TL;DR
- Don’t just build an app—build a platform. Virtual care requires connected workflows, not one-off video consults.
- Start with your care model. Whether it’s mental health, fertility, or rehab, your clinical vision should define your roadmap.
- Architect for scale from day one. Modular systems, reusable AI workflows, and integration-ready infrastructure ultimately prevail.
- Use AI to reduce admin, not replace care. Intake, follow-ups, and documentation support are high-impact areas of focus.
- Build for continuity, not just consults. Features such as asynchronous messaging and personalized care plans help keep patients engaged.
- Work with a partner who has experience in healthcare. Accelerators like TelePrep AI, CarePlan AI, and HealthConnect CoPilot can cut dev time by 30–40%
I. What Are Open Models and Why Do They Matter?
A. Definition and Core Benefits
In simple terms, open models are artificial intelligence tools you can run within your hospital systems. There’s no need to connect to an external server or rely on cloud platforms. That means you don’t have to send any patient data outside your firewall.
These models work directly on your local hardware, whether it’s a hospital data center or an on-premises server, giving your team complete control. You’re not locked into recurring usage fees or vendor terms. Instead, it’s a one-time setup that you can customize, monitor, and maintain as needed.
For healthcare organizations focused on compliance, privacy, and operational control, open models provide a safer and more flexible approach to leveraging AI in day-to-day workflows.
Key Benefits for Hospitals and Providers:
- Set up once and run without ongoing API fees
- Reliable performance even without internet access
- Tailor the system to match your clinical workflows
- Patient data stays within your internal environment, simplifying HIPAA alignment
B. Core Characteristics of OpenAI’s Open Models
OpenAI’s suite of open models, including the widely discussed GPT-OS, was designed with practical healthcare needs in mind. These models don’t just answer questions; they can handle more complex workflows, such as reviewing medical documents, summarizing clinical notes, or analyzing patient data for care planning.
As Atul Deo, Director of Product at AWS, explains:
Here’s What Makes Them Stand Out:

II. How Can Open Models Help Healthcare Teams?
AI isn’t new to healthcare, but running it securely, cost-effectively, and on your terms has always been a challenge. Most healthcare organizations rely on third-party cloud platforms, which often raise concerns about data privacy, compliance, and long-term costs. Open models change that by providing health systems with a way to bring AI in-house without compromising control or flexibility.
Here’s how these models can support hospital systems, clinics, and care teams.
A. Enable HIPAA-Compliant AI Apps Without the Cloud
One of the biggest concerns with AI in healthcare is data safety. Providers work with protected health information (PHI), and any external data transfer introduces risk. Open models stay inside your environment, which helps support HIPAA compliance and reduces dependency on external vendors.
By running AI directly on your internal servers, hospitals can build and operate applications that support clinical and operational needs without ever sending data off-site. This opens the door to use cases that were previously off-limits.
With Open Models, Health Systems Can Build Tools for:
- Clinical decision support: Help physicians assess symptoms, review histories, or suggest next steps based on evidence, all in real-time.
- Medical imaging support: Utilize AI to aid radiologists in identifying patterns or reviewing imaging results more efficiently.
- Triage and intake automation: Speed up patient intake processes with intelligent front-line screening tools.
- Patient education tools: Deliver clear, accurate health information through virtual assistants that speak the patient’s language, both literally and clinically.
These solutions don’t need internet access, don’t rely on vendor APIs, and can be updated and refined based on your team’s real-world experience.
Related read: How to Become HIPAA Compliant?
B. Improve Privacy and Security
Healthcare CIOs and compliance officers are justified in being cautious about data movement. The more systems your data passes through, the more potential points of failure exist.
With open models, you eliminate the need to share PHI with external parties. All patient data remains within your network. There’s no cloud connection, no external storage, and no third-party access, making it easier to meet internal security protocols, satisfy auditors, and reduce risk.
Key Privacy and Security Advantages Include:
- Local data processing: Everything stays on-site, within your hospital network.
- Air-gapped compatibility: Open models can be deployed in tightly restricted environments.
- Secured device integrations: Whether it’s wearables or bedside monitoring systems, open models can support secure, encrypted data connections internally.
For hospitals that are already investing heavily in cybersecurity, open models make it easier to protect patient data while still leveraging the latest AI capabilities.
C. Make AI Work in Low-Connectivity Settings
Not every clinic has consistent high-speed internet, especially in rural communities or mobile health units. That’s where open models offer a significant advantage.
Because these models don’t require an ongoing internet connection, they can be deployed in environments with limited or unreliable connectivity. They can run on a local device, process data in real-time, and help care teams deliver services even when cloud-based tools are unavailable.
