TL;DR
Wearable devices for burnout detection are helping hospitals and digital health teams measure clinician stress before it escalates. By analyzing signals such as heart rate variability (HRV), sleep quality, activity levels, and stress response, these devices create a physiological snapshot of workforce well-being. The promise is real: early detection, proactive intervention, and reduced turnover. Yet, without validation, privacy safeguards, and workflow alignment, these systems risk producing noise instead of actionable insight.
Burnout is no longer an individual problem; it’s a systemic risk that affects every layer of healthcare. The World Health Organization classifies burnout as an occupational phenomenon, and studies show that over 60% of clinicians report symptoms of emotional exhaustion. The ripple effects are serious—lower care quality, higher errors, and rising attrition costs.
In response, hospitals and digital health innovators are turning to wearable devices for burnout detection. These devices monitor continuous physiological signals to identify early signs of stress and fatigue. The idea is simple yet powerful: turn real-time data into early warnings before burnout reaches a breaking point.
However, precision in measurement does not always translate to accuracy in meaning. HRV dips, disrupted sleep, or low activity may signal fatigue, but they can also reflect temporary stress, lifestyle factors, or context-specific challenges. The future of burnout detection lies not in more sensors, but in validated insights that clinicians trust and leadership can act on.
I. Understanding the Physiology of Burnout
A. Translating Human Fatigue into Data
Burnout begins long before it is visible in performance reviews or patient outcomes. The earliest signals often live in the body. Heart Rate Variability (HRV) is one of the most reliable physiological markers of stress and recovery. A lower HRV indicates that the body is operating in a constant state of sympathetic activation, which over time leads to physical and emotional exhaustion.
Sleep quality provides another early clue. Fragmented or shortened REM sleep correlates strongly with cognitive fatigue and irritability. Over a sustained period, poor sleep predicts higher burnout risk, especially in shift-based roles.
Activity trends also reveal patterns of disengagement. When step counts drop and movement becomes irregular, it often mirrors decreased motivation and mental fatigue. Finally, stress index readings, derived from electrodermal activity or cortisol-linked data, offer real-time insight into the physiological toll of chronic stress.
Together, these metrics paint a biological portrait of burnout, translating subjective feelings of exhaustion into measurable data points that can inform timely interventions.

B. Devices Powering Burnout Insights
The growing ecosystem of wearables has made continuous monitoring practical and scalable across healthcare settings.
- Fitbit devices are used in several hospital wellness programs for longitudinal tracking of HRV, sleep, and recovery patterns.
- Oura Ring adds depth with precise sleep stage analytics and a readiness score that reflects overall recovery.
- Garmin offers advanced stress and activity monitoring, making it suitable for high-performance roles like emergency care staff.
- Apple Watch, through HealthKit, allows seamless integration with hospital EHR systems, enabling real-time monitoring within care dashboards.
Each of these devices provides continuous, objective insights into clinicians’ well-being. When connected to analytics platforms or EHRs, they shift well-being management from reactive surveys to proactive care grounded in data.
II. How Wearable Devices Detect Burnout
A. Continuous Monitoring and Correlation
Wearable devices for burnout detection work by collecting continuous physiological data and identifying deviations from an individual’s baseline. Instead of relying on self-reported fatigue surveys or episodic check-ins, these devices capture subtle physiological changes that often precede emotional exhaustion.
When heart rate variability declines over several consecutive days, or when sleep quality consistently worsens, the system can flag potential burnout risk. Combining HRV, sleep, and stress readings into a unified fatigue index allows healthcare organizations to track recovery trends, not just stress peaks.
This data-driven approach provides early warnings that leadership teams can act on. For instance, a sustained decline in readiness scores across a department could indicate scheduling stress or systemic overwork rather than isolated individual fatigue.
