TL;DR
- Choose a platform if speed, lower upfront effort, and pilot deployment matter most
- Choose build if EHR control, workflow customization, and long-term flexibility matter most
- For most provider organizations, the real decision is ownership of the integration layer
I. Introduction
Healthcare leaders evaluating remote patient monitoring often face one core decision: buy a ready-made RPM platform or build a custom EHR-integrated solution. Platforms help teams launch faster, but custom builds offer greater workflow control, tighter Epic/Cerner integration, and stronger long-term flexibility. This guide compares both options across deployment speed, integration depth, compliance, architecture, and ROI so provider organizations can choose the right path.
What used to be a decision driven by compliance and interoperability is now about creating a system that truly fits their clinical needs and operational goals. In this post, we will break down the pros and cons of each option and provide actionable insights to help you decide which approach aligns best with your hospital’s strategic vision.
II. Why EHR Integration Matters in RPM Strategy
A. The EHR as the Core of Patient Care
The Electronic Health Record (EHR) is the backbone of healthcare delivery. It houses not only patient data but also the entire clinical, financial, and population health workflows. When you integrate a remote patient monitoring system directly with your EHR, you ensure that patient data from wearables and remote devices is seamlessly linked to the clinical workflows that clinicians already rely on. This integration eliminates silos, allowing for real-time data access and actionable insights across care teams.
RPM systems—whether platform-based or custom—deliver more value when they are tightly integrated with EHR workflows and clinical decision-making processes.
For a deeper look at implementation patterns, see our guide to RPM EHR integration with Epic, Cerner, and FHIR.
B. Streamlined Clinical Workflows Through EHR Integration
When RPM data flows directly into EHR workflows, clinicians can act on patient insights without switching systems or relying on external dashboards. This allows clinicians to take action on remote patient data within the same systems they already use, without needing to learn new interfaces or switch between multiple platforms. This seamless integration promotes higher clinician adoption rates and improves the speed and accuracy of decision-making.
III. What a Remote Patient Monitoring Platform Offers — and Where It Stops
A. Key Benefits of RPM Platforms
- Rapid Deployment: A remote patient monitoring platform allows for quick implementation. With prebuilt FHIR connectors and wearable SDKs, you can connect a wide range of devices to your system in just a few months. This is a key advantage for organizations looking to deploy a solution fast.
- Built-in Compliance: One of the major benefits of platforms is that they come with HIPAA and SOC-2 compliance already built in. This ensures that the platform is secure and ready to handle sensitive patient data from day one.
- Minimal IT Burden: Because the platform is managed in the cloud, internal IT teams are relieved from the responsibility of maintaining the infrastructure. This reduces operational complexity, allowing your staff to focus on patient care instead of system management.
B. Limitations of RPM Platforms
- Limited Customization: One of the trade-offs of RPM platforms is the limited customization options. While platforms can integrate with various devices and EHR systems, the ability to tailor workflows and patient alerts to meet the unique needs of your organization is often restricted.
- Data Silos: While platforms offer great device compatibility, patient data often exists outside the EHR, making it challenging to obtain a comprehensive view of the patient’s health. This lack of full integration can hinder clinical decision-making, as clinicians may need to access multiple systems to get the complete patient picture.
- Escalating Vendor Dependency and Costs: As your RPM needs grow, so too do licensing and vendor fees. Over time, this dependency can result in higher costs and reduced flexibility. The platform may also be limited by the vendor’s roadmap and future product offerings, preventing your system from evolving to meet changing needs.
How to Evaluate Remote Patient Monitoring Companies
When comparing remote patient monitoring companies, healthcare leaders should evaluate more than device support and dashboard features. The real differentiators are EHR integration depth, workflow flexibility, alert orchestration, reporting, compliance posture, and the ability to support future care models without heavy vendor dependence.
