TL;DR
- A custom telemedicine app becomes essential when SaaS platforms can’t support evolving care models, integrations, or scale.
- As virtual care expands beyond basic visits, organizations need workflow-driven systems, deeper EHR connectivity, and the flexibility to add capabilities like AI and RPM.
- The real advantage isn’t just faster launch, it’s the ability to scale efficiently, reduce operational friction, and build a platform that adapts as clinical and business needs grow.
What happens when your telemedicine platform starts slowing down your care delivery instead of enabling it?
Most digital health teams don’t feel this at launch. It shows up later when workflows become complex, integrations break, and scaling introduces friction across systems.
As virtual care moves beyond basic video visits, the need shifts from simple tools to connected, workflow-driven platforms.
That’s where a custom telemedicine app becomes less of an option and more of a strategic necessity.
I. Why Are Digital Health Startups and Providers Building Custom Telemedicine Apps?
What happens when your telemedicine platform starts limiting your care model instead of enabling it?
That’s the moment most teams realize something is off.
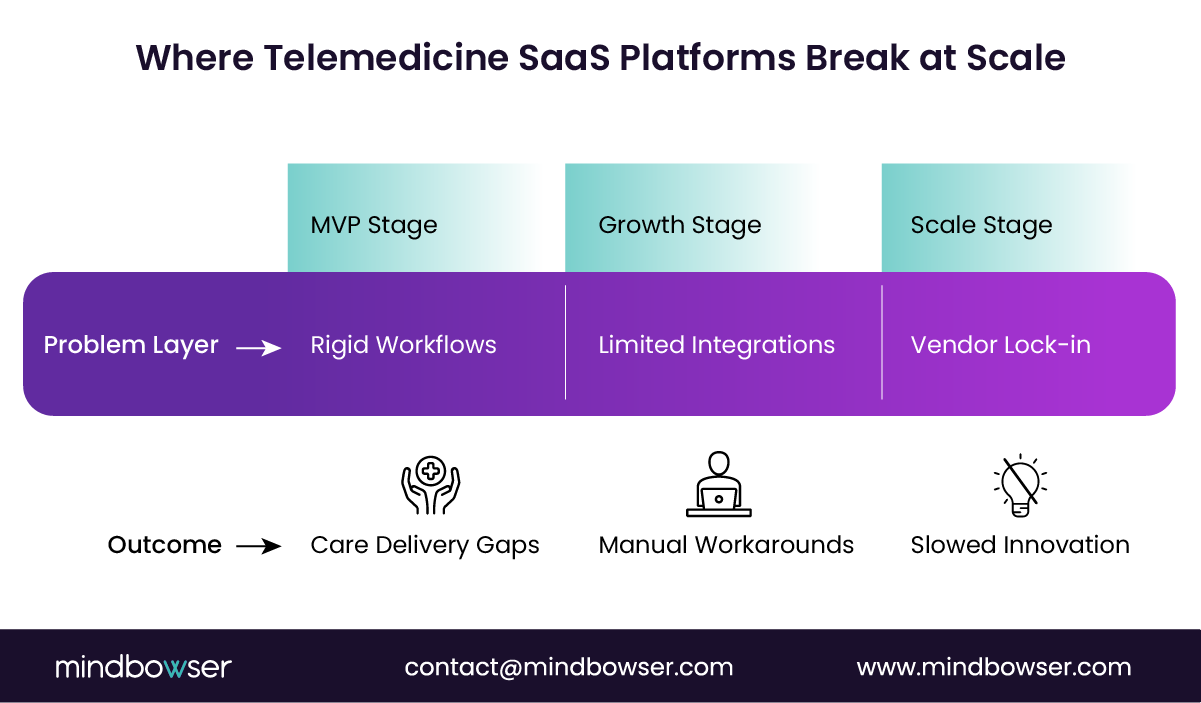
What began as a fast MVP using a SaaS telehealth tool turns into a bottleneck. Clinical workflows don’t quite fit. Integrations feel forced. Scaling introduces friction at every layer.
This isn’t a temporary spike. It’s a structural shift in how care is delivered.
And here’s the problem.
Most off-the-shelf telemedicine platforms were built for basic virtual visits, not for:
- Longitudinal care programs
- Multi-specialty expansion
- Value-based care workflows
- Deep EHR and device integrations
So when startups and providers scale, cracks appear.
A familiar scenario:
- A Series B digital health company expands into chronic care. They need RPM integration, care plans, async follow-ups, and payer reporting.
Related read: Telemedicine Software Development with AI: From Clinical Summaries to RPM Integration
But their platform?
- Video works
- Scheduling works
- Everything else becomes manual workarounds
That’s not scale. That’s technical debt disguised as progress.
That shift forces a different mindset.
From feature adoption → workflow ownership
From vendor dependency → platform control
From short-term speed → long-term scalability
A custom telemedicine app is not about reinventing video calls. It’s about building a system where:
- Clinical workflows match real care delivery
- Data flows cleanly across systems
- Product decisions align with outcomes and revenue
And one uncomfortable truth.
The cost of staying on SaaS often shows up later, in lost efficiency, provider burnout, and stalled innovation.
Digital health leaders move to custom when their business model outgrows their tools.
A. What Limitations Do SaaS Telemedicine Platforms Create?
If SaaS telemedicine platforms are so easy to launch with… why do they become the first thing teams want to replace?