B. Data Flow and System Integration
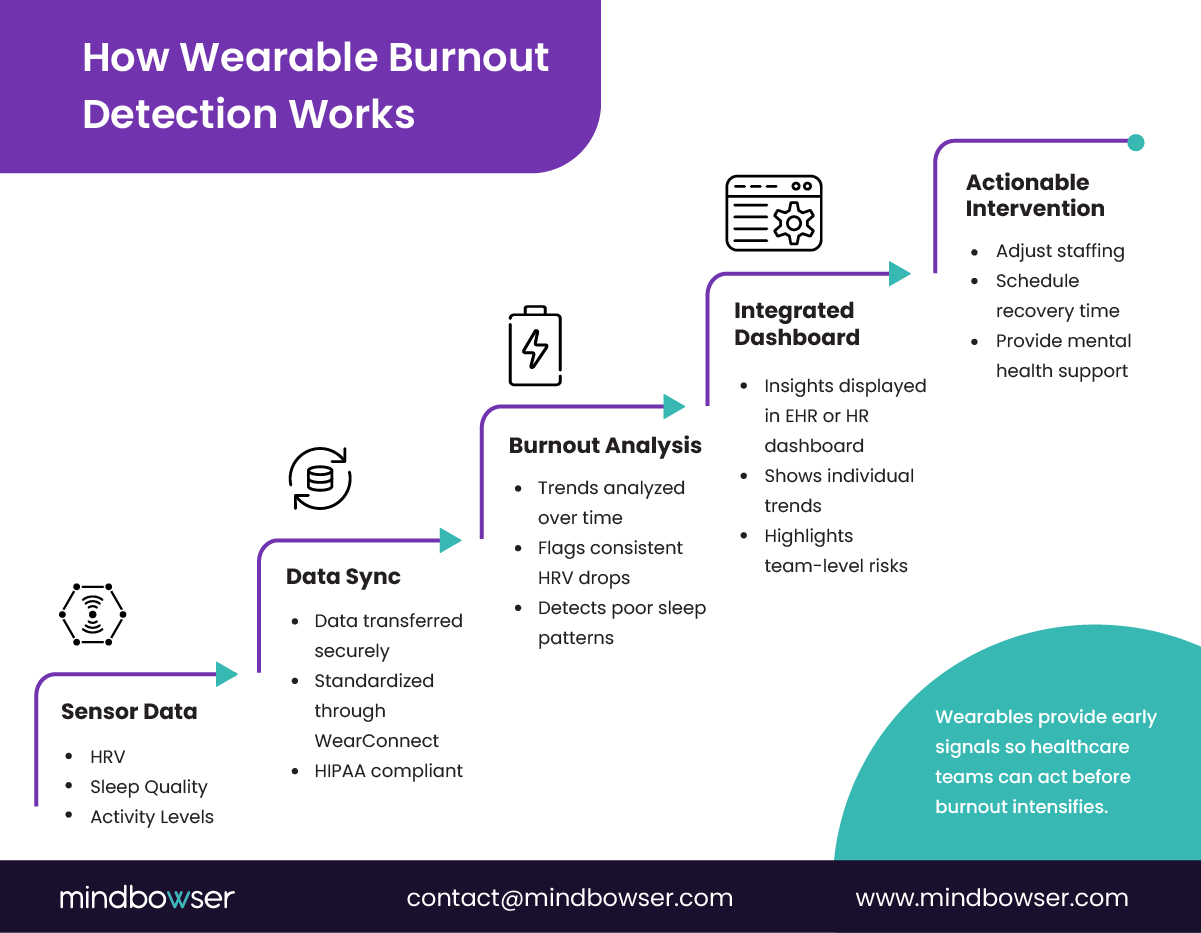
The true value of wearable devices for burnout detection lies in their integration within a broader digital health ecosystem. A typical workflow connects data from the device to analytics engines, then to EHR or HR dashboards where leaders can interpret the insights.
For example, wearable data can flow from Fitbit or Oura sensors to a unified analytics platform through integration tools like WearConnect. WearConnect aggregates data in real time, standardizes it across devices, and ensures compliance with privacy standards. From there, the data syncs into EHR systems to provide context, such as shift history or workload intensity.
