TLDR
- Cerner EHR system integration connects clinical, operational, and billing systems through HL7, FHIR, APIs, and secure data workflows.
- It improves clinical efficiency, reduces duplicate work, enhances billing accuracy, and strengthens decision-making across the enterprise.
- Cerner stands out for flexible interoperability, scalable architecture, and strong support for modern digital health applications.
- HealthConnect CoPilot accelerates safe, repeatable Cerner integrations with reusable HL7 and FHIR connectors, monitoring, and standardized API patterns.
- Ideal for CIOs, CTOs, CMIOs, and CFOs, modernizing infrastructure and reducing EHR integration risk
Health systems are under pressure to unify clinical, operational, financial, and patient experience workflows. Most organizations use many digital health applications across scheduling, care management, telehealth, billing, and population health. When these platforms are not connected to the EHR, the result is fragmented data and slow decision-making.
This is why Cerner EHR system integration has become a strategic focus for CIOs and CTOs. Cerner is no longer just a charting tool. It is the central operating system of clinical care, and integrating it effectively determines how well a hospital manages patient outcomes, revenue integrity, regulatory compliance, and overall workflow efficiency.
Cerner, now Oracle Health, continues to hold a significant share of the U.S. acute care hospital EHR market. Definitive Healthcare data shows Epic at about 37.7 percent market share and Oracle Health (Cerner) at about 21.7 percent of U.S. inpatient hospitals in 2024, confirming that Cerner remains a core platform across the provider landscape.
At the same time, the global electronic health record market is projected to grow from about 31.2 billion dollars in 2024 to 40.4 billion dollars by 2030, reflecting steady demand for EHR modernization and integration. For leadership teams, this means the EHR is a long-term investment, and integration choices made today will shape clinical and financial performance for the next decade.

I. What Makes Cerner EHR System Integration Different From Other EHR Platforms?
A. How Does Cerner Support Interoperability in Real Clinical Environments?
A key advantage of Cerner EHR is its flexible interoperability stack. The platform supports multiple integration models that help health systems modernize without replacing their existing infrastructure.
Cerner enables the following:
- HL7 v2 messaging for ADT, orders, results, billing, and scheduling
- FHIR APIs for structured and standardized clinical data
- REST and JSON-based APIs for modern digital health integrations
- SMART on FHIR application support for embedded third-party apps
- Real-time data availability across inpatient and ambulatory settings
This combination of legacy and modern standards makes Cerner suitable for large health systems, regional hospitals, and growing digital health platforms.
B. How Does Cerner Improve Clinical Efficiency and Patient Outcomes?
Effective Cerner EHR system integration delivers improvements across several workflows:
- Clinicians can access complete patient histories in a single view
- Orders and results sync more reliably across departments
- Reduced double documentation saves valuable provider time
- Care managers track patients with clearer timelines and data
- Fewer missed results improve patient safety
These improvements are especially valuable for emergency departments, inpatient units, and high-volume specialty clinics where clinicians rely on rapid information retrieval.
C. Why is Cerner Easy to scale across multi-site health systems?
Cerner’s architecture is modular, allowing organizations to expand without redesigning existing workflows. Large systems often choose Cerner because it can support:
- Multi-facility deployments
- Regional health information exchanges
- Enterprise analytics layers
- Complex billing and coding workflows
- Population health registries
For smaller practices, Cerner EHR offers configurations that match their size while maintaining enterprise-level reliability.
This balance of customization and scalability sets Cerner EHR apart when compared to systems like Epic, which often require more rigid implementation structures.