Because convenience at the start often turns into constraint at scale.
Most SaaS platforms are designed for standard virtual visit workflows. That works for early-stage validation. It breaks when care delivery becomes nuanced, multi-layered, and data-driven.
Let’s unpack where the friction shows up.
1. Restricted Customization
SaaS platforms operate on predefined logic.
You get:
- Fixed patient journeys
- Limited workflow branching
- Minimal control over UI/UX
Now consider a real-world need:
- A cardiology program requires pre-visit vitals, device data ingestion, and post-visit care plans with automated follow-ups.
Can your platform adapt?
Usually not.
So teams build workarounds. External forms. Manual tracking. Disconnected systems.
That’s not product design. That’s patchwork.
Key issue: Your care model starts bending to fit the tool, rather than the tool supporting the care model.
2. Limited Integrations
What happens when your telemedicine app can’t talk to your EHR, billing system, or RPM devices in real time?
Everything slows down.
Most SaaS platforms offer surface-level integrations, often through:
- Basic APIs
- Delayed data sync
- Limited support for FHIR-based interoperability
But modern care delivery depends on:
- Real-time EHR updates
- Device streaming (RPM)
- Automated billing and coding workflows
Without deep integration, you get:
- Data silos
- Duplicate entry
- Incomplete patient records
And for leadership?
No single source of truth.
3. Platform Dependency
This is the silent risk.
When you rely on SaaS:
- Your roadmap depends on vendor priorities
- Feature releases are out of your control
- Pricing scales with usage, not value
Now imagine:
- You want to introduce AI-driven visit summaries or asynchronous care pathways.
But your vendor?
Doesn’t support it. Or delays it. Or charges heavily for customization.
Growth stalls. Innovation slows.
And one more concern leaders often underestimate.
Data ownership.
Who controls patient interaction data? How easily can you migrate it? Can you build analytics on top of it?
If the answer isn’t clear, that’s a strategic risk.
SaaS telemedicine platforms help you start fast. But they often limit how far you can go.
B. Why Do Digital Health Startups Prefer Custom Telemedicine Apps?
If SaaS creates friction… what exactly makes custom worth the investment?
It comes down to one thing.
Control over how care is delivered, measured, and scaled.
For digital health startups and provider organizations, a custom telemedicine app is not just a technical upgrade. It is a strategic lever that directly impacts clinical outcomes, operational efficiency, and revenue models.
Let’s break that down.
1. Unique Care Models Demand Flexible Architecture
No two care models are identical.
A behavioral health platform needs asynchronous therapy and journaling.
A chronic care platform needs RPM, alerts, and longitudinal tracking.
A specialty clinic may require hybrid care, with in-person and virtual components coordinated.
Can a one-size-fits-all platform support all that?
Rarely.
Custom apps allow teams to design:
- Workflow-first experiences instead of feature-first interfaces
- Dynamic care pathways based on patient conditions
- Automated clinical protocols tied to outcomes
The product becomes an extension of the clinical model rather than a constraint.
2. Data Ownership Becomes a Strategic Asset
Who owns your patient data, and can you actually use it?
This question becomes critical as organizations scale.
With custom platforms, you gain:
- Full access to longitudinal patient data
- Control over analytics, reporting, and AI models
- Freedom to integrate across systems without restrictions
Contrast that with SaaS:
- Limited data export
- Restricted analytics layers
- Vendor-controlled infrastructure
Now consider value-based care.
You need to track outcomes, utilization, adherence, and cost efficiency across cohorts.
Without full data control?
You’re guessing instead of optimizing.
That level of impact requires ownership at the data layer.
3. Feature Scalability Without Vendor Constraints
Growth introduces new requirements. Fast.
- New specialties
- New payer models
- New geographies
- New compliance needs
With a custom telemedicine app, you can:
- Add features incrementally without breaking the system
- Introduce AI capabilities, RPM, or care coordination layers
- Adapt quickly to regulatory or reimbursement changes
With SaaS?
You wait. Or workaround. Or switch platforms entirely.
None of those scales well.
And here’s the executive reality.
Speed is not just about launching fast. It’s about iterating without friction.
This works. Period.
Digital health startups prefer custom telemedicine apps because they align technology with business models, not the other way around.
C. When Should Organizations Build?
So, when is the right moment to move from SaaS to a custom telemedicine app? Too early, and you overinvest. Too late, and you stall growth.
This decision is less about timing and more about signals.
Let’s look at the inflection points.
1. New Virtual Care Models Are Emerging
As your care delivery evolves beyond simple video visits, SaaS begins to show its limits.
Think about:
- Chronic care management programs
- Behavioral health with async + sync care
- Hospital-at-home or hybrid care models
These models require:
- Multi-step workflows
- Continuous patient engagement
- Integration with devices and care teams
If your platform can’t support longitudinal care, you’re not delivering modern healthcare; you’re replicating clinic visits online.
Nearly 50% of healthcare services could be delivered virtually. McKinsey.
That opportunity demands infrastructure that goes beyond video.
Signal: If your care model is changing faster than your platform can adapt, it’s time to build.
2. Multi-Specialty Scaling Introduces Complexity
Growth sounds simple. It isn’t.
