TL;DR
- Telemedicine software development has evolved beyond simple video visits into a full clinical workflow infrastructure.
- Modern platforms integrate AI-generated clinical documentation, remote patient monitoring (RPM), and deep EHR interoperability to support the entire virtual care lifecycle from intake and documentation to monitoring and follow-up.
- For healthcare CIOs and digital health leaders, scalable telemedicine platforms now focus on reducing physician workload, managing continuous patient data safely, and creating unified digital care systems that improve operational efficiency and patient outcomes.
“Is your telemedicine platform actually reducing clinician workload or just moving the same work to another screen?”
Many health systems rushed into virtual care during the pandemic, deploying video visit tools as fast as possible. But once the novelty faded, a harsher reality set in. Physicians still had to write notes manually. RPM dashboards lived outside the EHR. Clinical workflows remained fragmented.
Today, leading health systems are rethinking telemedicine software development from the ground up. The goal is no longer just enabling virtual visits. It is building a digital clinical infrastructure in which AI-generated documentation, remote patient monitoring, and EHR workflows operate as a single system.
This guide explores how healthcare organizations are architecting telemedicine platforms that reduce documentation burden, securely manage continuous patient data, and turn virtual care into a scalable clinical workflow.
I. Why Has Telemedicine Software Development Shifted from Video to Workflow Infrastructure?
A. What Changed After Pandemic-Era Virtual Care?
During the pandemic, virtual visits solved one urgent problem: patient access when clinics were closed. But healthcare delivery did not stay in emergency mode. It matured.
Hybrid care is now permanent. Health systems run a mix of in-person, virtual, and remote monitoring programs. Virtual care is no longer an exception. It is part of routine operations.
That shift forced a rethink of telemedicine software development. Early platforms focused on a single task: launching a video call. They served as temporary front doors but were disconnected from clinical workflows.
Several structural changes accelerated the transition:
- Reimbursement stabilized. CMS and commercial payers formalized virtual care billing pathways.
- Regulatory frameworks have matured. Telehealth policies now define expectations for documentation, security, and data handling.
- Clinical integration became mandatory. Virtual visits must now write directly into the EHR.
- Hybrid operations require continuity. Patients move between physical and virtual care environments.
As a result, modern telemedicine software development is no longer about enabling video encounters. It is about building digital care pathways that mirror real clinical operations.
Video became the entry point. Workflow became the system.
B. Why Is Video Alone No Longer Enough?
Many early telehealth vendors still offer platforms centered around video visits. Hospitals adopting them quickly discover the problem.
The clinician workload never changed.
Physicians still document visits manually. Orders still require separate EHR navigation. Follow-up tasks still happen outside the telehealth interface. The result is fragmented workflows that slow adoption.
The limitations become even clearer when organizations expand virtual programs:
- Documentation burden remains high. Physicians spend significant time writing notes after virtual visits.
- RPM introduces continuous data streams. Devices generate thousands of daily measurements.
- Compliance requirements increased. Audit trails, consent capture, and documentation integrity are now expected.
- Operational fragmentation hurts clinician trust.
These pressures are forcing CIOs to rethink telemedicine software development as a clinical infrastructure rather than a communication tool.
A video visit without integrated documentation, data ingestion, and EHR synchronization creates operational friction. Systems that scale virtual care instead treat telehealth as part of the clinical workflow.
That means the platform must handle documentation, monitoring, escalation, and billing in a unified architecture.
Modern telemedicine software development, therefore, focuses on workflow orchestration, not just on video delivery.
C. What Defines Modern Telemedicine Software Development?
Today’s leading virtual care platforms share one architectural principle: the visit is only one step in the care lifecycle.