Use Cases for Low-Connectivity Settings:
- Rural clinics: Run AI locally without needing to connect to external servers.
- Mobile units: Use AI during field visits or emergency deployments.
- Backup support: Maintain AI tools’ operation during planned or unplanned network outages.
This makes open models especially important for health systems with large geographic footprints or those serving hard-to-reach communities.

III. Who Benefits Most From Local AI Models?
Open models aren’t just another technology trend. They represent a practical solution for some of healthcare’s most persistent challenges, particularly in areas such as security, cost control, and system flexibility. While their impact is broad, the real value becomes apparent when we examine the types of organizations and roles that stand to gain the most.
A. Industries That Can Now Safely Use AI
The idea of running AI inside your organization, without needing to send data to the cloud, makes these models valuable across sectors. But in healthcare, where data privacy and regulation are top priorities, the benefits are obvious.
Healthcare
Hospitals, clinics, and digital health platforms can use open models for:
- Remote patient monitoring (RPM): Analyze data from home devices to flag early warning signs.
- Diagnostics: Help clinicians review test results and imaging more efficiently and accurately.
- Discharge planning: Summarize the patient’s history and outline next steps before they leave the hospital.
Finance
Banks and insurers handling sensitive client data can benefit from:
- Risk scoring: Analyze client profiles and financial history in-house.
- Compliance: Build systems that meet strict internal and external audit requirements.
Legal
Law firms and legal departments can use open models for:
- Contract analysis: Review internal documents for risk and compliance.
- Brief summarization: Speed up case prep while keeping information secure.
Government
Government agencies involved in healthcare, emergency management, or justice can benefit from:
- Field operations: Run models securely in restricted or offline environments.
- Sensitive data workflows: Process confidential records without external dependencies.
Across all these sectors, the appeal remains the same: deploy advanced AI while maintaining full data control locally.
B. Healthcare Stakeholders Impacted
Within healthcare specifically, several roles are directly impacted by the shift toward open models. These are the individuals who manage AI strategy, develop the tools, or are responsible for ensuring patient safety and regulatory compliance.
CTOs and CIOs
Chief technology and information officers are responsible for aligning IT infrastructure with strategic goals. With open models, they can:
- Reduce reliance on costly external APIs
- Deploy AI without cloud integration challenges
- Ensure compliance while enabling innovation
Clinical Product and Development Teams
Teams building healthcare applications from telehealth platforms to diagnostic tools can use open models to:
- Customize logic and workflows to match provider needs
- Avoid vendor lock-in and retain IP ownership
- Test and iterate quickly without needing external approvals
Compliance and Privacy Officers
These professionals are responsible for ensuring the organization remains compliant with HIPAA, SOC 2, and other relevant regulatory frameworks. Open models help them:
- Maintain PHI governance
- Simplify documentation for audits
- Minimize exposure to third-party risks
Digital Health Founders and Series B+ Teams
Startups entering scale mode often face a trade-off between moving fast and meeting compliance expectations. Open models let them:
- Differentiate with more secure, localized AI
- Serve health systems that demand on-prem solutions
Reduce operating costs by avoiding usage-based pricing
Is Your Organization Ready to Leverage Local AI Models for Better Security, Compliance, and Cost Savings?
IV. What Are the Big Opportunities?
Open models unlock real, measurable value across healthcare, not just in theory, but in ways that impact care delivery, operations, and business models today. The ability to run high-performing AI directly within a hospital’s systems introduces entirely new opportunities for mid-size providers and digital health companies.
These aren’t marginal gains. They involve structural changes to how health systems can operate and innovate without incurring risk or runaway costs.
A. For Mid-size US Hospitals
Mid-size health systems often face the same compliance, staffing, and cost pressures as larger networks, but without the same scale or capital. Open models help level the playing field.
Here’s where they can make a meaningful difference:
1. Automate Administrative Tasks
Clerical work continues to consume large portions of staff time. Open models can take over repetitive back-office operations, including:
- Claims processing
- Prior authorization workflows
- Patient intake form classification
- Appointment scheduling and follow-up reminders
These tasks don’t require a connection to a cloud-based AI vendor. They can be done entirely in-house, which lowers your costs and eases the load on your administrative team.
2. Streamline Clinical Documentation
Documentation fatigue contributes heavily to burnout among clinicians. Open models can turn spoken or written notes into structured EHR entries, SOAP notes, referral letters, or discharge summaries.
With tools running locally, physicians can see immediate value without worrying about where their notes are going or who might see them.