Adding specialties means:
- Different intake workflows
- Different clinical protocols
- Different documentation needs
- Different billing pathways
A dermatology flow is not a cardiology flow. A mental health visit is not a post-surgical follow-up.
SaaS platforms tend to standardize.
But real healthcare?
It diversifies.
Without customization, teams end up:
- Creating parallel systems
- Managing fragmented workflows
- Increasing operational overhead
That directly impacts provider efficiency and patient experience.
Scaling specialties without platform flexibility creates hidden operational costs.
3. Platform Integration Becomes Mission-Critical
At scale, your telemedicine app doesn’t operate in isolation.
It must connect with:
- EHR systems (FHIR-based interoperability)
- Billing and revenue cycle tools
- Remote patient monitoring devices
- Analytics and reporting platforms
What happens when these integrations fail or lag?
Care slows down. Data becomes unreliable. Decisions lose accuracy.
That’s not just a tech issue. It’s a financial one.
A custom telemedicine app allows you to:
- Design integration-first architecture
- Enable real-time data exchange
- Maintain a unified patient record
No workarounds. No silos.
Organizations should build when their growth introduces complexity that SaaS platforms cannot support without friction.
II. What Features Should a Custom Telemedicine App Include?
Building a custom telemedicine app is more than just offering video consultations. It’s about creating a comprehensive digital health platform that aligns with clinical workflows, enhances provider efficiency, and improves patient outcomes.
Let’s break down the essential features that make a telemedicine app truly effective.
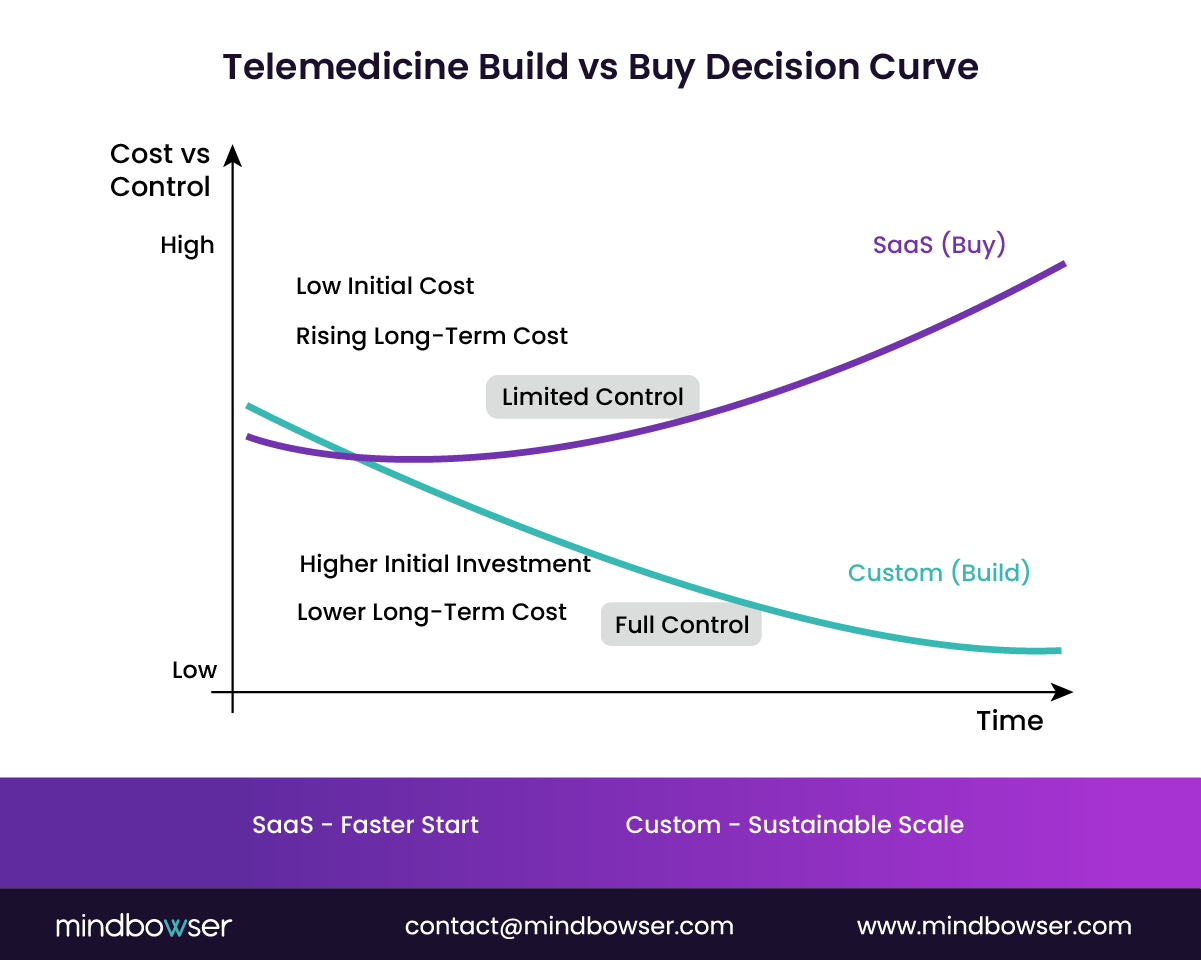
A. What Core Modules Are Required for Telemedicine Platforms?
A custom telemedicine platform should have three interconnected layers to ensure smooth functionality across all user types:
- Patient Application: The patient-facing application is where engagement happens, so it needs to offer more than just appointment booking. The patient app should provide a seamless onboarding process, allow for easy scheduling, and enable secure messaging for ongoing communication with providers. This module is the cornerstone of patient experience, ensuring that users can access care quickly, intuitively, and securely.