Multi-sensor fusion further strengthens these insights. By correlating HRV, sleep, and activity data with contextual factors such as patient census or night shifts, the system can differentiate between temporary stress spikes and chronic burnout risks.
Ultimately, success comes not from more sensors but from seamless data flow, secure integration, and meaningful interpretation that clinicians and administrators can trust.

III. Validating Burnout Detection Models
A. Why Stress Is Not the Same as Burnout
A temporary spike in stress does not necessarily indicate burnout. Many clinicians perform under high stress yet remain highly engaged. Burnout occurs when stress becomes chronic, leading to emotional exhaustion and detachment.
Wearable devices for burnout detection often rely on physiological proxies such as HRV or sleep disruption. While valuable, these signals can misinterpret short-term stress as long-term fatigue if not contextualized. For instance, a surgeon’s HRV may drop during a high-intensity shift but recover quickly after rest. Without proper time-series analysis, this could be flagged incorrectly as burnout risk.
Accurate models must differentiate between acute stress (situational and recoverable) and chronic strain (persistent and harmful). Recognizing this difference is key to building tools that support clinicians instead of overwhelming them with false alerts.
B. Building Evidence-Based Models
Validated burnout detection requires more than wearable data. It needs clinical grounding. The Maslach Burnout Inventory (MBI) remains the benchmark for measuring emotional exhaustion, depersonalization, and reduced personal accomplishment. Integrating MBI scores with wearable-derived physiological data creates a robust dataset that blends subjective and objective measures.
Several ongoing studies have started correlating HRV patterns and sleep quality with validated burnout scores. These longitudinal studies help establish thresholds for meaningful change rather than relying on generic cutoffs. The result is a more personalized model that understands each clinician’s baseline.
Hospitals that combine validated instruments with wearable data are finding stronger predictive power and better acceptance from clinicians, who are more likely to trust tools backed by peer-reviewed evidence.
C. Ethical and Privacy Considerations
Trust is the foundation of successful burnout detection initiatives. Clinicians must believe their data will be used for support, not surveillance. Any deployment of wearable devices for burnout detection must clearly define ownership, access rights, and data-sharing boundaries.
Compliance with HIPAA and GDPR is non-negotiable. Data should be anonymized when aggregated for workforce analytics and encrypted at rest and in transit. Clear consent protocols help ensure clinicians understand what is tracked and why.
Ethical governance also includes transparency in how burnout scores influence decisions. The goal is to empower clinicians with insights, not penalize them. When handled responsibly, wearable data becomes a powerful ally in protecting the workforce rather than a monitoring tool that breeds mistrust.
IV. Integrating Burnout Detection into EHRs and Health Platforms
A. Contextualizing Wearable Data
For wearable devices for burnout detection to be truly effective, the data they collect must connect with clinical and operational systems. When wearable data sits in isolation, it only provides snapshots of stress or fatigue. Integrated into Electronic Health Records (EHRs), the same data becomes context-rich and actionable.
Linking wearable metrics such as HRV or sleep patterns with shift schedules, workload intensity, or patient volumes helps hospital administrators see how operational pressures affect clinician well-being. For example, an HRV decline across a department might coincide with extended shifts or increased patient admissions, allowing leadership to adjust staffing or rest schedules proactively.
Embedding burnout dashboards within EHR interfaces enables both individual clinicians and HR leaders to view insights in real time. Tools built on FHIR/HL7 APIs and SMART-on-FHIR frameworks make it possible to visualize wellness data alongside medical records securely and efficiently.
B. Compliance and Governance
Data integration in healthcare cannot happen without strict compliance. Mental health and wellness indicators collected through wearables are classified as sensitive health information under HIPAA and GDPR. This means every data exchange must follow encrypted transmission protocols and maintain clear consent documentation.
Hospitals implementing wearable burnout detection must also establish governance frameworks defining who can access the data and how it will be used. Access should be role-based and limited to those involved in workforce well-being or organizational health.