3. Improve Patient Safety
When AI works alongside clinical teams, the results speak for themselves:
- A 16% reduction in diagnostic errors
- A 13% drop in treatment mistakes
These improvements don’t require a massive system overhaul. Mid-sized hospitals can implement open models gradually, starting with high-impact workflows such as ER triage, early warning alerts, or decision support during care transitions.
Open models also support faster internal innovation. Instead of waiting on vendor timelines or submitting data to a third party, clinical leaders can work directly with internal IT teams to adjust and improve how AI supports care.
B. For US Digital Health Startups
Once a digital health startup reaches product-market fit, the focus shifts to differentiation and scale. For AI-native teams, open models provide more than just technical benefits; they unlock new ways to build, price, and deliver value to providers and payers.
1. Build Specialized Agentic AI
Instead of relying on generic models with generic answers, healthtech teams can:
- Build and fine-tune models for highly specific tasks, like medical coding or triage logic.
- Customize workflows that mirror real-life provider behavior.
- Deploy internal AI agents that perform tasks end-to-end, like surfacing a diagnosis and drafting the referral letter in one loop.
These capabilities drive adoption among clinicians who want tools that understand their daily challenges, not just text prompts.
2. Deliver Clinical Intelligence
Startups like OpenEvidence and Ambience Healthcare are already demonstrating how open models can power tools that extract evidence from research literature, EHRs, and clinical guidelines, right when a provider needs it.
When you control the model and the environment, you can fine-tune outputs to reflect the latest research and provider preferences without relying on API limits or delays in third-party documentation.
3. Enable Precision Medicine at Scale
From pharmacogenomics to remote monitoring, modern care is increasingly personalized. Open models can process massive, complex datasets:
- Predicting how a patient might respond to medication
- Flagging side effects early
- Identifying candidates for clinical trials
- Designing treatment plans based on a person’s health history and current biomarkers
These workflows were previously limited by access, infrastructure, or cost. Now, startups can deploy them in a compliant, secure, and scalable way without sending any data out of bounds.
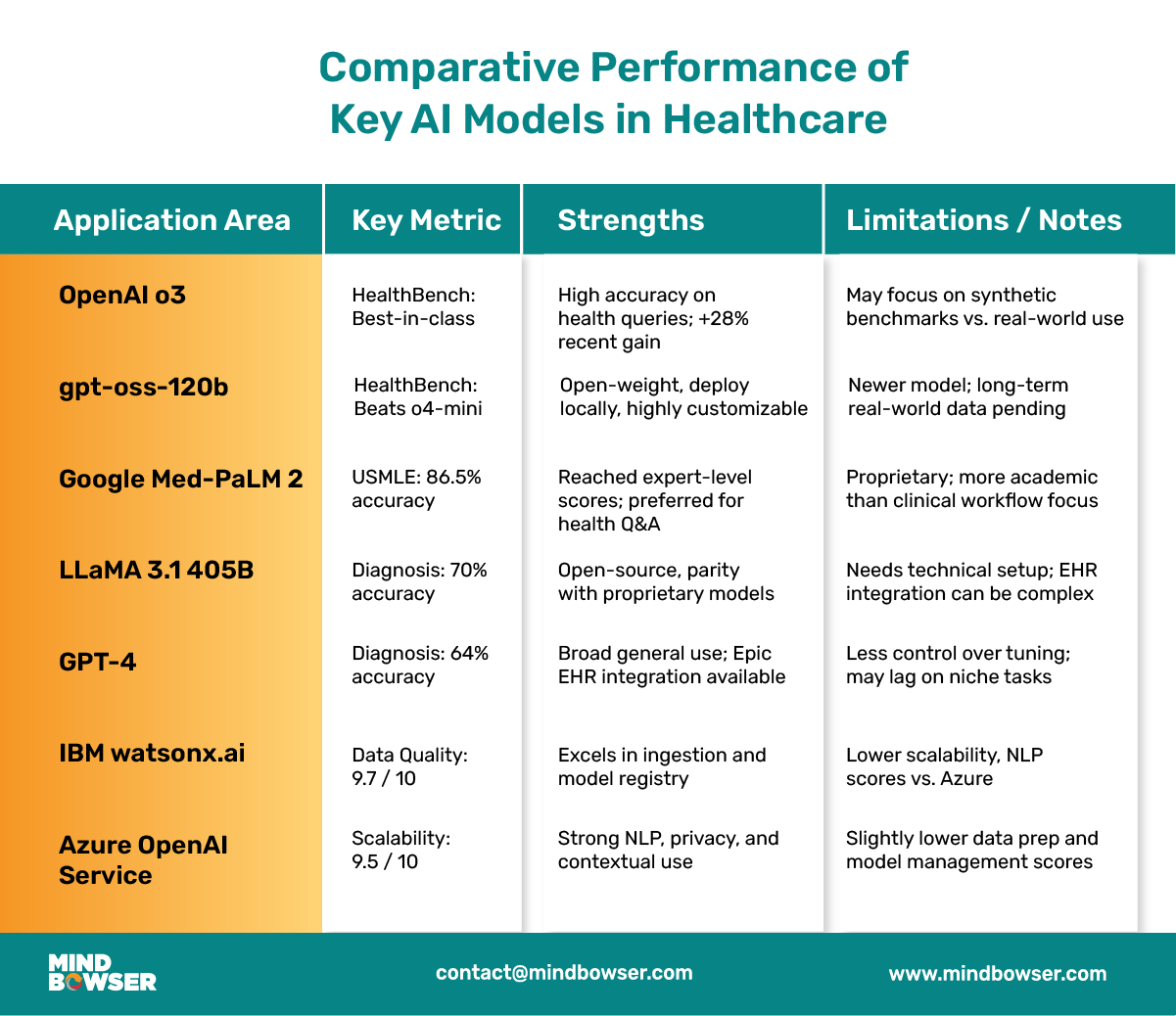
This table helps teams understand how open models compare with proprietary platforms. While top commercial models remain strong, open models like GPT-OSS are closing the gap and offer something others can’t: full control.