- Provider Dashboard: The provider dashboard is designed to optimize workflows and reduce administrative overhead. It should integrate various clinical tools, allowing healthcare professionals to manage patient interactions, access medical records, input clinical data, and generate prescriptions seamlessly. A unified view of patient information, including visit history, vitals, and device data, ensures providers can deliver informed care quickly and accurately.
- Admin Portal: The admin portal is essential for managing the platform at scale. It allows administrators to manage provider schedules, track billing, handle user access control, monitor platform performance, and ensure compliance with regulations. Operational efficiency depends on this module, especially as the organization grows and requires centralized control and oversight.
B. What Clinical Capabilities Are Essential in Telemedicine Apps?
For a telemedicine app to be truly effective, it must integrate clinical capabilities that streamline the care journey. These are the critical features that make the platform functional for healthcare providers and their patients:
- Secure Video Consultations: The core of telemedicine is, of course, video consultations. WebRTC technology is often used to provide real-time, secure, low-latency video interactions. These sessions must be encrypted, with adaptive bitrate streaming for different network conditions, ensuring a high-quality experience for both patients and providers. The ability to offer secure video calls without disruption is a foundational requirement.
- Electronic Prescriptions & Clinical Documentation: Integrating e-prescriptions and clinical documentation into the platform is essential for efficient care delivery. Custom telemedicine apps allow for seamless interaction with EHR systems, enabling healthcare providers to issue prescriptions, document visit summaries, and update patient records in real time. This reduces administrative burdens and ensures the accuracy and completeness of medical records.
- Patient Intake & Triage: A well-designed intake process can significantly improve the patient experience and reduce wait times. Custom telemedicine platforms should include symptom checkers, automated intake forms, and triage workflows that guide patients through the necessary steps before their consultation. This allows providers to get a complete view of the patient’s condition ahead of the visit, ensuring they’re fully prepared to deliver the right care.
C. What Advanced Features Differentiate Modern Telemedicine Platforms?
To stay competitive in the rapidly evolving digital health landscape, telemedicine platforms need to go beyond basic video visits and administrative functions. Here are the advanced features that set apart modern, high-performing telemedicine apps:
- AI-Powered Clinical Summaries: AI can reduce friction in clinical workflows, such as automating visit summaries and generating clinical documentation. AI tools can process patient data and generate clinical insights, which helps reduce physician burnout and improve productivity. AI-driven decision support tools can also guide clinical decision-making, helping providers make better-informed choices during patient consultations.
- Remote Patient Monitoring (RPM) Integration: Remote patient monitoring is essential for continuous care, especially for patients with chronic conditions. Integrating RPM into telemedicine apps enables providers to track patient vitals, receive real-time alerts for anomalies, and intervene promptly when necessary. This makes the care model more proactive, reducing hospital readmissions and improving patient outcomes. RPM is a critical feature for value-based care models.
- Care Coordination Tools & Population Health Analytics: As telemedicine becomes more integrated into broader healthcare delivery models, care coordination becomes increasingly important. Custom telemedicine platforms should include features for shared care plans, task assignment, and real-time communication among care teams. Population health analytics can help identify trends in patient health, track outcomes across different cohorts, and enable healthcare providers to manage chronic conditions more effectively.
III. What Features Should a Custom Telemedicine App Include?
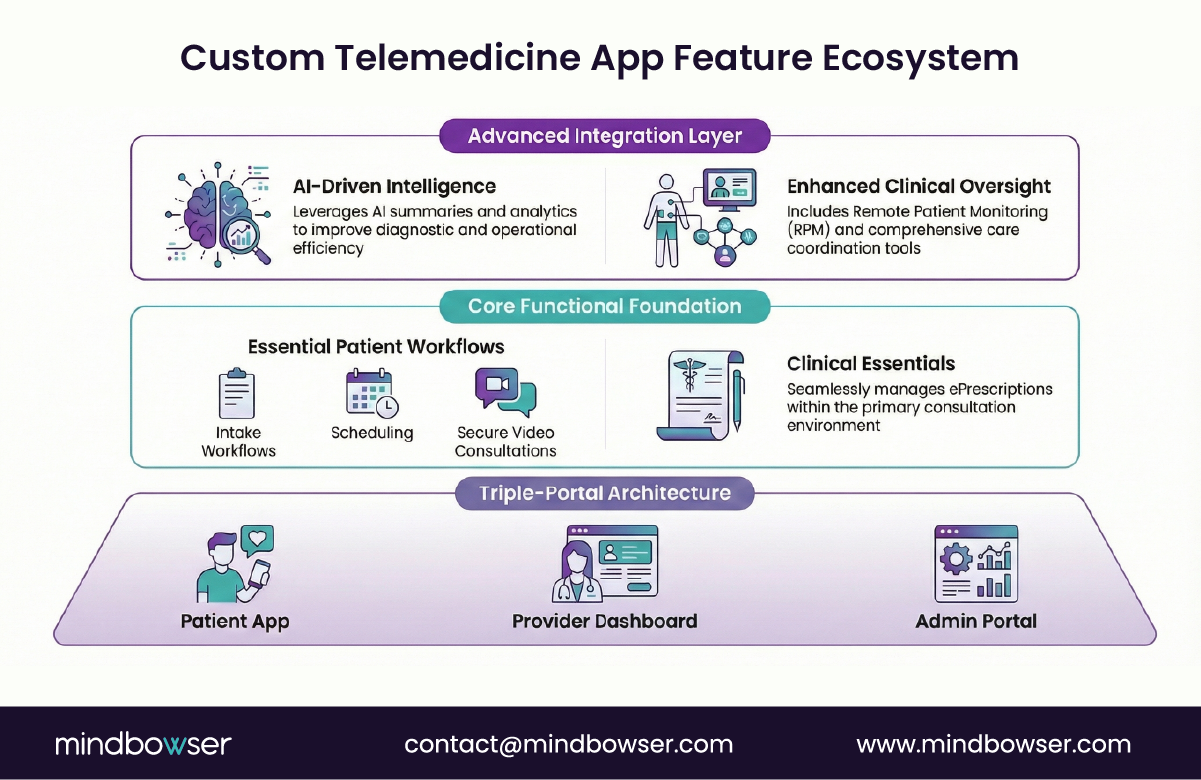
What separates a telemedicine app that “works” from one that actually drives outcomes, retention, and revenue?