- EHR and FHIR integration maturity
- Device ecosystem compatibility
- Workflow and alert customization
- Reporting and analytics depth
- Security and compliance readiness
- Pricing model and vendor lock-in risk
IV. When Building Your Own EHR-Integrated RPM Makes Sense
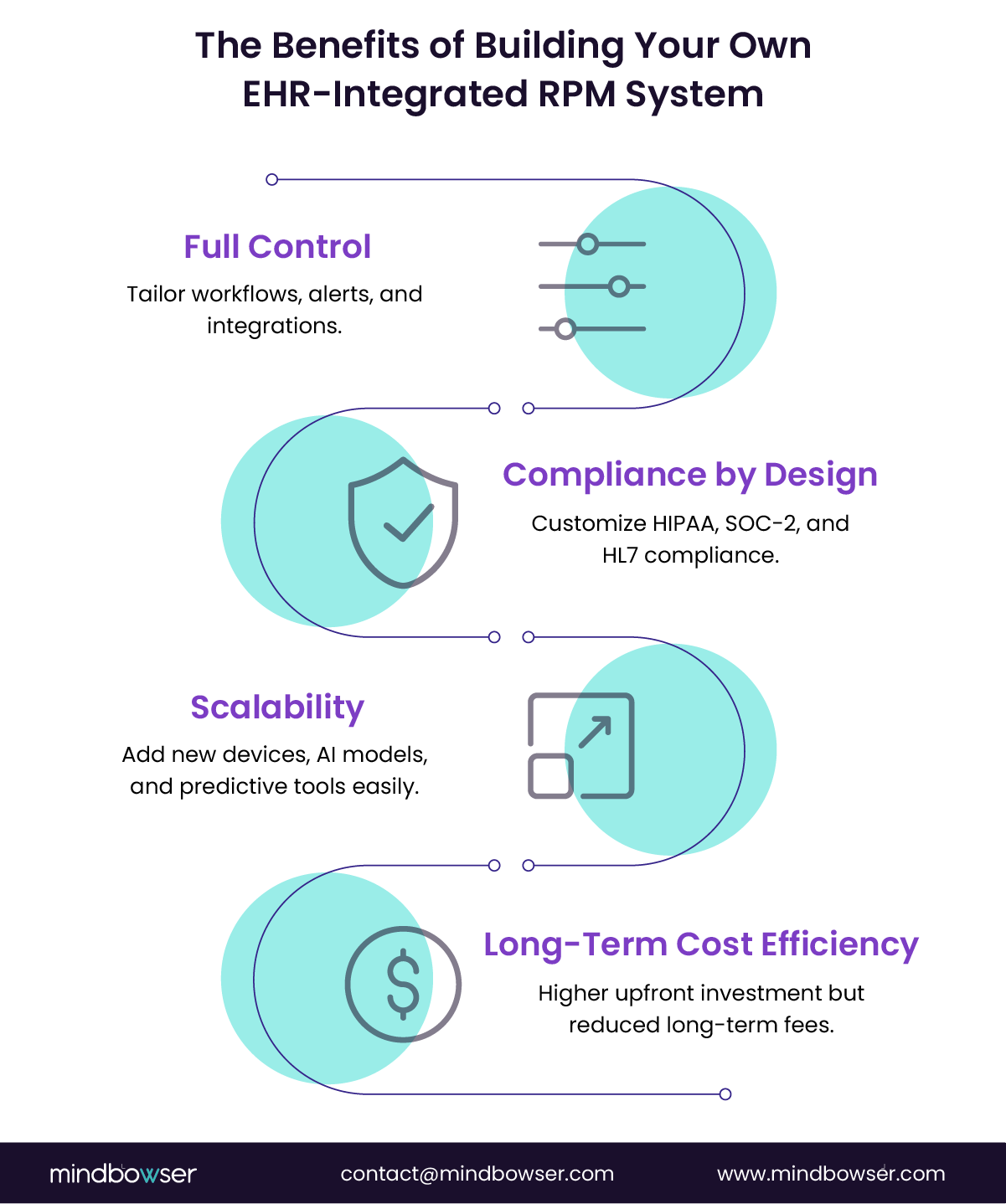
A. Strategic Advantage of Full Control
When you build your own EHR-integrated RPM system, you gain complete control over the data, workflows, and innovation cycle. You can design the system to fit your organization’s specific needs, ensuring that it aligns with your clinical goals and operational objectives. Unlike with a platform, where you are dependent on external vendors, a custom solution provides the flexibility to evolve as your needs change.
