TL;DR
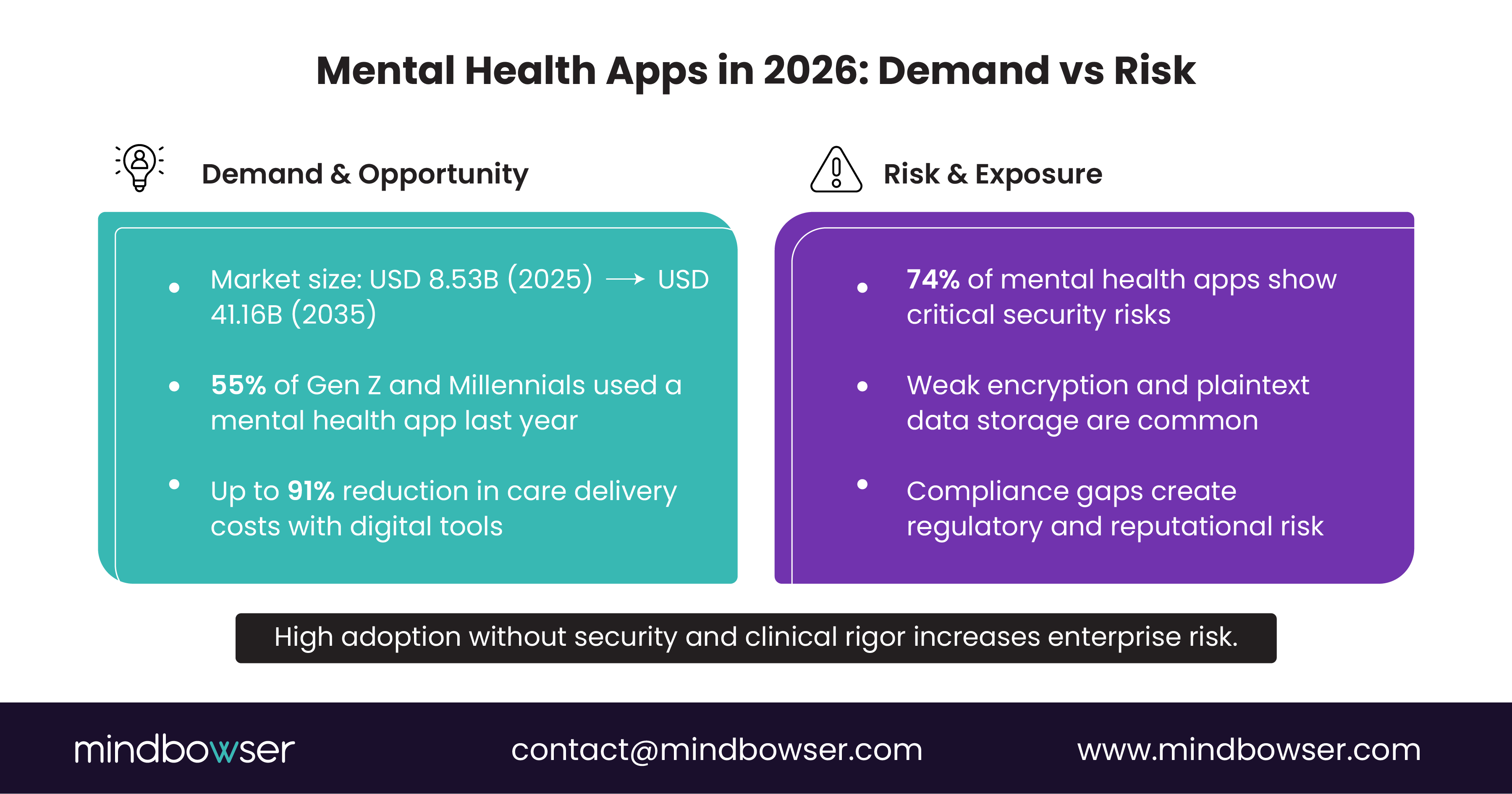
- The global mental health apps market reached USD 8.53B in 2025 and is projected to surpass USD 41.16B by 2035, making 2026 a decisive window for scalable, defensible product bets.
