TL;DR
- Virtual care cannot scale when telehealth visits, remote patient monitoring data, and EHR workflows operate in separate systems.
- Telehealth interoperability connects these environments using standards such as HL7, FHIR APIs, and SMART on FHIR, ensuring patient data moves reliably across platforms.
- When telehealth systems integrate with clinical workflows, clinicians see unified patient records, RPM alerts reach the right care teams, and AI insights become clinically useful rather than isolated analytics.
Why do telehealth visit notes or RPM alerts sometimes fail to appear in the clinician’s EHR workflow?
The answer often lies in gaps in telehealth interoperability. As virtual care expands beyond video visits to include remote patient monitoring, care coordination, and AI insights, disconnected systems lead to fragmented patient data and increased clinician workload.
This guide explains how standards such as HL7, FHIR APIs, and SMART on FHIR help digital health platforms connect telehealth systems to EHR and RPM infrastructure to support scalable virtual care.
I. Why Does Telehealth Interoperability Decide Whether Next-Gen Virtual Care Actually Scales?
A. What Telehealth Interoperability Means for Modern Virtual Care Platforms
Telehealth has evolved far beyond video consultations.
Today’s virtual care platforms support remote patient monitoring, asynchronous messaging, digital triage, care coordination, and AI-assisted clinical insights. These capabilities promise continuous care beyond hospital walls.
But the promise only works when information moves across systems.
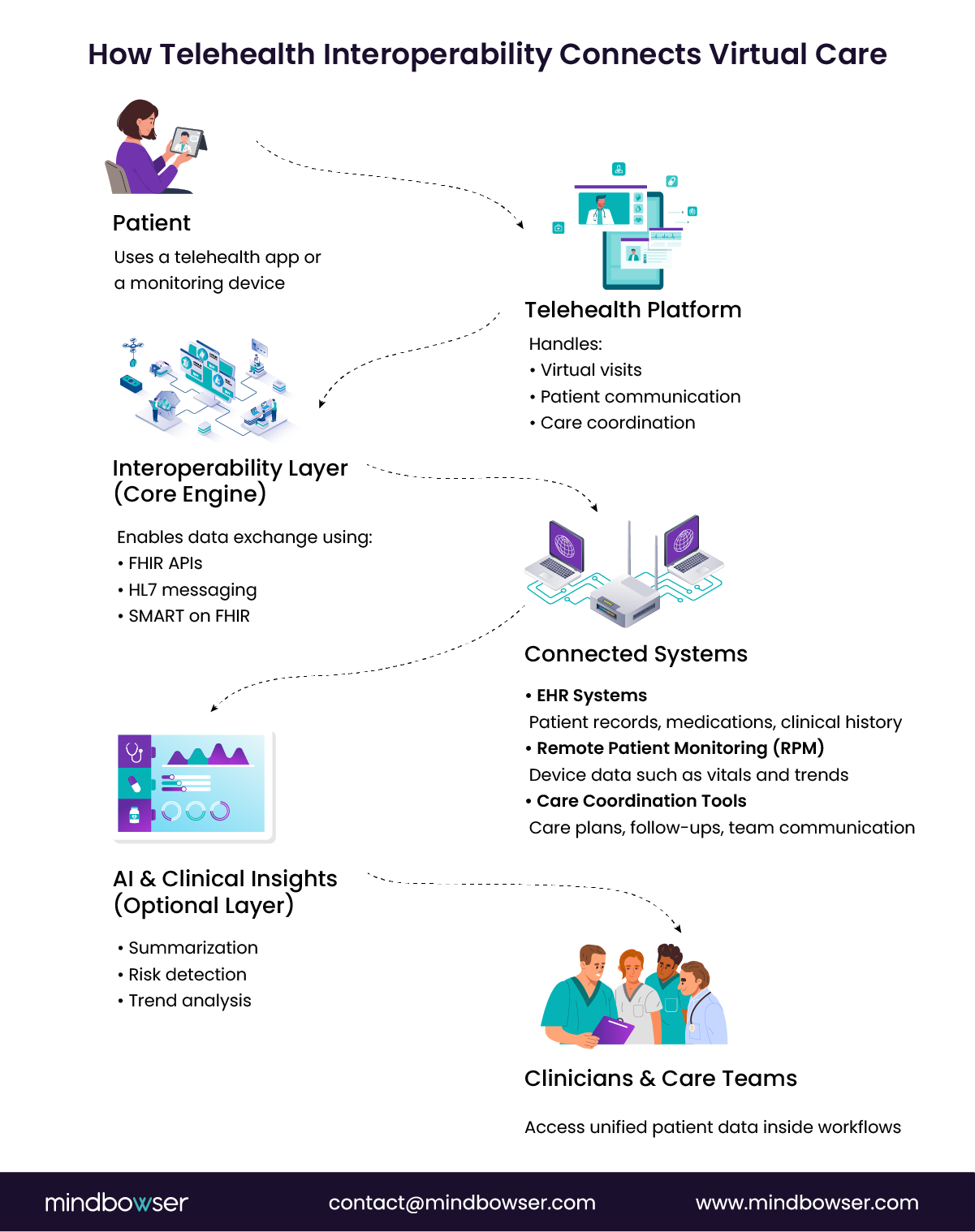
Telehealth interoperability refers to the ability of virtual care platforms to exchange patient data with other healthcare systems in ways that clinicians can use inside real workflows. That includes:
- EHR integration with hospital systems
- Remote patient monitoring device data ingestion
- Care coordination tools across teams
- Payer and claims data exchange
- Analytics and clinical summarization tools
Without this connectivity, virtual care becomes another isolated system.
Healthcare standards make that connectivity possible. HL7 interoperability frameworks, FHIR APIs, and SMART on FHIR enable the structured exchange of clinical data across healthcare systems. Telehealth applications can retrieve patient records, write encounter notes back to the EHR, and launch applications directly inside clinician workflows.
Consider a common scenario. What happens when an RPM alert fires but the data never reaches the clinician responsible for that patient?
