TL;DR
- RCM automation replaces manual tasks with intelligent workflows across the revenue cycle.
- Speeds up processes like eligibility checks, claims submission, and payment posting.
- Reduces errors and boosts claim acceptance with AI-driven validation and coding.
- Improves cash flow by minimizing denials and shortening accounts receivable (A/R) cycles.
- Addresses staffing shortages by freeing teams from repetitive work.
- Strengthens compliance through audit-ready logs and real-time regulatory updates.
- Essential for value-based care, where financial accuracy and speed directly impact sustainability.
Managing finances in healthcare isn’t just about balancing books—it’s about keeping the entire system running smoothly. Yet, the revenue cycle remains one of the most complex and error-prone parts of the process. Manual workflows, repetitive tasks, and delayed claims can quietly drain time, energy, and money from already stretched teams.
That’s where revenue cycle management automation steps in. By replacing slow, manual steps with smart, rule-based automation, teams can process claims more efficiently, minimize human error, and maintain control over financial outcomes. No more chasing denials or fixing costly mistakes after the fact.
The result? A faster, cleaner revenue cycle with fewer rejections, improved cash flow, and happier teams. With automation doing the heavy lifting, healthcare organizations can redirect focus where it belongs—on delivering quality care, not battling spreadsheets.
Automating manual billing workflows isn’t just about speeding up processes—it’s about freeing up teams to focus where it counts. As Patrice Wolfe, CEO of AGS Health, puts it,
Watch: Revenue Cycle Management Automation (How It Reduces Denials & Speeds Up Cash Flow)
What is Revenue Cycle Management Automation?
Revenue Cycle Management (RCM) automation refers to the use of technology to automate tasks across the revenue lifecycle, eliminating the need for manual input. It replaces time-consuming steps, such as data entry, eligibility checks, and claim submission, with automated workflows, thereby reducing the likelihood of human error and streamlining the process.
As Alan Hester, President at Nividous, points out in our HealthTech with Purpose podcast series:
1. Scope of Automation Across the Revenue Lifecycle
RCM automation can span nearly every phase of the revenue cycle, including:
- Patient registration and eligibility verification
- Charge capture and medical coding
- Claims creation, submission, and tracking
- Denial management and appeals
- Payment posting and reconciliation
- Patient billing and follow-ups
Each step, when automated, contributes to smoother operations and faster revenue realization.
At Banner Health, automation isn’t theoretical it’s operational. As Adrienne Moore shares:
2. Key Technologies Involved
Several technologies power RCM automation, each designed to streamline specific processes:
- Robotic Process Automation (RPA): Handles repetitive tasks like data extraction, claim status checks, and EOB reconciliation.
- Artificial Intelligence (AI) and Machine Learning (ML): Learn from patterns to predict denials, suggest coding improvements, and optimize workflows.
- Natural Language Processing (NLP): Converts unstructured clinical notes into structured codes or billing information.
- Optical Character Recognition (OCR): Digitizes paper records, insurance cards, and forms into machine-readable data.
- API and System Integrations: Seamlessly connect billing, EHR, clearinghouses, and payer systems to eliminate silos and reduce friction.
Related read: A Guide to Healthcare Revenue Cycle Management
Why Is Revenue Cycle Management Automation Critical in Modern Healthcare?
Automation isn’t just a convenience in revenue cycle management—it’s becoming a necessity. As the complexity of healthcare billing increases, so do the operational challenges that hinder revenue collection and heighten the risk of errors. Automation directly addresses these issues with speed, accuracy, and scalability.
1. Rising Administrative Costs and Staffing Shortages
Manual revenue processes require significant workforce. With ongoing staffing shortages, particularly in back-office operations, healthcare teams face increasing pressure to do more with fewer resources.
2. Fragmented Manual Workflows Causing Delays
Disjointed systems and siloed data lead to bottlenecks. Whether it’s waiting on prior authorizations or manually checking insurance eligibility, these delays pile up across the revenue cycle.
As Mark Scrimshire, the Chief Interoperability Officer at Onyx Health, notes:
3. High Claim Denial Rates and Rework Burden
Every rejected or denied claim adds extra work. When staff must manually review and correct errors, it eats into productivity and further delays payments.
4. Regulatory Pressures and Compliance Risks
Billing errors can lead to compliance issues and financial penalties. Keeping up with evolving payer rules and coding updates requires a level of consistency that automation can ensure.
5. The Push for Value-Based Care and Financial Sustainability
As healthcare shifts toward outcome-based reimbursement, organizations must manage their financial operations with precision. Automation helps maintain cash flow while adapting to new reimbursement models.