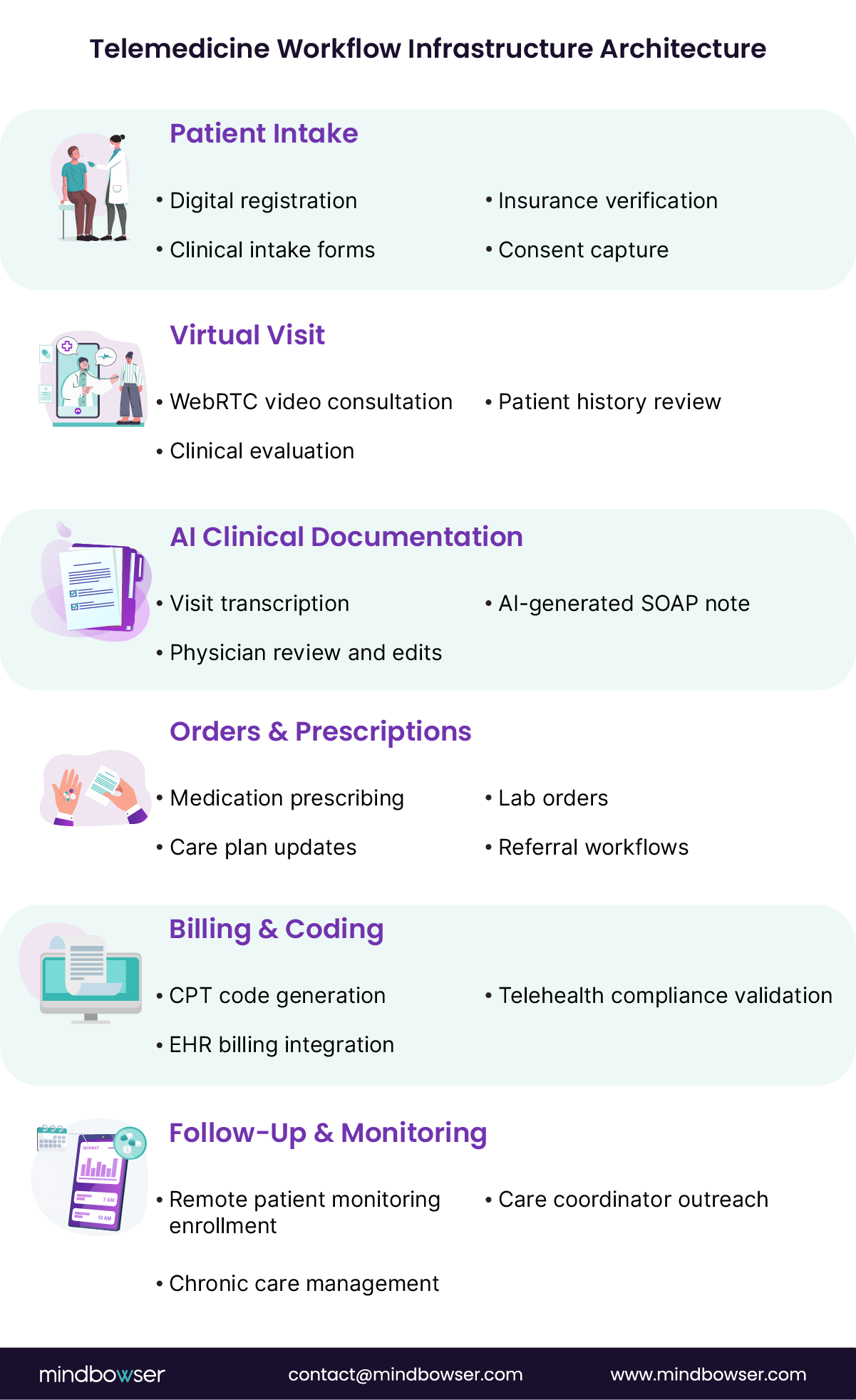
Modern telemedicine software development integrates four foundational capabilities:
- AI-assisted clinical summaries
Visit audio can be transcribed and converted into structured SOAP notes that clinicians review and sign. Solutions such as the AI Medical Summary accelerator, a prebuilt module for generating structured clinical notes from visit transcripts, demonstrate how documentation automation can reduce physician workload while preserving clinical accuracy. - Embedded documentation workflows
Clinical notes, orders, prescriptions, and billing codes are generated inside the telehealth workflow rather than requiring manual EHR navigation. - Device-agnostic RPM ingestion
Remote patient monitoring platforms must ingest device telemetry from blood pressure monitors, glucometers, pulse oximeters, and wearables without creating alert overload. - Secure EHR-native integration
FHIR APIs and HL7 interfaces allow data to flow directly into the patient record, closing the loop between virtual visits and longitudinal care management.