Without telehealth interoperability, the alert may remain within a device vendor’s dashboard rather than trigger action in the care team’s workflow.
This is why enterprise health systems evaluate telehealth platforms first by their integration capabilities. Virtual care must function as an extension of the clinical record, not a separate tool.
Effective telehealth interoperability connects virtual visits, monitoring data, and EHR workflows into one coordinated clinical experience.
Related read: Telehealth EHR Integration Development: How to Build Connected and Compliant Virtual Care Workflows
B. Where Data Silos Appear in Telehealth and Remote Patient Monitoring
Even well-designed telehealth products often end up with hidden data silos.
Patient intake tools may store demographic and insurance information in a scheduling platform. Digital triage questionnaires may be embedded within patient engagement tools. Visit documentation may remain inside the telehealth platform itself.
Meanwhile, remote patient monitoring vendors often maintain separate dashboards for device readings.
The result is fragmented clinical information:
- Patient intake systems capture medical history outside the EHR
- Telehealth visit notes remain disconnected from hospital records
- RPM device metrics stay trapped inside vendor dashboards
When telehealth interoperability is weak, clinicians must manually move information between systems.
The technology exists to fix this problem. The challenge lies in connecting workflows across tools that were never originally designed to work together.
C. What Happens When Telehealth Platforms Lack Interoperability
When telehealth interoperability is missing, clinicians experience immediate operational friction.
Documentation must be entered in multiple systems. Visit summaries may need to be copied into the hospital EHR. Medication lists become inconsistent across platforms.
Patients feel the impact as well. They often repeat their medical history, medications, and allergies during each virtual encounter.
The clinical risk is greater with remote patient monitoring. If device alerts never integrate into clinician workflows, care teams may miss early warning signals. That gap undermines the entire value proposition of continuous monitoring.
Virtual care works only when information flows across systems. When telehealth interoperability fails, virtual care becomes fragmented care.
Scaling next-generation virtual care requires interoperability first, features second.
