TL;DR
Clinical decision support system implementation is not just a software purchase. Hospitals must budget for integration engineering, clinical governance, workflow redesign, and ongoing optimization, in addition to the cost of clinical decision support software. A sustainable CDS program requires clear budgeting across capital, operational, and clinical time investments while linking initiatives to measurable outcomes such as patient safety, reduced length of stay, and improved value-based care performance. When planned correctly, CDS becomes a long-term clinical capability that improves care quality while protecting hospital margins.
It often starts with a quality report. A medication safety event. A delayed diagnosis. A treatment pathway that wasn’t followed consistently.
Someone inevitably says, “We need stronger decision support in the EHR.”
But the moment clinical decision support system implementation enters the conversation, the focus shifts to a different challenge: how hospitals should actually budget for it. For a more detailed understanding of the various types of Clinical Decision Support Systems (CDSS), please refer to our comprehensive overview of different types of CDSS
The challenge is that clinical decision support is rarely just a technology purchase. It is a multi-year operational capability that touches clinical workflows, governance structures, and hospital finances.
Watch Before You Invest in Clinical Decision Support System Implementation
I. Start With the Budget Model, Not the Vendor Quote
Hospitals often begin implementing clinical decision support systems by reviewing vendor proposals. That is backwards. The first step should be to define what decision support will do operationally within the hospital and how it will generate measurable value.
Without that clarity, budgets become software line items instead of sustainable clinical programs.
A. Define “Clinical Decision Support System Implementation” for your hospital
A clinical decision support system implementation is not simply turning on alerts in an electronic health record. It is the structured deployment of guidance tools that influences clinician decisions during care delivery.
Operationally, CDS can include:
- Order sets that standardize treatment pathways
- Care pathways embedded into clinical workflows
- Documentation templates that reinforce compliance and quality reporting
- Inbox nudges that prompt follow-up actions
- Medication safety checks and utilization guidance
These tools are typically delivered through clinical decision support software integrated directly into EHR workflows.
Hospitals planning the implementation of a clinical decision support system must also choose how the technology will be delivered. Three delivery models dominate the market today:
- EHR-native decision support built directly within the EHR platform
- EHR-embedded decision engines connected through integration frameworks
- Standalone CDS platforms that integrate through APIs or interoperability standards
Each approach has implications for customization, integration effort, and long-term maintenance.
Just as important is defining what success looks like before implementation begins. A hospital’s clinical decision support system implementation should link directly to strategic goals such as:
- Improving patient safety and reducing preventable harm
- Increasing adherence to evidence-based care pathways
- Improving throughput and reducing treatment delays
- Supporting value-based care performance
- Reducing unnecessary utilization and variation in care
Without clear outcome targets, CDS programs drift toward alert fatigue rather than measurable improvement.
CDS Delivery Models Hospitals Must Evaluate
| Delivery Model | Description | Pros | Limitations |
|---|---|---|---|
| EHR-Native CDS | Built directly within the EHR platform | Deep workflow integration | Limited customization |
| EHR-Embedded CDS | External CDS engine embedded within EHR workflows | Flexible decision logic | Integration complexity |
| Standalone CDS Platform | Independent decision support engine integrated via APIs | Highly customizable | Requires strong interoperability |
B. Separate capital, operating, and clinical time costs upfront
A successful clinical decision support system implementation requires a budgeting structure that reflects how the program actually operates.
Most hospitals underestimate the labor intensity of CDS deployment. Integration engineers, clinical informatics specialists, and service-line physicians all contribute time before the first alert or order set reaches production.
Budget planning should therefore separate three cost categories:
1. Capital investment
- Discovery and workflow mapping
- Integration engineering
- CDS rule configuration
- Testing and go-live preparation
2. Operational costs
- Software licensing
- Platform hosting and monitoring
- Ongoing integration maintenance
- Content updates and optimization cycles
3. Clinical time costs
- Physician validation of rules and order sets
- Governance committee meetings
- Continuous monitoring of alert performance
A clinical decision support system implementation is rarely owned by IT alone. Budget ownership typically spans:
- IT and integration teams
- Clinical informatics
- Quality improvement leadership
- Pharmacy and medication safety
- Service-line medical leadership
- Finance and population health teams
Because CDS evolves as clinical pathways change, most organizations should budget on a multi-year model that includes subscription costs plus continuous optimization work.
