What if your watch could detect an irregular heartbeat before you felt it? Or your ring could silently flag the early signs of sleep apnea while you sleep?
This isn’t a vision for the distant future. It’s happening right now in 2026. Wearable technology in healthcare is evolving from fitness gadgets to intelligent clinical companions that extend the reach of care beyond hospital walls.
As demand for personalized, data-driven care grows, wearables are gaining significant traction. The market continues to expand rapidly as providers, MedTech companies, and digital health platforms invest in continuous monitoring, connected care, and real-time patient insight.
Wearables now offer more than vitals. They deliver context, trends, and behavioral signals that help clinicians make faster, smarter decisions at scale. For health systems, founders, and product leaders, this shift is not optional. It’s structural.
The biggest shift in 2026 is that wearables are no longer being evaluated only for patient engagement, they are increasingly being designed as part of care delivery, operational efficiency, and long-term clinical strategy.
What Are Healthcare Wearables and Why Are They Gaining Momentum?
Healthcare wearables are smart devices worn on the body that collect, transmit, and sometimes analyze physiological data in real time. Unlike traditional monitoring tools confined to clinical settings, these devices extend care into homes, daily routines, and sleep cycles.
The momentum is no accident. Healthcare is moving toward proactive, continuous care, where tracking heart rhythm, glucose, oxygen saturation, and sleep quality is part of everyday clinical insight, not an exception.
Here’s why healthcare wearables are gaining serious traction:
- Rise in chronic disease: Conditions like diabetes, hypertension, and COPD demand constant oversight. Wearables help clinicians and patients stay ahead of complications.
- Boom in remote care: Virtual-first and home-based models rely on wearables to bridge the gap between visits.
- Demand for real-time feedback: Patients expect immediate insight into sleep, stress, activity, and recovery.
- Behavioral accountability: Self-tracking turns patients into active participants in their care journey.
Wearables today are no longer step counters. They are becoming clinical tools that inform care plans, flag anomalies, and trigger early intervention. And the momentum is accelerating.
Types of Healthcare Wearables
The wearable landscape in healthcare continues to mature in 2026, moving well beyond basic fitness tracking.
Today’s devices are designed to collect clinical-grade data passively, continuously, and often invisibly, making them viable tools for real-world care delivery. Here’s a breakdown of the most impactful categories shaping healthcare wearables in 2026.
Smartwatches
Examples: Apple Watch Series 11 (FDA-cleared AFib and sleep apnea detection), Samsung Galaxy Watch 8 (blood pressure monitoring), Google Pixel Watch 3 (ECG)
Smartwatches have become frontline health monitors. In 2026, leading devices offer FDA-cleared capabilities for atrial fibrillation detection, sleep apnea screening, blood pressure monitoring, and ECG recording.
These watches provide clinicians with longitudinal insight into heart health, sleep patterns, and daily activity, all without disrupting a patient’s routine. For many patients, a smartwatch is now the first signal that something is off.
Biosensors and Smart Patches
Examples: Dexcom G7 (14-day wear), BioIntelliSense BioSticker (FDA-cleared), Abbott Lingo (wellness CGM)
Biosensors and adhesive patches are built for continuous, low-friction monitoring.
Devices like Dexcom G7 enable extended glucose monitoring, while FDA-cleared patches such as the BioIntelliSense BioSticker track vital signs such as respiratory rate, temperature, and activity around the clock. Abbott Lingo expands access through a wellness-focused CGM, providing users with actionable metabolic insights without clinical overhead.
These tools are especially valuable in chronic care, post-acute monitoring, and hospital-at-home models.
Rings and Discreet Wearables
Examples: Oura Ring Gen 4 (FDA sleep apnea detection), Ultrahuman Ring Air (HRV and recovery tracking)
Rings are emerging as powerful, low-profile health monitors. In 2026, devices like Oura Ring Gen 4 bring FDA-cleared sleep apnea detection into a form factor patients are willing to wear 24/7.
Ultrahuman Ring Air focuses on heart rate variability and recovery, offering insight into stress, readiness, and overall cardiovascular load.
Their discreet design drives adherence, while the data quality supports both wellness and clinical use cases.
Emerging Trends in Healthcare Wearables
In 2026, wearables will no longer be passive trackers. They’re active participants in care delivery, powered by smarter AI, deeper interoperability, and expanding clinical validation.
These trends are pushing wearables from optional add-ons into core healthcare infrastructure.