II. What Architecture Breaks Telehealth Data Silos Across EHR, RPM, and AI Systems?
Virtual care leaders often discover interoperability challenges only after their platforms begin to scale.
The first integrations appear manageable. One EHR connection. One RPM vendor. A few APIs. Then, enterprise clients request additional integrations. Suddenly, the architecture becomes difficult to maintain.
The solution is not more integrations. It is a better interoperability architecture.
“Telehealth interoperability succeeds when integrations become reusable infrastructure, not one-off engineering projects.”
A. Which Interoperability Architecture Patterns Work Best for Telehealth Platforms
Imagine a virtual care startup preparing for its first enterprise deployment.
The product team has built a strong telehealth experience. Video visits work well. RPM dashboards provide device readings. AI generates visit summaries.
Then the health system asks a simple question.
Can the platform integrate with Epic, Cerner, and Meditech without custom work for each deployment?
This is where telehealth interoperability architecture becomes a strategic decision.
1. Point-to-Point Integrations
Early-stage platforms often begin with direct integrations between systems. A telehealth platform connects directly to an EHR through HL7 messages or custom APIs. RPM vendors connect through another interface.
This approach works initially, but becomes difficult as the platform grows. Each new health system introduces:
- Different EHR configurations
- Different authentication requirements
- Different clinical workflows
“Point-to-point integrations solve the first integration problem. They rarely solve the tenth.”
2. API-First Interoperability Platforms
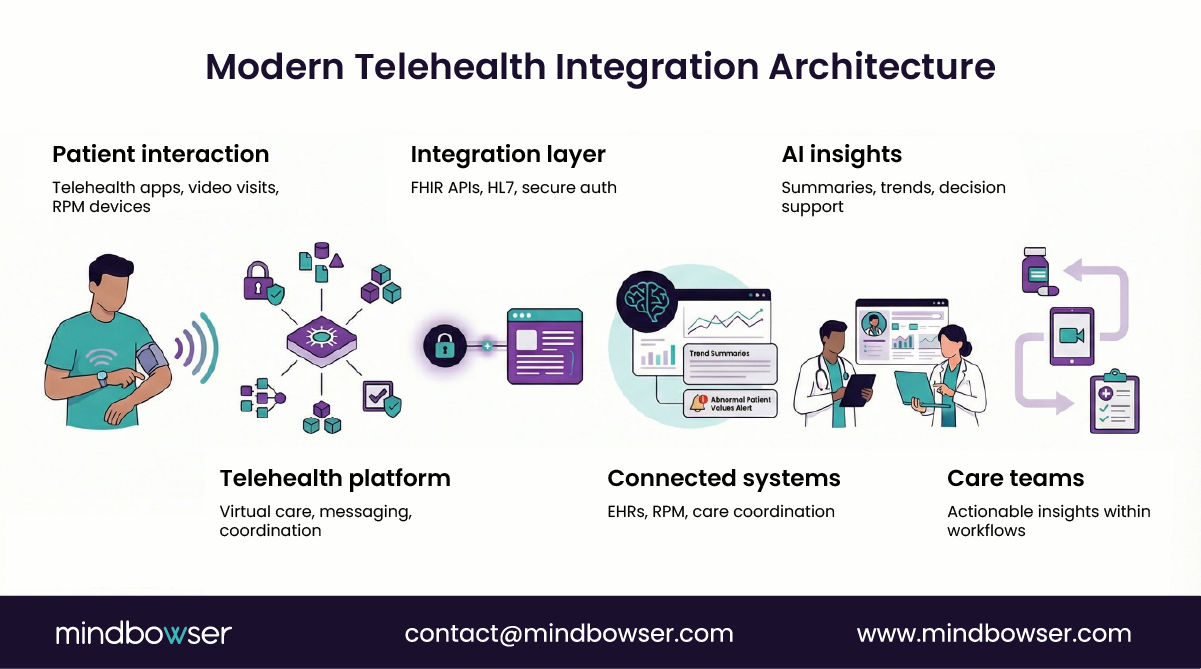
More mature virtual care platforms move toward API-first architecture. Instead of building direct integrations for every partner system, they create a central integration layer that manages communication between systems.
