TL;DR
Clinical decision support systems improve patient care by helping clinicians make safer, faster decisions at critical moments. By analyzing real-time patient data within clinical workflows, CDSS reduces medication errors, identifies early signs of deterioration, and reinforces evidence-based treatment decisions. For hospitals operating under value-based care models, CDSS plays a direct role in improving patient safety, consistency of care, and clinical outcomes.
“How can clinicians make the safest decision when they must evaluate complex patient data in seconds?”
In modern healthcare environments, clinical decisions must be made quickly while balancing patient history, medications, lab results, and evolving treatment guidelines. Even experienced clinicians face challenges in identifying risks in real time.
Clinical decision support systems improve patient care by delivering timely, data-driven insights directly within clinical workflows. Instead of relying on memory or manual checks, clinicians receive guidance at the exact moment decisions are made reducing risk and improving care quality.
Watch Now: How Clinical Decision Support Systems Drive Better Clinical Outcomes
I. Why Clinical Decision Support Systems Improve Patient Care Today
Healthcare clinicians now operate in an environment where clinical data volumes, guideline libraries, and quality reporting expectations continue to expand. Physicians must evaluate medications, comorbidities, and diagnostic signals within seconds while maintaining patient safety and adherence to guidelines.
A clinical decision support system helps manage this complexity by delivering context-aware recommendations directly within clinical workflows. Rather than relying on memory or static reference tools, clinicians receive timely guidance using real-time patient data.
For hospital leaders responsible for quality, safety, and value-based care outcomes, the clinical decision support system has become a strategic capability embedded within the EHR ecosystem.
A. What Is a Clinical Decision Support System?
A clinical decision support system (CDSS) is a technology layer within clinical workflows that analyzes patient-specific data and delivers real-time recommendations to clinicians.
Instead of acting as a static reference tool, CDSS supports decision-making directly at the point of care, helping clinicians identify risks and make evidence-aligned decisions at critical moments in care.
To understand how CDSS works at a foundational level, explore what a clinical decision support system is.
B. Why Clinical Decision Support Systems Matter Now
Healthcare delivery has grown more complex over the past decade.
Clinicians must now navigate:
- expanding clinical guideline libraries
- rapidly evolving treatment standards
- patients with multiple chronic conditions
- increasing documentation and quality reporting requirements
This complexity creates a persistent risk: unwarranted variation in clinical decisions.
Two physicians treating the same patient for the same condition may follow different protocols simply because clinical guidance is difficult to access in real time.
A well-designed clinical decision support system reduces this variation by embedding guideline-aligned recommendations directly within the care workflow.
Hospitals are also facing new financial pressure from value-based reimbursement models. Performance metrics tied to safety, readmissions, and preventive care now affect hospital revenue and public quality reporting.
A clinical decision support system helps health systems respond to these pressures by:
- improving adherence to evidence-based protocols
- identifying medication safety risks earlier
- Closing preventive care gaps
- detecting patient deterioration sooner
For CIOs and CMIOs, the clinical decision support system is not simply a technology feature inside the EHR. It is an operational tool that helps translate clinical guidelines into consistent practice across the organization.
C. What Is Evidence-Based Clinical Decision Support?
Not all decision support improves care. The effectiveness of a clinical decision support system depends on the quality and transparency of its clinical logic.
Evidence-based clinical decision support links every recommendation to validated clinical research, consensus guidelines, or regulatory standards. Each alert, rule, or risk score should trace back to clearly documented evidence.
Hospitals must also maintain rigorous governance around decision support content.
Key governance responsibilities include:
- clinical committee review of decision rules
- version control for guideline updates
- approval workflows for new alerts or order sets
- monitoring alert overrides and clinical outcomes
These controls ensure the clinical decision support system remains accurate, clinically relevant, and trusted by frontline providers.
Without governance, decision support can drift away from current clinical evidence. With strong oversight, it becomes a continuously improving safety mechanism embedded across care delivery.
A clinical decision support system succeeds when it combines clinical evidence, workflow integration, and disciplined governance to guide decisions where they matter most, at the bedside.
II. How Does a Clinical Decision Support System Work?
Clinical leaders evaluating a clinical decision support system often ask a practical question first: how does it actually work inside clinical workflows?
At its core, a clinical decision support platform functions as a real-time analytic layer within the EHR environment. It continuously evaluates patient data, applies clinical logic based on guidelines or predictive models, and delivers recommendations directly to clinicians during care delivery.
