TL;DR
- Telehealth software platforms help you launch fast. Custom builds help you scale right. That tension defines every virtual care strategy today.
- Platforms offer speed, lower upfront cost, and ready workflows. Custom development offers control, differentiation, and long-term scalability.
- Most healthcare organizations don’t choose one forever. They evolve.
Start with speed. Shift to control. Combine both for scale.
The real decision is not build vs buy. It is when to switch, what to control, and how to avoid rework later.
Are you building your telehealth strategy for speed or for scale?
Most healthcare organizations start with telemedicine software platforms to launch quickly, but as complexity grows, those same systems can become constraints.
The real challenge is not choosing between platform and custom. It is knowing when to evolve and what to control.
I. Why Are Telehealth Software Platforms Transforming Virtual Care Delivery?
A. What are telehealth software platforms?
Telehealth software platforms are the foundation of virtual care delivery.
They provide the infrastructure needed to connect patients and providers through video consultations, scheduling, and clinical workflows.
Think of them as the operating layer that enables virtual care, not just a communication tool.
1. Telehealth platforms vs telemedicine apps
Platforms provide the core infrastructure, while apps deliver the user-facing experience.
Most applications rely on underlying platforms for workflows, compliance, and integrations.
2. Telehealth platforms vs virtual care tools
Tools solve specific problems, such as video or messaging.
Platforms connect these capabilities into a unified care delivery system.
3. Examples of telehealth platforms in use
Providers, hospitals, and digital health startups use telemedicine software platforms to launch and scale virtual care services.
These platforms enable faster deployment while standardizing core workflows.
Telehealth platforms provide the infrastructure that powers virtual care, connecting interactions, workflows, and systems into a single delivery model.
Related read: Telemedicine Software vs Virtual Care Platforms: Which Model Scales for Mid-Market Hospitals?
B. Why telehealth platforms are gaining rapid adoption
Telehealth adoption accelerated because it solved immediate access problems.
What started as a response to COVID-19 has become a permanent shift in care delivery. The drivers are now structural rather than temporary.
This is no longer about convenience. It is about system efficiency.
1. Expansion of virtual care after COVID-19
A significant portion of this demand has sustained, making virtual care a standard delivery channel.
2. Growing patient demand for access
Patients now expect faster, more flexible care experiences.
Recent search trends reflect this shift toward immediacy and convenience, with rising queries like “instant prescriptions,” “UTI symptoms,” and condition-specific telehealth services indicating growing demand for on-demand, problem-focused care rather than general consultations.
Telemedicine software platforms enable on-demand access, reduced wait times, and improved engagement across care journeys.
3. Provider focuses on efficiency and capacity
Health systems are using telehealth to expand reach and improve utilization.
Telehealth platforms are gaining adoption because they improve access, efficiency, and capacity, but their long-term effectiveness depends on how well they adapt to complex care delivery needs.
C. Market growth and adoption trends
Telehealth is no longer a trend. It is a structural shift.
Adoption is now driven by investment, new care models, and system-wide integration into healthcare delivery.
The question is no longer if telehealth will grow, but how it will scale.
1. Telehealth market growth and investment trends
This reflects a long-term redistribution of care delivery, not temporary demand.
2. Rise of digital health startups building virtual care solutions
Startups are using telemedicine software platforms to launch quickly and validate care models.
As they scale, many shift toward custom architectures to support differentiation and integration needs.
3. Healthcare organizations integrating telehealth into hybrid care models
Hospitals are embedding telehealth into hybrid care delivery, combining virtual and in-person services.
WHO-backed initiatives continue to push digital access, especially for underserved populations.
Telehealth growth is driven by capital, innovation, and hybrid care adoption, but long-term success depends on building systems that can scale beyond initial platform capabilities.
