Build interoperability without replacing your EMR or EHR

How HealthConnect CoPilot Addresses EMR and EHR Limitations?
Provider organizations often operate in environments where EMRs, EHRs, and third-party systems do not consistently share data. Differences in data models, API maturity, and workflow logic slow down interoperability efforts.
This fragmentation limits the full value of both EMRs and EHRs and increases manual work for clinical and technical teams.
HealthConnect CoPilot gives organizations a unified integration layer that standardizes data mapping, streamlines system connectivity, and reduces engineering overhead. It supports predictable integration timelines and enables consistent information exchange across clinical and operational systems.
A. Unified Data Standardization
CoPilot simplifies data normalization from multiple platforms.
Capabilities include:
- Standard mapping across EMRs, EHRs, and ancillary systems
- Alignment with FHIR profiles for structured exchange
- Automated transformation of clinical and operational fields
- Reduction of manual reconciliation and rework
This creates a reliable data foundation for analytics, reporting, and quality measurement.
B. Faster Integration Timelines
CoPilot accelerates multi-system integrations by providing prebuilt patterns and connectors.
Common outcomes:
- Shorter development cycles
- Fewer custom interfaces to maintain
- Predictable onboarding of new partner systems
- Simplified testing and deployment across environments
Alera used this approach to streamline connections across multiple care settings and achieved more consistent data flow with less engineering effort.
C. Workflow Orchestration Across the Enterprise
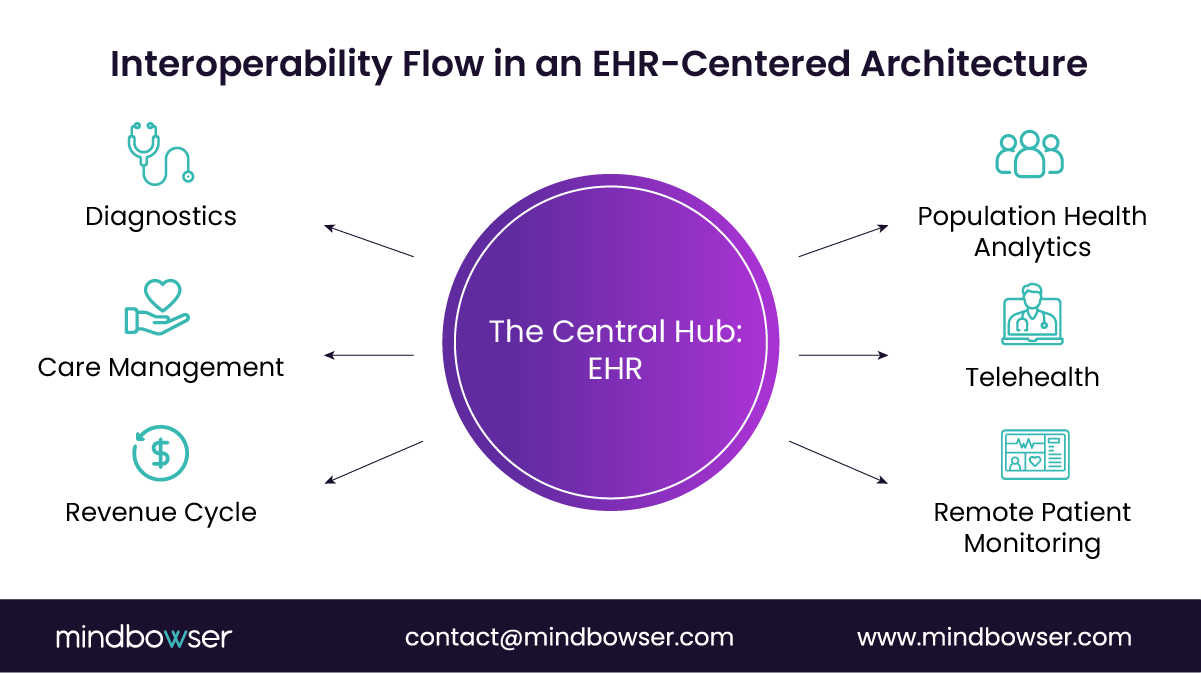
CoPilot coordinates workflows that span intake, care management, diagnostics, referrals, and population programs.
The platform supports:
- Routing of structured data to the right teams at the right time
- Alignment of clinical and operational steps across departments
- Reduction in manual follow-ups and cross-team communication gaps
This improves throughput and strengthens coordination across distributed care teams.
D. Readiness for Analytics, Reporting, and Population Health
By unifying data into a consistent model, CoPilot enables downstream systems to operate more effectively.
This supports:
- Enterprise analytics
- Population health programs
- Risk scoring and segmentation
- Reporting for value-based care
The organization gains a scalable data architecture that evolves with new care models.