The goal is simple: deliver the right clinical insight at the exact moment a decision must be made.
A. The Operating Model of a Clinical Decision Support System
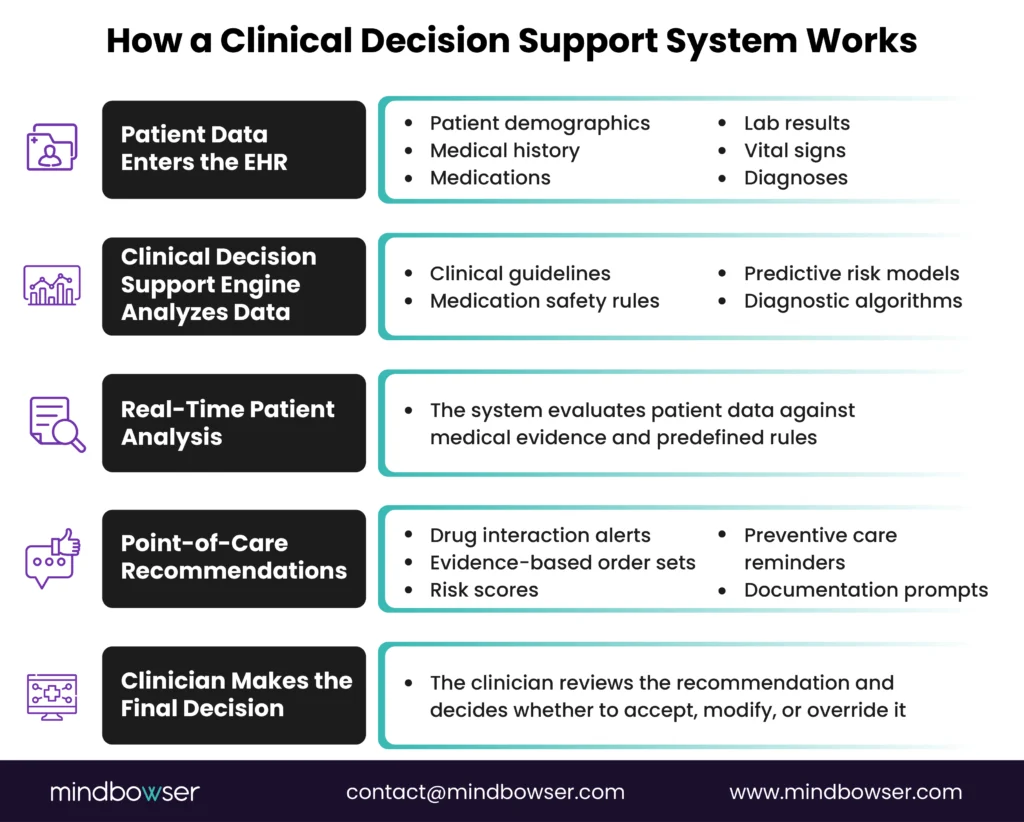
A modern clinical decision support system operates through three core layers: clinical data inputs, decision logic, and clinical outputs.
Each layer contributes to transforming raw patient data into actionable guidance.
- Clinical Data Inputs
The first layer involves collecting patient data already stored within the electronic health record.
Common data sources include:
- Patient demographics
- Diagnoses and problem lists
- Medication histories
- Laboratory results
- Allergies
- Vital signs
- Imaging results
The clinical decision support system continuously monitors these data streams. When relevant patterns appear, the system triggers evaluation rules.
For example, a patient admitted with heart failure who receives a medication that worsens fluid retention may trigger a medication safety alert.
- Decision Logic
The second layer applies clinical logic that determines when recommendations should appear.
Decision logic may include:
- Guideline-based rules
- Risk scoring algorithms
- Predictive Models
- Medication safety knowledge bases
For example:
- If a patient has a documented penicillin allergy and an antibiotic related to penicillin is ordered, the system generates an alert.
- If vital signs and lab patterns indicate early sepsis risk, the system may trigger a deterioration alert.
More advanced environments use predictive modeling to analyze thousands of historical patient records and identify patterns associated with complications.
The clinical decision support system then evaluates whether to present a recommendation against predefined thresholds.
- Clinical Outputs
The final layer involves presenting actionable guidance to clinicians.
Outputs typically include:
- Medication interaction alerts
- Preventive screening reminders
- Evidence-based order set suggestions
- Documentation prompts
- Patient risk scores
The key principle is relevance. The clinical decision support system must provide guidance that directly supports the clinician’s current task.