This layer typically handles:
- FHIR APIs for structured clinical data exchange
- HL7 interoperability for legacy systems
- Authentication and authorization workflows
- Data transformation between formats
With this model, new integrations connect to the integration layer rather than to the product directly. This design improves telehealth interoperability by enabling the platform to support multiple health systems without rebuilding the integration logic each time.
3. SMART on FHIR Embedded Applications
Enterprise health systems increasingly expect telehealth platforms to work inside the EHR. This is where SMART on FHIR becomes valuable.
SMART on FHIR allows telehealth applications to launch directly within EHR environments while securely accessing patient data through FHIR APIs.
Consider a clinician workflow. A physician opens a patient’s chart in the hospital EHR. From that chart, they launch a telehealth application through SMART on FHIR. The telehealth platform automatically retrieves:
- Patient demographics
- Medication lists
- Allergy information
- Recent clinical encounters
The visit documentation can then be written back into the EHR. This architecture creates a more natural clinician workflow and strengthens interoperability for telehealth across systems.
B. What Core Interoperability Components Should Be Built Before Scaling a Telehealth Platform
Even with the right architectural pattern, several foundational components must be in place before telehealth platforms can scale safely.
1. Patient Identity Matching
Healthcare data moves across many systems. Each system may represent the same patient differently. A telehealth platform might receive:
- Demographic records from the EHR
- Device enrollment information from an RPM vendor
- Intake forms from a patient portal
Without identity matching, these records may not connect correctly. Patient matching strategies typically rely on demographic fields combined with probabilistic matching algorithms.
“Interoperability is meaningless if the wrong patient record receives the right data.”
2. Clinical Terminology Standardization
Different systems often represent clinical data using different codes. For example:
- Lab values may use LOINC codes
- Diagnoses may use SNOMED CT or ICD codes
- Device readings may follow proprietary vendor formats
An interoperability layer must normalize these formats so downstream systems interpret the data correctly. FHIR APIs help standardize data structure, but terminology mapping ensures the meaning of that data remains consistent.
3. Consent Management and Access Control
Virtual care platforms exchange protected health information across multiple systems. This requires strong access control and consent management. Systems must track:
- Which applications can access patient data
- What data types can be shared
- How access is audited
Healthcare buyers expect HIPAA-aligned security architecture combined with detailed audit trails.
4. Data Validation and Integration Monitoring
Healthcare integrations rarely remain static. APIs evolve. Data formats change. Vendors update device firmware. Without monitoring pipelines, integrations can silently fail.
Interoperability platforms therefore implement:
- Data validation checks
- API monitoring
- Automated alerts for failed integrations
This operational layer ensures that telehealth interoperability continues working after deployment.
C. How Remote Patient Monitoring Data Becomes Clinically Actionable
Remote patient monitoring introduces a new category of healthcare data. Instead of periodic clinical observations, RPM devices generate continuous streams of physiological data.
Examples include:
- Blood pressure readings
- Glucose measurements
- Pulse oximetry values
- Weight changes for heart failure monitoring
However, raw device data alone does not improve care.
Consider a thought exercise. A patient with heart failure uses a connected scale at home. Their weight increases by two pounds overnight. The device dashboard captures the measurement. But if that reading remains inside the vendor dashboard, clinicians may never see it.