- Adoption has crossed the tipping point: 55% of Gen Z and Millennials report using a mental health app in the past year, reshaping expectations for care access across providers, employers, and payers.
- Digital mental health tools have delivered up to a 91% reduction in care delivery costs compared to traditional therapy, shifting the ROI conversation from “nice to have” to “operational imperative”.
- Security remains the largest downside risk: static and dynamic analysis have found that 74% of tested mental health apps had critical security risks, including weak cryptography and plaintext data storage.
- Mental health apps operating across regions must comply with both HIPAA and GDPR, typically combining strict encryption requirements with explicit, granular consent flows and increasingly aligning with healthcare interoperability standards.
- Mindbowser helps product leaders de-risk builds by combining healthcare UX, compliance-ready architecture, analytics, and interoperability into production-grade mental health platforms built for outcomes, not experiments.
“If you launched or funded a mental health app today, could you confidently defend it to a regulator, a clinician, and a CFO at the same time?”
That is the question facing CPOs, CTOs, and Heads of Digital across:
- venture-backed mental health startups,
- provider organizations modernizing behavioral health access, and
- employers and payers funding digital mental health benefits at scale.
The challenge is not demand. Its credibility and risk.
Most on-demand mental health apps still suffer from the same structural gaps:
- fragmented feature sets optimized for engagement, not outcomes,
- limited clinical validation beyond surface-level content, and
- architectures that treat compliance and security as retrofits rather than foundations.
Yet the market has moved decisively. The global mental health apps market reached USD 8.53B in 2025 and is projected to surpass USD 41.16B by 2035. Capital is flowing, but scrutiny is rising faster.
Before investing further in development or scale, executive teams must resolve three questions upfront:
- Clinical credibility: Will this app deliver evidence-backed support or will it be dismissed as “wellness content” by clinicians and buyers?
- Compliance readiness: Is HIPAA and GDPR compliance built into encryption, consent, and data flows from day one or deferred as technical debt?
- Business outcomes: Can we demonstrate measurable clinical outcomes and ROI within 12–18 months to employers, payers, or health systems?
This guide reframes the “top features” conversation for 2026 through the lens of risk, outcomes, compliance, and return on investment, not feature checklists.
I. Why On-Demand Mental Health Apps Matter in 2026?
On-demand mental health apps are no longer experimental tools at the edge of care delivery. They have become a front door, often the first and sometimes the only point of engagement for millions of users navigating stress, anxiety, burnout, and chronic mental health conditions.
Adoption data makes this shift unambiguous. 55% of Gen Z and Millennials report using a mental health app in the past year, setting a new baseline expectation for immediacy, personalization, and digital-first access across employer-sponsored benefits, payer programs, and provider extensions. For health systems and funded startups alike, not offering a credible digital option increasingly looks like a gap in access strategy.
The economic signal is just as strong. Digital mental health tools have delivered up to a 91% reduction in care delivery costs compared to traditional therapy, driven by scalable interventions, asynchronous support, and more efficient clinician utilization. In a margin-constrained environment, this has pushed mental health apps from “engagement layer” to cost-structure lever, especially for employers and payers under pressure to show outcomes within contract cycles.
However, demand and ROI are colliding with an uncomfortable reality. Static and dynamic analysis have found that 74% of tested mental health apps had critical security risks, including weak cryptography and plaintext data storage. For executives, this creates a high-stakes imbalance: rapid adoption on one side, and material regulatory, reputational, and patient-safety risk on the other.
In 2026, the winners in digital mental health will not be the teams that ship fastest but those that build secure, clinically credible, and outcome-measurable platforms from the ground up.
II. Top 12 Must-Have Features for a 2026 Mental Health App
Below, we move through the features by feature. Each one is framed for product, clinical, compliance, and ROI decision-making in 2026.