II. What Core Capabilities Define Modern Telehealth Software Platforms?
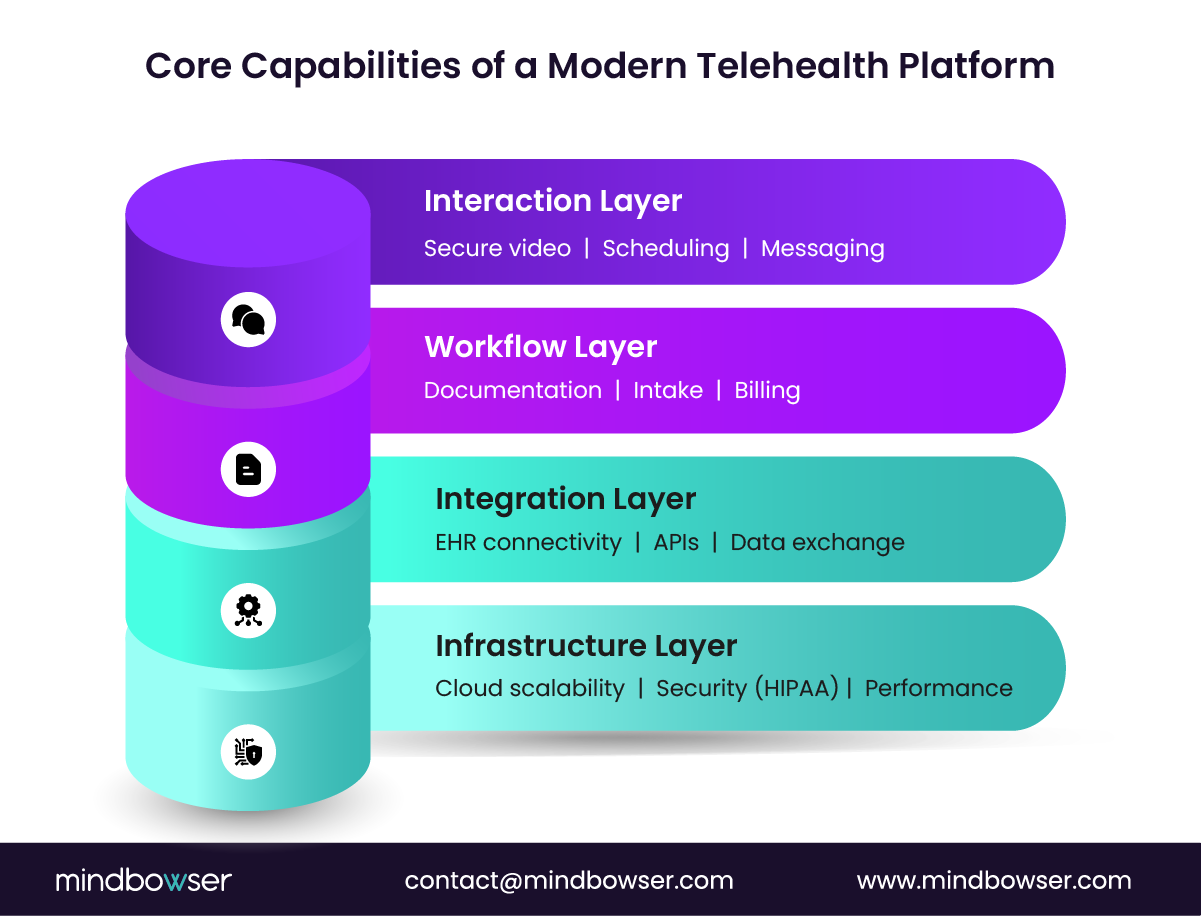
A. Patient and provider interaction capabilities
Interaction is where telehealth either works or fails.
Patients and providers judge virtual care based on how easy, fast, and reliable interactions feel. If this layer breaks, adoption drops regardless of clinical quality.
If the experience feels clunky, trust erodes immediately.
1. Secure video consultations
Video is the core interaction layer, but it must be secure, stable, and low-latency to support clinical accuracy and compliance.
Anything less disrupts care delivery and patient confidence.
2. Appointment scheduling and virtual waiting rooms
Scheduling drives access and utilization.
Studies show that digital reminders and scheduling systems can reduce missed appointments by up to 23-34%.
3. Messaging and asynchronous care
Not all care requires live interaction.
Secure messaging enables follow-ups, clarifications, and chronic care engagement without increasing clinician workload.
Why schedule a visit when a message solves the problem?
Interaction capabilities define patient experience and provider efficiency, making them critical to telehealth adoption but insufficient alone for long-term scalability.
B. Clinical and operational workflows
Telehealth workflows look simple until scale exposes the gaps.
Most telemedicine software platforms handle basic consultations well. But as care expands into multi-step journeys involving intake, treatment, follow-ups, and coordination, workflows begin to fragment.
What happens when care is no longer a single visit, but an ongoing process?
1. Electronic prescriptions and documentation
Platforms support e-prescriptions and clinical notes, but often rely on predefined templates.
As complexity grows, clinicians face limitations in adapting documentation to evolving care models, increasing the administrative burden instead of reducing it.
2. Patient intake and onboarding workflows
Digital intake simplifies initial access, but disconnected workflows can lead to repeated data capture and inconsistent patient journeys.
Structured intake must feed the entire care lifecycle, not just the first visit.
3. Billing, reimbursement, and claims integration
Revenue workflows depend on accurate documentation and system alignment.
At scale, rigid billing logic and limited payer integration create delays, errors, and operational friction. CMS reimbursement expansion has made telehealth viable, but workflow gaps still impact revenue realization.
Clinical and operational workflows define whether telehealth is sustainable, and as complexity increases, rigid platform workflows often create inefficiencies that push organizations toward more flexible solutions.
C. Infrastructure and interoperability capabilities
This is where most telehealth strategies either scale or stall.
Front-end features get attention. Infrastructure determines longevity.
As virtual care expands, telemedicine software platforms must do more than support visits. They must connect, exchange, and scale data across the healthcare ecosystem.
1. Integration with EHR and healthcare systems
No telehealth platform operates in isolation.
To deliver meaningful care, platforms must integrate with:
- Electronic Health Records (EHRs)
- Lab systems
- Pharmacy networks
- Revenue cycle systems
This ensures that virtual visits are not siloed experiences but part of a longitudinal patient record.
Interoperability remains a major priority and challenge in healthcare, with organizations continuing to invest in better data exchange and system integration.
If your telehealth system cannot talk to your EHR, are you delivering care or just conducting calls?
Integration depth matters here. Many platforms offer basic integrations, but deeper workflows often require custom extensions.
2. API-driven healthcare ecosystems
Modern telehealth platforms are increasingly API-first.
This means they expose capabilities that allow organizations to:
- Build custom patient experiences
- Integrate third-party tools
- Extend workflows beyond platform limits
APIs turn platforms into building blocks instead of closed systems.
That shift is critical for digital health companies that want to innovate without rebuilding infrastructure from scratch.