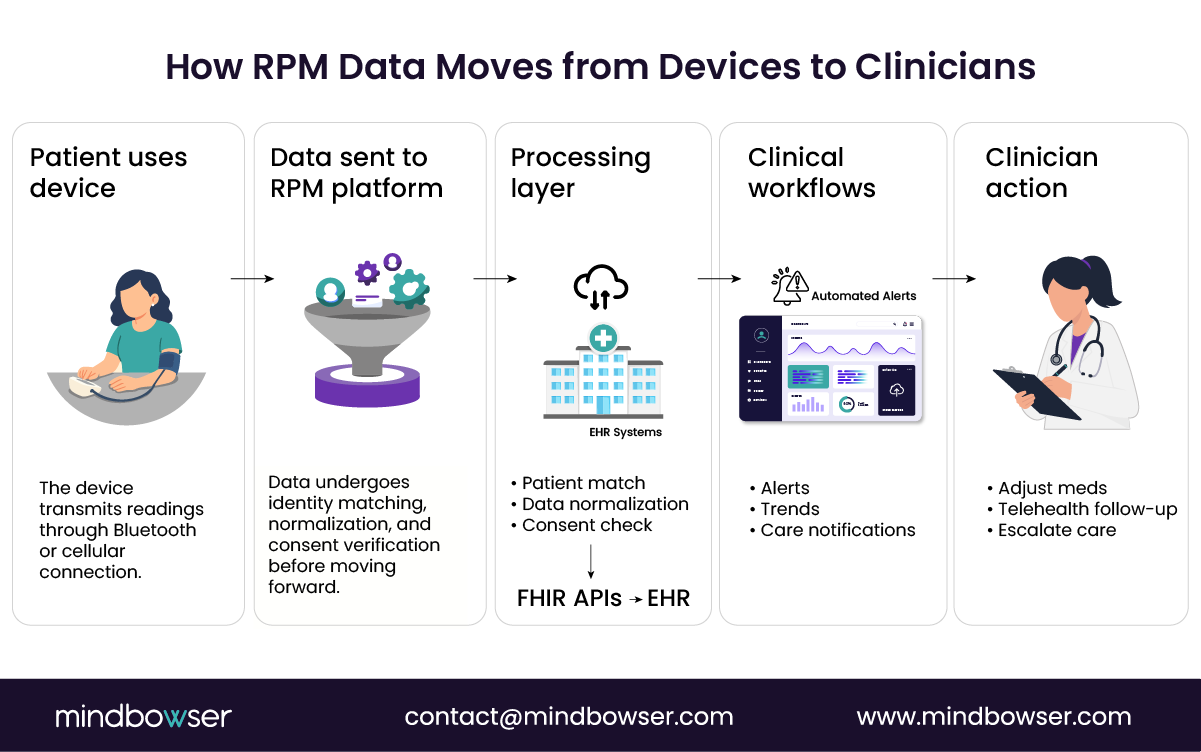
This is where telehealth interoperability becomes critical. RPM data must move through several stages before it becomes clinically actionable:
- Data ingestion from device vendors
- Normalization into standardized formats such as FHIR resources
- Identity matching to the correct patient record
- Clinical summarization that highlights meaningful trends
AI can assist with the final step. Algorithms may detect patterns such as rapid weight gain or abnormal trends in vital signs, generating alerts or summaries for clinicians.
RPM does not create value from more data. It creates value from a better signal.
The goal is to integrate those signals into clinician workflows where they can influence care decisions.
D. How Telehealth Platforms Maintain Interoperability After Deployment
Interoperability is not a one-time project. Healthcare ecosystems evolve constantly. New EHR versions appear. FHIR specifications expand. RPM vendors introduce new device types.
Telehealth platforms therefore require operational strategies to maintain interoperability over time.
Continuous API Monitoring
Integration pipelines should track API performance and detect failures quickly. Automated alerts help engineering teams respond before clinicians experience workflow disruptions.
Version Management
FHIR APIs and healthcare integration standards evolve regularly. Platforms must support version management so that new integrations remain compatible with existing deployments.
Security and Compliance Reviews
Because telehealth platforms exchange protected health information across multiple systems, ongoing security reviews are essential. These reviews verify that authentication, authorization, and audit logging remain aligned with regulatory expectations.
For enterprise buyers evaluating virtual care platforms, these operational capabilities signal long-term reliability. Telehealth interoperability is not simply a technical capability. It is an ongoing operational commitment.
Looking to Connect Remote Patient Monitoring with Your Telehealth Platform?
III. How Can Digital Health Startups Build Telehealth Interoperability Without Slowing Product Growth?
Digital health founders often face a difficult tradeoff. Move fast and build product features, or slow down to build interoperability infrastructure.