It’s not just features.
It’s how those features map to clinical workflows, provider efficiency, and patient engagement across the care journey.
Let’s break this into what matters most.
A. Core Modules and Clinical Capabilities
At the foundation, every custom telemedicine app needs three interconnected layers:
- Patient-facing experience
- Provider-facing workflows
- Administrative control
But here’s where many teams get it wrong.
They build features in isolation instead of designing connected systems.
1. Patient App: Engagement Drives Retention
The patient interface is not just for booking calls. It’s where adherence, satisfaction, and outcomes are shaped.
Core capabilities include:
- Appointment scheduling with dynamic availability
- Secure messaging and async communication
- Video consultations
- Access to prescriptions and visit summaries
But here’s the deeper question.
Does your app guide patients through care or just react to requests?
High-performing platforms add:
- Guided intake workflows based on condition
- Reminders tied to treatment plans
- Continuous engagement beyond visits
That’s not a UX upgrade. That’s a clinical impact.
2. Provider Dashboard: Workflow Efficiency Is Everything
Providers don’t need more tools. They need fewer clicks.
A well-designed dashboard enables:
- Unified patient view (history, notes, vitals, device data)
- Real-time alerts and notifications
- Documentation and ePrescription workflows
- Integrated video consultations
- Now consider a common failure point.
Providers switching between:
- Video platform
- EHR
- Notes system
- Billing tool
- That fragmentation kills productivity.
Custom platforms solve this by embedding:
- EHR integrations (FHIR-based)
- Automated documentation flows
- AI-assisted note generation
Physicians spend nearly 2 hours on EHR tasks for every hour of patient care.
Reducing that burden directly impacts margins and burnout.
3. Admin Portal: Operational Control at Scale
As organizations grow, operational complexity increases fast.
Admins need visibility into:
- Provider schedules and utilization
- Patient flow and no-show rates
- Billing and reimbursement tracking
- Compliance and audit logs
Without this layer?
Scaling becomes guesswork.
A custom telemedicine app enables:
- Role-based access control
- Real-time reporting dashboards
- Automated workflow management
Admin tools are not back-office features. They are growth enablers.
B. Advanced Features That Drive Differentiation
Once the foundation is in place, differentiation begins.
This is where leading platforms move ahead.
1. AI-Powered Clinical Workflows
AI is not just hype in telemedicine. It’s already reducing friction.
Use cases include:
- Automated visit summaries
- Clinical decision support
- Risk stratification
Imagine reducing documentation time by 50%.
That’s not future-state. It’s happening now.
2. Remote Patient Monitoring (RPM) Integration
Care doesn’t stop after the visit.
RPM enables:
- Continuous tracking of vitals
- Alerts for anomalies
- Data-driven interventions
This is critical for:
- Chronic care
- Post-discharge monitoring
- Value-based care models
Without RPM, telemedicine becomes episodic.
With it, care becomes continuous.
3. Care Coordination and Multi-Channel Engagement
Modern care involves teams.
Physicians, nurses, care managers, specialists.
A custom platform enables:
- Shared care plans
- Cross-team communication
- Task assignment and tracking
What happens when coordination fails?
Care gaps. Readmissions. Poor outcomes.
That’s both a clinical and financial risk.
The right features don’t just enable telemedicine. They transform it into a scalable, outcome-driven care platform.