Beyond compliance, hospitals must commit to transparent data use. Clinicians should know how their information contributes to aggregate reports, what is anonymized, and how the insights will inform staffing or wellness programs. Trust is built not just through encryption, but through ethical intent clearly communicated from leadership.
V. The Promise and the Pitfalls
A. The Promise
Wearable devices for burnout detection are transforming how healthcare organizations understand and manage workforce well-being. They shift the focus from reactive surveys to continuous, real-time monitoring that helps identify early warning signs.
The first promise lies in early detection. By observing subtle declines in HRV or prolonged sleep disturbances, hospitals can intervene before burnout escalates. This data can support proactive scheduling adjustments, mental health check-ins, or workload balancing programs.
Second, wearable monitoring introduces objectivity. Instead of relying solely on self-assessment, administrators gain measurable indicators of stress and fatigue. These insights enable evidence-based well-being programs that can be linked to ROI outcomes such as reduced turnover and higher engagement.
Third, passive data collection makes the process non-intrusive. Clinicians do not need to fill surveys or report their mood; their devices quietly track physiological patterns. The resulting analytics empower HR, quality, and clinical leaders to identify system-level risks while preserving individual privacy.

B. The Pitfalls
Despite their promise, wearable systems are not flawless. The most common challenge is context blindness. A wearable can track physiological stress but cannot interpret emotional resilience, leadership dynamics, or organizational culture. A nurse’s HRV dip after a long shift may reflect dedication, not disengagement.
Another pitfall is data misinterpretation. Without clinical validation and longitudinal benchmarking, devices may trigger false alarms or overlook genuine burnout patterns. Overreliance on short-term metrics risks creating unnecessary anxiety or distrust.
Privacy concerns also remain significant. Clinicians must feel confident that their data will not be used for performance evaluation. Clear boundaries, consent mechanisms, and anonymized reporting are essential to maintain trust.
Finally, workflow misalignment often limits impact. Insights from wearables only drive change when they integrate with scheduling, HR, and EHR systems. Without actionable pathways, even the most advanced analytics end up as unread dashboards rather than meaningful well-being interventions.
Bridge Wearable Insights with HIPAA-Compliant EHR Integration
VI. The Road Ahead: Future of Burnout Detection
A. Multi-Modal Analytics
The next generation of wearable devices for burnout detection will not rely on a single data stream. Instead, multi-modal analytics will combine different biometric and behavioral signals to create a comprehensive view of mental and physical strain.
Emerging models integrate HRV, sleep, voice tone, and typing rhythm to identify subtle shifts in cognitive load and emotional state. For example, a combination of slower typing speed, monotone voice patterns, and poor sleep quality may indicate fatigue before it becomes burnout.
By analyzing multiple dimensions, these systems move closer to true behavioral intelligence, distinguishing between situational stress and sustained exhaustion. The more diverse the signals, the more reliable the insights—especially when combined with validated psychological assessments and contextual data such as workload or patient volume.
B. From Individuals to Organizations
The future of burnout detection will evolve from individual monitoring to organizational resilience mapping. Instead of focusing only on personal fatigue, hospitals will use aggregated, anonymized data to identify stress patterns across departments.
This shift enables leadership teams to visualize workforce well-being at scale. Heatmaps and trend dashboards can highlight where fatigue is highest, helping leaders adjust shift rotations, staffing levels, or patient assignments. For instance, if data shows rising stress levels in ICU units during certain weeks, administrators can deploy relief staff or modify workflows to prevent system-wide burnout.
At this stage, wearable data becomes a management tool for preventive workforce planning, not just individual recovery. The insights support strategic decisions that improve retention, patient safety, and overall care quality.
VII. How Mindbowser Can Help
Healthcare organizations exploring wearable devices for burnout detection often face three challenges: secure integration, compliance validation, and real-world usability. Mindbowser helps solve all three through proven engineering expertise and healthcare-specific accelerators.