In reality, the most successful platforms do both by approaching telehealth interoperability as a phased capability rather than a single large engineering project.
“Interoperability is not a feature release. It is an architectural roadmap.”
A phased approach allows digital health companies to support enterprise integrations while maintaining product velocity.
A. Phased Interoperability Rollout
Consider a virtual care startup preparing for its first deployment to a health system. The platform already supports telehealth visits and remote patient monitoring. But the health system CIO asks a critical question:
Can the platform exchange patient records with our EHR?
Instead of attempting full integration immediately, many successful platforms implement telehealth interoperability in phases.
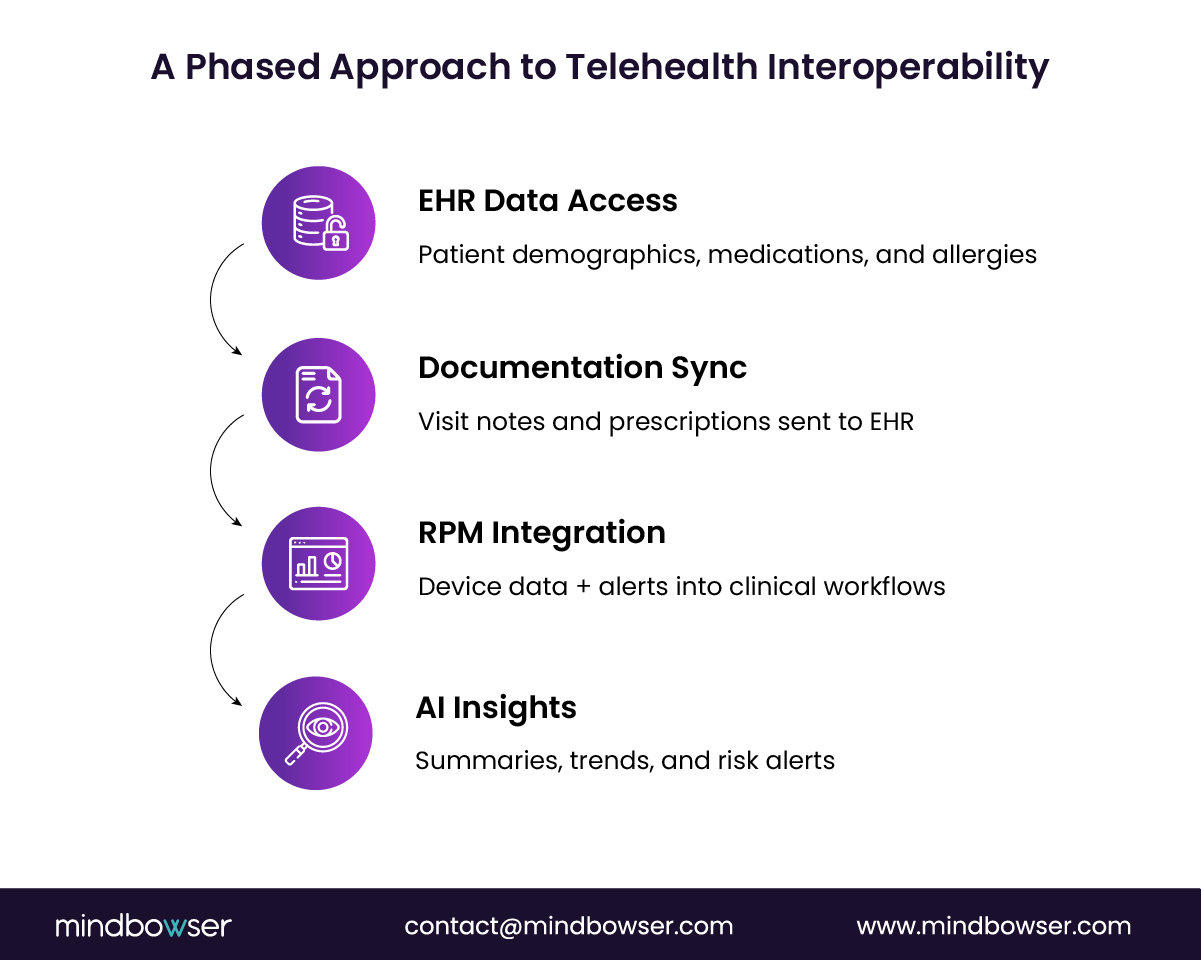
Phase 1: Retrieve Core Patient Data
The first phase focuses on retrieving essential patient information from the EHR. FHIR APIs allow telehealth platforms to access structured patient records, such as:
- Demographics
- Medication lists
- Allergies
- Active conditions
This data enables clinicians to conduct telehealth visits with an accurate patient context.