IV. What Technology Stack Powers a Custom Telemedicine App?
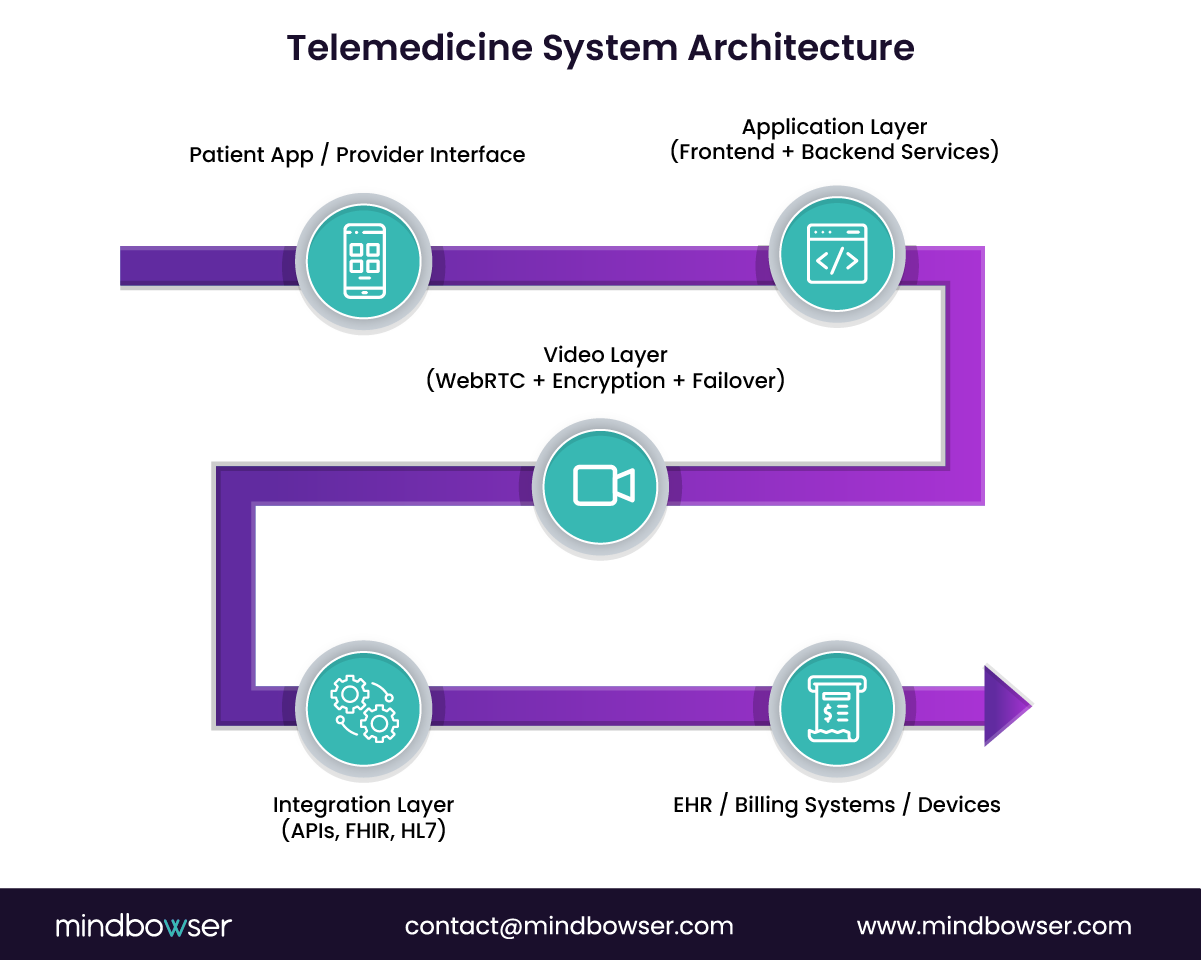
What breaks first when your telemedicine platform scales: UI, backend, or video?
In most cases, it’s not one layer. It’s the lack of alignment across all three.
No single technology defines a high-performing custom telemedicine app. It’s defined by how well those technologies work together under real clinical load.
Let’s unpack the stack.
A. Frontend and Backend Foundations
Your frontend is what users see. Your backend is what determines whether the system holds up under pressure.
For patient and provider apps, teams typically use:
- Flutter or React Native for cross-platform development
- Web interfaces (React.js) for admin and provider dashboards
Why this matters:
- Faster development cycles
- Consistent UX across devices
- Lower maintenance overhead
On the backend:
- Node.js for real-time performance (ideal for messaging, notifications)
- Python for data-heavy workflows and AI integration
And then comes infrastructure.
- AWS or Azure for cloud scalability
- Microservices architecture for modular growth
- Containerization (Docker/Kubernetes) for deployment flexibility
Here’s the real question.
Can your system handle a 10x patient load without re-architecture?
If not, the problem isn’t traffic. Its foundation.
B. Video Infrastructure: The Core of Virtual Care
Video is not just a feature. It is the clinical interface.
Most modern platforms rely on:
- WebRTC for real-time, low-latency communication
- End-to-end encryption protocols for secure sessions
- Adaptive bitrate streaming for variable network conditions
But here’s where many systems fail.
They assume video works the same in all environments.
In reality:
- Hospital networks behave differently from home Wi-Fi
- Mobile networks introduce instability
- Global expansion adds latency challenges
So production-ready systems include:
- Failover mechanisms (switching between video providers if needed)
- Session recovery logic
- Real-time monitoring of call quality
If video drops during a critical consult, trust drops with it.
That’s not just UX. That’s patient experience and retention.
C. Healthcare Integration and Interoperability
What’s the value of a telemedicine app if it operates in isolation?
None.
Integration is where most implementations struggle and where custom platforms win.