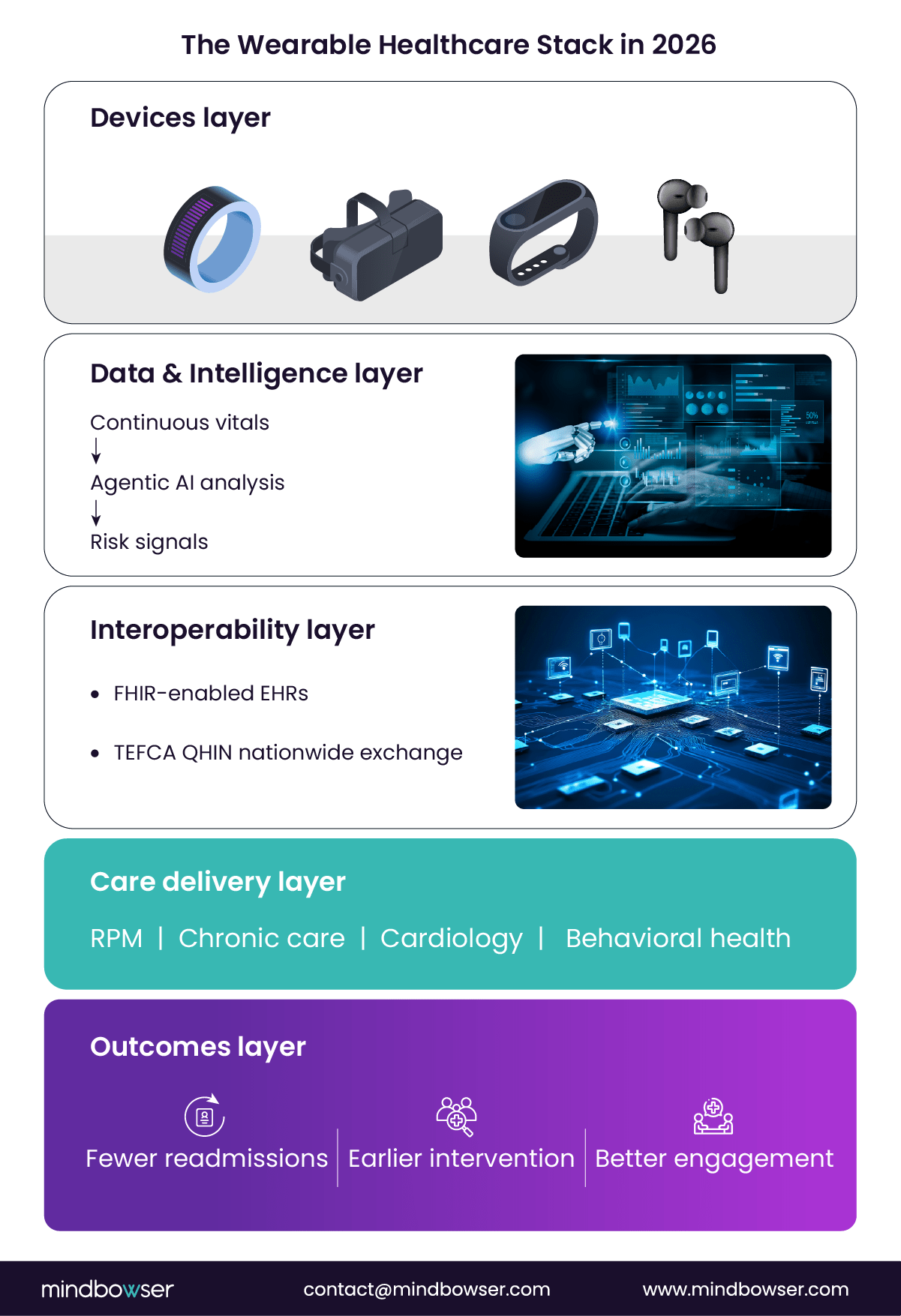
AI-Powered Predictive Monitoring
Wearables now deploy agentic AI models that go beyond pattern recognition. These systems can observe, reason, and act within defined clinical guardrails.
In practice, this means wearables can:
- Detect anomalies like arrhythmias, sleep apnea, or glucose irregularities before symptoms surface
- Continuously adapt thresholds based on patient behavior and historical data
- Generate prioritized risk signals that guide timely outreach from care teams
This shift turns wearables into early-warning systems rather than retrospective reporting tools.