Mindbowser builds compliant wearable ecosystems that combine device data, EHR connectivity, and AI-driven analytics into a unified well-being framework. The focus is on outcomes that matter—better clinician engagement, lower attrition, and measurable ROI.
Our WearConnect accelerator enables real-time device connectivity and data standardization across Fitbit, Oura, Garmin, and Apple HealthKit integrations. This shortens build time, ensures HIPAA-compliant data flow, and simplifies scalability across multiple devices and care settings.
For analytics and insights, AI Medical Summary transforms raw wearable and clinical data into usable dashboards that leadership teams can act on. By combining physiological metrics with validated burnout indices, hospitals gain visibility into workforce wellness while maintaining individual privacy.
From design to deployment, Mindbowser supports organizations in four key stages:
- Integration and Interoperability – Connecting wearables and health apps with EHR systems using SMART-on-FHIR and HL7 standards.
- Data Compliance – Ensuring HIPAA, GDPR, and SOC2 alignment for all data pipelines.
- Analytics Enablement – Building predictive and preventive wellness dashboards for clinicians and administrators.
- Validation and Scaling – Testing models against clinical standards like the Maslach Burnout Inventory to ensure accuracy and trust.
Mindbowser’s work with health systems and digital health startups has demonstrated tangible outcomes, including faster validation cycles, higher clinician engagement, and reduced operational fatigue. For hospitals investing in workforce well-being or startups building next-generation burnout detection tools, Mindbowser provides the engineering foundation to make those initiatives secure, scalable, and effective.

Conclusion
Wearable devices for burnout detection represent one of the most practical intersections of digital health innovation and workforce resilience. They bring precision to what was once subjective, allowing hospitals and digital health organizations to recognize fatigue before it compromises care. The technology offers measurable progress: better engagement, lower absenteeism, and early intervention for at-risk clinicians.
However, the success of these systems depends on responsible implementation. Accuracy without validation is noise. Data without privacy is a risk. Insights without workflow integration are unused. To deliver meaningful value, organizations must build frameworks that combine validated physiology, trusted governance, and actionable analytics.
Burnout prevention is not achieved by tracking stress alone. It requires a partnership between data, design, and empathy. The best technology solutions are those that protect the clinician’s well-being while strengthening the organization’s capacity to deliver high-quality care.
Wearable devices for burnout detection are not the end goal—they are the beginning of a more informed, humane, and sustainable approach to healthcare.
Yes, if implemented correctly. Wearable data related to clinician health or mental well-being qualifies as Protected Health Information (PHI) under HIPAA. Hospitals and startups using wearable devices for burnout detection must ensure encrypted data transfer, secure storage, and explicit consent from users. Platforms that integrate with EHRs through standards like FHIR or SMART-on-FHIR must also follow strict access control and audit protocols.
HRV is one of the most studied indicators of physiological stress, but it does not measure burnout on its own. Accuracy improves when HRV data is combined with sleep, activity, and behavioral trends over time. The most reliable systems use validated benchmarks such as the Maslach Burnout Inventory (MBI) alongside wearable data to minimize false positives and personalize thresholds.
Yes. Wearable data can integrate with EHR systems through FHIR/HL7 APIs and SMART-on-FHIR applications. Tools like Mindbowser’s WearConnect simplify this process by standardizing device data and ensuring compliance. Integration allows burnout insights to appear directly within clinician dashboards, making well-being tracking a natural part of daily workflows.
Hospitals implementing validated burnout detection platforms report measurable ROI through improved retention, lower sick leave, and reduced overtime costs. By preventing burnout-related turnover, organizations can save an estimated $250,000 to $500,000 per physician annually, depending on specialty. In digital health environments, these systems also accelerate clinical validation, improve product engagement, and reduce churn.
Adoption depends on transparency and trust. Clinicians are more likely to engage when data is used to support well-being rather than evaluate performance. Programs that emphasize privacy, voluntary participation, and data ownership consistently show higher engagement and sustained participation over time.
