Alerts that appear outside the clinical context often create alert fatigue and are quickly ignored.
Key Components of a Clinical Decision Support System
| Component | Description |
| Clinical Data Inputs | Patient data from EHR, labs, medications, problems, and vital signs |
| Decision Logic | Clinical rules, guidelines, and predictive models |
| Clinical Outputs | Alerts, reminders, order sets, documentation prompts, and risk scores |
| Workflow Integration | Delivery within clinician workflows inside EHR systems |
B. What Is Point of Care Decision Support?
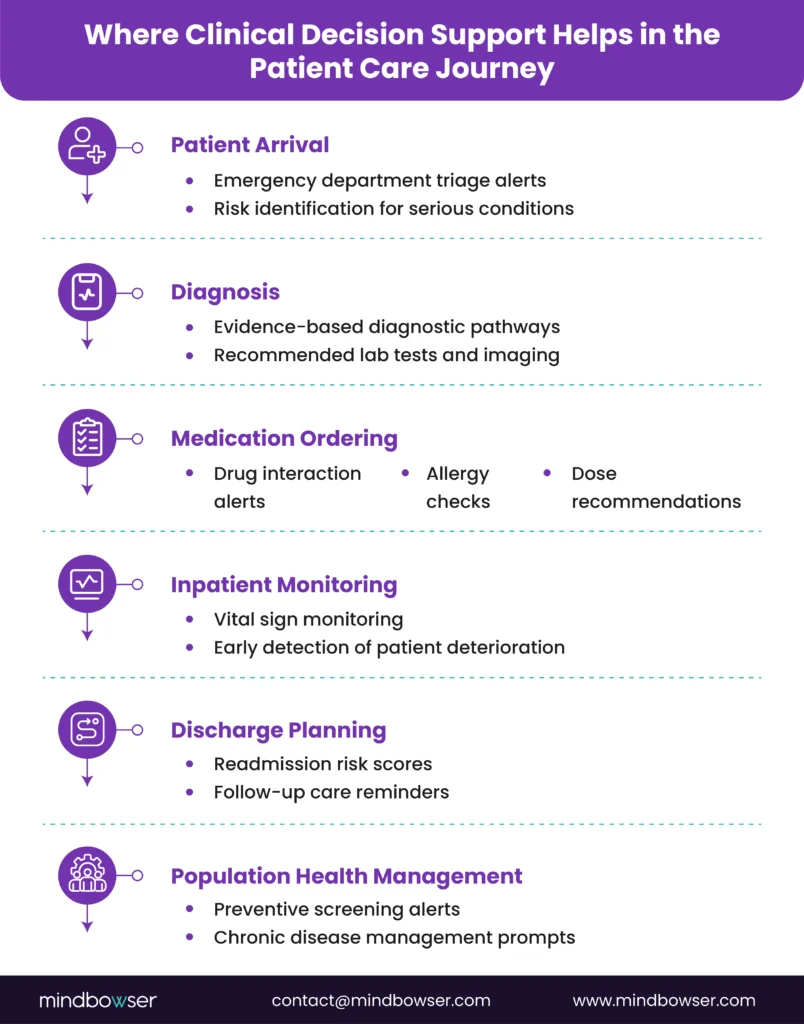
The most effective CDS implementations focus on point-of-care decision support, meaning clinical guidance appears exactly when clinicians are making decisions.
In practice, this follows a simple principle:
Right information, right person, right time.
A clinical decision support system achieves this by embedding recommendations directly inside the EHR interface clinicians already use.
Examples include:
- Medication alerts appearing during order entry
- Preventive screening reminders during outpatient visits
- Deterioration warnings during inpatient monitoring
- Discharge planning prompts during care transitions
Point-of-care decision support can be delivered through two primary formats.
1. Interruptive Decision Support
Interruptive alerts require the clinician to acknowledge the message before continuing.
These alerts are typically reserved for high-risk scenarios such as:
- Severe drug interactions
- Allergy conflicts
- Dangerous dosing levels
Because these alerts interrupt workflow, they must be carefully governed.
2. Non-Interruptive Decision Support
Non-interruptive CDS presents guidance without stopping the clinician’s workflow.
Examples include:
- Recommended order sets displayed during diagnosis entry
- Documentation prompts
- Clinical dashboards showing risk scores
This approach allows the clinical decision support system to guide decisions while minimizing alert fatigue.