E. Executive Takeaway
HealthConnect CoPilot gives provider organizations a practical way to reduce fragmentation, strengthen data exchange, and build a more integrated digital environment without replacing existing EMRs or EHRs
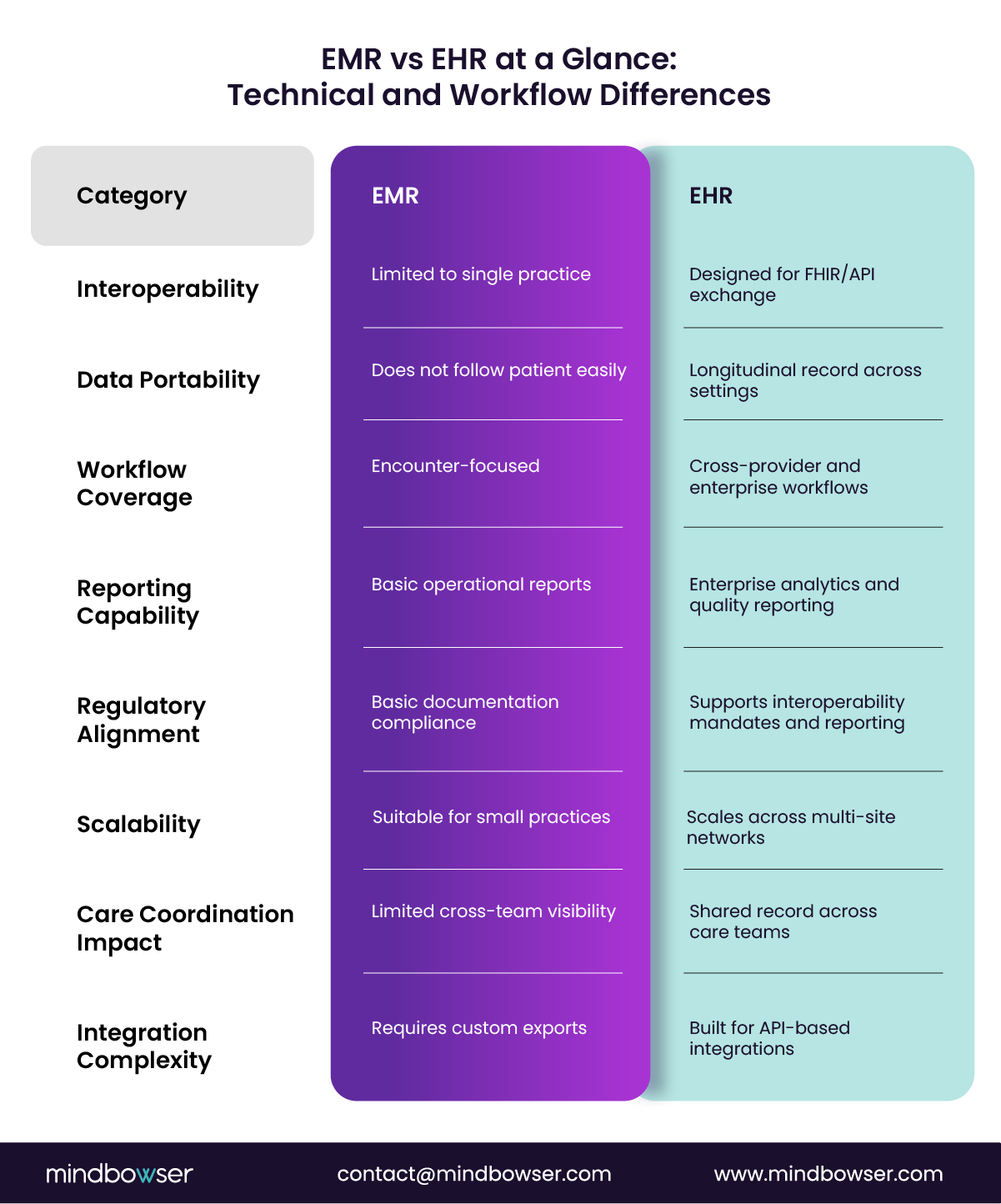
Think of EMRs as your digital filing cabinet for patient records—great for internal use but not very social. EHRs, on the other hand, are more like a patient’s online social profile, allowing for sharing and collaboration across different healthcare providers.
Absolutely! EMRs are best for tracking patient data within a single practice, like a trusty old notebook. EHRs, however, are designed to share that info across the healthcare universe, making them more of a global networking tool.
Imagine trying to throw a party without a guest list—chaos, right? EHR integration is like having an organized guest list that connects different healthcare systems, making patient care more coordinated and less like a game of telephone.
Sure thing! If your doctor uses an EMR, they might not know what’s going on with your care outside their office. With an EHR, it’s like your medical history has a VIP pass to all your healthcare providers, ensuring they’re all on the same page.
Look for blogs that don’t just list features but also explain them with real-world examples. A great EHR/EMR blog will make you chuckle while enlightening you on the quirks of different systems, turning dry facts into entertaining reads.