Hospitals that treat CDS as a one-time deployment often discover that the real work begins after go-live.
| CDS Type | Budget Range | Description |
|---|---|---|
| Custom CDS Hooks Integration | $75K – $150K | Tailored integration with specific clinical workflows and data sources. |
| AI-powered CDS Platform | $200K – $500K | Advanced decision support leveraging AI and machine learning for personalized recommendations. |
| Basic CDS Integration | $50K – $100K | Standard integration with pre-defined rules and protocols. |
| Enterprise-Level CDS | $300K – $1M+ | Full-scale enterprise implementation for large health systems with complex needs. |
C. Tie CDS to value-based care and margin protection
Finance committees approve budgets when the operational value is clear. CDS programs must therefore be framed in both financial and clinical terms.
Modern clinical decision support software contributes to margin protection in several ways:
- Preventable harm reduction, which lowers the cost of adverse events
- Reduced clinical variation, which improves supply utilization and pharmacy management
- Shorter length of stay, freeing bed capacity, and increasing throughput
- Improved documentation and compliance, which support accurate reimbursement
Hospitals that approach clinical decision support system implementation as a safety, quality, and financial strategy rather than a technology project tend to build stronger executive alignment.
The budget model should begin with value creation, then work backward to the technology and staffing required to achieve it.
II. The Hidden Cost Drivers of Clinical Decision Support
Hospitals rarely underestimate the cost of clinical decision support software itself. The real surprises appear elsewhere.
Integration engineering, terminology normalization, clinical validation, and governance structures often represent the largest share of the clinical decision support system implementation budget. These are operational capabilities, not vendor deliverables.
Executives planning the implementation of a clinical decision support system should therefore evaluate the hidden cost drivers early in the budgeting process.
A. Integration architecture drives most implementation complexity
The most underestimated cost in implementing a clinical decision support system is integration.
Clinical decision support does not function in isolation. It depends on patient context, orders, medications, diagnoses, lab values, and care pathways. All of this information must flow reliably between systems in real time.
Modern healthcare decision support software often integrates through:
- FHIR APIs
- CDS Hooks frameworks
- HL7 messaging interfaces
- Terminology services for standardized clinical vocabularies
Each integration point requires engineering effort, testing cycles, and ongoing maintenance.
For example, medication safety CDS may require data feeds from:
- The EHR order entry system
- Pharmacy dispensing systems
- Medication knowledge bases
- Laboratory systems for renal dosing adjustments
Without a clean interoperability architecture, CDS logic fails or produces unreliable alerts.
Hospitals planning clinical decision support system implementation should therefore evaluate:
- API maturity of their EHR platform
- Availability of interoperability standards such as CDS Hooks
- Internal integration engineering capacity
For a deeper look at how CDS logic connects to real clinical workflows inside the EHR, including how decision support engines use CDS Hooks and interoperability APIs to deliver real-time guidance to clinicians, see this technical walkthrough.
Integration complexity often determines the true timeline and cost of implementing a clinical decision support system.
B. Terminology mapping and clinical logic validation require significant clinical time
Decision support systems depend on structured clinical data.
Diagnoses, medications, procedures, and lab values must all be mapped to standardized vocabularies such as:
- SNOMED CT
- LOINC
- RxNorm
- ICD-10
This mapping ensures that CDS rules trigger consistently across different workflows and patient populations.
During clinical decision support system implementation, hospitals typically must perform:
- terminology normalization
- mapping of order sets to coded concepts
- validation of rule triggers and thresholds
These activities require oversight by physicians and clinical informatics.
A common scenario illustrates the challenge.
A sepsis alert rule may depend on:
- lactate values
- vital sign thresholds
- infection diagnoses
- antibiotic ordering patterns
Each variable must be validated against real patient records to ensure the CDS rule fires appropriately.
Clinical review cycles often include:
- Evidence review
- Clinical pathway alignment
- Simulation testing using historical patient data
- Physician sign-off before activation
These governance steps protect patient safety but add significant time to the implementation of clinical decision support systems.
C. Adoption support and alert fatigue management must be budgeted early
Technology alone does not change clinical behavior.