C. Integration, Governance, and Safety Controls
Even well-designed CDS rules require continuous oversight.
Hospitals, therefore, implement governance frameworks to monitor how the clinical decision support system behaves in production environments.
Key governance practices include:
1. Workflow Integration
The CDS engine must be tightly integrated into EHR workflows.
If clinicians must leave the EHR to access decision support, adoption drops quickly.
Effective systems embed guidance directly inside:
- Medication ordering workflows
- Diagnostic evaluation screens
- Discharge planning tools
- Care management dashboards
2. Clinical Oversight Committees
Most hospitals establish multidisciplinary committees to manage the clinical decision support system.
Participants often include:
- CMIOs and physician informaticists
- Pharmacy leadership
- Nursing leadership
- Patient safety teams
- Health IT specialists
These groups evaluate new CDS rules, prioritize safety interventions, and ensure alignment with clinical guidelines.
3. Monitoring Overrides and Alert Fatigue
Alert fatigue remains a common challenge in CDSS environments.
Hospitals must monitor:
- Alert acceptance rates
- Override patterns
- Clinician feedback
- Clinical outcomes linked to alerts
Rules that clinicians consistently override may require redesign or removal.
4. Performance Drift Detection
Clinical guidelines evolve, and predictive models can degrade over time.
Health systems must regularly validate CDS rules to ensure they remain clinically accurate.
Continuous monitoring allows the clinical decision support system to remain aligned with current evidence and clinical practice patterns.
A clinical decision support system works when clinical data, decision logic, and workflow integration operate together under strong governance.
When implemented correctly, CDS becomes a quiet partner in clinical decision-making, supporting clinicians without slowing them down.
Schedule a consultation to explore CDSS solutions for your healthcare platform.
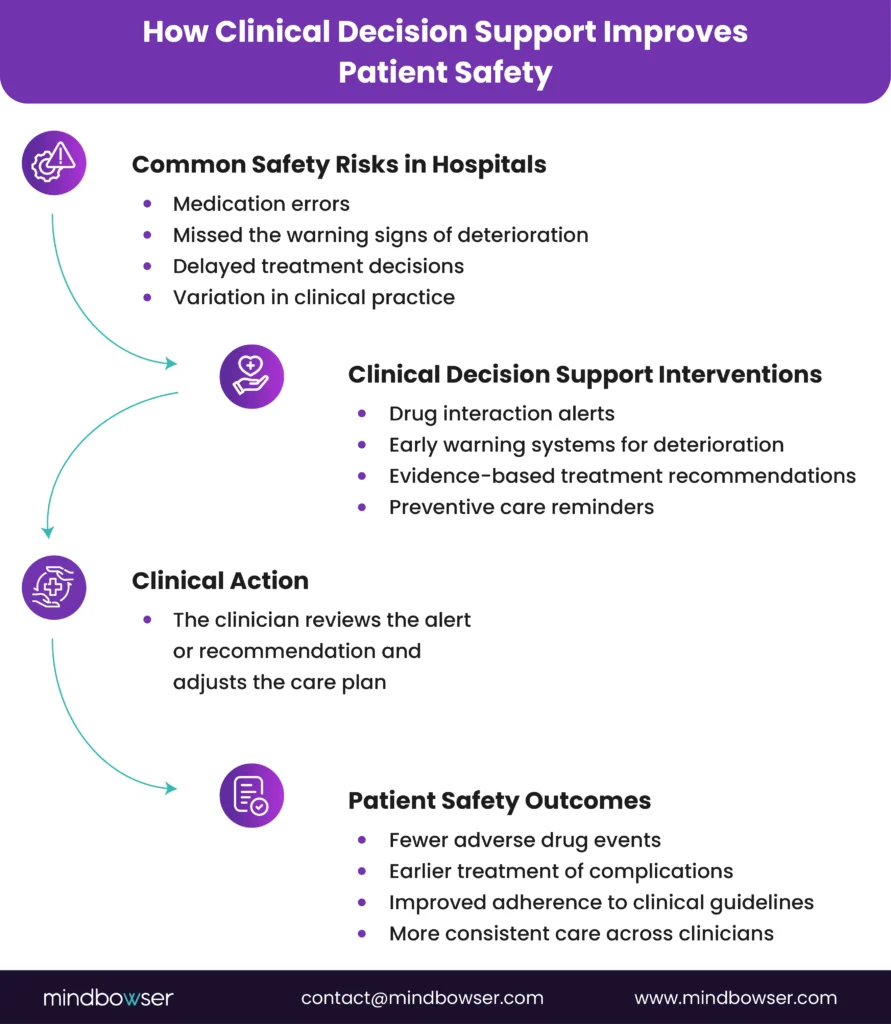
III. How Does CDSS Improve Patient Safety and Patient Care?
Hospitals adopt a clinical decision support system for one reason above all others: measurable improvement in patient safety and care quality.
