TL;DR
- Home health remote monitoring enables continuous patient tracking without hospital visits.
- RPM improves outcomes by enabling early intervention and reducing hospital readmissions.
- Caregiver involvement and real-time alerts improve adherence and coordination.
- Billing through CMS RPM CPT codes makes programs financially viable for agencies.
- Workflow-driven RPM helps home health teams scale care without increasing staff.
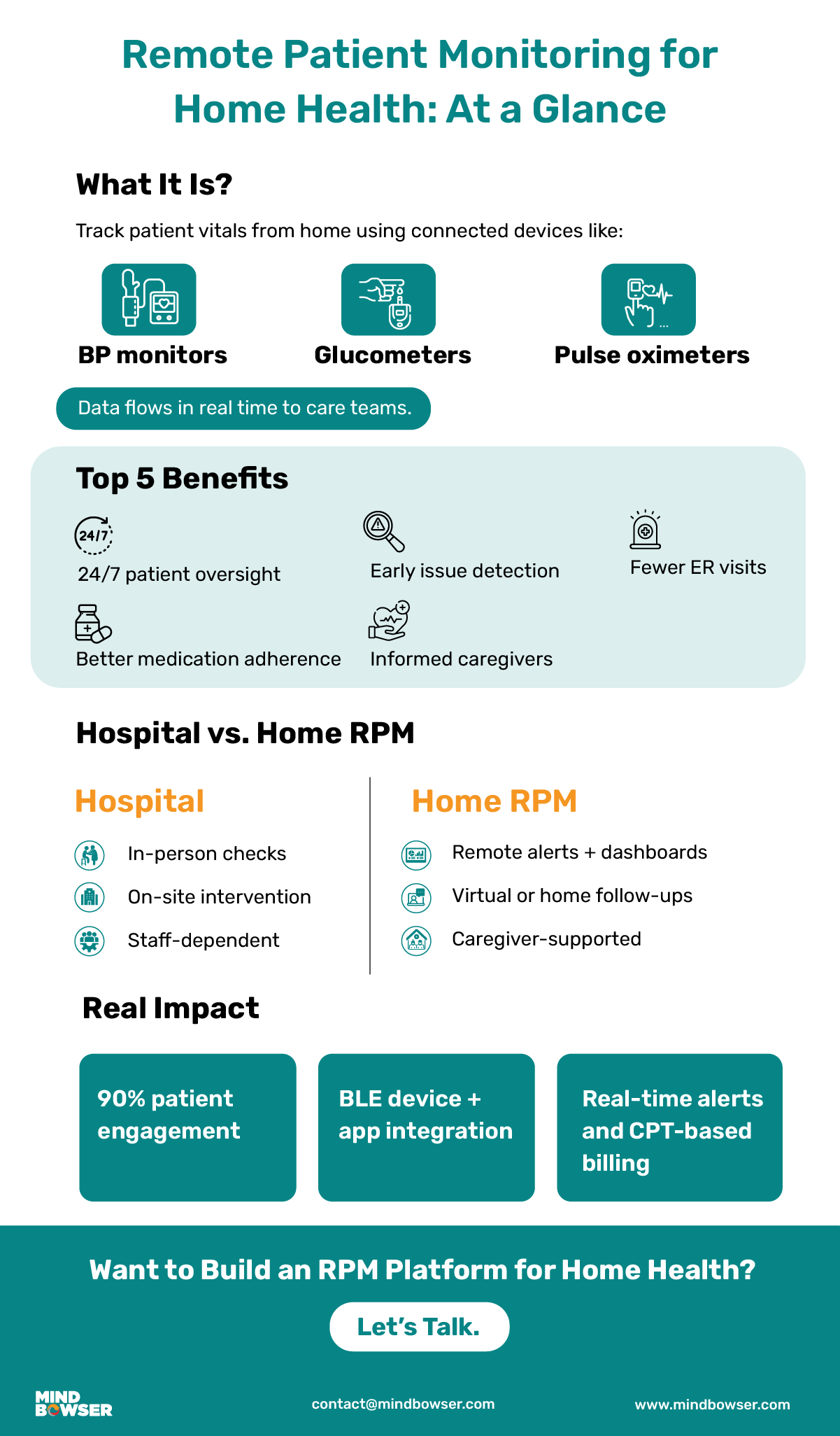
Home health remote monitoring enables providers to track patient health in real time while patients remain in their own homes. Instead of requiring frequent hospital or clinic visits, patients use connected medical devices such as blood pressure monitors, glucose meters, and pulse oximeters that transmit data directly to care teams. This allows healthcare providers to detect changes early, intervene quickly, and stay continuously connected without disrupting the patient’s daily environment.