Having this level of control means that you can adapt your RPM system to support new devices, workflows, and healthcare models without being limited by the platform’s capabilities. Over time, this customization yields dividends by enhancing patient outcomes, boosting clinician satisfaction, and minimizing operational inefficiencies.
B. Deeper Epic/Cerner Integration
A custom-built RPM system can integrate deeply with your existing Epic EHR or Cerner EHR. By building SMART-on-FHIR apps within Hyperspace, your RPM system can directly feed vital signs and other patient data into the clinician’s workflow. This native integration ensures that the information clinicians need is readily available and can be acted upon quickly, without the need to switch between multiple systems.
- Automating data ingestion: You can automate the intake of vital signs and other key data from remote devices directly into the EHR, saving clinicians time and improving accuracy.
- Alert routing: Alerts and notifications based on real-time data can be routed directly to the relevant care team members, enabling faster decision-making.
C. Clinical and Business ROI
Building your own RPM system offers a long-term cost benefit. While the initial investment may be higher, especially if you are integrating with an existing EHR, the return on investment (ROI) over time is substantial. Custom systems reduce reliance on third-party vendors, resulting in lower ongoing fees and less vendor lock-in.
Moreover, a custom EHR-integrated RPM system enables you to deliver a differentiated care experience that is aligned with your organization’s brand. You can tailor the system to meet the needs of both clinicians and patients, thereby driving engagement and improving health outcomes. This directly impacts your bottom line by reducing costs associated with readmissions and improving patient satisfaction.
D. Compliance and Security by Design
When you build your own RPM system, you have full control over compliance and security. This means you can design the system to meet HIPAA and SOC-2 requirements, as well as implement encryption and access controls tailored to your organization’s specific needs. By embedding compliance features into the system’s design, you ensure that patient data is always secure and that you are prepared for audits or reporting requirements.
Furthermore, building your own system enables you to establish custom audit trails and data access policies, ensuring complete transparency and accountability for all patient data.
E. Scalability by Design
A custom RPM system is scalable from the start. The vendor’s roadmap does not limit you and can be expanded to include new devices, AI models, or other functionalities as needed. Whether you want to integrate new wearables, implement predictive analytics for readmission risk, or roll out new population health management tools, you have the flexibility to grow your system as your needs evolve.
V. What a Scalable RPM Architecture Requires
A. Device ingestion layer
A scalable RPM architecture needs a reliable device ingestion layer to collect data from connected devices, wearables, and third-party health APIs without creating operational bottlenecks. This layer should normalize incoming data, validate device inputs, and route observations into downstream clinical and analytics workflows.
B. EHR and FHIR integration layer
To support clinician adoption, RPM data should flow into Epic, Cerner, or other EHR workflows through structured interoperability layers such as FHIR APIs, mapped observations, and event-based routing. Strong EHR integration reduces data silos and makes remote-monitoring insights more actionable inside existing care workflows.
C. Alerting and workflow orchestration
Alert thresholds, escalation logic, and clinician routing should reflect actual care workflows, not just device triggers. A strong RPM system should support alert prioritization, role-based routing, and follow-up workflows so care teams can respond quickly without increasing alert fatigue.
If alert design is a priority, explore our guide to clinician-first RPM alerts in Epic.
D. Security and DevSecOps
Healthcare RPM systems require secure release processes, audit logging, access controls, encryption, vulnerability testing, and infrastructure monitoring from the beginning. DevSecOps practices help teams release updates without compromising compliance, uptime, or patient-data security.