A well-governed clinical decision support system does not simply display information. It analyzes patient data in real time and guides clinicians toward safer decisions at critical moments.
In practice, this means fewer medication errors, earlier recognition of clinical deterioration, stronger adherence to evidence-based guidelines, and more consistent care delivery across the organization.
These improvements are most visible in several core areas of patient care.
A. Medication Safety
Medication errors remain one of the most common causes of preventable harm in hospitals.
One of the most direct ways CDSS improves patient care is through medication safety by automatically reviewing prescriptions against allergy lists, drug interaction databases, renal dosing guidelines, and patient-specific risk factors.
This analysis occurs during medication ordering, allowing clinicians to correct potential issues before drugs are administered.
Scenario: Preventing a High-Risk Drug Interaction
Consider a cardiology clinic visit.
A patient with atrial fibrillation requires anticoagulation therapy. The cardiologist prescribes a new medication during the consultation.
What the clinician may not immediately notice is that the patient already takes another medication metabolized through the same liver enzyme pathway. When combined, the drugs significantly increase bleeding risk.
As the prescription is entered, the clinical decision support system analyzes the full medication list and identifies the interaction.
An alert appears explaining the risk and suggesting safer alternatives.
The physician reviews the recommendation and adjusts the prescription before it reaches the pharmacy.
One small intervention prevents a potentially life-threatening complication.
This type of medication safety alert is one of the most widely deployed clinical decision support examples in hospital systems.
B. Diagnostic Accuracy
Diagnostic uncertainty is another area where decision support can improve patient care.
A clinical decision support system analyzes patterns across symptoms, laboratory results, and vital signs to identify patients at risk for specific conditions.
These systems do not replace physician judgment. Instead, they highlight risks that might otherwise be overlooked during busy clinical workflows.
Scenario: Recognizing Sepsis Earlier
A patient arrives in the emergency department with fatigue, mild fever, and slightly elevated heart rate.
Individually, none of these symptoms appears alarming.
However, the clinical decision support system evaluates the patient’s lab results, inflammatory markers, and vital signs together. The pattern suggests possible early sepsis.
The system generates a risk score and alerts the care team.
The physician orders blood cultures and antibiotics sooner than they might have otherwise.
For patients with sepsis, hours can determine survival. Early treatment significantly improves outcomes.
This is one of the most impactful clinical decision support examples, in which predictive analytics enables faster diagnosis.
C. Closing Preventive Care Gaps
Hospitals and health systems also use CDSS to improve preventive care and chronic disease management.
In high-volume outpatient environments, clinicians may not always remember every screening guideline or preventive care recommendation.
A clinical decision support system identifies care gaps and reminds clinicians when preventive services are due.
These reminders help improve adherence to quality metrics tied to value-based care programs.
Examples include:
- Cancer screening reminders
- Diabetes management alerts
- Vaccination prompts
- Chronic disease monitoring alerts
These interventions support evidence-based clinical decision support, ensuring guideline-based care is delivered consistently across patient populations.
D. Reducing Unwarranted Variation in Care
Variation in clinical practice is a persistent challenge for hospitals.
Two clinicians may treat the same condition using different protocols simply because guidelines are difficult to access during busy workflows.
A clinical decision support system addresses this challenge by embedding guideline-based recommendations directly inside the EHR.
Scenario: Guideline-Based Order Sets in Action
A patient with community-acquired pneumonia is admitted through the emergency department.
The attending physician begins entering admission orders.
At this moment, the clinical decision support system presents an evidence-based pneumonia order set aligned with national treatment guidelines.
The order set includes:
- Recommended antibiotics
- Appropriate laboratory tests
- Imaging studies
- Oxygen monitoring protocols
The physician can accept the order set with minor adjustments.
Instead of searching for guidelines, the clinician receives immediate support inside the workflow.
These types of embedded recommendations help hospitals improve consistency of care while supporting quality metrics tied to reimbursement programs.