But there’s a tradeoff.
How much control do you actually have over those APIs?
Limited API flexibility can create hidden constraints, especially as product complexity grows.
3. Cloud infrastructure and scalability
Virtual care demand is not linear. It spikes.
Flu seasons. Public health events. Product growth.
Telehealth platforms rely on cloud infrastructure to handle:
- High concurrency video sessions
- Real-time data exchange
- Multi-region availability
McKinsey estimates that cloud adoption could generate $100B-$170B in annual value for healthcare organizations by improving scalability, data access, and operational efficiency.
That efficiency is essential.
But scalability is not just about handling volume. It is about handling complexity at scale:
- Multiple care programs
- Diverse patient populations
- Expanding integrations
This is where platform boundaries often emerge.
Infrastructure and interoperability define whether a telehealth platform can evolve with your organization or become a constraint as your care model grows.
III. What Are Custom Telemedicine Builds and Why Do Some Companies Choose Them?
A. What custom telemedicine development means
Custom telemedicine development shifts telehealth from a tool to a product.
Instead of relying on predefined platform capabilities, organizations build proprietary systems aligned to their care models, workflows, and growth strategy.
This is not a configuration. It is full ownership of how care is delivered digitally.
1. Building proprietary telehealth platforms
Custom builds give organizations control over patient experience, data architecture, and product roadmap.
This turns telehealth into a strategic asset, not just an operational layer.
2. Custom architecture for healthcare workflows
Healthcare workflows vary across specialties and care models.
Custom systems allow organizations to design condition-specific pathways and multi-step care journeys without platform constraints.
3. Tailored digital health solutions for specific specialties
From chronic care to behavioral health, custom platforms enable deeper alignment with specialty needs.
When care models become complex, standard platforms often require compromise. Custom systems remove that tradeoff.
Custom telemedicine development enables full control over workflows, integrations, and patient experience, making it essential for organizations building differentiated and scalable virtual care products.
B. When digital health companies prefer custom development
Organizations don’t choose custom builds early. They are pushed into them.
The shift typically happens when telemedicine software platforms begin limiting growth, workflows, or differentiation.
The signal is not technical. It is operational friction.
1. Unique clinical workflows
As care models evolve, standard workflows become restrictive.
Programs like chronic care or multi-step treatment pathways require flexible, workflow-first systems that platforms often cannot support without compromise.
2. Advanced integrations with healthcare infrastructure
Growth increases integration demands across EHRs, devices, and analytics systems.
When real-time data exchange and deeper interoperability become critical, platform limitations begin to slow execution.
3. Product differentiation for digital health startups
For startups, telehealth is not infrastructure. It is the product.
Custom development enables ownership of patient experience, workflows, and data, which becomes essential for long-term differentiation and valuation.
Digital health companies move toward custom development when platform constraints begin to impact workflows, integrations, and product differentiation.
C. Challenges of custom telehealth development
Custom builds offer control, but they shift the burden to you.
What platforms and abstract, custom systems require you to own across engineering, compliance, and operations.
The tradeoff is simple: flexibility in exchange for responsibility.
1. Higher development costs
Custom platforms require investment in infrastructure, integrations, and product development.
This creates a long-term asset, but demands upfront capital and sustained investment.
2. Longer product launch timelines
Building from scratch increases time-to-market compared to platform-based approaches.
Teams must balance speed of launch with long-term scalability.
3. Compliance and security responsibility
Custom systems must meet HIPAA and security requirements by design.
With healthcare breaches averaging $10.93 million per incident (IBM), security becomes an ongoing operational discipline, not a one-time setup.
Custom telehealth development provides flexibility and control, but requires higher investment, longer timelines, and full ownership of compliance and security.
Ready to Build a Telehealth Strategy That Scales Beyond Your First Platform?
IV. Telehealth Software Platforms vs Custom Builds: What Are the Key Differences?
A. Platform vs Custom Development Comparison
This is the decision that shapes your next 3-5 years.
Most leadership teams frame it as a technical choice. It is not. It is a strategic operating model decision.
What happens to your care model when your platform can no longer support it?
Are you building a feature or a healthcare product?
Below is how telemedicine software platforms and custom builds compare across the dimensions that actually matter at scale:
1. Platform vs Custom Telehealth Development
Deployment speed: Platforms enable rapid launch using ready infrastructure. Custom builds are built strategically for long-term product evolution.
Cost structure: Platforms have lower initial investment with subscription pricing. Custom builds are a strategic investment creating a proprietary digital health asset.
Customization: Platforms offer standardized workflows for quick adoption. Custom builds offer fully customizable workflows tailored to clinical and business needs.
Integrations: Platforms include pre-built integrations with common healthcare tools. Custom builds provide complete control over integrations with EHR, RPM, analytics, and AI systems.
Scalability: Platforms scale within the platform ecosystem. Custom builds are designed for enterprise scale and long-term product growth.
Product differentiation: Platforms offer standard telehealth capabilities. Custom builds enable unique virtual care experiences and differentiated products.
This table looks straightforward. The reality is not.
Here is what often happens in practice:
- Platforms accelerate early traction
- Custom builds enable long-term defensibility
The tension sits in the middle.
2. The hidden tradeoffs leaders encounter
Speed vs control: You launch in weeks with a platform. You refine for years with custom systems.