E. Reusable architecture for future programs
The strongest RPM architectures are designed for reuse across future care programs. Once device ingestion, EHR integration, alerting, and security layers are in place, organizations can extend the same foundation to chronic care, post-discharge monitoring, hospital-at-home, and specialty workflows without rebuilding the platform core.
What Deployment Readiness Looks Like
- Device onboarding is standardized
- EHR mapping is tested
- Alert routing is clinically validated
- Audit logs and access controls are active
- Release, uptime, and monitoring processes are in place
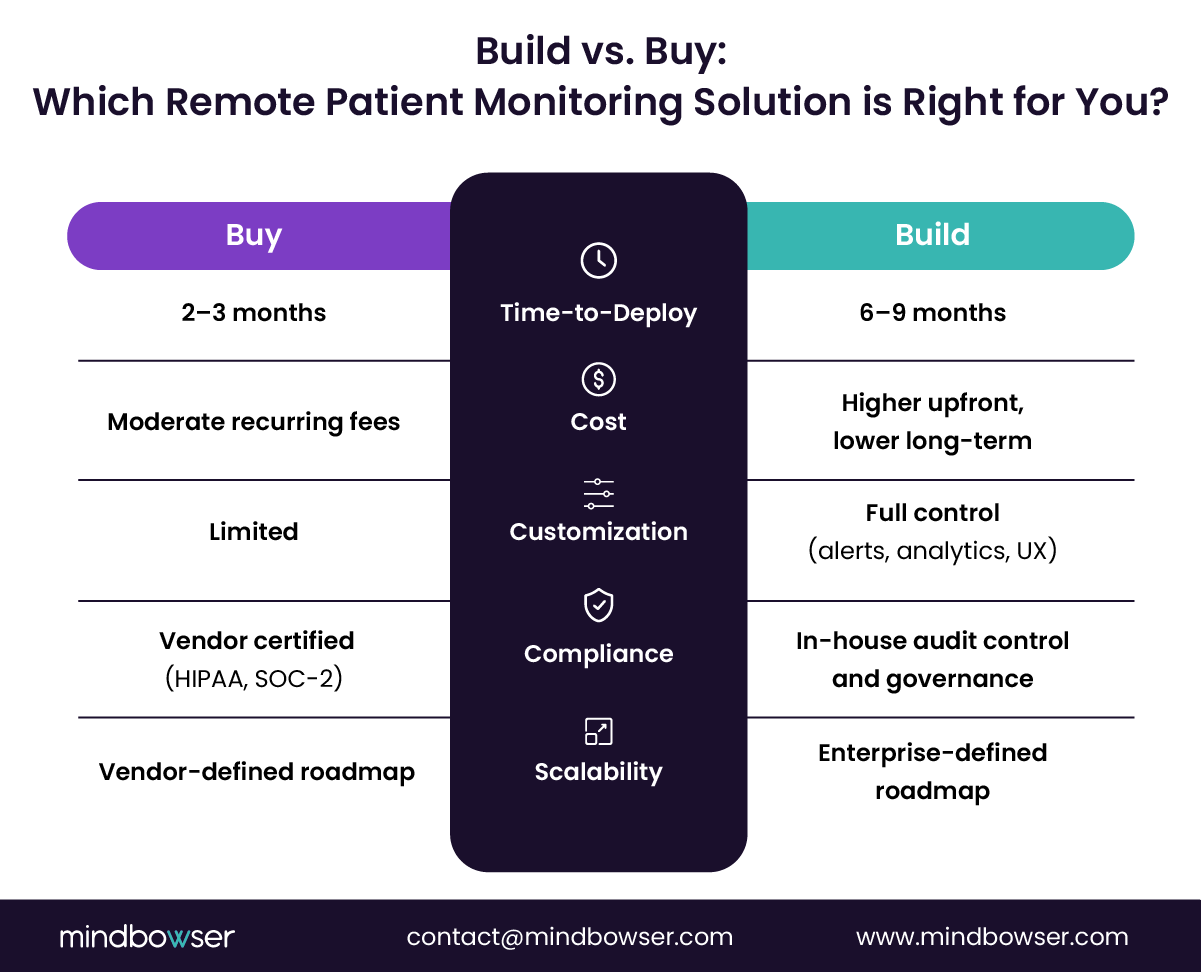
VI. Head-to-Head: Remote Patient Monitoring Platform vs. Build-Your-Own EHR-Integrated RPM
VII. Build Once, Reuse Everywhere: Leveraging FHIR for Scale
A. Future-Proof Your RPM Build
When you build your own EHR-integrated RPM system, you can future-proof your solution by leveraging FHIR APIs. These standardized data exchange protocols allow your system to easily integrate with new devices, AI tools, and health data platforms as they emerge. This scalability ensures that your RPM system remains adaptable and capable of supporting future healthcare innovations.