Clinicians quickly ignore CDS alerts that interrupt workflow or appear clinically irrelevant. Alert fatigue remains one of the biggest risks in the implementation of clinical decision support systems.
Hospitals, therefore, must invest in adoption strategies that include:
- clinician co-design of decision logic
- careful selection of interruptive vs. passive guidance
- monitoring of alert acceptance rates
- continuous rule refinement
Successful CDS programs typically establish a formal governance structure with representatives from:
- clinical informatics
- pharmacy
- quality improvement
- service-line leadership
This governance body evaluates alert performance and prioritizes rule updates.
Without these processes, healthcare decision support software becomes cluttered with outdated alerts and conflicting rules.
Adoption support should therefore be treated as an ongoing operational cost rather than a one-time implementation activity.
The most expensive part of implementing a clinical decision support system is not the technology. It is the clinical, technical, and governance infrastructure required to keep decision support relevant and trusted by clinicians.
Planning a Clinical Decision Support System Implementation?
III. Building a Finance-Ready Budget for CDS Programs
Hospital executives approving technology investments want clarity on three questions: What will this cost, who owns the program, and what value will it generate?
A clinical decision support system implementation requires a structured financial model that accounts for technical build work, ongoing operations, and the clinical governance needed to sustain the program.
Hospitals that treat clinical decision support system implementation as a multi-year operational capability tend to avoid the budgeting gaps that derail many CDS initiatives.
A. Map all cost categories before vendor negotiations
Vendor quotes typically represent only a fraction of the true cost of implementing a clinical decision support system. The full budget must include implementation labor, operational support, and clinician participation.
A practical way to structure budgeting for the implementation of a clinical decision support system is to categorize costs into four areas.
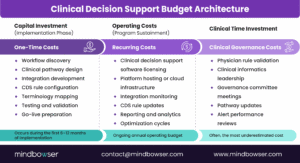
1. One-time implementation costs
These expenses occur during the initial deployment phase and include technical and workflow design activities:
- CDS discovery and use-case prioritization
- Workflow mapping and clinical pathway design
- Integration development and API configuration
- Rule logic development and validation
- Testing cycles and go-live preparation
- Clinician training and rollout support
These activities often require both external expertise and internal staff time.
2. Recurring operational costs
Once live, clinical decision support software requires ongoing maintenance and governance.
Recurring costs may include:
- Annual software licensing or subscription fees
- Platform hosting or cloud infrastructure
- Integration monitoring and maintenance
- Continuous rule updates and optimization
- Reporting and performance monitoring
Hospitals that underestimate these operational costs often struggle to sustain their clinical decision support system implementation programs.
3. Clinical time investment
CDS success depends on clinician leadership.
Budget models should allocate time for:
- physician informatics oversight
- rule validation committees
- service-line governance meetings
- clinical pathway updates
Physician time spent validating CDS logic is often one of the highest hidden costs of clinical decision support system implementation.
4. Contingency and expansion capacity
Hospitals frequently expand CDS programs after early success. New service lines, additional quality initiatives, or regulatory requirements may require new rule sets.
Including a contingency budget allows organizations to scale clinical decision support software without restarting the budget process.
Budget Categories for Clinical Decision Support System Implementation
| Budget Category | Example Cost Components |
|---|---|
| One-Time Costs | Discovery, workflow mapping, integration build, testing, training, and go-live. |
| Recurring Costs | Software licenses, hosting, governance time, monitoring, and content updates. |
| Clinical Time Costs | Physician validation, informatics oversight, and governance meetings. |
| Contingency Budget | Integration surprises, service-line expansion, and de-implementation costs. |
B. Plan a phased investment rather than a single deployment
Many hospitals attempt to deploy large CDS programs all at once. This approach often overwhelms clinical teams and increases the risk of implementation.
A more sustainable strategy for implementing a clinical decision support system is phased deployment.
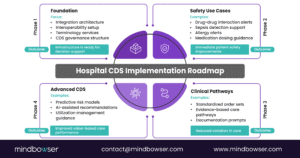
Typical phases include:
Phase 1: Foundational infrastructure
- CDS integration architecture
- terminology services
- governance structure
Phase 2: High-impact safety rules
- medication safety alerts
- sepsis detection workflows
- high-risk drug interactions
Phase 3: Clinical pathway support
- standardized order sets
- care pathways for high-volume conditions
- documentation support tools
Phase 4: Advanced decision intelligence
- predictive risk models
- utilization management guidance
- AI-assisted recommendations
This phased model spreads investment over multiple years and allows hospitals to demonstrate early value from healthcare decision support software.