A. Feature #1: Seamless UI and UX
In mental health products, UI and UX are not cosmetic decisions. They directly influence clinical adherence, user trust, and downstream outcomes. A confusing or overstimulating interface increases abandonment risk and can undermine care delivery.
Aspect | What to Decide in 2026 |
UX | Design for emotionally taxed users with minimal cognitive load and clear navigation |
Clinical | Avoid engagement mechanics that conflict with therapeutic intent |
Data / Security | Secure session handling without repeated authentication friction |
Analytics / ROI | Track drop-off points against symptom improvement and retention |
From a leadership perspective, seamless UX is not about delight alone. It is about reducing friction at moments of vulnerability, where even small usability failures can lead to lost engagement and weaker outcomes.
Mindbowser applies healthcare-specific UX research, accessibility standards, and iterative testing to design interfaces that support sustained engagement while meeting compliance and security requirements.
B. Feature #2: Self-Assessment Tools
Self-assessment tools act as the entry point to care and risk stratification. In 2026, they must go beyond engagement checklists and be defensible as clinically grounded instruments that inform next-step interventions rather than serve as self-diagnosis tools.
Aspect | What to Decide in 2026 |
UX | Keep assessments short, adaptive, and easy to complete under stress |
Clinical | Use validated screening frameworks and clinician-reviewed scoring logic |
Data / Security | Treat responses as PHI with encryption and strict access controls |
Analytics / ROI | Link assessment scores to engagement, escalation, and outcomes |
From a product leadership standpoint, poorly designed self-assessments introduce both clinical and legal risk. Overly long or ambiguous questionnaires reduce completion rates, while non-validated tools can undermine provider trust and payer adoption.
Mindbowser works with clinical stakeholders to design assessment flows that are evidence-aligned, auditable, and analytics-ready, enabling teams to defend both care decisions and outcomes.
C. Feature #3: Personalized Content
Personalization is one of the strongest engagement levers in mental health apps, but it is also one of the easiest ways to introduce compliance, safety, and trust issues. In 2026, personalization must be deliberate, explainable, and governed by consent rather than opaque algorithms.
Aspect | What to Decide in 2026 |
UX | Make it clear why specific content is recommended and allow user control |
Clinical | Ensure personalization reinforces care plans rather than replacing them |
Data / Security | Use explicit consent and limit secondary data usage |
Analytics / ROI | Measure impact on adherence, symptom improvement, and retention |
For product leaders, the question is no longer whether to personalize, but how far. Over-automated recommendations without clinical guardrails can drift into unsafe territory, while under-personalization reduces engagement and perceived value.
Mindbowser helps teams design personalization frameworks that balance relevance with transparency, using consent-driven data models and analytics that support outcome measurement without overexposing user data.
D. Feature #4: Mood Tracking
Mood tracking converts subjective experience into longitudinal data that can inform both self-awareness and care decisions. In 2026, this data should be treated with the same rigor as any other health signal, especially when it influences recommendations or escalation paths.
Aspect | What to Decide in 2026 |
UX | Keep logging simple and non-intrusive to avoid survey fatigue |
Clinical | Align mood models with evidence-based emotional regulation frameworks |
Data / Security | Encrypt mood entries and restrict internal access by role |
Analytics / ROI | Analyze trends over time rather than isolated data points |
From a leadership perspective, mood tracking becomes risky when it is overinterpreted or underprotected. Raw mood data without a clinical context can lead to false conclusions, while weak security controls expose highly sensitive emotional information.
When implemented correctly, mood tracking strengthens engagement, enables early pattern detection, and supports measurable outcomes without increasing regulatory exposure.
Want to Create a Mental Health App that Makes a Real Difference? Let's Talk!