What happens when a virtual care physician prescribes medication without visibility into the patient’s existing prescriptions? Basic data retrieval solves that risk while establishing the foundation for deeper interoperability.
Phase 2: Bidirectional Clinical Documentation
Once retrieval workflows stabilize, the next step is sending clinical documentation back to the EHR. Telehealth visit notes, prescriptions, and encounter summaries must appear in the patient’s medical record.
This bidirectional exchange is a core requirement for telehealth interoperability because clinicians rely on the EHR as the system of record.
“If the encounter note never reaches the EHR, the visit effectively disappears from the clinical timeline.”
FHIR APIs and HL7 interoperability frameworks enable telehealth platforms to transmit structured encounter data while maintaining compatibility with existing healthcare systems.
Phase 3: Integrate Remote Patient Monitoring Workflows
The next layer of telehealth interoperability involves remote patient monitoring. RPM programs generate continuous streams of patient data that must integrate with clinical workflows.
Imagine a chronic disease management program that monitors patients with hypertension. Patients submit daily blood pressure readings through connected devices. Where does that data appear for clinicians?
If readings remain inside device dashboards, clinicians must check multiple systems. A better approach routes RPM readings into structured clinical workflows where care teams can:
- View trend summaries
- Receive alerts for abnormal values
- Document follow-up actions
This integration turns device data into operational care signals.
Phase 4: Integrate AI for Clinical Insights
Once data flows reliably across systems, AI capabilities become more valuable. AI models can analyze RPM trends, summarize telehealth encounters, and surface care recommendations.
But AI systems depend heavily on telehealth interoperability. Algorithms require consistent data inputs from EHR systems, RPM devices, and telehealth encounters.
Equally important, AI outputs must remain traceable. Clinical teams need to understand:
- What data informed the model
- When the insight was generated
- How the recommendation entered the workflow
“AI in healthcare becomes useful only when its outputs are grounded in interoperable clinical data.”
This final phase transforms telehealth platforms into intelligent care coordination systems.
B. Enterprise Interoperability Readiness Package
As telehealth platforms pursue enterprise clients, interoperability readiness becomes part of the product narrative. Hospital CIOs rarely approve platforms that require unclear integration efforts.
Digital health companies often prepare a readiness package that includes:
Technical Integration Documentation
Engineering teams must document how their systems connect with healthcare environments. This typically includes:
- Supported FHIR APIs
- HL7 message capabilities
- Authentication methods
- Integration architecture diagrams
Security and Compliance Architecture
Because telehealth interoperability involves protected health information, security architecture is critical. Health systems expect vendors to demonstrate:
- HIPAA-aligned data protection
- Role-based access controls
- Audit logging and traceability
- Encrypted data exchange
Clinical Workflow Design
Enterprise buyers care less about APIs and more about workflows. Product teams should demonstrate how telehealth integrations improve clinical operations. For example:
- How telehealth visit notes appear in the EHR
- How RPM alerts reach care teams
- How patient summaries support clinician decision-making
If a clinician must open three systems to review a virtual patient, has interoperability actually improved the workflow? Real telehealth interoperability reduces complexity for clinicians.
Operational Outcome Metrics
Enterprise buyers increasingly evaluate telehealth platforms using operational metrics. Examples include:
- Reduced documentation duplication
- Faster onboarding of new health systems
- Improved clinician adoption of virtual care tools
These metrics reinforce the strategic value of interoperability infrastructure.