The result is earlier intervention, fewer unexpected escalations, and stronger continuity of care.
EHR and Health System Integration
Interoperability has crossed a tipping point. 80%+ of major EHRs will be FHIR-enabled by 2026, making it much easier to embed wearable data directly into clinical workflows.
Platforms like HealthConnect CoPilot now allow:
- Real-time wearable vitals to appear inside Epic, Cerner, and Athena dashboards
- Alerts to trigger within existing clinician workflows
- Standardized, secure data exchange without custom plumbing
Wearable data is no longer stuck in patient apps or PDFs. It’s becoming part of the clinical record, where it can actually influence care decisions.
For organizations building connected care ecosystems, seamless wearable integration is essential to ensure device data flows securely into patient apps, dashboards, and clinical systems.
Expansion into Behavioral and Mental Health
Wearables are playing a growing role in mental and behavioral health by translating biometric signals into meaningful context.
Modern devices can:
- Monitor sleep quality, circadian rhythm, and recovery
- Track HRV and activity patterns associated with stress and burnout
- Surface early indicators of anxiety or depressive episodes
This data is increasingly paired with digital mental health platforms and therapy workflows.
From Consumer Devices to Clinical-Grade Tools
In 2026, the number of FDA-cleared and clinically validated wearable devices continues to grow, signaling stronger provider trust and wider adoption across remote monitoring, chronic care, and home-based care models.

Capabilities once limited to hospitals are now available on the wrist, chest, or finger, including:
- Atrial fibrillation detection
- Sleep apnea screening
- Continuous glucose and cardiac monitoring
This evolution expands access to care, supports home-based models, and allows health systems to monitor patients at scale without expanding brick-and-mortar capacity.
Build Your Scalable, Clinically Integrated Wearable Health Platform Today
Benefits of Wearables for Healthcare Providers and Hospitals
Wearables are no longer just enhancing patient experience. In 2026, they are reshaping how providers and hospitals deliver care, manage risk, and protect margins.
Continuous data from outside the clinic unlocks measurable clinical and financial upside across the system.
Fewer Hospital Readmissions

Remote monitoring enables clinicians to spot deterioration early and intervene before conditions escalate. This directly reduces emergency visits and avoidable readmissions, especially for chronic and post-discharge patients. These are some of the most valuable outcomes of a well-designed remote patient monitoring program.
Just as important, reimbursement has caught up. CMS reimburses $50+ per 30-day RPM period, making wearable-driven monitoring financially viable at scale. For value-based programs, this creates a clear line between better outcomes and sustainable revenue.
Related read: Value-Based Health Care: Transitioning to a Model for Better Patient Health Outcomes
Better Medication Adherence
Wearables support adherence through reminders, behavioral nudges, and passive monitoring.
When care teams identify patterns indicating missed doses or side effects, they can intervene early rather than waiting for deterioration. This is especially impactful for seniors and patients managing multiple medications.
Improved Clinical Decision-Making
Real-time insight into vitals, sleep, glucose, and activity replaces guesswork with evidence.
Clinicians gain longitudinal context instead of relying on episodic snapshots or patient recall.
The result is faster diagnosis, more precise treatment plans, and stronger care coordination across teams.
Streamlined Clinical Workflows
Wearables automate data capture and flow it directly into dashboards and EHRs. This reduces manual entry, eliminates fragmented logs, and frees clinicians to focus on patient care rather than administration. Less noise. More signal.
Rich Data for Research and Population Health
Continuous, longitudinal data from wearables fuels clinical research, population health analysis, and predictive modeling. When structured correctly, this data supports outcome studies, algorithm training, and program optimization without adding burden to care teams.
Higher Patient Satisfaction
Patients value proactive care, personalized insights, and fewer unnecessary visits. Wearables give them transparency and a sense of control, which builds trust and engagement over time. That trust shows up in retention, adherence, and outcomes.
Must-Have Features in Future Healthcare Wearable Apps
Building a wearable healthcare app is no longer about connecting a single device to a phone. It’s about designing a secure, interoperable system that integrates seamlessly into clinical workflows and patients’ lives. These features separate pilots from platforms.
Real-Time Health Alerts with Customizable Thresholds
Wearable apps must deliver timely alerts for events like abnormal heart rate, glucose spikes, or oxygen drops. Just as important, thresholds must be tailored to individual patients and care plans.
One-size-fits-all alerts create noise. Personalized alerts create action.