II. How Does Cerner EHR System Integration Work Across a Modern Healthcare Stack?
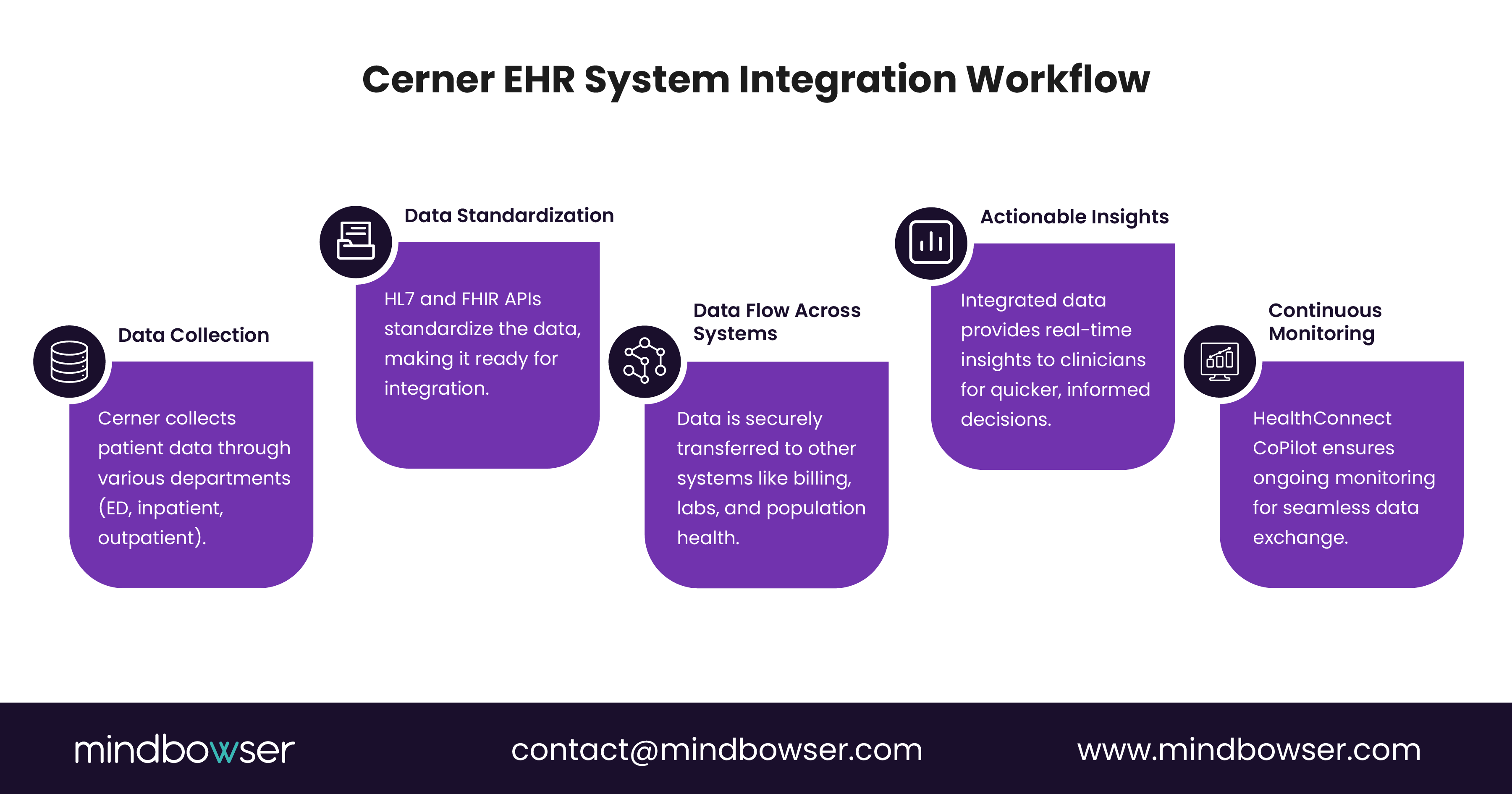
A. What Role Do HL7 Interfaces Play in Cerner Integration?
Most hospitals rely on HL7 messages to power core workflows. Cerner EHR supports a robust set of HL7 v2 interfaces that handle:
- Patient registration and ADT events
- Lab, radiology, and ancillary orders
- Clinical results and documentation updates
- Billing events and charge transactions
- Scheduling updates across service lines
These messages form the backbone of Cerner EHR system integration, providing reliable, real-time communication between the Cerner EHR and downstream systems.
B. Why Bidirectional Scheduling Matters in Cerner Integrations
Scheduling automation depends on Cerner receiving updates, not just sending them. Reminders, confirmations, and cancellations only work reliably when SIU or ADT write-back is enabled. Without write-back, digital applications operate as read-only mirrors that quickly diverge from the live Cerner schedule.