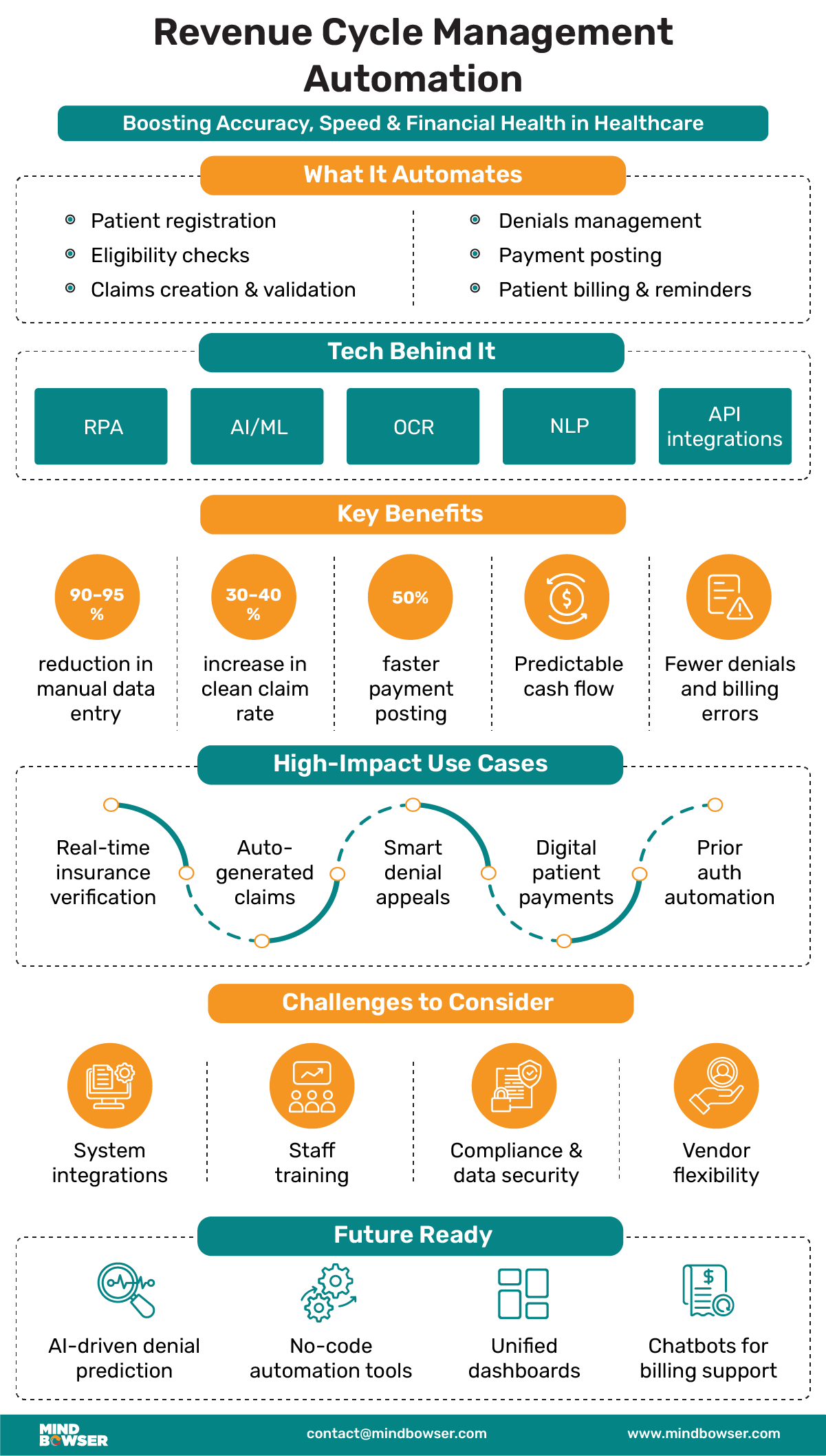
Benefits of Revenue Cycle Management Automation
Implementing automation across the revenue cycle brings measurable improvements in accuracy, speed, and team efficiency. By reducing manual work, healthcare organizations can focus on financial health while minimizing disruptions in billing and collections.
1. Fewer Errors and Rejections
- Eliminates manual data entry errors: Automation pulls accurate data from integrated systems, reducing typos and mismatches.
- Increases claim acceptance rates: Clean claims lead to fewer rejections and faster payments.
- Boosts accuracy in coding and documentation: AI and NLP help validate documentation and suggest proper codes.
2. Faster Turnaround on Claims and Payments
- Accelerates pre-authorization, claim submission, and payment posting: Tasks that typically take days can be completed in minutes.