By using FHIR, your system can expand without major overhauls, enabling you to continually incorporate the latest advancements in patient monitoring and care delivery. As new devices and technology come online, you can seamlessly integrate them into your existing system, maintaining continuity in your workflows.
B. Standardized Data Exchange Supports AI and Population Health Tools
- AI Models for Disease Prediction: A FHIR-integrated RPM system enables seamless integration with predictive analytics tools, such as those that forecast readmission risk or medication adherence. By incorporating real-time patient data from wearable devices and other sources, these AI models can enhance clinical decision-making and improve patient outcomes.
- Integration with Population Health Dashboards: You can utilize FHIR to integrate your RPM system with population health dashboards, offering a unified view of patient health across various care settings. This integration helps healthcare providers track and manage patient populations more effectively, identifying at-risk individuals and implementing timely interventions.
FHIR-based interoperability makes it easier to reuse RPM infrastructure across devices, care settings, and future digital health programs. This is especially useful for provider organizations expanding into chronic care, post-discharge monitoring, and hospital-at-home workflows.
These interoperability advantages become even more valuable when applied to high-priority care models such as hospital-at-home, cardiac follow-up, and chronic disease management.
VIII. Key Use Cases for EHR-Integrated Remote Patient Monitoring
A. Hospital-at-Home Programs
Some hospitals now use RPM to safely discharge patients earlier. Vitals and symptoms are tracked at home using wearable sensors. Automated alerts help clinical teams step in if signs worsen, reducing readmission rates and freeing up hospital beds.
B. Post-Discharge Cardiac Monitoring
After heart surgery or a cardiac event, remote monitoring tracks blood pressure, heart rate, and medication adherence. For post-discharge cardiac monitoring, RPM can help care teams detect deterioration earlier and intervene faster when workflows are connected to the EHR.
C. Chronic Disease Management
Remote patient monitoring is also effective for ongoing management of chronic conditions such as diabetes, hypertension, and COPD. Instead of relying only on episodic visits, providers can monitor trends over time and intervene before the patient deteriorates. This improves continuity of care and supports more proactive population health management.
IX. Compliance and Security Considerations for Platform vs Build
Both RPM platforms and custom-built RPM systems can support compliance when security, auditability, and governance are designed properly. Platforms simplify initial setup, while custom builds offer more control over encryption, access policies, audit trails, and integration-specific security rules.
A. Embedded Compliance
One of the primary concerns when adopting a remote patient monitoring system is ensuring that patient data is handled in a compliant and secure manner. With a remote patient monitoring platform, compliance is often built into the vendor’s platform. However, when you build your own RPM system, you retain full control over compliance features. This allows you to tailor your system to meet HIPAA, SOC-2, and other regulatory requirements from the outset.
By building compliance into the architecture of your EHR-integrated RPM system, you eliminate the risk of compliance gaps that may arise later in the process. This proactive approach ensures your system is ready for audits and reporting requirements, reducing the risk of data breaches or regulatory penalties.