This drift creates operational noise. Staff see one schedule in Cerner while patients receive messages based on data from external tools.
Many teams implement read-only scheduling interfaces, believing they are sufficient, only to discover later that they cannot automate confirmations, reschedules, or follow-up sequences. Full workflow automation requires Cerner to acknowledge and store each scheduling update in real time.
For digital health leaders, the lesson is simple: read-only scheduling solves visibility, but write-back unlocks true automation and reduces administrative burden.
C. How Are FHIR and REST APIs Used for Modern Applications?
Digital health companies and internal innovation teams increasingly rely on:
- FHIR endpoints for clinical summaries, conditions, medications, vitals, and labs
- REST APIs for appointment management, patient access, and task workflows
This allows organizations to integrate:
- Remote patient monitoring programs
- Telehealth platforms
- Digital front door tools
- Care management applications
- Predictive analytics models
FHIR makes Cerner EHR more future-ready than many legacy EHR systems, whose APIs remain limited.
For teams adopting modern APIs, understanding how HL7 and FHIR complement each other helps define scalable integration patterns.
D. How Does Cerner Ensure Data Privacy and HIPAA Compliance During Integration?
Cerner EHR incorporates several controls to ensure compliant integration:
- Encrypted data transfer and at-rest storage
- Strict audit tracking of PHI access and modification
- Role-based access and user authentication
- Secure SDKs for partner integrations
- Logging for anomalous or high-risk access
For CIOs and security leaders, consistent compliance patterns across all interfaces reduce operational risk.
E. How Does Integration Improve Patient and Provider Access to Records?
Integrated Cerner environments allow:
- Patients to access results, summaries, and visit histories through portals
- Providers to view a complete record without switching systems
- Care teams to coordinate more effectively through shared visibility
When executed well, integration enhances the patient experience and improves clinician workflows.
F. How Does Cerner Simplify Billing and Revenue Cycle Operations?
Cerner supports revenue cycle improvements by integrating:
- Charge capture with clinical documentation
- Automated billing events
- Denial management workflows
- Insurance eligibility and verification data
Organizations that link Cerner EHR with external billing partners often see reductions in:
- Duplicate claims
- Incorrect coding
- Manual charge fixes
- Claim submission delays
This directly improves margin and cash flow.
G. Why Cerner Integrations Take Longer Than Expected
Even experienced engineering teams underestimate the real timeline of Cerner HL7/FHIR integrations. Custom integration stacks built with Mirth, Kafka, or microservices typically require three to six months to design, test, and stabilize across Cerner environments.
AI tooling can assist with generating schemas or mappings, but engineers must still debug routing rules, validate message formats, and resolve discrepancies that emerge during HL7 testing cycles.
Cerner integrations require more than API calls. They involve VPN and tunnel provisioning, endpoint whitelisting, certificate management, FHIR key request approvals, and repeated validation of SIU/ADT messages. These steps extend timelines because each environment, sandbox, test, and production, behaves differently.
During due diligence, CTOs routinely ask about message stability, scalability across multiple facilities, uptime SLAs, and the maintenance burden once the integration is live. These considerations often reshape project timelines more than the application build itself.
Accelerate Cerner EHR system integration with proven HL7 and FHIR connectors
III. How Does Cerner Compare With Other EHR Solutions?
A. How Does Cerner Compare With Epic?
Epic has a highly mature ecosystem, but it is also more rigid and standardized. Cerner stands out for:
- Greater interface openness
- Flexible integration models
- A broader mix of deployment options
- More adaptable configurations for small and mid-sized systems
- Strong support for third-party applications
For health systems prioritizing integration over standardization, Cerner often provides more room to innovate.