E. Feature #5: Sessions, Webinars, and Psychoeducation
Educational sessions and psychoeducation content shape how users understand their symptoms, options, and expectations of care. In 2026, this content must reinforce clinical pathways rather than function as generic wellness media.
| Aspect | What to Decide in 2026 |
UX | Deliver content in short, modular formats that fit real usage patterns |
Clinical | Ensure sessions are created or reviewed by qualified professionals |
Data / Security | Control access to live and recorded sessions, especially when PHI is discussed |
Analytics / ROI | Track completion and downstream behavior change, not just views |
For executive teams, the risk lies in ungoverned content sprawl. Without clinical oversight and version control, educational libraries quickly become outdated or misaligned with evidence-based practice.
Well-structured psychoeducation, when tied to assessments and progress tracking, supports informed engagement and improves the likelihood of measurable outcomes.
F. Feature #6: Daily Activities and Exercises
Daily activities and exercises translate intent into behavior. In 2026, their value is determined less by volume and more by consistency, adaptability, and clinical alignment.
| Aspect | What to Decide in 2026 |
UX | Design for habit formation without creating pressure or guilt |
| Clinical | Align exercises with recognized therapeutic models such as CBT or mindfulness |
Data / Security | Capture only what is necessary and store it securely |
Analytics / ROI | Measure adherence and its relationship to symptom change |
From a product leadership standpoint, daily interventions should support sustainable routines rather than novelty-driven engagement. Overly complex exercises reduce follow-through, while poorly aligned activities weaken clinical credibility.
When these features are adaptive and measured accurately, they become a key driver of long-term retention and improved outcomes.
G. Feature #7: Progress Tracking
Progress tracking turns day-to-day engagement into evidence of impact. In 2026, it is one of the primary mechanisms executives use to evaluate whether a mental health app is delivering value beyond usage metrics.
Aspect | What to Decide in 2026 |
UX | Present progress in clear, non-judgmental visual formats |
Clinical | Track milestones that reflect meaningful clinical change |
Data / Security | Aggregate data securely with role-based access |
Analytics / ROI | Translate user progress into outcome and ROI reporting |
For leadership teams, progress tracking is the bridge between product metrics and business outcomes. Without it, conversations with employers, payers, or provider partners remain subjective.
Well-designed progress indicators support transparency, accountability, and continuous improvement across both care delivery and product strategy.
H. Feature #8: Community and Support Groups
Community features can significantly increase engagement and retention, but they also introduce complexity in moderation, safety, and compliance. In 2026, these features must be designed as controlled environments rather than open social spaces.
Aspect | What to Decide in 2026 |
UX | Enable participation without forcing identity disclosure |
Clinical | Clearly separate peer support from clinical care |
Data / Security | Protect anonymity and maintain audit trails |
Analytics / ROI | Measure retention and safety indicators together |
From a product and risk perspective, unmanaged communities can quickly become liabilities.
Clear usage guidelines, reporting mechanisms, and escalation paths are essential to protect users and the organization.
When governed properly, support groups reinforce belonging and normalize help-seeking behavior without crossing clinical or regulatory boundaries.
I. Feature #9: Teletherapy Integration
Teletherapy has moved from a differentiator to an expectation. In 2026, the strategic question is not whether to offer virtual therapy, but how tightly it is integrated into clinical workflows and the broader care ecosystem.
Aspect | What to Decide in 2026 |
UX | Make scheduling, modality selection, and session access frictionless |
Clinical | Support licensed providers with appropriate documentation workflows |
Data / Security | Secure video, messaging, and session records end-to-end |
Analytics / ROI | Track utilization, wait times, and outcome correlations |
For executive teams, teletherapy integration affects both scale and cost structure. Poorly integrated tools increase clinician burden and reduce throughput, while secure and efficient workflows improve access without inflating operational costs.
A well-implemented teletherapy layer also creates the foundation for future interoperability with provider systems and care teams.
J. Feature #10: Crisis Management Resources
Crisis management features represent a non-negotiable safety layer in any mental health app. In 2026, they must be designed for immediacy, clarity, and responsible escalation rather than as passive resource lists.