This architecture reflects a new reality: telemedicine software development now builds digital clinical infrastructure rather than communication tools.
The result is measurable operational improvement. Documentation time drops. RPM programs scale safely. Clinicians stay inside one workflow.
Bottom line: successful virtual care platforms integrate AI documentation, monitoring data, and EHR connectivity into a single operational system. These architectural principles align with the workflow-first approach outlined in Mindbowser’s healthcare content blueprint for digital health platforms.
Table 1: Evolution of Telemedicine Platforms
| Capability | Pandemic-Era Telemedicine | Modern Telemedicine Software Development | Operational Impact |
| Core Function | Video visits | Workflow orchestration | Full care lifecycle support |
| Documentation | Manual entry | AI clinical summaries | 50–70% documentation time reduction |
| RPM Integration | External dashboards | Embedded RPM ingestion | Continuous monitoring |
| EHR Integration | Scheduling only | Full data exchange | End-to-end clinical workflow |
II. How Does AI Clinical Documentation Transform Telemedicine Workflows?
A. Why Documentation Is the Biggest Bottleneck in Virtual Care
Ask any CMIO what slows virtual care adoption. The answer is predictable: documentation.
Video visits shortened patient access time, but they did little to reduce physician administrative burden. In many health systems, clinicians still spend as much time documenting a telehealth visit as they do an in-person encounter. The interface changed. The workload did not.
This is where telemedicine software development has shifted its priorities. Instead of focusing only on communication, modern platforms aim to eliminate the documentation burden created during the visit itself.
The operational challenge is straightforward:
- Virtual visits generate unstructured conversational data
- Clinicians must convert that conversation into structured clinical documentation
- Documentation must meet coding, compliance, and billing requirements
- All notes must synchronize with the EHR
Manual documentation slows clinicians and limits the number of virtual visits a provider can safely handle in a day.
Physicians often spend 1–2 hours on documentation for every hour of patient care. Virtual visits do not eliminate that overhead. In some cases, they increase it because clinicians switch between telehealth tools and EHR interfaces.
For CIOs evaluating telemedicine software development, the key question is no longer “Can we enable video visits?”
