospital. Remote monitoring, virtual care, and patient engagement platforms all depend on access to data stored inside the Epic EHR. This is where Epic FHIR APIs become critical.
Digital health platforms typically operate outside the core Epic EHR environment. They collect patient-generated data from devices, mobile apps, and connected care systems. To make that information clinically useful, applications must combine it with the patient’s medical record.
Epic FHIR APIs provide that bridge.
A typical architecture works like this:
- A digital health platform collects patient-generated data
- The application retrieves clinical context from the Epic EHR
- Device data and clinical records are analyzed together
- Insights are delivered to clinicians through dashboards or workflows
Without access to Epic clinical data, most digital health platforms cannot operate effectively.
A. Example: Remote Patient Monitoring
Consider a heart failure monitoring program. A patient records daily measurements from connected devices, such as:
- Blood pressure monitors
- Weight scales
- Pulse oximeters
The monitoring platform continuously receives this data. To interpret the readings correctly, the system retrieves patient information from the Epic EHR using Epic FHIR APIs, including:
- Medications
- Diagnoses
- Recent encounters
- Care plans
This combination allows clinicians to evaluate whether device readings reflect normal variation or a potential deterioration.
B. Where This Integration Appears Most Often
Healthcare organizations commonly rely on Epic FHIR APIs when building:
- Patient engagement mobile applications
- Remote patient monitoring platforms
- Population health analytics tools
- Care coordination systems
- Clinical AI decision-support applications
Each of these platforms retrieves clinical data from the Epic EHR while performing analytics or workflow support outside the core EHR environment.
As digital health services continue to expand, Epic FHIR APIs are becoming the standard method for connecting external healthcare platforms to the Epic EHR.
X. Governance, Security, and Compliance for Epic Integrations
Technical connectivity is only one part of integrating with the Epic EHR. Health systems also evaluate governance, security, and compliance before granting access to Epic FHIR APIs. For many organizations, these operational controls determine whether an integration is approved.
Every health system operating the Epic EHR maintains its own vendor onboarding process. External platforms requesting access to Epic FHIR APIs typically undergo security reviews that evaluate how patient data will be accessed, stored, and protected.
Common review areas include:
- HIPAA compliance and data protection controls
- Encryption standards for data in transit and at rest
- Identity management and access control policies
- Audit logging and monitoring of API activity
- Breach response and incident management procedures
Because Epic FHIR APIs allow applications to retrieve protected health information, health systems must ensure vendors meet strict security standards before production access is approved.
Another important governance factor involves OAuth scope approval. Applications must request specific scopes when calling Epic interoperability APIs, such as access to patient demographics or clinical observations. These scopes are reviewed and approved by hospital interoperability or IT governance teams.
If a requested scope is not approved within a particular Epic EHR environment, the application will not be able to retrieve that data through Epic FHIR APIs.
Vendor agreements are also common. Health systems frequently require:
- Business associate agreements (BAAs)
- Vendor risk assessments
- Interoperability governance reviews
- Production change management procedures
These steps may seem administrative, but they play a major role in Epic EHR integration timelines. Security and compliance approvals often take longer than the technical implementation itself.
For CIOs and digital health leaders, the key takeaway is organizational alignment. Successful deployment of Epic FHIR APIs requires coordination between engineering teams, compliance departments, and hospital interoperability leaders.
Technical readiness alone is rarely sufficient. Integrations with the Epic EHR move forward only when security, governance, and operational oversight requirements are fully satisfied.
XI. Why Mindbowser to Build a Custom EHR with Epic Integration Capabilities?
Integrating with the Epic EHR requires more than connecting APIs. Successful platforms must pass hospital security reviews, support multiple Epic configurations, and operate within strict governance controls.
Mindbowser helps healthcare organizations build custom platforms that integrate with Epic FHIR APIs while meeting the operational and compliance requirements of modern health systems.
A. Compliance-First Architecture for Epic Ecosystems
Epic integrations must pass security and governance reviews before production access is approved. Mindbowser designs systems that implement SMART on FHIR correctly, apply least-privilege OAuth scopes, encrypt PHI in transit and at rest, and maintain full audit visibility.
This reduces approval friction and helps integrations move through hospital onboarding processes faster.
B. Integration Patterns That Scale Across Epic Clients
Each health system running the Epic EHR has different configurations and approved API scopes. Mindbowser builds scalable integration architectures that include middleware layers, configurable resource mapping, centralized token management, and monitoring frameworks.
This allows platforms to onboard multiple Epic customers without rebuilding integrations for each organization.
C. Custom Platforms That Extend Epic Workflows
Hospitals rarely want to replace Epic. Instead, they need targeted capabilities that extend it.
Mindbowser develops platforms that integrate with Epic while supporting advanced capabilities, including care coordination dashboards, remote patient monitoring systems, AI-driven clinical insights, and population health analytics.
Epic remains the system of record while the external platform delivers workflow intelligence.
D. ROI-Focused Development for Healthcare Organizations
Epic integration must translate into measurable outcomes. Mindbowser aligns architectural decisions with operational goals, such as improved clinician efficiency, reduced manual processes, and scalable platform growth, for digital health companies.
Successful Epic FHIR integrations are not just technical projects. They are a strategic infrastructure for modern healthcare platforms.

Building Custom Healthcare Platforms That Integrate with Epic
As healthcare organizations expand digital services, the ability to integrate reliably with the Epic EHR has become a core requirement for modern healthcare platforms.
Epic FHIR APIs provide a powerful interoperability layer that allows applications to retrieve clinical data, support digital health services, and enable new care delivery models. However, they are not a plug-and-play solution. Each Epic environment introduces unique governance, configuration, and operational considerations.
For healthcare CIOs, CTOs, and platform leaders, success depends on designing an integration architecture that accounts for site variability, security approvals, and long-term scalability.
Organizations that approach Epic interoperability as a strategic capability, not just an API integration, are best positioned to build platforms that scale across the evolving Epic ecosystem.
Epic FHIR APIs are standards-based interfaces that securely allow external applications to access clinical data from the Epic EHR. They use the HL7 FHIR standard and SMART on FHIR authentication to retrieve structured healthcare data such as patient records, medications, and encounters.
Integration timelines typically range from 3 to 6 months per health system. While the technical API implementation may take a few weeks, most of the time is spent on security reviews, vendor approvals, and operational onboarding required by each Epic EHR organization.
Write access is limited and controlled by each health system. Many Epic EHR environments allow applications to read clinical data through Epic FHIR APIs, but writing data back to the system is often restricted to specific resources such as observations or patient-generated data.
Not automatically. Each health system running the Epic EHR has its own configuration, approved scopes, and API availability. Platforms integrating with Epic FHIR APIs must support site-specific configurations when onboarding multiple Epic customers.
Epic FHIR APIs are best suited for modern applications that need real-time access to structured clinical data. For deeper clinical workflows or high-volume operational integrations, organizations may also need HL7 messaging or other Epic interoperability interfaces.