Aspect | What to Decide in 2026 |
UX | Provide one-tap access during high-stress moments |
Clinical | Align escalation paths with recognized crisis response standards |
Data / Security | Minimize data retention and avoid unnecessary logging |
Analytics / ROI | Track incidents, response times, and resolution outcomes |
From a leadership perspective, crisis support is closely tied to liability and trust. Ambiguous instructions or delayed access can have serious consequences, while over-collection of data during crisis events increases regulatory risk.
Clear, well-governed crisis pathways reinforce user safety and demonstrate organizational responsibility to regulators, partners, and users alike.
K. Feature #11: Data Security and Privacy
Data security and privacy are foundational requirements, not feature enhancements. In 2026, mental health apps are expected to meet healthcare-grade security standards by default, especially given the sensitivity of behavioral health data.
| Aspect | What to Decide in 2026 |
UX | Communicate privacy practices clearly and in plain language |
Clinical | Preserve trust by minimizing unnecessary data exposure |
Data / Security | Enforce encryption, role-based access, and continuous monitoring |
Analytics / ROI | Reduce breach risk, audit costs, and compliance overhead |
For executive teams, security failures represent material business risk. Regulatory penalties, loss of customer trust, and partner hesitation can quickly outweigh any short-term gains from rapid feature delivery.
A security-first approach enables sustainable scale, cross-region deployment, and long-term enterprise adoption without recurring remediation cycles.
L. Feature #12: Accessibility Features
Accessibility determines who can realistically use your mental health app and who is excluded. In 2026, accessibility is both a regulatory expectation and a practical requirement for reaching diverse populations.
Aspect | What to Decide in 2026 |
UX | Design interactions that work across cognitive, visual, and motor needs |
Clinical | Ensure accessibility does not alter therapeutic intent |
Data / Security | Maintain compatibility with assistive technologies without data leakage |
Analytics / ROI | Track expanded reach and reduced abandonment across user segments |
For leadership teams, accessibility failures translate into missed reach, reputational risk, and potential regulatory exposure. Aligning with standards such as WCAG helps ensure usability without introducing unintended barriers.
When accessibility is embedded from the start, it strengthens equity, improves adoption, and supports long-term scalability across markets.
III. Costs and Timeline for Mental Health App Development in 2026
By 2026, the cost of building a mental health app will no longer be driven primarily by UI or basic feature delivery. The real cost determinants are clinical rigor, depth of compliance, integrations, and post-launch accountability.
For executive teams, the more relevant question is not “What will this cost to build?” but “What level of operational, regulatory, and outcome risk are we underwriting?”
A. Typical Investment Ranges by Scope

B. Mental Health App Development Process (2026 View)
In regulated mental health products, skipping or compressing steps rarely saves time. It usually shifts risk downstream.
- Discovery and Clinical Framing
- Define target population, use cases, and care boundaries
- Select assessment frameworks and therapeutic models
- Identify regulatory exposure early
- Compliance and Security Architecture
- Map HIPAA and GDPR requirements to data flows
- Design encryption, access controls, consent, and audit logging
- Establish security baselines before feature development
- UX and Product Design
- Design low-friction flows for stressed users
- Validate accessibility requirements
- Prototype critical moments such as onboarding and crisis access
- Feature Development and Integration
- Build core features with secure APIs
- Integrate teletherapy, analytics, and third-party services where needed
- Prepare for future interoperability and scaling
- Validation, Testing, and Risk Review
- Security testing and privacy validation
- Clinical review of assessments and content
- Performance and usability testing
- Launch and Post-Launch Operations
- Monitoring, logging, and incident response
- Ongoing compliance checks and updates
- Continuous improvement based on outcome and usage data
C. Key Cost Drivers Executives Must Account For
- Feature scope and depth
Shipping a checklist of features is cheaper than operationalizing them. For example, mood tracking without analytics is low-cost but low-value. Mood tracking tied to outcomes, escalation, and reporting changes the cost profile. - Clinical validation and governance
Involving clinicians in assessment design, content review, and escalation logic adds time and cost upfront but significantly reduces downstream rework, liability, and buyer friction. - Integrations and ecosystem fit
Connecting with EHRs, employer identity systems, or payer platforms introduces architectural complexity but is often required for enterprise adoption and revenue scale. - Security and compliance posture
HIPAA and GDPR compliance are not one-time checkboxes. Encryption, access controls, audit logging, consent management, and periodic reviews materially affect both build timelines and ongoing budgets. - Post-launch operations
Monitoring, security updates, analytics refinement, and regulatory audits are recurring investments. Teams that underfund this phase often incur higher costs later through remediation or reputational damage.