V. Why This Changes the Game for Healthcare CTOs
Chief technology officers in healthcare face a challenging balance: delivering innovation while meeting stringent regulatory and budget demands. With every new digital initiative, CTOs must weigh factors like patient privacy, security, interoperability, vendor management, and cost efficiency.
Open models shift that equation. They remove many of the roadblocks that have historically hindered the implementation of AI in healthcare environments. Instead of being limited by external infrastructure or locked into expensive vendor ecosystems, CTOs can now run advanced AI systems entirely within their infrastructure.
A. Before vs. After Comparison
Let’s take a look at how things worked before open models and how they work now.

What This Means for Healthcare Systems:
- You no longer need to pay recurring fees for every request, every task, or every user.
- You’re not waiting for an external vendor to approve a change or unlock a new feature.
- You don’t need to send any PHI to an external cloud just to enable AI.
- You can tailor AI to how your care teams operate, not how an external system was designed.
These changes don’t just reduce complexity. They allow CTOs to lead with flexibility and confidence, knowing the tools they build will meet both clinical expectations and board-level requirements.
B. CTO-Focused Benefits
Let’s break down what this unlocks for healthcare IT leaders.
1. Reduced Operational Costs
Instead of incurring monthly cloud bills based on unpredictable usage, your team pays once and deploys as needed. This predictable pricing model gives you better financial visibility while keeping budgets under control.
For organizations managing multiple care sites or applications, this also opens up the ability to scale without incurring additional expenses.
2. Full Workflow Ownership
Customization is a critical issue in healthcare. No two hospital systems operate in the same way, and a generic AI model often fails to account for local protocols, clinical preferences, or documentation styles.
With open models:
- You can retrain or fine-tune the model using your de-identified data
- You control how recommendations are made and when they are surfaced
- You can adapt to new clinical guidelines or administrative requirements without delays
In other words, your AI system can evolve in tandem with your organization.
3. Stronger Clinical Buy-In
Healthcare technology adoption depends on clinician trust. Doctors, nurses, and staff want to know:
- How is this tool helping me?
- Can I trust what it’s telling me?
- Is it using patient data responsibly?
Open models support transparency. Developers can demonstrate how the model arrived at its answer. Clinical leaders can review and audit outputs. That builds trust, and trust leads to usage.
4. Data Governance and Compliance Confidence
One of the biggest advantages of open models is data locality. Patient data doesn’t leave your network. There are no third-party processors, no vague external audit trails, and no need for additional HIPAA business associate agreements.
This allows your compliance team to:
- Simplify documentation
- Reduce the scope of risk assessments
- Maintain full oversight of how and where PHI is used
The result? Faster approvals, smoother audits, and fewer concerns when introducing new workflows.
Open models transform AI from a product that healthcare organizations purchase to one they build, own, and evolve with. For forward-thinking CTOs, it’s not just a technical upgrade’s a shift in how innovation is delivered across the enterprise.
Ready to Take Control of Your AI Infrastructure and Unlock the Benefits of Open Models?
Talk to our team and accelerate your product’s clinical utility—without slowing down development.
VI. Business Model Shifts for HealthTech Startups
For digital health startups, especially those with a working product and Series B+ funding, open models present a rare opportunity that changes both how you build and how you sell. These models give startups a way to deliver AI in healthcare without being dependent on someone else’s infrastructure, pricing, or roadmap.