It also gives clinicians time to adapt workflows before introducing more advanced capabilities.
C. Define measurable success metrics before implementation
Finance committees expect technology investments to show measurable results.
Hospitals implementing clinical decision support systems should therefore establish success metrics before deployment begins.
Metrics typically fall into three categories: clinical outcomes, operational efficiency, and financial impact.
For example, CDS programs supporting sepsis protocols might measure:
- time to antibiotic administration
- sepsis mortality rates
- ICU utilization
Medication safety CDS might measure:
- adverse drug event reduction
- pharmacy intervention rates
- medication cost per case
Operational CDS may track:
- length of stay
- discharge efficiency
- clinician documentation time
These metrics demonstrate how healthcare decision support software contributes to both quality improvement and financial sustainability.
CDS Program Success Metrics
| Category | Example Metrics |
|---|---|
| Clinical | Harm event reduction, pathway adherence, time-to-treatment. |
| Operational | Length of stay, throughput, clinician time, alert burden. |
| Financial | Avoidable utilization, pharmacy savings, margin per case, readmission penalties. |
Hospitals that define these metrics early create stronger accountability across clinical, IT, and finance teams.
Clinical decision support system implementation should begin with a clear financial structure and measurable outcomes. When budgeting aligns with operational reality, CDS programs become sustainable engines for safety, efficiency, and value-based care performance.
Build a Scalable Clinical Decision Support System
IV. Governance, Optimization, and Long-Term Value Realization
The long-term success of clinical decision support system implementation depends on governance, continuous optimization, and measurable outcomes.
Hospitals that treat CDS as a living clinical program tend to see sustained improvements in safety, utilization, and financial performance. Those who treat it as a one-time deployment often experience alert fatigue, declining clinician trust, and outdated rules.
Strong governance ensures that the implementation of clinical decision support systems remains aligned with evolving clinical evidence, operational goals, and value-based care requirements.
A. Establish a formal CDS governance structure
Decision support affects clinical behavior across nearly every department. Governance structures must therefore include representation from multiple hospital functions.
A typical CDS governance framework includes:
1. Clinical leadership
- Chief Medical Information Officer (CMIO)
- Service-line physician champions
- Nursing informatics leadership
2. Operational leadership
- Quality improvement teams
- Pharmacy leadership
- Population health management
3. Technical leadership
- IT architecture and interoperability teams
- Clinical informatics specialists
- Data analytics teams
This governance group typically meets monthly or quarterly to evaluate CDS performance and prioritize rule updates.
Common governance responsibilities include:
- reviewing alert acceptance and override rates
- approving new CDS rules or care pathways
- retiring low-value or outdated alerts
- aligning CDS with quality initiatives and regulatory programs
Without governance oversight, even the best clinical decision support software gradually loses relevance.
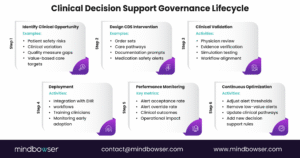
B. Monitor alert performance and clinician trust
Alert fatigue is one of the most common failure points in the implementation of clinical decision support systems.
If clinicians encounter too many irrelevant alerts, they quickly develop the habit of overriding or ignoring them. Over time, this behavior erodes trust in decision support tools.
Hospitals should therefore track several operational indicators for CDS performance:
- alert acceptance rates
- alert override rates
- clinician feedback and satisfaction
- alert firing frequency per encounter
High-performing CDS programs maintain a careful balance between guidance and workflow disruption.
For example:
- Interruptive alerts should be reserved for high-risk patient safety scenarios.
- Passive guidance, such as inline suggestions or pathway prompts, can support lower-risk decisions without interrupting clinicians.
Monitoring these metrics allows hospitals to continuously refine healthcare decision support software so that it remains helpful rather than disruptive.
C. Link CDS outcomes to real operational and financial results
Executive leadership supports technology investments when results are visible.