The real question is: Can we reduce clinician documentation workload while maintaining compliant clinical records?
AI clinical documentation addresses that challenge directly.
B. How AI Clinical Documentation Works in Telemedicine Platforms
AI documentation systems convert clinical conversations into structured notes that clinicians can review and approve.
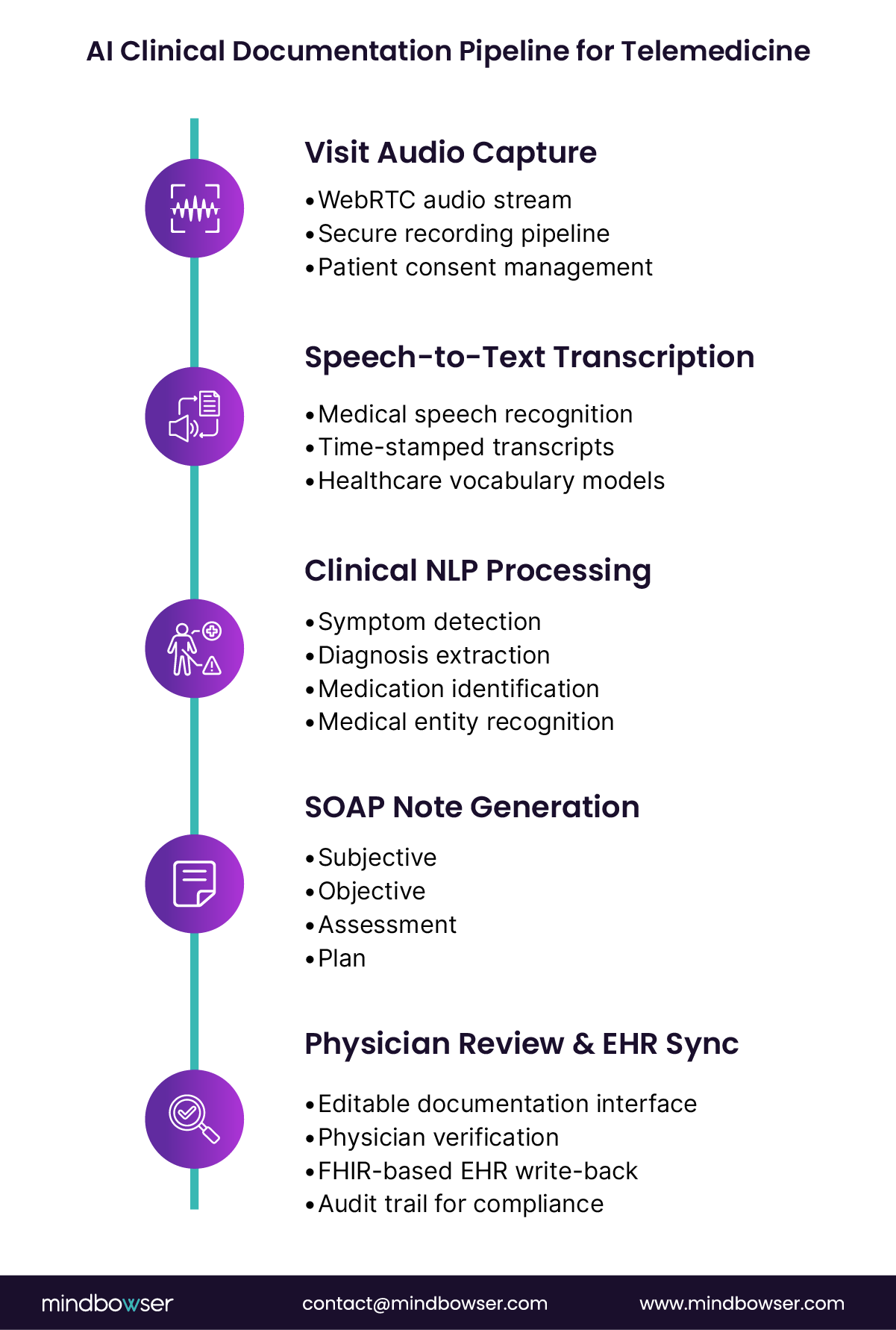
In modern telemedicine software development, the documentation pipeline typically follows five steps:
- Audio capture during the visit
The telehealth platform records the clinical conversation through WebRTC audio streams. Capture occurs automatically once consent is confirmed. - Speech-to-text transcription
AI transcription services convert the audio into time-stamped clinical transcripts. Healthcare-tuned speech models improve accuracy for medical terminology. - Clinical NLP processing
Natural language processing models identify medical entities such as symptoms, diagnoses, medications, and procedures. - SOAP note generation
The system organizes extracted information into structured Subjective, Objective, Assessment, and Plan sections. - Physician review and verification
Clinicians review the generated note in an editable interface, make any needed adjustments, and sign the documentation.
The goal is simple: transform conversational data into clinical documentation without forcing physicians to retype the visit narrative.
This architecture is becoming a core requirement in telemedicine software development because it directly targets the largest source of clinician friction.
C. Integrating AI Documentation into EHR Workflows
AI documentation is only useful if it integrates cleanly into clinical systems.
Standalone AI scribes create another interface clinicians must manage. That defeats the purpose. The most effective implementations embed documentation generation directly into the telehealth workflow.
Mindbowser’s AI Medical Summary accelerator, a prebuilt module for generating structured clinical notes from visit transcripts, demonstrates how AI-generated documentation can flow directly into the patient chart while preserving compliance and auditability.
In modern telemedicine software development, integration typically includes:
- FHIR-based note insertion into EHR records
- Editable review interfaces with audit trails
- Version tracking for documentation changes
- Structured metadata for billing and coding
- Secure HIPAA-compliant storage of transcripts
This integration ensures AI-generated documentation becomes part of the clinical record rather than an external artifact.