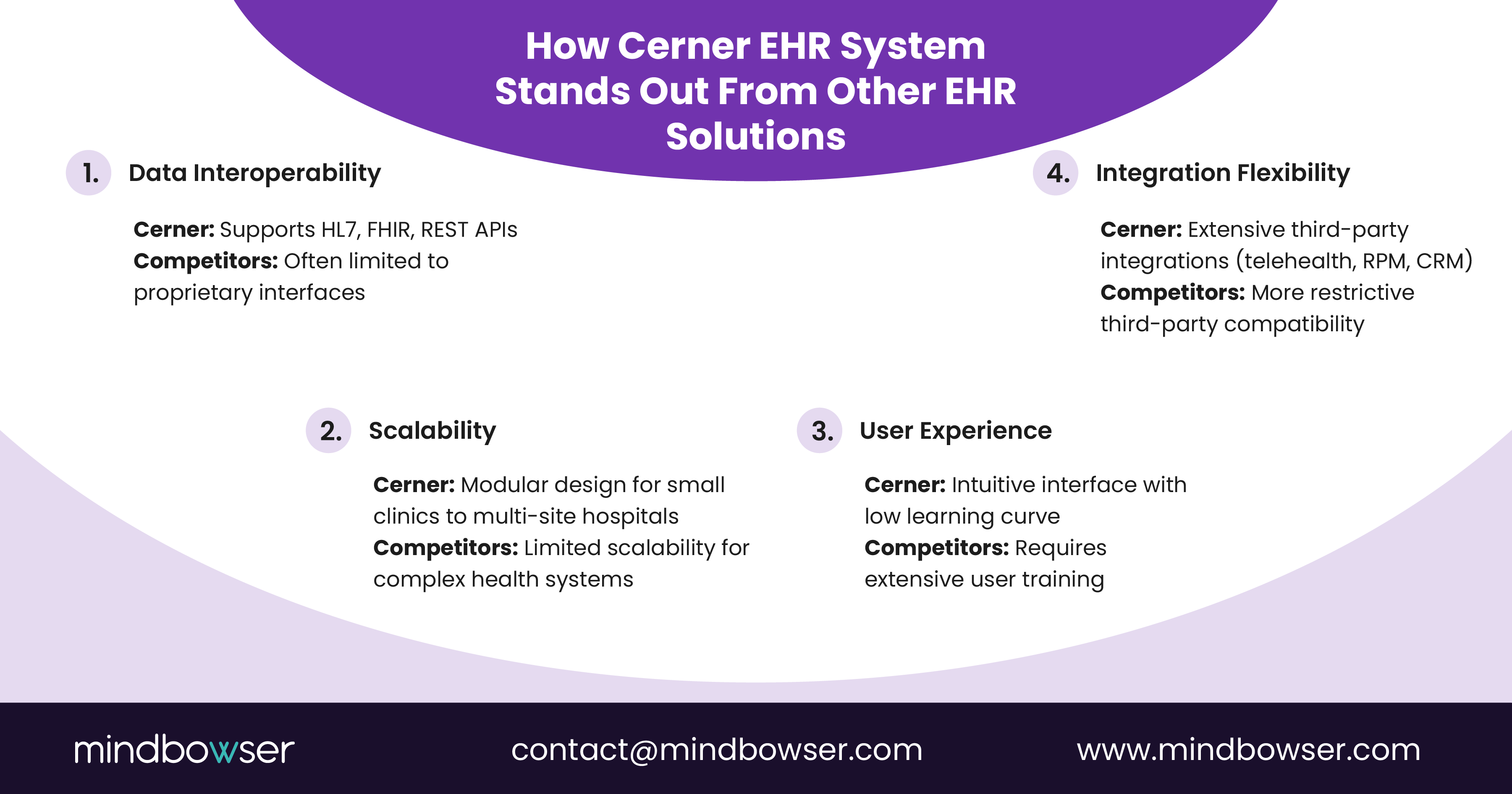
B. How Does Cerner Compare With athenahealth or Meditech?
athenahealth offers strong cloud capabilities but has limited enterprise-scale compared to Cerner. Meditech serves smaller hospitals effectively but lacks the advanced interoperability stack Cerner provides.
Across interoperability, scalability, and EHR ecosystem depth, Cerner remains a strong middle ground between highly rigid systems and overly simple ones.
C. Which Metrics Prove the Value of Cerner EHR System Integration?
Executives want evidence that the Cerner EHR system integration delivers measurable value. The most effective programs define a clear baseline and track improvement across specific metrics, for example:
1. Clinical metrics
- Time to retrieve a complete patient summary in high acuity settings
- Reduction in duplicate tests due to incomplete data
- Closed-loop result follow-up rates
2. Operational metrics
- Percentage of orders and results flowing through integrated interfaces
- Reduction in manual work queues tied to data mismatches
- Interface-related downtime incidents per quarter
3. Financial metrics
- Decrease in charge corrections related to documentation gaps
- Reduction in claim denials tied to missing or inconsistent data
- Days in accounts receivable and net collection rate
At the market level, the ongoing adoption of EHR systems reinforces why integration investments matter.