Cross-Device Compatibility
Healthcare no longer runs on one form factor. A future-ready app must support smartwatches, rings, patches, phones, and earbuds, ensuring consistent data capture regardless of how patients engage.
Multi-device support improves adherence and fills data gaps. If one device fails, another continues to capture the signal. That redundancy matters in clinical monitoring.
HIPAA-Compliant Secure Messaging
Care coordination belongs inside the app. Secure, encrypted messaging between patients and care teams reduces friction, shortens response times, and keeps sensitive conversations compliant with HIPAA and enterprise security standards.
Related read: HIPAA Compliance in Wearable Health Technology Key Considerations.
Data Synchronization with Backend Systems
Wearable data only becomes valuable when it reaches the right systems. Apps must sync cleanly with EHRs, care management platforms, and analytics tools so insights flow directly into care plans instead of living in silos.
This is increasingly achievable as TEFCA QHIN exchanges now live for nationwide data sharing, creating a foundation for trusted, large-scale health data exchange across networks.
Offline Support for Low-Connectivity Environments
Care does not stop when connectivity drops. Wearable apps must cache data locally and sync automatically once a connection is restored. This capability is critical for rural populations, home health programs, and post-discharge monitoring.
Actionable Insights with Personalized Recommendations
Raw data overwhelms users. Apps need to translate trends into clear, relevant guidance, such as sleep-impact patterns or behavior-recovery insights. The goal is clarity, not charts.
Flexible Notification Controls
Too many alerts lead to fatigue for both patients and clinicians. Users must be able to tune urgency, frequency, and delivery channels so critical signals stand out, and non-urgent updates stay quiet.
Scalable, Future-Proof Architecture
As device types, user volumes, and data streams grow, the underlying architecture must scale without rewrites. A future-proof design supports:
- Multi-device ingestion
- Real-time processing
- Multi-region deployments
- Regulatory evolution
Common Pitfalls in Wearable Healthcare Solutions
Even with the right strategy and investment, healthcare teams often face avoidable challenges when building wearable-enabled solutions. Understanding these pitfalls early can help reduce delays, improve adoption, and ensure better outcomes.
Inconsistent Data Quality Across Devices
Not all wearables deliver the same level of accuracy. Variations in device quality can lead to unreliable data, especially across different user conditions. It’s important to validate device data and define clear thresholds before using it in clinical workflows.
Lack of Clinical Context in Data Presentation
Simply sending wearable data to systems is not enough. If the data lacks context—such as trends, baselines, or actionable insights clinicians are less likely to use it effectively. Data must be presented in a way that supports real decision-making.
Overloading Users with Unnecessary Features
Trying to capture every possible metric often leads to complex systems that neither patients nor providers use. Focus on collecting and presenting only the data that drives action and improves care outcomes.
Delays Due to Poor Integration Planning
Building integrations from scratch without proven frameworks or accelerators can slow down development. A strong wearable integration strategy ensures faster implementation and reduces technical risks.
Real-Life Use Cases Shaping the Future
In 2026, wearable technology is actively shaping care delivery across multiple specialties. These use cases show how continuous data, when paired with clinical workflows, drives better outcomes and operational efficiency.
Real-World Product Examples
The future of wearable healthcare is already taking shape through real-world platforms that connect device data with actionable care workflows.
Connected Monitoring Platforms
We have built wearable-enabled platforms that use device data to support real-time monitoring, patient engagement, and better care decisions. These solutions help care teams track patient vitals remotely and take action early when risks are detected. This is a key part of remote patient monitoring solutions, where patient data is continuously tracked outside clinical settings.
Integrated Health Experiences
We have also developed solutions that go beyond standalone apps by bringing health monitoring into everyday use. These platforms combine data from multiple devices to deliver simple insights, improve engagement, and support preventive care. This approach depends on strong wearable integrations to ensure data flows smoothly between devices, apps, and healthcare systems.
Diabetes Monitoring: Dexcom Integrated with EHR
Continuous glucose monitoring has taken a clear step forward. In 2026, diabetes programs are transitioning from Dexcom G6 to G8, expanding accuracy, wear time, and real-time insights.
When CGM data flows into EHRs through platforms like HealthConnect CoPilot, care teams can:
- Spot glucose trends before they become events
- Adjust insulin or lifestyle plans remotely
- Reduce avoidable clinic visits while maintaining control
For patients, this means fewer surprises. For providers, it means proactive diabetes management at scale.