The operational impact is substantial. Health systems implementing AI documentation in virtual care programs often report:
- 50–70% reduction in documentation time
- Faster visit turnaround
- Improved clinician satisfaction
- More scalable telehealth operations
For digital health leaders, the takeaway is clear. Telemedicine software development must include documentation automation as a core capability, not an optional feature.
Platforms that embed AI documentation into clinical workflows remove friction. And when clinicians save time, virtual care adoption grows.
Table 2: Telemedicine AI Architecture Layers
| Layer | Function | Technology Components |
| Capture Layer | Visit audio capture | WebRTC, recording pipeline |
| Processing Layer | Transcription + NLP | Speech-to-text, clinical NLP |
| Structuring Layer | SOAP note generation | Medical entity extraction |
| Review Layer | Physician verification | Editable UI with audit trail |
| Integration Layer | EHR write-back | FHIR APIs, HL7 interfaces |
III. How Does Remote Patient Monitoring Integrate with Telemedicine Platforms?
A. Why RPM Is Expanding the Scope of Telemedicine Platforms
Remote patient monitoring (RPM) changes the nature of virtual care. Instead of episodic encounters, clinicians receive continuous physiological data from patients between visits.
This shift forces a major rethink of telemedicine software development.
Traditional telehealth platforms assumed a simple interaction model: patient schedules a visit→ physician conducts a video consultation→ clinician documents the encounter.
RPM introduces an entirely different operational model:
- Devices collect patient data continuously
- Measurements stream into clinical systems daily
- Risk thresholds must be monitored automatically
- Care teams intervene when readings cross defined limits
Without an integrated infrastructure, this process quickly becomes unmanageable. Clinicians may receive thousands of measurements per week from blood pressure monitors, glucose meters, pulse oximeters, and weight scales.
Modern telemedicine software development, therefore, treats RPM as a native component of the virtual care platform rather than an external dashboard.
The architectural objective is straightforward: ingest device data, interpret clinical signals, and route alerts without overwhelming clinicians.
That requires several foundational capabilities:
- Device ingestion pipelines
- Measurement normalization
- Risk detection logic
- Care team escalation workflows
- EHR documentation synchronization
When these capabilities are built directly into telemedicine software development, RPM becomes a scalable clinical program rather than a fragmented technology experiment.
Table 3: RPM Integration Architecture
| Component | Purpose | Operational Impact |
| Device Ingestion | Collect device telemetry | Device-agnostic scaling |
| Data Normalization | Standardize measurements | Cross-device compatibility |
| Threshold Logic | Risk detection | Automated triage |
| Care Team Routing | Assign actions | Reduced alert fatigue |
| EHR Sync | Documentation and billing | Closed-loop workflows |
B. Managing Continuous Patient Data Without Alert Fatigue
The biggest operational risk in RPM programs is alert overload.
A single patient with hypertension may submit daily blood pressure readings. Multiply that by hundreds or thousands of patients, and the data volume becomes significant.
Poorly designed RPM systems generate alerts for every abnormal reading. That approach overwhelms clinicians and leads to alert fatigue.
Effective telemedicine software development solves this problem by introducing intelligent triage layers.