Key standards and systems include:
- FHIR (Fast Healthcare Interoperability Resources) for structured data exchange
- HL7 interfaces for legacy system compatibility
- Integration with EHRs (Epic, Cerner, Athenahealth)
- Billing and revenue cycle systems
But integration is not just about connectivity.
It’s about:
- Real-time synchronization
- Data normalization across systems
- Maintaining a single source of truth
Without this:
- Providers work with incomplete data
- Billing errors increase
- Reporting becomes unreliable
That gap directly affects outcomes.
The right technology stack is not about tools. It’s about building a system where frontend, backend, video, and integrations work as a unified, scalable platform.
Speak With Our Healthcare Engineering Team About Your Telemedicine Platform Goals
V. What Compliance Requirements Must Telemedicine Apps Meet?
What’s the fastest way to lose trust in digital health?
Not a bad UI. Not a slow app.
A compliance failure.
In healthcare, your custom telemedicine app is not just a product. It is part of a regulated system where security, privacy, and auditability are non-negotiable.
And here’s the catch.
Compliance is not something you “add later.”
It must be designed into the architecture from day one.
A. Security Standards
At the core, telemedicine platforms must protect Protected Health Information (PHI) at every layer.
This includes:
- HIPAA compliance (U.S. baseline requirement)
- End-to-end encryption (data in transit and at rest)
- Role-Based Access Control (RBAC) to limit data exposure
But let’s make this real.
What happens if a provider accidentally accesses the wrong patient record?
Without proper access controls and audit trails:
- Violations go unnoticed
- Risk exposure increases
- Legal consequences follow
Healthcare data breaches cost an average of $10.93 million per incident.
IBM Cost of a Data Breach Report
That’s the highest of any industry.
So security is not just about protection. It’s about financial risk mitigation.
Key architectural elements include:
- Secure authentication (OAuth 2.0, MFA)
- Audit logs for every data interaction
- Zero-trust access principles
Security is a product feature, not a backend task.
B. Regulatory Considerations
Compliance goes beyond data security.
Telemedicine introduces clinical, legal, and reimbursement complexities.
Key areas include:
- Provider licensing across states or regions
- Patient consent management for virtual care
- Documentation aligned with billing and reimbursement rules
Here’s a common blind spot.
A platform enables cross-state consultations without requiring validation of licensing requirements.
Result?
- Legal exposure
- Denied reimbursements
- Operational disruption
And then there’s reimbursement.
Telehealth reimbursement policies expanded significantly post-COVID, but variability still exists across payers. – CMS
That means your system must support:
- Accurate coding workflows
- Documentation completeness
- Integration with billing systems
Otherwise, revenue leakage becomes inevitable.
C. Compliance by Design
Can you bolt compliance onto a system after launch?
Technically yes.
Practically? Painful. Expensive. Risky.
High-performing teams take a different approach:
- They build compliance into the system architecture.
This includes:
- Security-first infrastructure design
- Continuous monitoring and threat detection
- Automated compliance checks within workflows
For example:
- Consent capture embedded into intake flows
- Access controls tied to user roles are dynamically
- Alerts for suspicious activity
This reduces:
- Manual compliance overhead
- Human error
- Audit complexity
And increases:
- Trust with providers and patients
- Readiness for audits and certifications
- Speed of scaling into new markets
Compliance, when done right, becomes an enabler, not a blocker.
A custom telemedicine app must treat compliance as a core system requirement, not a checklist. Security, regulation, and architecture must move together.
VI. How Do You Build and Launch a Custom Telemedicine App?
Everyone talks about building telemedicine platforms. Few talk about what actually derails them.
It’s rarely the code.
It’s unclear workflows, poor sequencing, and scaling too late.
Building a custom telemedicine app is not a single project. It’s a phased execution strategy that balances speed, compliance, and long-term scalability.
Let’s walk through how experienced teams approach it.
A. Development Phases
Do you build everything up front or evolve in layers?
The second approach wins. Every time.
1. Discovery: Define the Care Model Before the Code
This is where most failures begin.
Teams jump into development before fully mapping:
- Patient journeys
- Provider workflows
- Integration requirements
Instead, high-performing teams start with:
- Workflow mapping across care stages
- Clinical and operational requirements
- Data flow architecture
If workflows are unclear, development becomes guesswork.
Your architecture should reflect how care is delivered, not just how features are built.
2. MVP: Build for Validation, Not Perfection
The MVP is not a stripped-down product. It’s a focused system that validates core workflows.
Typical MVP scope includes:
- Video consultations
- Scheduling and intake
- Basic provider dashboard
- Initial EHR integration
The goal?
- Validate user adoption
- Identify workflow friction
- Gather real usage data
Not to impress stakeholders with features.
Startups that iterate based on real user feedback are significantly more likely to achieve product-market fit. –Harvard Business Review
This phase sets the foundation for everything that follows.
3. Scaling: From Product to Platform
Once validated, the system expands.
This is where complexity increases:
- Multi-specialty workflows
- RPM integration
- AI-driven features
- Advanced analytics
- And here’s where early decisions matter.
If your MVP was not designed with scalability in mind:
- Refactoring becomes expensive
- Performance issues emerge
- Integration debt compounds
Scaling is not about adding features. It’s about evolving architecture.
B. Timeline and Cost
How long does it take, and what does it actually cost?