Standardization vs differentiation: Platforms enforce consistency. Custom builds enable uniqueness.
Vendor dependency vs ownership: Platforms reduce operational burden. Custom builds give you full control over the roadmap and data.
What happens when your vendor roadmap diverges from your product roadmap?
That is where many organizations hit friction.
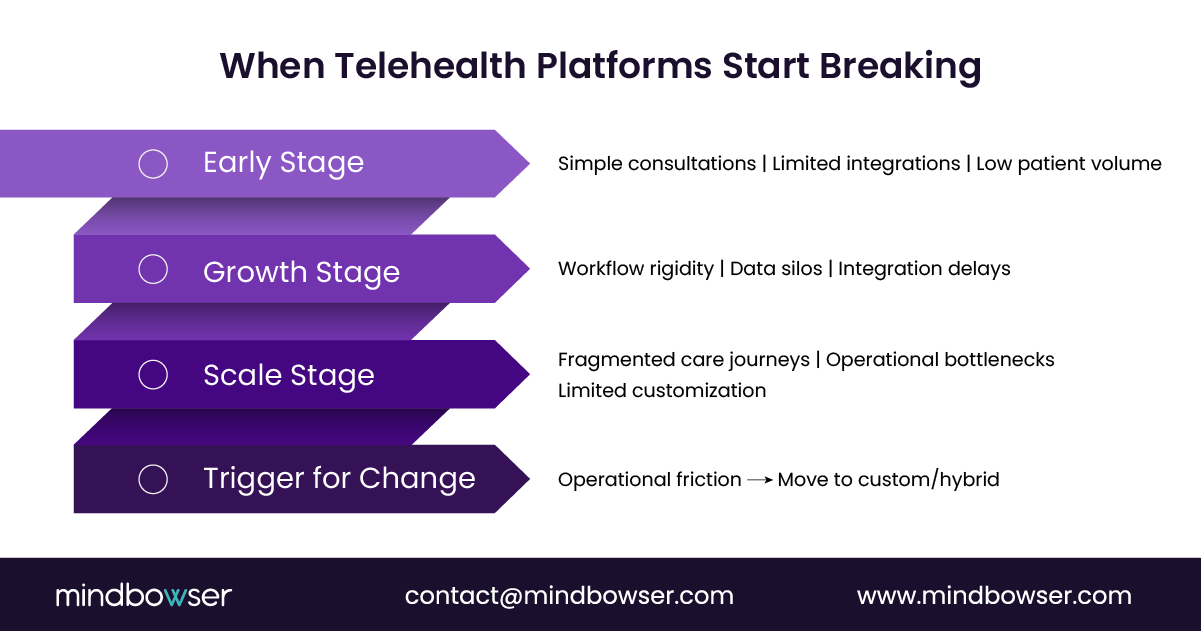
3. What changes at scale?
At a small scale, platform limitations are invisible.
At the growth stage, they become operational constraints:
- Limited workflow flexibility
- Integration bottlenecks
- Restricted data access
This is why many digital health companies evolve toward hybrid or custom models as they scale.
Telehealth platforms and custom builds are not competing choices. They represent different stages of maturity, and the real advantage comes from knowing when to transition between them.
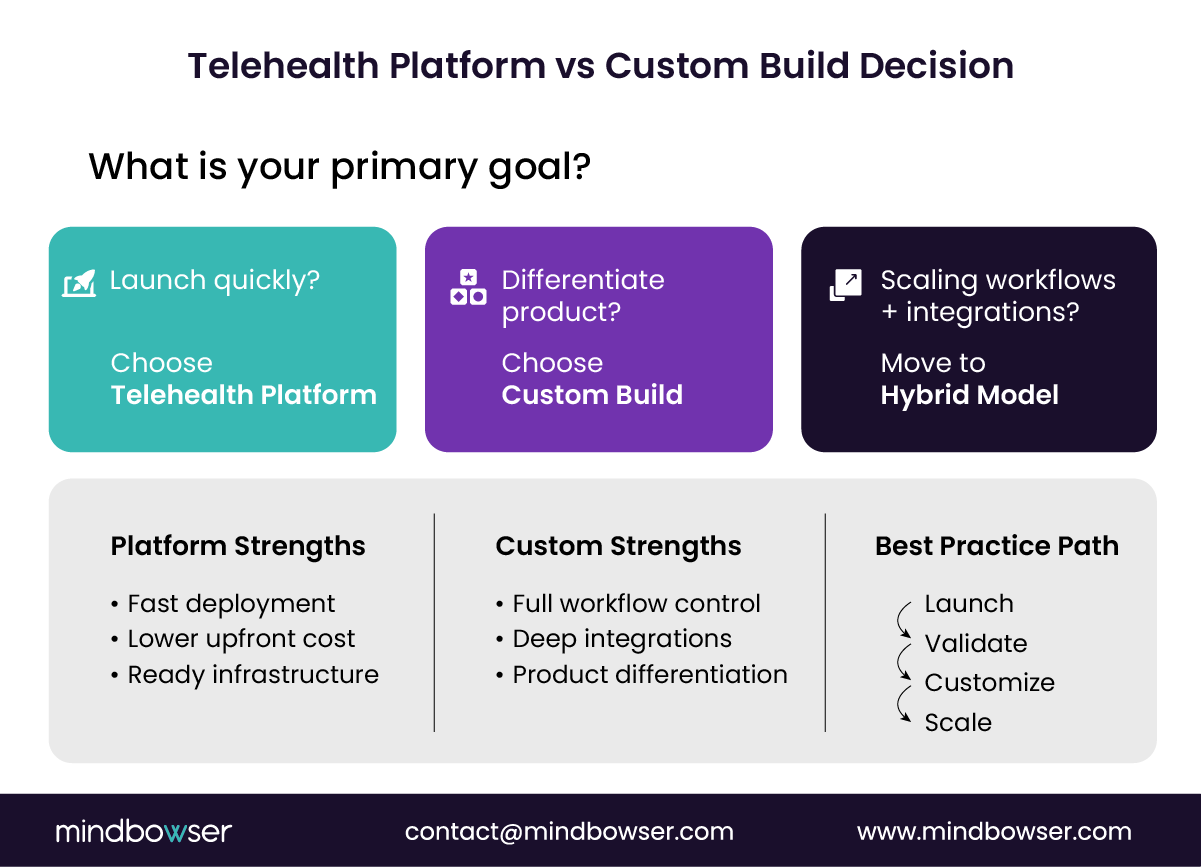
B. Which approach works best for different organizations
There is no universal right choice. Only contextual fit.