It’s not just a technical shift. It’s a strategic one.
Startups that adopt open models can unlock faster sales cycles, improved clinical adoption, and a pricing structure that facilitates long-term scaling for both the builder and the buyer.
A. Strategic Changes
Traditional AI offerings in healthtech are often built as cloud-based SaaS products. That model has its benefits and limitations:
- High ongoing infrastructure costs
- Vendor lock-in that limits flexibility
- Ongoing privacy and compliance concerns for provider customers
- Resistance from IT teams who want more control over data
Open models offer a clear alternative.
Here’s how the business model shifts with open AI architecture:
1. Offer One-Time Pricing Instead of Subscriptions
Rather than billing hospitals monthly for API usage or cloud hosting, you can provide AI as a one-time license or a fixed deployment fee. This structure is attractive to hospitals looking to minimize variable costs and reduce long-term budget exposure.
It also puts your product in line with other capital investments hospitals already make, like EHR modules, imaging software, or lab systems.
2. Serve Privacy-Focused Buyers with On-Premise Installations
Many large hospital systems have security policies that make them cautious about third-party software, especially tools that send data to the cloud. By offering a local deployment model, your startup can gain entry into organizations that might otherwise decline.
This includes:
- Government-funded hospitals
- Academic medical centers
- Rural networks with limited bandwidth
- Providers operating under strict internal data governance rules
You become a vendor who says, “Yes, we can meet your privacy policy” rather than asking them to make exceptions.
3. Avoid Cloud Costs and API Rate Limits
Every cloud-based product eventually reaches a ceiling where infrastructure costs start to eat into margins. If your AI relies on commercial APIs, you may also face limits on how fast or how often you can run certain functions.
With open models:
- You control how many calls are made, how fast they run, and how much it costs
- You’re not passing rising API fees onto your customers
- You can support unlimited users or concurrent sessions without changing your pricing
That flexibility can make your product more competitive, especially when buyers compare it to SaaS tools with usage-based pricing.
B. Market Readiness Signals
There’s growing alignment between what healthcare investors are looking for and what open models can help startups deliver. Series B+ companies need to demonstrate not just product-market fit but enterprise readiness. That includes:
- Clear value for large systems
- A path to profitability
- A product that checks compliance boxes out of the gate
Open models support all of those goals.
1. Investors Are Favoring AI-Native, Compliance-Secure Platforms
We’re seeing increasing attention from venture capital firms toward startups that:
- Build their own AI models
- Retain full control over deployment
- Can sell to hospitals without needing extra security reviews or BAAs
Startups that adopt open models demonstrate significant engineering capabilities and a profound understanding of healthcare IT challenges. That gives investors confidence in your product and in your team’s ability to secure long-term deals.
2. IP Differentiation and Clinical Traction
When you train or fine-tune a model for a specific clinical use case, you’re not just integrating another vendor’s API. You’re building something defensible.
This allows you to:
- Develop intellectual property that adds value during fundraising
- Deliver features competitors can’t replicate quickly
- Show real-world outcomes that prove clinical impact
Whether you’re selling to hospitals, payers, or employers, this kind of differentiation is what moves a pilot into a long-term contract.
In short, open models give healthtech founders a new kind of playbook:
- Build smarter
- Sell faster
- Scale more profitably
For Series B+ startups, this is how you transition from a great demo to a market leader without compromising on compliance or margin.
VI. Business Model Shifts for HealthTech Startups
For digital health startups, especially those with a working product and Series B+ funding, open models present a rare opportunity that changes both how you build and how you sell. These models give startups a way to deliver AI in healthcare without being dependent on someone else’s infrastructure, pricing, or roadmap.
It’s not just a technical shift. It’s a strategic one.
Startups that adopt open models can unlock faster sales cycles, improved clinical adoption, and a pricing structure that facilitates long-term scaling for both the builder and the buyer.
A. Strategic Changes
Traditional AI offerings in healthtech are often built as cloud-based SaaS products. That model has its benefits and limitations:
- High ongoing infrastructure costs
- Vendor lock-in that limits flexibility
- Ongoing privacy and compliance concerns for provider customers
- Resistance from IT teams who want more control over data
Open models offer a clear alternative.
Here’s how the business model shifts with open AI architecture:
1. Offer One-Time Pricing Instead of Subscriptions
Rather than billing hospitals monthly for API usage or cloud hosting, you can provide AI as a one-time license or a fixed deployment fee. This structure is attractive to hospitals looking to minimize variable costs and reduce long-term budget exposure.
It also puts your product in line with other capital investments hospitals already make, like EHR modules, imaging software, or lab systems.