- Speeds up insurance verification and eligibility checks: Instant access to payer data avoids back-and-forth delays.
3. Predictable and Optimized Cash Flow
- Real-time tracking of receivables: Know what’s outstanding and what’s been paid without digging through spreadsheets.
- Reduction in days in accounts receivable (A/R): Shorter revenue cycles lead to better financial stability.
4. Higher Productivity Across Teams
- Frees up staff for strategic tasks: Less time spent on manual work allows teams to focus on resolving complex issues.
- Reduces burnout from repetitive tasks: Automation eases workloads and improves staff satisfaction.
Automation embedded in clinical workflows has reduced lab ordering time by as much as 85%, minimizing delays and easing clinician workload. Elsewhere, cloud infrastructure optimization resulted in a 30–40% cost reduction, redirecting resources toward patient-facing priorities.
5. Stronger Regulatory and Audit Readiness
- Maintains detailed logs and audit trails: Every action is traceable, which simplifies audits.
- Keeps pace with evolving billing and coding standards: Automation platforms update automatically with new compliance rules.
In healthcare, compliance demands precision and speed. One maternal health platform used automation to achieve SOC 2 Type 2 audit readiness in just three weeks—cutting prep time by 30% compared to industry norms.
Let’s Talk About Automating Your Revenue Cycle
Tired of rework, delays, and missed reimbursements? Let’s explore how automation could improve your bottom line.
High-Impact Use Cases for Revenue Cycle Management Automation
Automation isn’t just a broad concept—it delivers concrete value when applied to specific, high-volume, and error-prone tasks. These are the areas where automation can have the most significant impact on day-to-day revenue operations.
1. Patient Pre-Registration and Scheduling
- Auto-fill forms using EHR and insurance data to reduce duplicate entry
- Validate demographics and insurance info upfront to prevent delays later
2. Real-Time Eligibility and Benefit Checks
- Connects to payer APIs for instant insurance verification
- Confirms coverage details before services are rendered to avoid claim denials
3. Claims Creation and Validation
- Auto-generates clean claims with accurate codes, modifiers, and documentation
- Performs validation checks before submission to ensure compliance with payer rules
4. Denials Management and Appeals
- Flags common denial trends and automatically routes them for appeal
- Prepares appeal packages based on predefined workflows and documentation requirements
5. Payment Posting and Reconciliation
- Matches EOBs and remittances to charges with high accuracy
- Posts payments and adjustments in real-time to the billing system
6. Prior Authorization Automation
- Submits and tracks prior auth requests automatically through payer portals
- Triggers reminders or escalations if approval is delayed
7. Patient Billing and Collections
- Sends timely reminders via email, SMS, or patient portal notifications
- Enables digital payment options and auto-setups for installment plans
8. Reporting and Analytics
- Tracks performance KPIs like denial rates, clean claim ratios, and A/R days
- Highlights revenue leakage points and recommends process improvements
Related Read: Comprehensive Guide to the RCM Process in Healthcare
Steps to Implement RCM Automation Successfully
Rolling out revenue cycle management automation isn’t just about buying software—it requires careful planning, team alignment, and continuous improvement. Here’s how to approach implementation the right way:
1. Audit Your Current Revenue Cycle Processes
Start by identifying bottlenecks, error-prone tasks, and redundant workflows. Mapping the existing process helps reveal areas ripe for automation.
2. Identify Repetitive, Rules-Based Tasks for Automation
Look for tasks like data entry, claim status checking, or eligibility verification that follow repeatable patterns.
3. Set Clear Goals
Define what success looks like—such as reducing A/R days by 20% or increasing the clean claim rate by 30%. Clear KPIs help measure progress.
4. Select Automation Tools That Integrate With Your Systems
Choose platforms that work with your billing software, EHR, and payer portals. Compatibility ensures a smoother rollout and less disruption.
5. Run Pilot Programs in Specific Departments
Start small with a test group or workflow to gauge the effectiveness of your approach. Proving success in one area helps secure buy-in for broader rollout.
6. Train Staff and Build Cross-Functional Automation Champions
Prepare your team for changes with training and support. Having internal champions can accelerate adoption.
7. Monitor and Optimize Post-Implementation Metrics
Track KPIs continuously, gather feedback, and refine automation rules to maintain high performance.
Key Challenges to Watch Out For
While revenue cycle management automation brings substantial benefits, it’s important to plan for the common challenges that can arise during implementation and scaling.
1. Complex EHR and Billing System Integrations
Many healthcare systems run on legacy platforms. Integrating automation tools with these systems can be technically demanding without the right APIs and middleware.