The mistake most teams make is copying what others are doing. The smarter move is aligning your telemedicine software platform strategy with your stage, complexity, and growth intent.
What works for a hospital system may fail for a startup. And vice versa.
1. Healthcare providers launching telehealth quickly
For provider groups and mid-sized health systems, the priority is often clear:
- Expand access fast
- Reduce patient leakage
- Improve operational efficiency
Telehealth platforms fit well here.
They allow organizations to:
- Launch virtual visits in weeks, not months
- Integrate basic workflows with existing systems
- Minimize upfront investment
If your goal is access expansion, speed matters more than customization.
However, as care models evolve into chronic care programs or specialty services, these organizations often revisit their architecture.
2. Digital health startups building scalable products
Startups operate under a different constraint:
- Validate quickly
- Iterate rapidly
- Differentiate early
Most begin with platforms to accelerate MVP development.
But once product-market fit emerges, priorities shift toward:
- Unique care models
- Patient engagement differentiation
- Data ownership
This is where custom development starts becoming attractive.
If your product is your platform, can you afford to depend on someone else’s?
The transition point is critical. Move too early, and you slow down. Move too late, and you inherit limitations.
3. Enterprise healthcare organizations with complex systems
Large health systems face a different reality altogether:
- Multiple EHR environments
- Complex payer relationships
- Diverse patient populations
For them, telehealth is not a feature. It is part of a broader digital health ecosystem.
Platforms can support initial deployment. But long-term success often requires:
- Deep interoperability
- Custom workflow orchestration
- Integration across departments and services
This is why many enterprise organizations move toward hybrid or custom architectures over time.
The question is not whether they will customize. It is how and when.
The best approach depends on your organizational stage and strategic priorities, but most healthcare organizations evolve from platform-first to more customized architectures as complexity and scale increase.
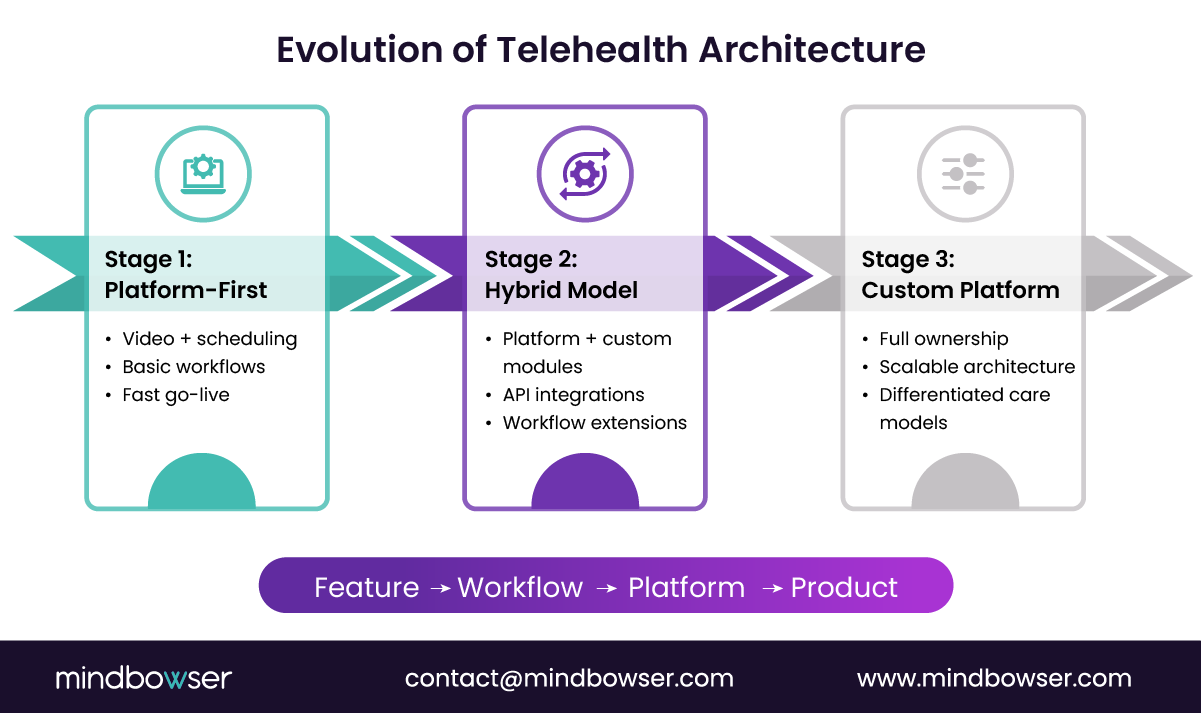
C. Hybrid platform models emerging in digital health
The smartest teams don’t choose. They combine.