Types of Clinical Decision Support Interventions
| Type of CDS | Example |
| Medication Safety | Drug interaction alerts and allergy checks |
| Diagnostic Support | Risk stratification tools and deterioration alerts |
| Care Gap Alerts | Preventive screening reminders |
| Guideline Adherence | Evidence-based order sets |
| Operational Support | Readmission risk scoring and discharge planning prompts |
Measurable Patient Outcomes: What the Data Shows
- Perinatal risk: Closing the gap on missed signals:
In obstetric care, missed laboratory abnormalities during labor and delivery represent a significant source of preventable harm. When a clinical decision support system was integrated into a perinatal EHR environment, predictive models trained on maternal health records and real-time vital data surfaced risk signals that standard monitoring often missed. The result was a measurable improvement in the detection of at-risk pregnancies before complications escalated. - Sepsis: Hours determine survival:
Sepsis remains one of the leading causes of in-hospital mortality, and delayed recognition is its primary driver. Clinical decision support systems that analyze combinations of vital signs, lactate levels, white blood cell counts, and documentation patterns have demonstrated the ability to generate sepsis risk scores hours before clinical deterioration becomes visible to the care team. Each hour of delay in sepsis treatment increases mortality risk — a CDSS that surfaces an early warning at the point of care translates directly into faster antibiotic administration, earlier cultures, and improved survival rates. - Medication safety: Reducing adverse drug events at the source:
In high-volume environments, a clinical decision support system that flags renal dosing errors, drug-allergy conflicts, and dangerous interaction combinations during order entry prevents harm before it reaches the patient. In specialized perioperative settings, CDSS implementations have shown improvement rates exceeding 90% in reducing missed lab abnormalities that would otherwise affect surgical planning.
The Broader Impact on Patient Care
Across these interventions, the clinical decision support system improves patient care in several measurable ways:
- Fewer adverse drug events
- Earlier detection of clinical deterioration
- Improved adherence to treatment guidelines
- Reduced variability in clinical practice
- Stronger performance on quality metrics
When implemented with strong governance and workflow integration, the clinical decision support system becomes a safety layer within everyday clinical operations.
It quietly supports clinicians in the background, helping them make safer decisions without slowing care delivery.
The greatest impact of a clinical decision support system occurs not through more alerts, but through timely, evidence-aligned guidance delivered at the point of care.
For a detailed breakdown of ROI, cost savings, and operational impact, see benefits of clinical decision support systems
IV. Designing a Clinical Decision Support System That Clinicians Actually Use
Many hospitals deploy clinical decision support systems with the right intentions, yet struggle with clinician adoption. Alerts are ignored, recommendations are bypassed, and clinicians perceive the system as disruptive rather than helpful.
The difference between a successful and ineffective clinical decision support system rarely lies in the technology itself. Instead, it depends on thoughtful design, governance, and continuous monitoring.
For CIOs and CMIOs, the challenge is clear: build a clinical decision support system that clinicians trust and actually use during care delivery.
A. Prioritizing High-Impact Clinical Use Cases
Hospitals often begin CDSS initiatives by implementing a wide range of alerts simultaneously.
This approach frequently backfires.
Instead, successful programs start by identifying high-impact clinical decisions where decision support can improve patient safety.
Typical starting points include:
- Medication interaction alerts
- Sepsis detection alerts
- Renal dosing recommendations
- Preventive care reminders
- High-risk discharge planning
Scenario: Starting with the Highest Risk Decision
A hospital initially deploys dozens of alerts across its EHR system.
Clinicians quickly become overwhelmed and begin overriding most notifications.
The clinical informatics team reviews safety data and identifies that medication dosing errors in renal failure patients represent a major source of adverse drug events.
They redesigned the clinical decision support system to prioritize renal dosing alerts during medication ordering.
Within months, clinicians begin accepting these alerts more frequently because they appear at the exact moment they are needed.
Adoption improves.
Patient safety improves.
The lesson is simple: prioritize decisions with the highest clinical risk.
B. Reducing Alert Fatigue
Alert fatigue remains one of the most common barriers to effective CDS adoption.
If clinicians receive too many alerts, they quickly learn to ignore them. Research has shown that many hospitals have alert override rates exceeding 80 percent for certain alert categories.
A well-designed clinical decision support system minimizes unnecessary interruptions while preserving alerts that protect patient safety.