B. Customizable Encryption and Access Controls
When you control the architecture of your RPM system, you have the flexibility to implement customized encryption, PHI anonymization, and data access controls. These customizable features are crucial for meeting stringent security requirements and maintaining patient trust. In addition, you can design your system’s access control protocols to ensure that only authorized users can view sensitive patient data, providing a higher level of security than many third-party platforms offer.
Custom audit trails and data access logging also become part of your compliance design. These features allow you to track who accesses patient data, when it is accessed, and for what purpose, ensuring full transparency and accountability.
C. Reducing Build Time with Mindbowser Accelerators
Building a custom EHR-integrated RPM system from scratch can be a time-consuming process. However, Mindbowser offers accelerators like WearConnect and AI Medical Summary that reduce the time and effort needed to get your system up and running. These pre-built solutions help accelerate the integration process while ensuring compliance with established standards. By using these tools, healthcare organizations can significantly shorten the development timeline while maintaining high levels of compliance and security.
Need to Connect RPM Data, Alerts, and Clinician Workflows Inside Epic or Cerner?
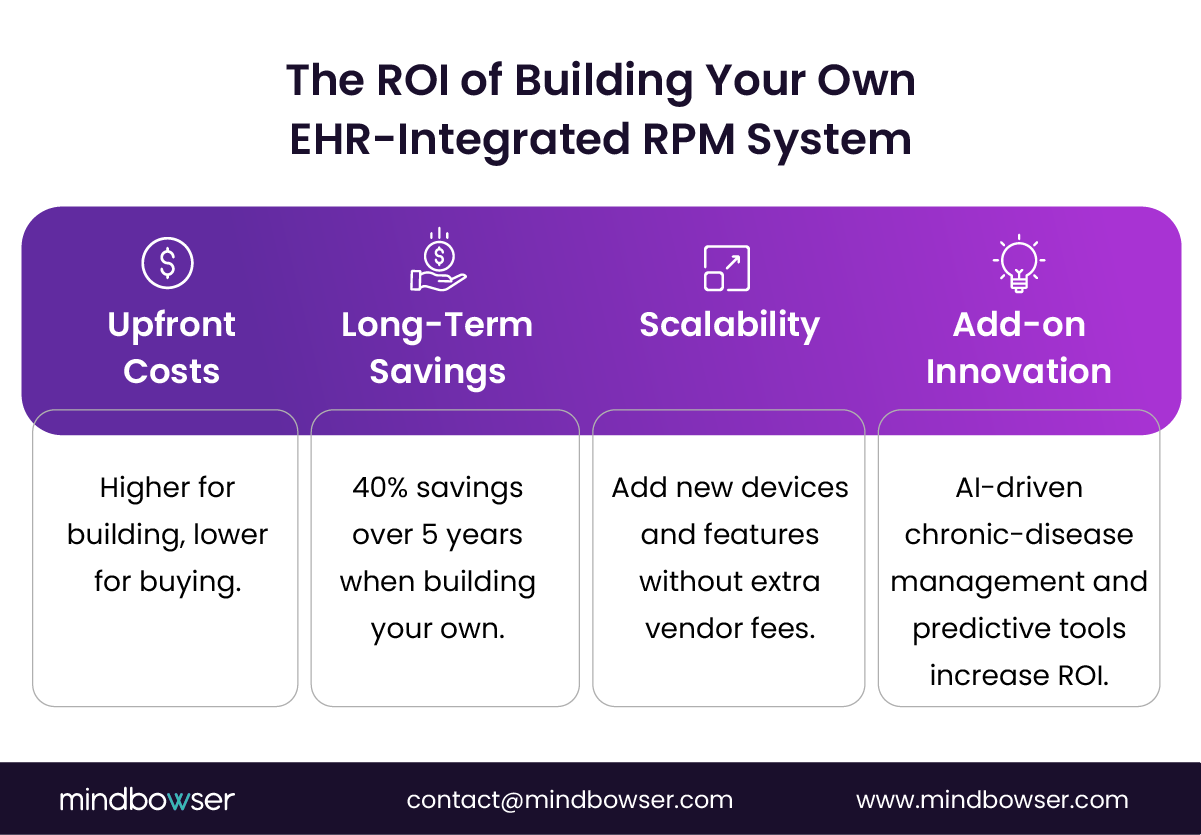
X. ROI Framework: When Platform Wins vs When Build Wins
The ROI decision depends less on software category alone and more on program scale, workflow complexity, EHR integration depth, and long-term operating model.