The industry is moving beyond the platform vs custom debate. What’s emerging instead is a hybrid model that blends speed with control.
Why rebuild everything when you only need to control what differentiates you?
1. Platform infrastructure with custom modules
Organizations increasingly use telehealth platforms for:
- Video infrastructure
- Scheduling
- Basic workflows
Then layer custom components on top for:
- Clinical pathways
- Patient engagement logic
- Specialty care workflows
This approach reduces development time while preserving flexibility where it matters most.
2. API-first telehealth architectures
Modern platforms expose APIs that allow extension without full replacement.
This enables teams to:
- Replace modules incrementally
- Integrate specialized tools
- Build custom front-end experiences
You don’t need to rip and replace. You evolve.
However, success depends on how open and flexible the platform truly is. Limited APIs can still create hidden constraints.
3. Composable healthcare platforms
This is where things get interesting.
Composable architectures treat telehealth as a set of interchangeable components:
- Video engine
- Workflow orchestration
- Data layer
- Analytics
Each can be swapped or extended independently.
This aligns with how modern healthcare systems operate:
- Multi-vendor environments
- Rapidly changing care models
- Continuous innovation cycles
Hybrid models offer a pragmatic path forward, combining platform speed with custom flexibility, and are quickly becoming the preferred architecture for scalable virtual care.
V. How Should Digital Health Companies Evaluate Telemedicine Software Platforms?
A. Platform evaluation criteria
Choosing a telemedicine software platform is less about features and more about future fit.
The wrong choice does not fail immediately. It creates constraints as your product and care model evolve.
Will this platform still work when complexity increases?
1. Interoperability and EHR integration
Platforms must support bi-directional data exchange with EHRs and clinical systems using standards like HL7 and FHIR.
Without this, telehealth becomes a disconnected layer instead of part of the care continuum.
2. Security and HIPAA compliance
Healthcare platforms must ensure encryption, access control, and auditability by design.
With breaches exceeding $10 million per incident (IBM), security is a core architectural requirement, not an add-on.
3. Scalability and infrastructure performance
Platforms must handle increasing patient volume, concurrent sessions, and data complexity without performance degradation.
Cloud-based infrastructure supports this, but architecture quality determines real scalability.
Platform evaluation should focus on interoperability, security, and scalability, as these determine whether your telehealth system can support long-term growth.
B. Product strategy considerations
Platform decisions are product decisions.
Choosing a telemedicine software platform is not just about current needs, but also about how your product will evolve.
Are you optimizing for launch speed or long-term control?
1. Short-term speed versus long-term scalability
Platforms enable fast deployment and early validation.
But as workflows, integrations, and patient volumes grow, scalability limitations can create rework and architectural constraints.
2. Vendor lock-in risks
Platforms can restrict customization, data access, and roadmap flexibility.
If your product direction diverges from the platform, switching becomes costly and complex.
3. Platform extensibility for future features
Healthcare products evolve toward AI, remote monitoring, and advanced analytics.
Platforms must support extension through APIs or modular design, or risk becoming a bottleneck. McKinsey estimates generative AI could unlock $60B-$110B annually in healthcare, reinforcing the need for extensible systems.
Product strategy should guide platform decisions, balancing speed, control, and extensibility to avoid constraints as telehealth solutions scale.
C. Key questions startups should ask before selecting a platform
The wrong platform decision doesn’t fail immediately. It slows you down later.
That’s why smart teams don’t just evaluate features. They ask forward-looking questions that reveal hidden constraints.
Will this decision still hold when your product matures?
1. Can the platform support future integrations?
Your first integration is easy. Your tenth is not.
Startups should assess whether the telemedicine software platform can:
- Integrate with multiple EHR systems
- Support remote patient monitoring devices
- Connect with analytics and AI tools
What happens when you need real-time data across five systems?
If integration depth is limited, your product roadmap will be constrained.
2. Does it enable clinical workflow customization?
Clinical workflows evolve as your care model matures.
A platform should allow:
- Custom care pathways
- Dynamic patient journeys
- Multi-step treatment programs
If workflows are rigid, your team will spend time working around the system instead of improving care delivery.
Are you adapting your care model to the platform?
That is often the first warning sign.
3. Can it scale with patient demand and product growth?
Growth introduces both volume and complexity.
Evaluate whether the platform can:
- Handle increased patient load
- Maintain performance under peak demand
- Support expansion into new services or geographies
Deloitte notes that scalable digital health infrastructure is critical for sustaining virtual care growth, especially as hybrid care models expand.
Will performance hold when usage spikes 5x?
Many platforms work well at a small scale but struggle under pressure.
4. Who owns the data and experience?
This is often overlooked.
Clarify:
- Data ownership rights
- Access to patient insights
- Control over user experience
If you don’t own the experience, do you truly own the product?
This question becomes critical for startups building long-term value.