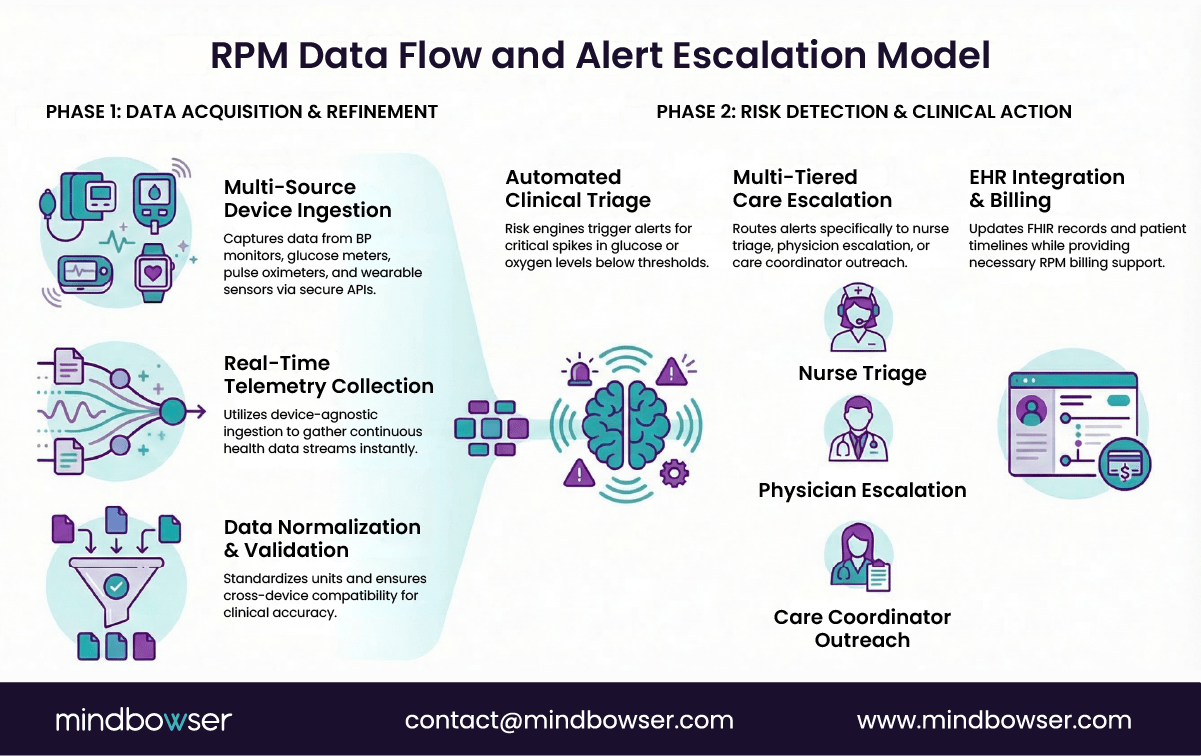
Instead of sending every data point to clinicians, platforms implement:
- Data filtering
Measurements are validated for completeness and plausibility before being entered into the monitoring pipeline.
- Threshold-based triage
Clinical thresholds determine when intervention is required. For example:
- BP > 180/120 triggers urgent escalation
- BP 150–160 may generate a care coordinator review
- Normal readings are simply recorded
- Trend analysis
Algorithms evaluate patterns across multiple readings rather than reacting to a single measurement.
- Care team routing
Alerts are directed to the appropriate team member:
- Nurses for moderate risk
- Physicians for critical escalations
- Care coordinators for patient follow-up
This layered architecture ensures RPM programs scale safely without overwhelming clinicians.
As a result, modern telemedicine software development treats data triage as a clinical workflow problem, not just a data ingestion problem.
C. Building Closed-Loop RPM Workflows with EHR Integration
RPM systems create value only when the data feeds back into clinical workflows.
If device measurements remain isolated in a monitoring dashboard, clinicians must manually transfer information into the EHR. That extra step undermines adoption and creates documentation gaps.
Modern telemedicine software development addresses this by enabling direct EHR synchronization.
Platforms integrate RPM data pipelines with clinical systems using standards such as:
- FHIR Observation resources
- HL7 interfaces
- SMART-on-FHIR integrations
- Secure device APIs
These integrations enable:
- Automated documentation of device measurements
- Billing support for RPM CPT codes
- Longitudinal patient monitoring inside the EHR
- Clinical decision support based on device data
Health systems implementing this architecture can manage chronic conditions at scale while maintaining clinical oversight.
For digital health leaders, the implication is clear. Telemedicine software development must support continuous monitoring workflows, not just real-time visits.
Virtual care platforms that integrate AI documentation and RPM infrastructure create a unified digital care environment.
And that environment is what allows virtual care to scale safely.
Want to Build an AI-Enabled Telemedicine Platform That Reduces Clinician Workload?
IV. What Architecture Enables Scalable Telemedicine Platforms?
A. Why Telemedicine Platforms Require Modular Architecture
Early virtual care systems were designed as lightweight applications. Their job was simple: connect a patient and clinician through a video interface.