A. When the Platform has the ROI Advantage
Platforms usually make more sense when speed matters most, internal engineering capacity is limited, or RPM is still being tested as a pilot.
B. When the Build has the ROI Advantage
Custom RPM systems make more sense when organizations need deep workflow customization, tighter EHR integration, reusable architecture, and lower long-term vendor dependency.
C. What Actually Drives the ROI Decision
The real ROI decision depends on program scale, number of devices, degree of workflow complexity, integration requirements, and long-term expansion plans.
XI. Decision Framework — Which Path Fits Your Organization
| Choose a platform if… | Choose build if… |
|---|---|
| You need fast launch | You need deep Epic/Cerner integration |
| IT capacity is limited | You need custom alerts and workflows |
| RPM is still a pilot | RPM is strategic and long-term |
| Standard workflows are enough | Differentiated care delivery matters |
A. Choose a Remote Patient Monitoring Platform if:
- Rapid deployment matters: Platforms help teams launch faster across clinics or service lines.
- Internal IT capacity is limited: They reduce the engineering burden with prebuilt infrastructure and integrations.
- RPM is still a pilot: A platform is often the lower-risk option for early-stage programs.
B. Choose to Build Your Own EHR-Integrated RPM if:
- You need deep Epic or Cerner integration: Custom builds support tighter workflow and data alignment.
- Long-term flexibility matters: You control the roadmap, integrations, and future expansion.
- Differentiated workflows are important: Custom architecture fits unique care models, alerts, and clinician processes.
XII. How Mindbowser Can Help?
Mindbowser helps provider organizations evaluate, design, and implement RPM solutions across both paths: selecting the right platform for faster rollout or building custom EHR-integrated RPM systems for long-term control and scalability.
Our accelerators, such as WearConnect and AI Medical Summary, enable faster deployment while ensuring that compliance and security are built in from the start. Whether you are building a custom RPM system or looking to enhance an existing solution, Mindbowser offers the tools and expertise to help you scale and innovate while reducing the complexity of integration.
With Mindbowser, you gain access to a dedicated team that will work alongside your organization to design and implement a tailored solution, ensuring that your EHR-integrated RPM system not only meets your current needs but is also scalable for future growth. We prioritize long-term success by providing ongoing support and innovation, making sure your system adapts to new challenges and opportunities in healthcare.
- RPM architecture planning
- Epic, Cerner, and FHIR integration
- compliance-first engineering
- custom alert and workflow design
- accelerators to reduce build time

Conclusion
There is no universal winner in the RPM platform vs build decision. Platforms are better for speed and lower short-term effort. Custom builds are better for organizations that need workflow control, deeper EHR integration, and reusable digital-health infrastructure. The right choice depends on your clinical model, internal IT capacity, and long-term RPM strategy.
An RPM platform is vendor-managed and faster to launch, while a custom build offers more control over workflows, integration, and long-term extensibility.
Build makes more sense when RPM is strategic, EHR integration is critical, and care workflows need customization.
Platforms may offer faster setup, but custom builds usually allow deeper workflow and data integration.
Not necessarily. A custom RPM system can be compliant if security, audit controls, and governance are designed into the architecture.
Common issues include vendor lock-in, rising license fees, limited workflow flexibility, and added integration effort over time.
Yes. A reusable FHIR-based architecture can support expansion across chronic care, post-discharge, hospital-at-home, and specialty care models.