5. What is the exit path?
Every platform decision should include an exit strategy.
Assess:
- Data portability
- Migration complexity
- Vendor dependencies
Because at some point, you may need to move.
The right questions reveal whether a telehealth platform will support your growth or quietly limit it, making early evaluation critical for long-term success.
VI. How Mindbowser Helps Build Scalable Telemedicine Platforms
A. Custom telemedicine platform development
Building telehealth is easy. Building it to scale is not.
This is where most organizations hit friction. They launch fast using a telemedicine software platform, but as complexity grows, workflows break, integrations lag, and patient experience fragments.
That is the moment when architecture becomes strategy.
Mindbowser approaches telehealth differently. Not as a feature set, but as a long-term digital health asset.
1. Designing scalable virtual care architecture
Every scalable telehealth system starts with the right foundation.
Mindbowser designs platforms that:
- Support hybrid care models from day one
- Enable modular expansion as products evolve
- Align infrastructure with clinical workflows
This avoids the common trap of rebuilding systems after initial growth.
You don’t just launch. You prepare to scale.
2. Integrating telehealth platforms with EHR systems
Disconnected systems create fragmented care.
Mindbowser focuses on deep interoperability, enabling:
- Real-time EHR integration using FHIR and HL7 standards
- Unified patient records across virtual and in-person care
- Seamless data flow across clinical and operational systems
If data is delayed, care is delayed.
This integration layer ensures telehealth becomes part of the care continuum, not a parallel system.
3. Building secure HIPAA-compliant infrastructure
Security is not added later. It is built into the architecture.
Mindbowser develops telemedicine platforms with:
- HIPAA-compliant data handling by design
- SOC 2-aligned infrastructure practices
- End-to-end encryption and audit-ready systems
Trust is infrastructure in healthcare.
This approach ensures organizations can scale confidently without compromising compliance or patient safety.
Mindbowser helps organizations move beyond basic telehealth platforms by designing scalable, secure, and interoperable virtual care systems aligned with long-term growth.
B. Accelerators that accelerate telehealth development
Speed matters. But controlled speed wins.
Custom telemedicine development often slows teams down. Not because of complexity alone, but because teams rebuild components that already exist in some form.
Why start from zero when you can start from momentum?
This is where Mindbowser’s accelerators change the equation.
1. HealthConnect CoPilot for clinical workflow orchestration
Clinical workflows are the hardest part to standardize and the most critical to get right.
HealthConnect CoPilot enables:
- Configurable care pathways
- Multi-step clinical workflows
- Coordination across providers and care teams
Instead of hardcoding workflows, teams can design, adjust, and scale them dynamically.
This reduces engineering dependency while improving clinical agility.
2. AI-enabled patient engagement and care coordination
Engagement is where many telehealth programs lose momentum.
Mindbowser integrates AI-driven capabilities to support:
- Automated patient follow-ups
- Smart care reminders
- Intelligent triage and routing
McKinsey estimates that AI could generate $150 billion annually in healthcare value, much of it from workflow automation and engagement improvements.
Care doesn’t end after the visit. That’s where outcomes are shaped.
These capabilities help organizations maintain continuous patient interaction without increasing clinician burden.
3. Integration frameworks for digital health platforms
Integration delays slow growth more than most teams expect.
Mindbowser provides pre-built integration frameworks that accelerate:
- EHR connectivity
- Remote patient monitoring integration
- Data synchronization across systems
This reduces time spent on foundational work and allows teams to focus on product differentiation and care innovation.
You build what matters. We accelerate the rest.
Mindbowser’s accelerators reduce development time, enable flexible workflows, and support scalable integration, helping organizations move faster without sacrificing long-term architecture.
C. Supporting digital health companies from MVP to scale
Most telehealth products don’t fail at launch. They fail during growth.
Early traction is achievable with a telemedicine software platform. But as usage increases, care models expand, and integrations multiply, systems begin to strain.
The real challenge is not building an MVP. It is sustaining momentum without rebuilding everything.
1. Building telemedicine products for startups
For early-stage digital health companies, speed and validation matter most.
Mindbowser supports startups by:
- Launching MVPs using platform + custom hybrid models
- Designing scalable architecture from day one
- Avoiding technical debt that slows future growth
This ensures startups can move fast without compromising future flexibility.
You validate quickly, but you don’t corner yourself later.
2. Scaling virtual care infrastructure
Growth introduces complexity:
- Higher patient volumes
- Multi-program care delivery
- Expanded integrations
Mindbowser helps organizations scale by:
- Transitioning from platform-first to hybrid or custom architectures
- Optimizing infrastructure for performance and reliability
- Supporting enterprise-grade scalability
Deloitte highlights that scalable digital infrastructure is essential for sustaining virtual care expansion in hybrid healthcare models.
Can your system handle 10x growth without breaking workflows?
That is the real test.
3. Enabling interoperability across healthcare ecosystems
As organizations scale, interoperability becomes a competitive advantage.
Mindbowser enables:
- Seamless data exchange across EHRs, RPM devices, and analytics systems
- Unified patient experiences across care settings
- Integration with broader digital health ecosystems
This transforms telehealth from a standalone service into a connected care platform.
Disconnected systems limit care. Connected systems expand it.
Mindbowser supports digital health companies across their lifecycle, from rapid MVP launches to enterprise-scale virtual care platforms, ensuring systems evolve without breaking.