That architecture does not scale.
As virtual care expands, telemedicine software development must support scheduling, clinical documentation, device ingestion, analytics, and billing. Each of these capabilities introduces its own integration and performance requirements.
A monolithic telehealth application cannot handle that complexity.
Modern telemedicine software development, therefore, follows a modular architecture in which core capabilities operate as loosely coupled services. This approach allows organizations to evolve components independently while maintaining continuity of clinical workflow.
Key architectural characteristics include:
- Service-based platform design
Separate services manage video sessions, documentation processing, device ingestion, and patient engagement. - API-first integration strategy
Clinical systems, device platforms, and analytics tools connect through secure APIs rather than direct database dependencies. - Interoperability standards
FHIR and HL7 interfaces enable structured data exchange with EHR systems. - Compliance-oriented infrastructure
Audit logging, consent capture, and secure data storage are built into the platform core.
This modular structure allows health systems to extend capabilities without disrupting existing workflows.
For CIOs planning large-scale programs, the architectural question becomes clear: Can the telemedicine platform evolve as new care models emerge?
Effective telemedicine software development ensures the answer is yes.
B. Core Components of a Telehealth Software Architecture
Scalable telehealth platforms typically consist of five foundational layers. Each layer addresses a specific operational requirement.
- Patient access layer
This interface handles patient scheduling, virtual waiting rooms, identity verification, and visit entry. Mobile and web applications typically operate here.
- Communication layer
Video and audio communication occur through WebRTC infrastructure. Session management, encryption, and connection reliability are managed at this level.
- Clinical workflow layer
This layer orchestrates clinical tasks, including:
- Intake forms
- AI documentation generation
- Orders and prescriptions
- Follow-up scheduling
Within modern telemedicine software development, this layer integrates AI-assisted clinical summaries and workflow automation.
- Data and monitoring layer
Device data ingestion and analytics pipelines operate here. RPM telemetry, patient-reported outcomes, and care plan metrics feed into the monitoring infrastructure.
- Integration layer
The integration layer synchronizes platform data with the EHR, billing systems, and clinical registries.
Typical integration technologies include:
- FHIR APIs
- HL7 messaging interfaces
- SMART-on-FHIR applications
- Secure event pipelines
This layered architecture ensures each capability can evolve independently while maintaining clinical interoperability.
C. Why EHR Integration Is the Backbone of Telemedicine Platforms
No matter how advanced the telehealth interface becomes, clinicians still rely on the EHR as the system of record.
If virtual care platforms operate outside the EHR workflow, clinicians must duplicate work across multiple systems. That duplication slows adoption and increases the risk of documentation errors.
Successful telemedicine software development, therefore, treats the EHR as the central integration point.
Key integration objectives include:
- Real-time patient context retrieval
Demographics, medication lists, allergies, and clinical history should appear automatically when a visit begins. - Structured documentation insertion
AI-generated clinical notes must be written directly into the patient chart. - Orders and prescriptions synchronization
Orders initiated during virtual visits must flow into existing clinical ordering workflows. - Billing and coding support
Telehealth services must map correctly to reimbursement rules.
Organizations building advanced virtual care platforms often combine AI documentation, RPM ingestion, and EHR integration into a unified architecture.
For CIOs and digital health leaders, the strategic takeaway is clear. Telemedicine software development is now infrastructure engineering.
Video enables interaction.
AI reduces documentation burden.
RPM expands clinical visibility.
But the system only works when everything connects through the EHR.
Scalable virtual care requires an architecture designed for interoperability, clinical workflow efficiency, and long-term platform evolution.
V. How Mindbowser Helps Healthcare Organizations Build AI-Enabled Telemedicine Platforms
A. Discovery Framework
Most telemedicine failures happen before engineering starts. The platform ships, but the workflow does not fit how care teams actually work. Mindbowser starts with a discovery process built for clinical operations, not feature lists.
Discovery focuses on three work products your leadership team can review:
- Clinical workflow mapping: We map intake, documentation, orders, billing capture, and follow-up across roles (physician, nurse, care coordinator, billing). This is where workflow gaps show up fast.