The honest answer: it depends on the scope, integrations, and depth of compliance.
But patterns exist.
1. MVP Timelines
- Basic MVP: ~3 to 6 months
- Integration-heavy MVP: ~6 to 9 months
Factors that influence speed:
- Complexity of workflows
- Number of integrations (EHR, billing, RPM)
- Compliance requirements
2. Cost Drivers
Decisions, not just development hours, shape costs.
Key drivers include:
- Feature complexity
- Integration depth
- Infrastructure (cloud, video, storage)
- Security and compliance requirements
A common mistake?
Underestimating integration costs.
Integrations often take more effort than core feature development.
3. Infrastructure Costs
Beyond build costs, ongoing expenses include:
- Cloud hosting (AWS/Azure)
- Video streaming services
- Data storage and processing
- Security monitoring
These scale with usage.
Which is why early architectural choices directly impact long-term margins.
C. Common Mistakes
Where do most telemedicine builds go wrong?
Not in ambition. In execution.
1. Ignoring Integrations Early
Teams focus on UI and core features first.
Integrations come later.
Result?
- Rework
- Delays
- Inconsistent data flows
2. Poor Workflow Design
If workflows are not clearly defined:
- Providers face friction
- Patients drop off
- Operations become manual
Remember:
Telemedicine is workflow-first, not feature-first.
3. Delaying Scalability Planning
Many teams assume they’ll “scale later.”
But without:
- Modular architecture
- Scalable infrastructure
- Clean integration layers
Scaling becomes expensive and slow.
Growth exposes every shortcut taken early.
Building a custom telemedicine app requires disciplined execution across discovery, MVP, and scaling, with architecture decisions made for the future, not just the present.
VII. How Mindbowser Can Help Build Custom Telemedicine Apps
What separates a successful telemedicine build from one that stalls after launch?
Not effort. Not intent.
Execution with the right partner.
A custom telemedicine app requires alignment across clinical workflows, engineering architecture, compliance, and speed to market. That’s where most teams struggle, especially when internal bandwidth is limited or fragmented.
This is where Mindbowser steps in.
Built on the principles outlined in the Mindbowser Blueprint v3.0, the approach is simple: design for real-world care delivery, build for scale, and launch faster without compromising compliance.
A. Strategic Discovery
Before writing a single line of code, do you fully understand your care delivery model?
Mindbowser starts with:
- Deep workflow mapping across patient, provider, and admin journeys
- Identification of integration points (EHR, RPM, billing)
- Architecture planning aligned with long-term scalability
This avoids the most expensive mistake in telemedicine:
- Building features before defining workflows.
Key outcome: A system blueprint that reflects how care actually flows rather than assumptions.
B. Engineering Platforms Built for Healthcare
Telemedicine is not just app development. It’s healthcare system engineering.
Mindbowser builds platforms with:
- Integrated video infrastructure + APIs for stable consultations
- Seamless EHR, billing, and RPM integrations
- Cloud-native architecture designed for growth and compliance
And critically:
- HIPAA and SOC 2 aligned systems by design
- Modular components that evolve without full rework
This reduces both technical debt and time to scale.
The platform is built as an ecosystem, not a collection of features.
C. Accelerating Innovation Without Breaking Systems
How do you introduce AI, analytics, and new care models without destabilizing your platform?
You build for it from day one.
Mindbowser enables:
- AI-driven features like clinical summaries and decision support
- Scalable data pipelines for analytics and reporting
- Continuous iteration without disrupting existing workflows
And here’s where speed matters.
Accelerator-driven development can reduce time-to-market by up to 40%.
That means:
- Faster MVP launches
- Quicker iteration cycles
- Earlier ROI realization
This works. Period.
Mindbowser helps organizations move from idea to scalable telemedicine platform by aligning strategy, engineering, and compliance without slowing innovation.

Building for Scale, Not Just Launch
A custom telemedicine app is not just about enabling virtual visits; it’s about building a foundation for scalable, connected, and outcome-driven care. As organizations grow, the ability to align workflows, integrate systems, and continuously evolve the platform becomes a direct driver of efficiency, patient engagement, and revenue.
The real advantage is not in launching fast, but in scaling without friction. Teams that invest in custom development gain control over their care models, data, and innovation roadmap, turning telemedicine from a feature into a long-term strategic asset. The platforms that win in digital health are those built to adapt, not those constrained by their starting point.
A custom telemedicine app is a purpose-built virtual care platform designed around specific clinical workflows, integrations, and business models. Unlike SaaS tools, it gives full control over features, data, and scalability.
Costs vary based on complexity, integrations, and compliance needs. Most MVPs range from mid-five to six figures, with additional investment required for scaling, infrastructure, and advanced features.
An MVP typically takes 3–6 months, while a fully integrated platform may take 6–12 months. Timelines depend heavily on workflow complexity, EHR integrations, and compliance requirements.
Core features include video consultations, scheduling, patient and provider dashboards, ePrescriptions, and EHR integration. Advanced capabilities like AI documentation, RPM, and analytics drive long-term value.
They embed compliance into architecture through encryption, secure authentication, role-based access control, and audit logs. This ensures patient data protection while meeting regulatory requirements from day one.
