Rehabilitation: Smart Wearables for Post-Surgical Recovery
Motion-aware wearables are increasingly used in post-operative rehab to track range of motion, gait, and activity consistency. These insights help therapists tailor recovery plans without requiring frequent in-person visits.
Patients stay engaged. Clinicians stay informed. Recovery stays on track.
Cardiology: Continuous Cardiac Insight at Home
Cardiac monitoring has moved beyond episodic checks. In 2026, devices like WHOOP 5.0 cardiac strain monitoring provide continuous insight into cardiovascular load, recovery, and stress.
Combined with wearable ECG and heart rhythm data, care teams can:
- Detect early signs of cardiac strain
- Personalize activity and recovery guidance
- Support safer rehabilitation and long-term heart health
This approach reduces unnecessary admissions while keeping high-risk patients under close watch.
Elderly Care: Fall Detection and Mobility Monitoring
Wearables equipped with motion sensors remain critical in elderly care.
Real-time fall detection triggers immediate alerts to caregivers or emergency services, while mobility trends indicate a gradual decline before a crisis.
The result is faster response times, safer aging at home, and greater confidence for families.
Wearables also track long-term activity and health patterns, helping detect gradual decline and enabling earlier intervention before serious events occur.
Post-Discharge RPM: Monitoring After Hospital Release
Hospitals are increasingly deploying wearable-based remote patient monitoring kits after discharge. Continuous tracking of vital signs and behavior during this vulnerable period enables clinicians to intervene early and prevent complications.
This model supports smoother transitions of care and directly contributes to lower readmission rates.
Common Challenges in Wearable Healthcare
Building effective wearable solutions requires more than device connectivity. It depends on secure integration, scalable infrastructure, and aligning data with real clinical workflows from the start.
Data Fragmentation and Interoperability
Different devices often use different data formats, making it difficult to integrate information into EHRs and clinical systems. Without standardization, valuable data remains underutilized.
Compliance and Data Security
Wearables handle sensitive health data, which requires strong security measures. Encryption, access controls, and compliance with healthcare regulations like HIPAA are critical to protect patient information.
Patient Adoption and Engagement
Even the most advanced device has limited value if patients do not use it consistently. Simplicity, reliability, and clear value are essential to ensure long-term usage.
Scalable Infrastructure
As wearable adoption grows, healthcare systems must handle increasing volumes of real-time data. Without a scalable architecture, performance and reliability can suffer.

Where Wearable Healthcare Is Headed Next?
The future of wearable technology in healthcare is no longer theoretical. In 2026, it’s actively reshaping how care is delivered, monitored, and scaled across the system.
From agentic AI–powered monitoring and FDA-cleared consumer devices to deep EHR integration and nationwide data exchange, wearables have become foundational infrastructure for modern care models. This shift is happening alongside massive market momentum. This shift is happening alongside strong market momentum, with sustained investment in digital health, remote monitoring, and interoperable care platforms across providers, payers, and digital health companies.
But devices alone don’t drive outcomes. Real impact comes from how wearable data is designed into workflows, translated into insight, and connected to clinical action. Health systems and founders who invest now in the right platforms, integrations, and user experiences will be positioned to lead as connected care becomes the default.
At Mindbowser, we help healthcare innovators turn wearable concepts into production-ready, compliant, and scalable solutions.
The future is wearable. Let’s build it together.
Wearables deliver continuous patient data, reduce hospital readmissions, improve medication adherence, and streamline clinical workflows. They also support better decision-making and enable scalable data collection for research and population health programs.
Modern wearables integrate with EHRs such as Epic, Cerner, and Athena using interoperability standards like HL7 and FHIR. Platforms like HealthConnect CoPilot enable secure data syncing, alerts, and visualization directly inside clinician workflows.
They can be, when designed correctly. HIPAA-compliant wearable solutions require end-to-end encryption, secure data storage, role-based access controls, and detailed audit logs to protect sensitive health information.
Fitness wearables are consumer-focused and may lack regulatory clearance and clinical accuracy. Clinical-grade wearables are often FDA-cleared, validated for medical use, and built to integrate with healthcare systems.
In 2026, key advancements include FDA-cleared sleep apnea detection (Oura Ring Gen 4), blood pressure monitoring on smartwatches (Samsung Galaxy Watch 8), and the use of agentic AI models that proactively detect risk and guide interventions rather than just reporting data.
