In recent years, there’s been a noticeable shift in how care is delivered. More patients—especially those recovering from surgery, managing chronic illnesses, or aging—are choosing home-based care. It’s more comfortable, often more affordable, and fits better into daily life.
Remote monitoring is making this model of care safer and more effective, giving providers the tools to manage health proactively rather than reactively.
What is Remote Patient Monitoring for Home Health?
Remote patient monitoring (RPM) for home health refers to using connected medical devices to track patients’ health metrics from the comfort of their homes. These devices—blood pressure cuffs, heart rate monitors, glucose meters, and pulse oximeters—capture real-time vitals and securely transmit the data to healthcare providers. In some cases, wearable devices and mHealth apps are also part of the ecosystem, especially when continuous monitoring is necessary.
The goal is simple: keep patients safe, informed, and supported between clinical visits. This form of care works especially well for patients recovering from hospitalization, managing long-term conditions like diabetes or chronic obstructive pulmonary disease (COPD), or requiring supervision due to age-related risks.
RPM doesn’t replace healthcare professionals—it extends their reach. Providers can monitor patient trends, identify potential problems before they worsen, and adjust care plans accordingly.
What is Home Health Remote Monitoring and How Is It Different?
Home health remote monitoring refers to the use of connected medical devices and digital tools to track patient health outside traditional care settings, typically in the patient’s home. While it builds on the broader concept of remote patient monitoring (RPM), the key difference lies in how care is delivered and managed.
In hospital environments, monitoring is continuous and clinician-led, with staff available for immediate intervention. In contrast, home health remote monitoring operates in a decentralized setting where patients, caregivers, and care teams collaborate remotely.
This model relies on:
- Connected devices that capture vitals like blood pressure, glucose levels, oxygen saturation, and heart rate
- Asynchronous data review, where clinicians assess trends through dashboards instead of real-time bedside monitoring
- Alert-based intervention, where care teams are notified only when readings deviate from patient-specific thresholds
- Caregiver involvement, especially for elderly or high-risk patients who need support with device usage and daily care
Because there is no constant clinical supervision, home health remote monitoring systems must be intuitive, reliable, and designed around real-world patient behavior. Simplicity, adherence, and workflow integration matter more than feature complexity.
The goal remains the same: extend clinical oversight beyond the facility. But in home health settings, success depends on making monitoring actionable for care teams while keeping it easy for patients and caregivers to use consistently.
Home Health Remote Monitoring Billing and Reimbursement
For home health agencies, the viability of remote patient monitoring depends heavily on reimbursement.
RPM programs can be billed using CMS-approved CPT codes, including:
• 99453 – Device setup and patient onboarding
• 99454 – Device supply and data transmission
• 99457 – 20 minutes of clinical monitoring and management
• 99458 – Additional monitoring time
These codes allow agencies to generate recurring revenue while improving patient outcomes through RPM reimbursement and CPT codes.
However, successful reimbursement requires:
• Proper documentation of patient engagement
• Minimum interaction time thresholds
• Integration with clinical workflows
Agencies that combine home health remote monitoring with structured care management workflows see stronger reimbursement consistency and better ROI.
How Home Health RPM Differs from Hospital Monitoring
What sets home health RPM apart from traditional in-hospital monitoring is its decentralized nature. No nurse is making routine rounds. Instead, care relies on a combination of:
• Remote alerts: Devices notify clinicians when readings cross thresholds.
• Asynchronous data reviews: Providers check dashboards or receive summaries rather than sitting by the bedside.
• Caregiver involvement: In many cases, family members assist with setup, usage, or interpretation of device readings.
Unlike in clinical settings where tech and staff are readily available, remote patient monitoring for home health must be simple, reliable, and intuitive enough to work without constant supervision.
Case Example: Home Health RPM Engagement at Scale
In a home health RPM program built for a post-acute care provider, we implemented a workflow-driven monitoring system combining connected devices, automated check-ins, and care manager dashboards.
The result:
• 90% patient engagement in daily monitoring routines
• Faster identification of high-risk patients
• Reduced manual follow-ups for care teams
By combining home health remote monitoring with structured workflows, the program improved both clinical responsiveness and operational efficiency.
Planning to Build an RPM Platform for Elderly Care?
See how we brought together BLE integration, real-time vitals tracking, EHR dashboards, and billing workflows — all tuned for home health delivery.