2. Concerns About Data Security and HIPAA Compliance
Automation deals with sensitive financial and patient data. Every tool must meet HIPAA requirements and ensure data is encrypted, access-controlled, and auditable.
3. Change Management Resistance From Staff
Team members may be hesitant to trust automation or fear job displacement. Clear communication, training, and showing how automation supports their work are essential.
4. Maintaining Accuracy During Transition Phases
Initial implementation phases can experience hiccups if workflows aren’t clearly defined or thoroughly tested. Continuous monitoring helps avoid costly mistakes.
5. Vendor Lock-In and Lack of Interoperability
Some automation platforms limit flexibility. Choosing systems that follow open standards and support third-party integrations will help avoid long-term restrictions.
Future Outlook for Revenue Cycle Management Automation
The future of revenue cycle automation goes beyond basic task automation. New technologies are pushing boundaries and helping healthcare organizations become more proactive, data-driven, and patient-friendly in their financial operations.
1. AI-Driven Predictive Analytics for Denial Prevention
Instead of reacting to denials, future systems will predict and prevent them. AI models can analyze historical data to flag claims likely to be rejected and recommend fixes before submission.
2. Conversational AI for Patient Billing Queries
Chatbots and virtual assistants will handle common billing questions, explain charges, and guide patients through payment options, freeing up support teams for complex issues.
3. Unified Dashboards Across Payers and Systems
Expect centralized views that consolidate claim statuses, financial performance, and patient billing insights across platforms, enabling real-time decision-making.
4. NLP for Intelligent Coding Suggestions
Natural Language Processing will help translate clinical notes into accurate billing codes, reducing the need for manual coder review and improving first-pass accuracy.
5. No-Code/Low-Code Platforms for Automation Customization
Non-technical users will soon be able to customize workflows without developer support, enabling faster iteration and better alignment with evolving billing practices.
Innovations like automated document parsing and real-time medical data processing are expanding the reach of automation from revenue tasks to clinical decision support and diagnostic operations.
See How It’s Working in the Real World
Want to see how healthcare organizations are reducing admin costs and improving reimbursement speed?
How Mindbowser Can Help
At Mindbowser, we help healthcare organizations simplify and modernize their revenue cycle through smart automation. Whether you’re looking to reduce claim denials, expedite collections, or integrate your EHR and billing systems, our team brings the right combination of healthcare expertise and technical skills to make it happen.
We specialize in:
- Custom RCM automation solutions that fit your workflows
- Integration with EHRs like Epic EHR, Cerner EHR, and Athenahealth EHR
- API-driven eligibility checks, claim scrubbing, and payment reconciliation
- Dashboards for real-time RCM insights and analytics
- HIPAA-compliant architectures built for scale and security
With proven experience in healthcare tech and platforms like HealthConnect CoPilot, we ensure your automation journey is compliant, effective, and future-ready. Whether you’re automating one step or the entire cycle, Mindbowser helps you move fast, without breaking things.

Conclusion
Revenue cycle management automation revolutionizes how healthcare organizations manage their financial operations. It reduces errors, speeds up collections, and creates predictable revenue streams by automating time-consuming tasks, such as claims processing, eligibility checks, and payment posting.
Beyond efficiency, automation helps teams stay audit-ready, maintain compliance, and focus their time on more strategic work. As healthcare continues to evolve, adopting smart automation is no longer optional—it’s essential for financial stability and long-term growth.
Revenue cycle management automation refers to the use of technologies like AI, RPA, and system integrations to automate repetitive financial workflows in healthcare. It replaces manual tasks such as eligibility checks, claims submission, and payment posting with automated processes, improving speed and accuracy.
Automation improves revenue cycle management by reducing errors, accelerating claims processing, and improving cash flow. It helps validate claims before submission, lowers denial rates, and provides real-time visibility into financial performance, enabling faster and more accurate decision-making.
Almost all stages, including insurance verification, claims creation, billing, denial management, payment posting, and patient communications.
Yes. It improves coding accuracy and performs eligibility checks up front, which significantly lowers rejection rates.
Most modern RCM automation platforms are built to integrate with existing systems using APIs or middleware solutions.
Savings from fewer reworks, faster reimbursements, and reduced administrative effort often lead to a strong return on investment within a few months of deployment.




















 BLOGS
BLOGS  NEWSROOM
NEWSROOM  CASE STUDIES
CASE STUDIES  WEBINARS
WEBINARS  PODCASTS
PODCASTS  ASSET HUB
ASSET HUB  EVENT CALENDAR
EVENT CALENDAR 





