2. Serve Privacy-Focused Buyers with On-Premise Installations
Many large hospital systems have security policies that make them cautious about third-party software, especially tools that send data to the cloud. By offering a local deployment model, your startup can gain entry into organizations that might otherwise decline.
This includes:
- Government-funded hospitals
- Academic medical centers
- Rural networks with limited bandwidth
- Providers operating under strict internal data governance rules
You become a vendor who says, “Yes, we can meet your privacy policy” rather than asking them to make exceptions.
3. Avoid Cloud Costs and API Rate Limits
Every cloud-based product eventually reaches a ceiling where infrastructure costs start to eat into margins. If your AI relies on commercial APIs, you may also face limits on how fast or how often you can run certain functions.
With open models:
- You control how many calls are made, how fast they run, and how much it costs
- You’re not passing rising API fees onto your customers
- You can support unlimited users or concurrent sessions without changing your pricing
That flexibility can make your product more competitive, especially when buyers compare it to SaaS tools with usage-based pricing.
B. Market Readiness Signals
There’s growing alignment between what healthcare investors are looking for and what open models can help startups deliver. Series B+ companies need to demonstrate not just product-market fit but enterprise readiness. That includes:
- Clear value for large systems
- A path to profitability
- A product that checks compliance boxes out of the gate
Open models support all of those goals.
1. Investors Are Favoring AI-Native, Compliance-Secure Platforms
We’re seeing increasing attention from venture capital firms toward startups that:
- Build their own AI models
- Retain full control over deployment
- Can sell to hospitals without needing extra security reviews or BAAs
Startups that adopt open models demonstrate significant engineering capabilities and a profound understanding of healthcare IT challenges. That gives investors confidence in your product and in your team’s ability to secure long-term deals.
2. IP Differentiation and Clinical Traction
When you train or fine-tune a model for a specific clinical use case, you’re not just integrating another vendor’s API. You’re building something defensible.
This allows you to:
- Develop intellectual property that adds value during fundraising
- Deliver features competitors can’t replicate quickly
- Show real-world outcomes that prove clinical impact
Whether you’re selling to hospitals, payers, or employers, this kind of differentiation is what moves a pilot into a long-term contract.
In short, open models give healthtech founders a new kind of playbook:
- Build smarter
- Sell faster
- Scale more profitably
For Series B+ startups, this is how you transition from a great demo to a market leader without compromising on compliance or margin.
Ready to Transform Your Digital Health Startup with Open Models?
Contact us to discover how you can scale faster, reduce costs, and enhance product differentiation.
VII. What Healthcare Builders Should Do Now
Whether you’re a hospital innovation leader, a healthtech founder, or part of a clinical product team, you may be asking, “Where do we begin with open models?”
The good news is that getting started doesn’t mean overhauling your entire infrastructure. With the right focus and partners, you can integrate open models into real clinical workflows, step by step.