Extending Clinical Oversight Beyond the Facility
24/7 Access to Patient Data
One of the biggest advantages of remote patient monitoring for home health is maintaining clinical oversight around the clock. Patients might be miles away from a clinic, but their vital signs are constantly monitored and reviewed. Care teams don’t have to rely solely on patient-reported symptoms or wait for in-person visits.
For example, through the solution we help build, providers gain real-time visibility into patient metrics like blood pressure, heart rate, and oxygen saturation—all updated via Bluetooth-connected medical devices. This live data feed equips clinicians to act swiftly when patterns shift or red flags appear, even before the patient realizes something’s wrong.
Our RPMCheck AI enhances this capability by enabling automated voice-based check-ins, which collect health data from home-based RPM devices and transmit it securely to care teams for timely review.
Clinical Escalation Without Travel
Remote patient monitoring for home health reduces the need for physical travel, both for patients and providers. If an elderly patient shows signs of a cardiac issue or abnormal glucose levels, the system can trigger alerts that prompt clinical review. Based on the severity, the team can respond with a phone call, video consultation, or schedule an urgent home visit.
This flexibility improves responsiveness while lowering the burden on emergency departments. With virtual triage and early intervention, health systems can address issues before they become crises.
Better Adherence Through Continuous Remote Tracking
Boosting Medication and Protocol Compliance
Remote patient monitoring for home health makes it easier for patients to follow their treatment plans consistently. When patients know their vitals are being tracked and reviewed, they will likely stick to medication schedules, therapy routines, and self-care protocols.
Daily readings—like checking blood pressure or blood sugar—aren’t just for doctors; they act as reminders and reinforce routines. When a patient skips a reading or submits an abnormal value, it signals a break in adherence, prompting timely follow-up.
We saw this firsthand in our work on a platform we helped build. The app offers patients a personalized exercise regimen with real-time heart rate monitoring. This immediate feedback loop helped patients stay on track, ensuring they completed their sessions safely and consistently.
A well-designed RPM care manager workflow ensures that alerts, follow-ups, and patient communication are handled efficiently without overwhelming clinical teams.
Monitoring Flags Anomalies for Early Intervention
RPM systems don’t wait for the next checkup—they alert providers when something looks off. A sudden drop in oxygen levels or a rising glucose trend doesn’t go unnoticed. These subtle shifts often signal worsening conditions that, if caught early, can be corrected without hospitalization.
With structured data flowing daily, care teams can spot deviations from the norm, investigate causes, and adjust treatment plans before symptoms escalate.
Many of these capabilities are powered by AI remote patient monitoring, which enables early risk detection and smarter alert prioritization.
Behavioral Support Through Digital Tools
Many RPM platforms also include mobile apps and digital health solutions that guide patients between clinical touchpoints. These tools offer:
• Reminders for readings or medication
• Educational content tailored to patient conditions
• Progress tracking to keep users motivated
Features like these are critical for home-based care, where clinical presence is limited. They help patients feel supported even when providers aren’t physically nearby.
In one instance, we helped the platform’s intuitive app pair instructional videos with heart rate tracking, encouraging patients to stay active and engaged throughout rehab.
Related read: Patient Monitoring: A Guide for Healthcare Providers
Want to See How RPM Can Reduce Hospital Visits and Improve Adherence in Your Home Care Program?
Fewer Hospital Visits and Emergency Escalations
Detecting Deterioration Early
One of the most important benefits of remote patient monitoring for home health is its role in preventing avoidable hospitalizations. Care providers can identify minor changes in patients’ condition long before they become critical by regularly monitoring vital signs.
For instance, a small but consistent increase in a patient’s resting heart rate or a dip in oxygen saturation can signal the early stages of deterioration. These markers often go unnoticed in traditional care models but are flagged immediately in an RPM setup.
With DischargeFollow AI, home health teams can proactively engage patients after discharge, reducing the risk of unplanned hospital visits.
Avoiding Unnecessary ER Admissions
RPM helps distinguish between real emergencies and manageable symptoms. For elderly or chronically ill patients, not every discomfort requires a trip to the hospital. But without monitoring, it’s hard to tell the difference. This uncertainty leads to frequent and often unnecessary ER visits.
Care teams can examine the patient’s previous developments and make well-informed judgments when implementing RPM. They can offer distant reassurance if the data appears stable. Real-time insights and a thorough comprehension of the patient’s situation serve as a guide for any necessary intervention.
The platform we helped to build demonstrates this value. Their integrated RPM system tracks patients post-discharge, allowing providers to catch issues before they become acute. This proactive approach improves patient outcomes and reduces the financial strain on families and care systems.