- Compliance risk assessment: HIPAA requirements are translated into system controls such as encryption, audit logs, role-based access, retention, and consent handling so nothing important gets “added later.”
- Architecture blueprint: We define the integration plan for EHR connectivity, AI documentation, and RPM ingestion with clear boundaries between services, data stores, and audit trails.
Discovery turns telemedicine software development from a “build features” project into an operational design exercise.
B. Engineering Approach
Mindbowser builds telemedicine platforms as EHR-connected workflow infrastructure, designed for HIPAA and SOC 2 expectations from day one.
That typically includes:
- HIPAA-compliant cloud infrastructure: encryption in transit and at rest, least-privilege access, centralized logging, and incident-ready monitoring.
- FHIR-based EHR integration: patient context retrieval, scheduling alignment, clinical note write-back, orders integration, and secure messaging support based on the EHR’s real change-control constraints.
- AI documentation implementation with AI Medical Summary: audio capture, transcription, and structured SOAP note, with clinician review, version history, and traceability, so the signed note can be audited end-to-end.
- RPM integration via HealthConnect CoPilot: device ingestion, normalization, threshold logic, role-based routing, and EHR write-back, so RPM supports care teams rather than overwhelming them.
This is telemedicine software development built as a clinical system, not an add-on tool.
C. Delivery Model
Most health systems don’t need a “big bang” release. They need a phased rollout with measurable gates.
Mindbowser delivers in three phases:
- Phased MVP: start with the EHR-integrated virtual visit workflow and documentation pathway.
- Integration-first development: ensure notes, orders, and billing capture work cleanly before expanding surface features.
- Measurable ROI tracking: track documentation time saved, chart closure speed, clinician adoption, and RPM alert volumes so leadership can prove operational impact.

What Defines Scalable Telemedicine Software Development in 2026?
Telemedicine is no longer just about enabling video visits. Health systems that successfully scale virtual care are investing in telemedicine software development that integrates AI documentation, RPM monitoring, and EHR workflows into a single clinical system.
AI must reduce documentation burden, RPM must support care teams without creating alert fatigue, and interoperability with the EHR must support real clinical workflows such as scheduling, notes, orders, and billing.
In 2026, the organizations leading in virtual care are those treating telemedicine software development as a digital clinical infrastructure built for efficiency, compliance, and measurable operational ROI.
The timeline depends on integration complexity and feature scope. A basic telehealth platform can be built in 3–4 months, but enterprise-grade telemedicine software development with EHR integration, AI documentation, and RPM capabilities usually takes 6–12 months. Most organizations deploy the platform in phases, starting with virtual visits and documentation automation before expanding into remote monitoring and advanced care workflows.
Telemedicine platforms must comply with HIPAA privacy and security rules, which require encryption of patient data in transit and at rest, secure access controls, and audit logging. Many healthcare organizations also require SOC 2–aligned infrastructure, role-based access management, and secure API integrations when exchanging data with EHR systems and medical devices. Compliance architecture should be built into telemedicine software development from the beginning rather than added later.
Modern telemedicine software development integrates billing workflows directly into clinical documentation systems. Virtual visits must generate structured documentation, CPT codes, and encounter records that align with payer requirements. For programs like remote patient monitoring, platforms also track device data and care management interactions to support RPM reimbursement codes such as CPT 99453, 99454, and 99457.
Yes. Many healthcare organizations operate across multiple EHR environments due to mergers, acquisitions, or specialty systems. Modern telemedicine software development uses interoperability standards such as FHIR APIs, HL7 messaging, and SMART-on-FHIR applications to exchange clinical data with different EHR platforms. This architecture allows telehealth systems to retrieve patient data, write clinical documentation, and synchronize orders across multiple systems.
Analytics helps health systems measure the operational and clinical performance of virtual care programs. Telemedicine platforms can track metrics such as visit volume, physician documentation time, patient engagement, RPM adherence, and clinical outcomes. These insights help digital health leaders identify workflow bottlenecks, improve patient monitoring programs, and evaluate the ROI of telemedicine software development initiatives.

