Effective strategies include:
- Limiting interruptive alerts to high-severity risks
- Using non-interruptive guidance for lower-risk recommendations
- Continuously monitoring override patterns
- Involving clinicians in alert design and refinement
Scenario: When Too Many Alerts Become Dangerous
A physician begins a busy morning clinic session.
Within the first ten patient visits, the EHR generates multiple alerts:
- A mild drug interaction warning
- Duplicate therapy alerts
- Documentation reminders
- Preventive screening notifications
After encountering dozens of alerts, the physician becomes conditioned to dismiss them quickly.
Later in the day, a high-severity drug interaction alert appears. Out of habit, the physician dismisses it without reviewing the warning.
The problem was not the important alert.
The problem was the volume of unnecessary alerts preceding it.
This is why many hospitals now redesign their clinical decision support systems to deliver fewer but more meaningful alerts.
C. Continuous Monitoring and Governance
A clinical decision support system should never be treated as a static tool.
Clinical guidelines evolve. Medication databases change. Predictive models may drift as patient populations shift.
Without active oversight, CDS rules can become outdated or clinically irrelevant.
Health systems, therefore, establish governance structures responsible for maintaining the safety and relevance of their clinical decision support systems.
Governance programs typically include:
- Multidisciplinary CDS review committees
- Physician informaticists responsible for rule validation
- Monitoring of alert acceptance and override patterns
- Regular updates aligned with new clinical guidelines
Scenario: Detecting Performance Drift
A hospital deploys a predictive alert that identifies patients at risk of sepsis.
During the first year, the alert performs well and improves early detection.
Two years later, however, clinicians began reporting that the alert triggers were too frequent.
A CDS governance team reviews performance data and discovers that changes in documentation practices altered the model’s inputs, causing the alert to generate more false positives.
The model is recalibrated, and performance improves.
Without ongoing monitoring, the clinical decision support system could have gradually lost clinician trust.
Why Governance Determines CDSS Success
Technology alone does not improve care.
The hospitals that achieve measurable safety improvements treat their clinical decision support system as a living clinical program rather than a one-time IT project.
Success depends on three principles:
- Clinical relevance
- Workflow integration
- Continuous oversight
When these elements work together, the clinical decision support system becomes a trusted safety partner rather than an obstacle to care.
Ready to improve patient outcomes? Learn how a Custom Clinical Decision Support System can support smarter clinical decisions.
V. How Mindbowser Helps Implement Clinical Decision Support Systems
For many hospitals, implementing a clinical decision support system is not primarily a technology challenge. It is an integration, governance, and workflow design challenge.
Health systems must align EHR data pipelines, clinical rules, governance processes, and user workflows before decision support can deliver measurable safety improvements.
Mindbowser works with hospitals and digital health organizations to design and implement a clinical decision support system that integrates directly into existing clinical environments while supporting long-term clinical governance.
The goal is simple: deliver evidence-based decision support that improves patient safety without disrupting clinician workflows.
A. Custom Clinical Decision Support System Development
Every hospital environment is different.
Patient populations vary, clinical protocols evolve, and EHR configurations differ across health systems. As a result, many organizations require a clinical decision support system tailored to their specific workflows and quality improvement priorities.
Mindbowser designs custom CDS architectures that align with each organization’s clinical operations.
Key capabilities include:
- Integration with EHR platforms and clinical data sources
- Rule-based and predictive decision support models
- Medication safety alert frameworks
- Risk stratification and early warning systems
- Population health and preventive care alerts
This approach ensures the clinical decision support system supports real clinical decisions rather than forcing clinicians to adapt to rigid software logic.
B. Advanced CDS and Predictive Clinical Intelligence
Modern CDSS implementations increasingly incorporate predictive analytics to detect risk earlier in the care process.
Mindbowser supports advanced clinical decision support system capabilities such as:
- Predictive risk scoring models
- Early deterioration detection
- Readmission risk prediction
- Treatment pathway guidance
These models evaluate historical patient data alongside real-time clinical signals to generate earlier warnings and more precise clinical guidance.
For example, Mindbowser improved predictive accuracy for childbirth outcomes by integrating advanced EHR data signals into clinical decision models.
By combining maternal health records, historical clinical patterns, and real-time patient data, the system enabled clinicians to identify potential risks earlier in the labor and delivery process. These insights supported more informed clinical decisions during critical moments of care.
These predictive capabilities extend the value of the clinical decision support system beyond alerts, enabling earlier clinical intervention and more proactive care management.