Involving Caregivers Through Shared Alerts
Family Access to Patient Data
Remote patient monitoring for home health doesn’t just benefit clinicians—it also brings caregivers and family members into the loop. With shared access to dashboards or simple SMS/email alerts, family members can stay informed about the patient’s condition in real time.
This is especially helpful for elderly patients or those who rely on loved ones for daily care. For example, if a patient’s blood pressure spikes, the care team and the caregiver can be notified immediately, allowing for faster action and peace of mind.
In one of our projects, the RPM platform was designed to support real-time data visibility for providers and caregivers. This transparency helped everyone involved make better decisions and act swiftly when needed.
Supporting Non-Clinical Decisions
Caregivers are often responsible for more than just medication. They manage hydration, nutrition, rest, and mobility—factors impacting recovery as much as clinical treatment. RPM alerts help guide these day-to-day choices.
For instance, if a patient’s oxygen levels drop overnight, the caregiver might open windows for ventilation, check the CPAP machine, or prepare to contact the provider if needed. With the right data at the right time, they’re no longer guessing—they’re informed and prepared.
Involving caregivers builds trust, improves adherence, and ensures that patients get consistent support, even when the care team isn’t physically present.
Related read: Patient Monitoring: A Guide for Healthcare Providers
How Mindbowser Supports Home Health Agencies with RPM Solutions
Mindbowser helps home health agencies build and scale remote patient monitoring systems that are practical, compliant, and easy for providers and patients. Our approach focuses on creating real-world solutions that improve care delivery without complicating already stretched clinical teams.
End-to-End RPM Platform Development
We’ve designed and delivered RPM systems that include:
• Mobile apps for patients to connect devices and submit vitals
• Web dashboards for care managers to track and prioritize interventions
• Admin panels to manage device logistics, service metrics, and billing data
Each module is designed with HIPAA compliance, accessibility, and caregiver coordination in mind.
Real-Time Data Flow & Alerts
Our systems enable Bluetooth and cloud-based integrations that keep data flowing securely. Care teams receive alerts on anomalies, allowing them to respond before symptoms escalate.
We also integrate voice-based follow-ups using our patient referral workflow RPMCheck AI—a ready-to-deploy voice solution that makes automated check-in calls to patients using RPM devices. This ensures care teams get timely vitals updates, even from patients who aren’t app-savvy.
Billing and Compliance Built-In
Our platforms support CPT tracking, insurance eligibility checks, and audit-ready logs. Everything is structured to help you meet CMS guidelines while optimizing reimbursement.
Whether you’re launching a new home health RPM program or looking to upgrade your existing setup, we can step in as your development and strategy partner, bringing together engineering, healthcare expertise, and regulatory readiness under one roof.
Looking to implement home health remote monitoring that improves outcomes and scales with your care team?
Talk to our experts to design a workflow-driven RPM solution tailored for your home health agency.

Conclusion
Remote patient monitoring for home health has reshaped how we care for patients outside traditional facilities. It bridges the gap between clinic visits, allowing providers to stay informed, patients to stay safe, and caregivers to stay connected.
The advantages are clear: real-time data, early intervention, fewer hospital trips, better adherence, and stronger coordination among care teams and families. As the demand for home-based care grows, RPM offers a practical, proven way to deliver better outcomes without overwhelming the system.
Suppose you’re exploring ways to bring RPM into your home health operations. In that case, it’s time to think beyond devices—think about building a system that truly works for patients, providers, and caregivers alike.
Home health remote monitoring uses connected devices to track patients’ vital signs and send data to care teams in real time, enabling remote clinical oversight and timely interventions.
It improves adherence, reduces hospital visits, enables early intervention, and helps caregivers stay involved in patient care.
Yes, RPM services can be reimbursed through CPT codes such as 99453, 99454, 99457, and 99458, depending on documentation and engagement requirements.
Patients with chronic conditions, post-surgical recovery needs, and elderly individuals benefit the most from continuous monitoring and early intervention.
By identifying early signs of deterioration, RPM allows providers to intervene before conditions worsen, preventing avoidable hospitalizations.




















 BLOGS
BLOGS  NEWSROOM
NEWSROOM  CASE STUDIES
CASE STUDIES  WEBINARS
WEBINARS  PODCASTS
PODCASTS  ASSET HUB
ASSET HUB  EVENT CALENDAR
EVENT CALENDAR 





