Hospitals that succeed in implementing clinical decision support systems consistently link CDS performance metrics to operational outcomes.
For example, decision support that standardizes clinical pathways can reduce unnecessary variation in care. This can produce measurable improvements in:
- length of stay
- supply and pharmacy utilization
- treatment consistency across clinicians
Decision support can also integrate predictive models and risk-scoring tools directly into EHR workflows.
In cases like these, healthcare decision support software becomes part of the hospital’s clinical intelligence infrastructure rather than simply a set of alerts.
Hospitals should therefore tie CDS results to strategic metrics such as:
- preventable harm reduction
- readmission performance under value-based contracts
- service-line margin improvement
- clinician productivity gains
When leadership can see clear links between the implementation of clinical decision support systems and operational outcomes, CDS evolves from a technology expense into a strategic clinical asset.

Treat CDS as a Clinical Capability, Not a Tool
Hospitals that plan budgets carefully, build strong governance structures, and track meaningful outcomes tend to achieve sustained results from CDS programs.
Successful clinical decision support system implementation is not defined by the number of alerts deployed or the sophistication of the underlying technology. It is defined by whether clinicians trust the guidance and whether the organization sees measurable improvements in safety, efficiency, and financial performance.
For hospital leaders preparing finance committee proposals, the key message is simple.
Decision support is not just software.
It is an operational capability that improves care quality, protects margins, and supports the transition to value-based healthcare.
Most hospitals complete the initial phase of clinical decision support system implementation in 6–12 months, depending on integration complexity and governance readiness. Early phases typically focus on high-impact safety rules and foundational architecture, while advanced decision-support capabilities are introduced over time. A phased approach allows hospitals to demonstrate early value while reducing disruption to clinicians.
Many hospitals use a hybrid approach. Core clinical decision support software capabilities may come from an EHR vendor or external platform, while hospitals develop custom rules and pathways aligned with their clinical protocols. Internal informatics teams often maintain decision logic even when the underlying infrastructure is vendor-supported.
Reducing alert fatigue requires careful design and governance during the implementation of clinical decision support systems. High-risk safety alerts should be interruptive, while lower-risk recommendations can appear as passive guidance within the workflow. Continuous monitoring of alert acceptance and override rates helps organizations refine rules and maintain clinician trust.
Successful implementation of a clinical decision support system requires cross-functional participation from clinical leadership, IT, pharmacy, quality improvement, and finance teams. Clinical informatics specialists typically coordinate governance, while physician champions validate decision logic and workflow design. Early collaboration ensures CDS rules align with operational priorities and care pathways.
ROI from healthcare decision support software is usually measured through improvements in patient safety, operational efficiency, and financial performance. Examples include reductions in adverse drug events, shorter length of stay, lower readmission penalties, and improved utilization management. Hospitals that track these metrics before and after implementation can clearly demonstrate the value of CDS investments.
Integration costs can vary significantly based on the EHR system in use. For instance, Epic integration typically requires more upfront investment due to its complexity, while Athena or Cerner systems may offer more flexible pricing based on the scale of implementation.
Ongoing costs for CDS systems typically include software subscriptions, maintenance of integration points, and rule updates. Hospitals must also allocate funds for clinical validation and continuous monitoring of alert performance to ensure the system remains effective over time.
CDS integration streamlines workflows by embedding decision support directly into the EHR. This reduces the time spent on manual checks, enhances patient safety, and allows clinicians to make more informed decisions, all within the existing workflow.
Smaller hospitals or health systems may benefit from modular CDS solutions that focus on high-impact areas like medication safety or sepsis detection, rather than a full-scale enterprise solution. Cloud-based solutions or those using standardized APIs can also reduce the initial costs of implementation.






























![10 Clinical Decision Support System Examples With Real Metrics [2026]](https://www.mindbowser.com/wp-content/uploads/2025/08/Clinical-Decision-Support-System-1024x324.jpg)

![5 Types of Clinical Decision Support Systems: Which One Fits Your Hospital? [2026]](https://www.mindbowser.com/wp-content/uploads/2026/03/medical-technology-network-telemedicine-health-insurance-virtual-hospital-healthcare-1024x585.jpg)