C. Governance and Clinical Oversight Frameworks
Technology alone does not guarantee the success of CDS programs.
Mindbowser works with hospital leadership teams to design governance frameworks that ensure the clinical decision support system remains clinically relevant, transparent, and continuously monitored.
Governance programs typically include:
- CDS review committees led by physician informaticists
- Rule approval and change management workflows
- Monitoring of alert acceptance and override patterns
- Periodic validation of predictive models
- Alignment with updated clinical guidelines
These governance practices ensure the clinical decision support system remains trusted by clinicians and aligned with patient safety goals.
D. Workflow Integration Across Clinical Environments
A clinical decision support system only works when guidance appears inside clinician workflows.
Mindbowser focuses heavily on workflow integration across multiple care settings:
- Inpatient hospital units
- Emergency departments
- Ambulatory care clinics
- Population health management programs
Decision support recommendations are embedded directly inside the EHR interface, so clinicians receive guidance during medication ordering, diagnostic evaluation, and care planning.
This approach ensures point-of-care decision support becomes a natural part of clinical decision-making rather than an additional step.

What Should Hospital Leaders Expect From a Clinical Decision Support System?
For CIOs and CMIOs, the value of a clinical decision support system ultimately comes down to measurable improvements in patient safety and clinical consistency.
When designed with strong workflow integration and clinical governance, a clinical decision support system helps clinicians make safer decisions by identifying medication risks, detecting patient deterioration earlier, and reinforcing evidence-based treatment guidelines directly at the point of care.
Hospitals that treat their clinical decision support system as a continuously monitored clinical program rather than a one-time technology deployment see the strongest outcomes, including fewer adverse drug events, improved guideline adherence, and better performance under value-based care models.
Implementation timelines vary depending on the hospital’s EHR environment and the complexity of the decision rules being added. Many organizations begin with a few high-priority safety use cases and expand over time. Initial deployments can take a few months, while full programs may evolve over several phases.
Yes. Smaller hospitals often benefit significantly because decision support helps clinicians quickly access guideline-based recommendations during busy workflows. It can also help standardize care across teams when specialist resources are limited.
Clinician trust usually depends on how well the system fits into their workflow and how accurate the recommendations are. When alerts are relevant and based on clear medical evidence, clinicians are far more likely to use them. Strong governance and regular updates also help maintain trust.
No. A clinical decision support system is designed to assist clinicians, not replace them. It highlights risks, provides evidence-based guidance, and supports decisions, but the final clinical judgment always remains with the healthcare provider.
Hospitals typically track outcomes such as reduced medication errors, earlier detection of patient deterioration, and improved adherence to clinical guidelines. Many organizations also monitor alert acceptance rates and quality metrics tied to value-based care programs. These measures help determine whether the system is improving patient safety and care quality.
Interruptive alerts require the clinician to acknowledge a message before continuing — these are reserved for high-severity risks like dangerous drug interactions or allergy conflicts. Non-interruptive decision support presents guidance passively, such as recommended order sets or documentation prompts, without stopping the clinical workflow. Most hospitals aim to minimize interruptive alerts to reduce alert fatigue.
Alert fatigue occurs when clinicians receive too many notifications and begin dismissing them without review. Research shows override rates can exceed 80% for certain alert categories. Effective CDSS programs address this by limiting interruptive alerts to genuinely high-risk scenarios, continuously monitoring override patterns, and involving clinicians in refining alert logic over time.
A clinical decision support system typically draws from patient demographics, diagnoses, medication histories, laboratory results, allergies, vital signs, and imaging results — all sourced from the EHR in real time. It applies clinical rules or predictive models to this data to generate patient-specific guidance at the point of care.































![10 Clinical Decision Support System Examples With Real Metrics [2026]](https://www.mindbowser.com/wp-content/uploads/2025/08/Clinical-Decision-Support-System-1024x324.jpg)
![Advanced Clinical Decision Support: Architecture, CDS Hooks, and Real Results [2026]](https://www.mindbowser.com/wp-content/uploads/2025/08/Mobile-Technology-in-Healthcare-1-1024x324.jpg)


![5 Types of Clinical Decision Support Systems: Which One Fits Your Hospital? [2026]](https://www.mindbowser.com/wp-content/uploads/2026/03/medical-technology-network-telemedicine-health-insurance-virtual-hospital-healthcare-1024x585.jpg)