As Dmitry Pimenov, Product Lead at OpenAI, notes:
This section outlines a simple action plan and use case examples to help teams move from awareness to execution.
A. Your 3-Step Action Plan
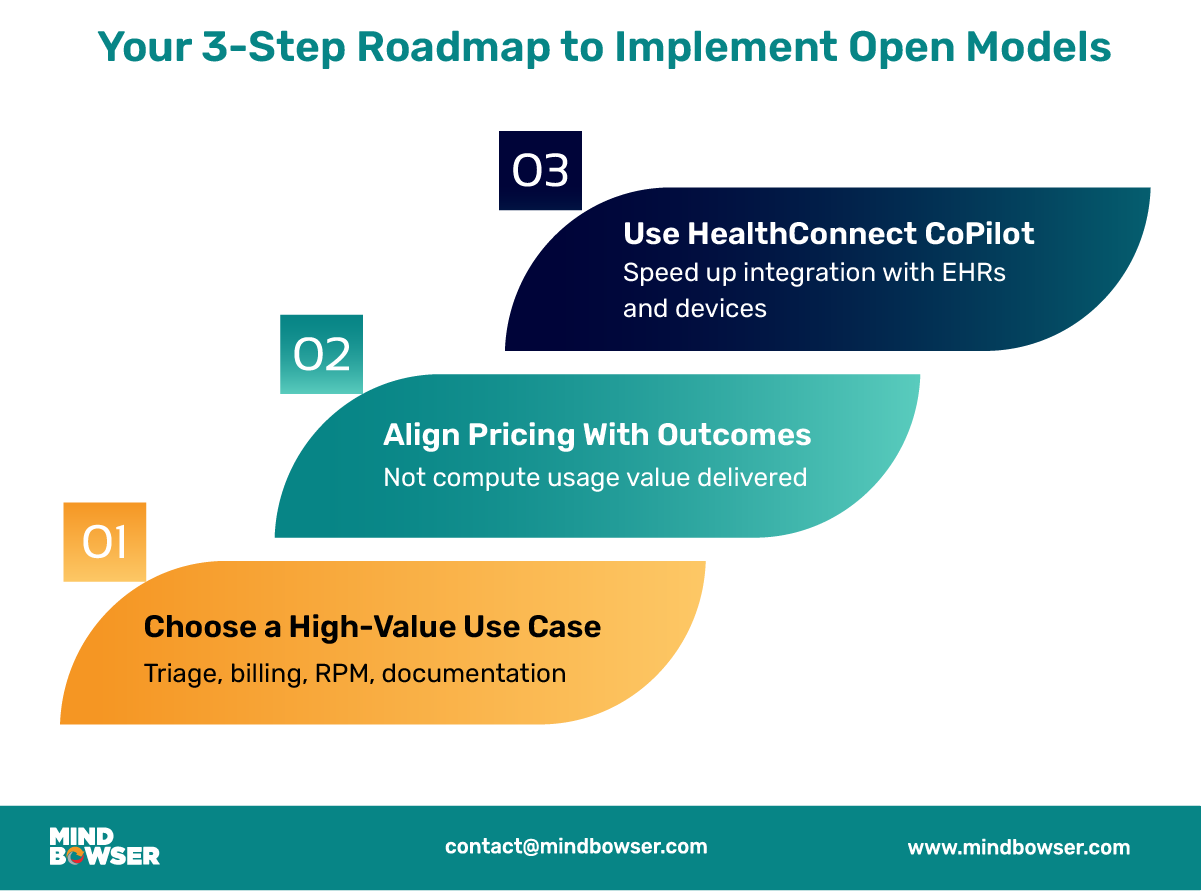
1. Pick a Regulated Use Case That Solves a Real Problem
Start with a use case where data sensitivity, speed, or cost makes traditional cloud-based AI harder to use. Good first candidates include:
- Triage bots that analyze intake symptoms and suggest next steps
- Billing assistants who review claims or detect missing codes
- Remote patient monitoring that works without sending data offsite
- Discharge planning that summarizes patient notes in real time
These use cases are measurable, meaningful, and easily contained within existing systems.
2. Price Based on Delivered Value, Not Volume
If you’re building a product around open models, avoid usage-based pricing. Instead, align your pricing to the business outcome your tool helps achieve.
For example:
- A tool that reduces documentation time by 30%? Price it against staff time saved.
- A claims tool that cuts denials by 20%? Price it based on recovered revenue.
- A patient engagement assistant that increases follow-up rates? Price it based on improved compliance metrics.
Buyers appreciate pricing that reflects performance, not compute usage.
3. Use Accelerators Like HealthConnect CoPilot to Speed Up Integration
For healthcare builders, integration is often the bottleneck. Connecting your AI to EHRs, HL7 feeds, or wearable devices is where great ideas can stall.
Our HealthConnect CoPilot solves that by offering:
- Pre-built modules for HL7 and FHIR workflows
- Connectivity with popular RPM devices and Apple Health
- Compliance-ready infrastructure for HIPAA and SOC 2
You don’t need to reinvent the wheel. Utilize platforms like HealthConnect to achieve production faster and more safely.
B. Use Case Ideas for Providers
If you’re a hospital IT or innovation team, consider where open models could help today, not five years from now.
1. Real-Time Pathology or Imaging Analysis
Open models can be trained to identify anomalies in radiology reports or pathology slides, enabling clinicians to prioritize critical cases.
2. High-Risk Patient Monitoring With Wearables
AI can analyze streams of vitals and send real-time alerts without sending data to the cloud. This is especially useful in cardiac, pulmonary, or post-op cases.
3. Smart Operations With RTLS and IoT
Utilize AI to analyze real-time location systems (RTLS) data and forecast delays, bottlenecks, or staff utilization gaps.
4. Mental Health and Post-Visit Engagement Bots
After discharge or a virtual consultation, AI-driven assistants can check in with patients, answer follow-up questions, and notify providers if anything seems amiss.
These are high-impact, low-barrier entry points for most care settings.
C. Use Case Ideas for Digital Health Builders
If you’re a health tech company building AI-native products, open models enable you to design more innovative tools with complete data control.
1. Synthetic Patient Data for Clinical Trials
Use open models to generate synthetic datasets for rare diseases or small patient groups, ideal for research, while maintaining privacy.
2. AI-Driven Claims and Revenue Cycle Tools
Automate coding, documentation gap detection, and payer response management all within your infrastructure.