From a leadership perspective, higher upfront investment in compliant architecture and outcome measurement tends to compress time to enterprise deals, renewals, and proof of value. Cost discipline in 2026 is less about minimizing spend and more about avoiding expensive course corrections after launch.

Why Mindbowser Is a Strong Build Partner for Mental Health Apps?
Building a mental health app in 2026 requires more than fast delivery. It demands product leadership that understands clinical risk, regulatory scrutiny, and the economics of digital care. Mindbowser partners with product and technology leaders to build platforms that can scale without compromising trust, compliance, or outcomes.
A. Product and UX Leadership
Mental health products succeed or fail at the intersection of usability and clinical intent. Mindbowser applies user-centered design, accessibility standards, and rapid experimentation to ensure products are intuitive for users under stress while remaining aligned with therapeutic goals. This approach reduces abandonment, supports adherence, and improves the reliability of outcomes.
B. Secure, Compliant Backend Architecture
Mental health apps operating across regions must comply with both HIPAA and GDPR, typically combining strict encryption requirements with explicit, granular consent flows. Mindbowser designs backend systems with encryption, role-based access control, audit logging, and privacy-by-design principles so compliance is built into the architecture rather than layered on later.
C. Interoperability and Data Strategy
As digital mental health becomes part of broader care delivery, interoperability is no longer optional. Mindbowser brings experience in healthcare data models, analytics, and standards-based integration, including support for SMART on FHIR where applicable. This enables mental health platforms to integrate with provider workflows, reporting systems, and enterprise stakeholders.
D. Delivery and Long-Term Support
Launching the app is only the beginning. Mindbowser supports teams through post-launch monitoring, security updates, performance optimization, and iterative feature enhancements. This long-term partnership model helps organizations adapt to regulatory changes, evolving clinical standards, and growing user populations without destabilizing the platform.
Clinical credibility requires more than licensed branding or content libraries. In 2026, it means using validated assessments, clinician-reviewed content, clearly defined escalation paths, and measurable outcomes tied to symptom improvement. Buyers increasingly expect evidence that features align with recognized therapeutic models and standards of care.
Any mental health app handling identifiable health data and offering assessments, therapy, or care recommendations must be designed to comply with HIPAA in the U.S. and GDPR for users in or connected to the EU. This typically includes encryption, role-based access, audit logs, and explicit user consent flows, especially for cross-region deployments.
Most organizations begin to see measurable outcomes within 12 to 18 months when apps are designed with analytics and outcome tracking from day one. ROI often comes from reduced care-delivery costs, improved engagement, and better utilization of clinical resources, rather than from user growth alone.
The most common risks include weak encryption, improper data storage, insufficient access controls, and inadequate monitoring. Behavioral health data is particularly sensitive, making security lapses more damaging both legally and reputationally. A security-first architecture significantly reduces long-term risk.
For enterprise adoption by providers, payers, or employers, integration is increasingly expected. Interoperability enables better care coordination, reporting, and clinical oversight. While not always required for early MVPs, it becomes a critical capability as platforms scale and pursue larger contracts.