C. How Mindbowser Helps Build Interoperable Telehealth Platforms
Building scalable telehealth interoperability requires specialized expertise in healthcare engineering. Mindbowser supports digital health companies and healthcare organizations in designing virtual care platforms that integrate reliably with healthcare ecosystems.
Telemedicine Platform Development
We build custom telehealth platforms designed to integrate with healthcare systems using established standards such as HL7 interoperability frameworks, FHIR APIs, and SMART on FHIR integration models. This approach ensures that virtual care tools function as extensions of clinical systems rather than isolated applications.
Remote Patient Monitoring Ecosystem Integration
Mindbowser helps organizations integrate RPM device platforms into telehealth environments. This includes:
- Device data ingestion pipelines
- Patient identity matching
- Clinical summarization workflows
- Alert routing into care management systems
The goal is to transform device readings into meaningful clinical signals.
AI Integration for Clinical Workflows
AI capabilities must support clinical workflows rather than replace them. Mindbowser integrates AI tools that assist with:
- Clinical summarization
- RPM trend analysis
- Documentation support for telehealth encounters
“Technology adoption in healthcare happens when systems reduce clinician effort, not when they add new dashboards.”

What Does an Interoperability-First Telehealth Strategy Enable?
Virtual care can only scale when telehealth visits, remote patient monitoring programs, and EHR workflows operate as a connected system rather than isolated tools. Telehealth interoperability enables that connection by allowing telehealth platforms to exchange patient data reliably across EHR systems, RPM devices, and analytics layers using standards such as HL7, FHIR APIs, and SMART on FHIR.
When these systems integrate into clinician workflows, telehealth visits appear in the clinical record, monitoring alerts reach the right care teams, and AI insights are drawn from consistent patient data. The result is not simply more digital health tools but a coordinated virtual care infrastructure that reduces clinician friction and supports continuous patient monitoring.
Telehealth interoperability refers to the ability of virtual care platforms to exchange patient data with healthcare systems, including electronic health records, remote patient monitoring devices, and care coordination tools. When systems can share structured clinical information, clinicians gain a complete view of the patient during virtual encounters. This connectivity reduces fragmented records and improves care coordination across virtual and in-person settings.
Several healthcare data standards support interoperability in telehealth. HL7 frameworks enable structured messaging between healthcare systems, while FHIR APIs allow modern applications to exchange clinical data through standardized web-based interfaces. SMART on FHIR allows telehealth applications to launch securely within EHR environments while accessing patient information.
Remote patient monitoring devices typically send physiological readings to device management platforms before integration with telehealth systems. Interoperable telehealth platforms ingest these readings, normalize the data, and match them to the correct patient record. Once integrated, the data can appear inside clinical workflows where care teams monitor trends and respond to alerts.
Interoperability allows telehealth visit data, patient records, and monitoring signals to appear within the same clinical system used by care teams. This reduces the need for clinicians to switch between multiple tools or duplicate documentation. As a result, clinicians can focus on patient care rather than manual data management.
AI tools help analyze large volumes of clinical data generated by telehealth encounters and remote monitoring programs. When systems are interoperable, AI models can access consistent patient records and device readings to generate meaningful insights. These insights can support clinical decision-making by summarizing patient trends or highlighting potential risks.
Startups typically build interoperability capabilities in phases to avoid slowing product development. Early steps often include retrieving patient records from EHR systems through FHIR APIs, followed by bidirectional data exchange for clinical documentation. As platforms mature, they integrate RPM data streams and workflow automation to support continuous virtual care.




















 BLOGS
BLOGS  NEWSROOM
NEWSROOM  CASE STUDIES
CASE STUDIES  WEBINARS
WEBINARS  PODCASTS
PODCASTS  ASSET HUB
ASSET HUB  EVENT CALENDAR
EVENT CALENDAR 





