3. Drug Discovery and AI Co-Scientists
Combine model fine-tuning with biomedical literature mining to create agents that assist in designing compounds or identifying trial candidates.
4. Personalized Treatment Planning
Open models can be trained to recommend care pathways based on genomics, patient history, and current vitals without sending any PHI outside your platform.
These ideas are not just possible, they’re already being built.

How Mindbowser Can Help
Open models are powerful, but deploying them successfully in healthcare takes more than just downloading weights and spinning up a server. You need the right partner, one who understands healthcare regulations, EHR integration, user experience, and the operational realities of clinical settings.
That’s where Mindbowser comes in.
We’ve spent over a decade helping healthcare organizations, from early-stage startups to enterprise hospital systems, design, build, and scale technology that meets clinical, technical, and regulatory standards. We don’t just understand AI. We understand healthcare.
Here’s how we help bring open models to life for real-world healthcare use cases:
1. Healthcare-Ready AI Development
We work with product and clinical teams to:
- Fine-tune open models like gpt-oss for clinical and administrative tasks
- Train models with healthcare-specific language and workflows
- Build internal agents that follow task chains (e.g., analyze → summarize → suggest)
- Ensure output is accurate, safe, and user-friendly for frontline staff
Whether you’re launching a triage assistant or building a decision support engine, we help you start with the right model and then shape it to your specific needs.
2. EHR, HL7, and FHIR Integration
Our HealthConnect CoPilot is a pre-built accelerator that handles:
- HL7 and FHIR integration with major EHRs
- Patient data normalization
- Wearable and RPM device connectivity
- HIPAA-compliant infrastructure for secure deployment
This saves months of engineering effort and gets your AI product connected to real clinical data faster with fewer compliance headaches.
3. Secure, On-Premise Deployment
We support your IT team in setting up:
- Edge-compatible AI environments (running on CPU/GPU with as little as 16 GB RAM)
- Open model hosting using tools like vLLM or Ollama
- Local workflows that meet internal audit and access control policies
From architecture to implementation, our teams know how to work inside the constraints and controls required by hospital IT and security teams.
4. Compliance-First Engineering
Mindbowser has deep experience building for:
- HIPAA and SOC 2 compliance
- FDA Software as a Medical Device (SaMD) guidelines
- CFR Part 11 (for clinical trial tools and data integrity)
We integrate security and compliance into every phase of design and development. That includes audit-ready documentation and support for third-party validation.
5. Full Product and Clinical Strategy Support
Our cross-functional teams bring together:
- Clinical SMEs to validate AI outputs
- Product designers to create intuitive workflows
- Backend engineers to handle data, infrastructure, and scaling
- Quality assurance experts to test edge cases and fail-safes
Whether you’re a hospital system building internal tools or a healthtech company going to market, we meet you where you are and help you get to where you want to go.

Final Thoughts
Healthcare has long needed a better way to use artificial intelligence that puts providers in control, protects patient data, and makes financial sense. Open models offer precisely that.
They allow hospitals, health systems, and digital health companies to run powerful AI tools locally, without relying on outside vendors or cloud-based infrastructure. This means you can design AI workflows around your patients, your teams, and your goals without compromising on privacy, compliance, or cost predictability.
For mid-size hospitals, open models offer a path to modernize clinical and administrative operations while keeping data in-house. For startups, they offer a competitive edge: the ability to build flexible, secure, and scalable products that are easier to sell to providers.
The shift from cloud-first to control-first AI is already underway. Health systems that move now can set the pace for how AI is used not just in labs, but on the front lines of care.
Open models run entirely within your infrastructure on local servers or secure on-premise environments. Because no data is sent to external APIs or third-party clouds, your team retains full control over protected health information (PHI). This makes it significantly easier to align with HIPAA, conduct risk assessments, and meet audit requirements.
Yes, in many cases, they can. Models like gpt-oss-120b have demonstrated performance that matches or even exceeds some commercial models in healthcare-specific benchmarks, including diagnostic reasoning and structured data tasks. The added advantage is full customizability and lower total cost of ownership.
Many open models can run on modest infrastructure. For example, gpt-oss-20b operates on edge devices with 16 GB of RAM. While high-volume workloads may benefit from GPU acceleration, most mid-size hospitals can deploy these models using standard compute environments already in place for EHR or imaging systems.
Start by identifying a workflow where automation could reduce friction, such as triage, note summarization, or claims review. From there, test an open model in a contained environment. Tools like Mindbowser’s HealthConnect CoPilot can simplify integration with EHRs, FHIR endpoints, and RPM data streams. Most teams begin with a pilot project, then expand once trust and ROI are proven.