Oracle Health still accounts for roughly one-fifth of U.S. acute care hospital EHR installations, and global EHR spending continues to rise toward the 40 billion-dollar range by 2030, indicating that EHR platforms remain central to digital health strategies rather than being replaced by point solutions.
By tying Cerner integration projects to a clear KPI set, CIOs and CFOs can justify investment and track real ROI over time.
IV. Build vs Buy: The Cerner Integration Dilemma for Healthcare Technology Leaders
Healthcare engineering teams face a strategic choice when integrating with Cerner: build connectivity internally or adopt a managed interoperability layer. Internal development requires deep familiarity with HL7 message structures, SIU/ADT workflow mechanics, ACK handling, FHIR authentication, TCP/MLLP connections, VPN setup, and routing logic across facilities.
These builds often take months and introduce long-term maintenance obligations.
Custom integrations just also scale across hospitals, each with unique feeds, environments, and mapping requirements. This increases operational cost and extends implementation timelines. In contrast, platform-based integrations shorten time-to-market to days once credentials and workflows are finalized.
Enterprise buyers consistently ask about compliance readiness, audit logs, backup and DR processes, sandbox limitations, SLAs, and references from similar Cerner deployments. These considerations shape both risk assessment and total cost of ownership. Leaders evaluating Cerner interoperability must weigh internal control against speed, predictability, and ongoing support needs.
V. How HealthConnect CoPilot Accelerates Cerner EHR System Integration?
Many health systems struggle with interface backlogs, lengthy testing cycles, and inconsistent integration patterns. Mindbowser’s HealthConnect CoPilot helps organizations overcome these challenges by offering:
- A pre-configured integration hub for Cerner HL7, FHIR, and API workflows
- Reusable mappings for patient administration, billing, and clinical data
- Monitoring and alerting for interface health
- Standardized authentication patterns for vendor integrations
- Faster onboarding of digital health applications
HealthConnect CoPilot helps technical teams avoid custom one-off builds and ensures integration consistency across the enterprise.

Why Cerner EHR System Integration Delivers Long-Term Strategic Value?
Cerner’s combination of interoperability tools, scalable architecture, and workflow adaptability makes it a strong choice for organizations that want to:
- Improve clinical efficiency
- Modernize patient experience
- Strengthen revenue integrity
- Scale digital health initiatives
- Reduce integration risk
With the right architecture, governance, and integration accelerators, Cerner becomes more than an EHR. It becomes the unified operational engine for clinical and financial performance.
To modernize EHR connectivity across service lines, explore our healthcare integration services that support Cerner, Epic, and custom workflows.
Cerner EHR system integration connects Cerner with clinical, operational, and financial systems using HL7, FHIR, REST APIs, and secure SDKs. This enables real-time data exchange, reduces fragmented workflows, and improves clinical accuracy, billing performance, and patient experience.
Cerner offers a flexible interoperability stack combining HL7 v2 interfaces, FHIR APIs, SMART on FHIR support, and REST-based workflows. This mix helps organizations modernize without replacing legacy infrastructure and supports more third-party applications than many rigid EHR ecosystems.
Real-world Cerner integrations often require:
• HL7 message mapping and ACK handling
• VPN setup and endpoint whitelisting
• Smart-on-FHIR credential approvals
• Multi-environment configurations (sandbox, test, prod)
Custom builds using tools like Mirth and Kafka frequently take 3–6 months to complete.
When Cerner credentials or interfaces are not yet configured, teams often start with CSV-based workflows for scheduling, reminders, or post-discharge follow-ups. These workflows break at scale and do not sync updates or cancellations back into Cerner.
Bidirectional scheduling requires Cerner SIU/ADT workflows.
Without SIU write-back, appointment updates from digital health apps never reach Cerner, causing mismatched calendars, patient confusion, and manual staff intervention.
