VII. What Does the Future Look Like for Telehealth Software Platforms?
A. AI-powered telehealth platforms
Telehealth is moving from virtual access to intelligent care delivery.
AI is transforming telemedicine software platforms by reducing clinician workload and enabling more proactive care models.
The shift is from enabling visits to guiding decisions.
1. AI-driven clinical documentation
AI automates transcription and clinical notes, reducing administrative burden and improving efficiency.
This allows clinicians to spend more time on care instead of documentation.
2. Virtual triage and care navigation
AI helps assess symptoms and route patients to the right level of care.
This improves access, optimizes provider capacity, and reduces unnecessary consultations.
3. Predictive healthcare insights
AI enables early identification of at-risk patients and supports proactive interventions.
AI is turning telehealth platforms into intelligent systems that improve efficiency, optimize care delivery, and enable more proactive healthcare models.
B. Integration of telehealth with remote patient monitoring
Virtual care is expanding beyond visits into continuous care.
Telehealth platforms are no longer limited to scheduled interactions. They are becoming part of a broader ecosystem where patient data flows continuously from outside clinical settings.
What if care didn’t stop when the consultation ended?
1. Wearables and IoT healthcare data
Devices such as smartwatches, glucose monitors, and cardiac sensors are generating real-time health data.
Modern telemedicine software platforms are beginning to integrate this data to:
- Track patient vitals continuously
- Detect early warning signs
- Support data-driven clinical decisions
This shifts care from episodic to continuous monitoring.
2. Continuous patient monitoring systems
Remote Patient Monitoring (RPM) enables providers to manage patients outside traditional settings.
This is especially critical for:
- Chronic disease management
- Post-discharge monitoring
- High-risk patient populations
CMS has expanded reimbursement for RPM programs, making them financially viable for more healthcare organizations.
Instead of waiting for deterioration, providers can intervene earlier.
That directly impacts outcomes and reduces hospital readmissions.
3. Chronic care management platforms
Telehealth combined with RPM creates a powerful model for chronic care.
Platforms can now support:
- Longitudinal care plans
- Automated alerts and interventions
- Ongoing patient engagement
WHO emphasizes that chronic diseases account for over 70% of global deaths, making continuous care models essential for modern healthcare systems.
Managing chronic conditions is not about one visit. It is about sustained engagement.
The integration of telehealth with remote patient monitoring is transforming virtual care into continuous care, improving outcomes while reducing the burden on healthcare systems.
C. Evolution of hybrid care ecosystems
Care is no longer virtual or physical. It is orchestrated.
The future of telemedicine software platforms is not about replacing in-person care. It is about blending digital and physical care into a unified experience.
Patients don’t think in channels. Why should healthcare systems?
1. Virtual-first healthcare models
Healthcare delivery is shifting toward virtual-first models where:
- Initial consultations happen digitally
- Triage determines the need for in-person care
- Follow-ups remain virtual
This model improves access while reducing unnecessary facility visits.
The goal is not fewer visits. It is smarter ones.
2. Integrated digital health platforms
Standalone tools are giving way to integrated platforms that connect:
- Telehealth
- Remote monitoring
- EHR systems
- Care coordination tools
This creates a single, unified care journey across touchpoints.
Patients experience continuity. Providers gain visibility. Systems operate more efficiently.
Disconnected tools create fragmented care. Integrated platforms create continuity.
3. Expansion of specialty telehealth services
Telehealth is moving beyond primary care into specialized domains:
- Behavioral health
- Dermatology
- Cardiology
- Oncology support
Each specialty introduces unique workflow and engagement needs.
This reinforces a key trend:
Generic platforms will struggle. Specialized, adaptable systems will lead.
Healthcare systems are increasingly designing service-line-specific virtual care models, supported by flexible platform architectures.
Hybrid care ecosystems represent the future of healthcare, where telehealth platforms act as the connective layer enabling seamless, continuous, and specialty-driven care delivery.

The Real Decision Behind Telehealth Strategy
Telehealth success is not defined by whether you choose a platform or a custom build, but by when and how you evolve between them. Telemedicine software platforms help you move fast, validate care models, and expand access, but long-term scale demands control over workflows, integrations, and patient experience.
As virtual care shifts toward hybrid models, AI-driven insights, and continuous monitoring, the underlying architecture becomes a strategy, not just a technical choice. The organizations that win will not be the ones that adopt telehealth first, but the ones that design it to adapt. The real question is simple: are you building for today’s access needs, or tomorrow’s care model?
Telehealth software platforms are digital systems that enable virtual care delivery, including video consultations, scheduling, and patient management. They act as the core infrastructure connecting patients, providers, and clinical systems.
Telemedicine software platforms connect patients and providers through secure digital interfaces that support communication, documentation, and care workflows. They integrate with systems like EHRs to ensure continuity of care across virtual and in-person settings.
A strong telehealth platform should include video consultations, scheduling, patient intake, EHR integration, and billing workflows. These features ensure care delivery is efficient, connected, and scalable.
Telehealth platforms provide the backend infrastructure for virtual care, while telemedicine apps are the user-facing interfaces. In simple terms, platforms power the system, and apps deliver the experience.
Early-stage startups typically use platforms to launch quickly and validate their product. As they scale and need differentiation, many transition toward custom development for greater control.
































